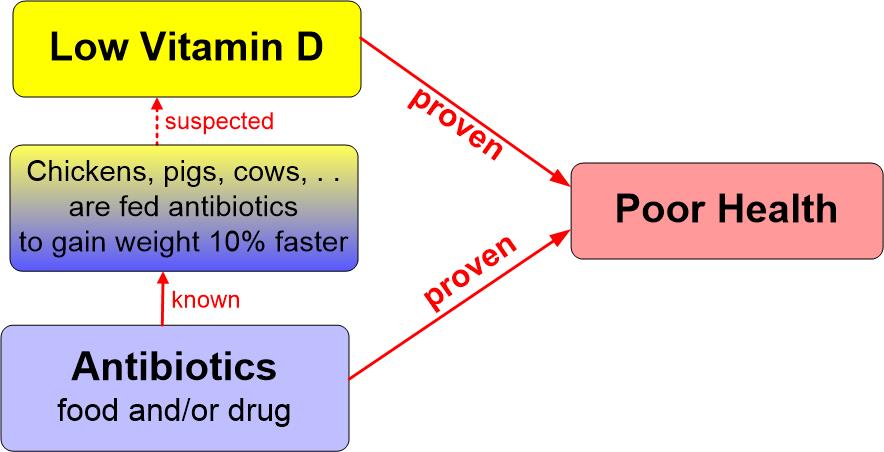
Antibiotics and Vitamin D are associated with many of the same diseases
Missing Microbes book (April 2014) powerfully relates
many disease increases to increased use of antibiotics
The author (Martin Blaser martin.blaser@med.nyu.edu ) , a world expert on antibiotics, makes very strong cases that antibiotics is the cause of many of the increases in diseases we have seen in the past 10-30 years: such as obesity, diabetes, asthma, autism, ...
Due to huge increase in antibiotics courses for humans AND virtually continuous low-level antibiotics for farm animals
(it increases weight by about 10% with no increase in feed cost)
Author provides strong support with both mouse and human trials.
Basically broad spectrum antibiotics kills off the "good" bugs as well as the bad ones. (Narrow spectrum are rarely available and are far far more expensive)
Vitamin D improves immune function, so vitamin D is able to treat many of the problems causes by antibiotics
Author calls for reduced used of antibiotics, especially in first 2 years of life
Similar calls for reduced antibiotics for humans and farm animals in Europe in a previous decade has not resulted in much change.
Risk Factors seem to have a maximum of about 15X for:
Vitamin D, Antibiotics, and Genetics
Risk Factors seem to be smaller for:
environment, exercise, smoking, pollution, toxins in food, etc.
{include}
Strong indications in Missing Microbes that early antibiotics increases the risk of obesity
Farmers have been giving low-level anitbiotics to animals since they learned long ago that it would increase by 10% the animal weight without increased cost of feed
Mice given low-level antibiotics for first 4 weeks of life become heavier later in life
Children who are given antibiotics in first 6 months of life are 5X more likely to become obese (study in England of 14,000 births)
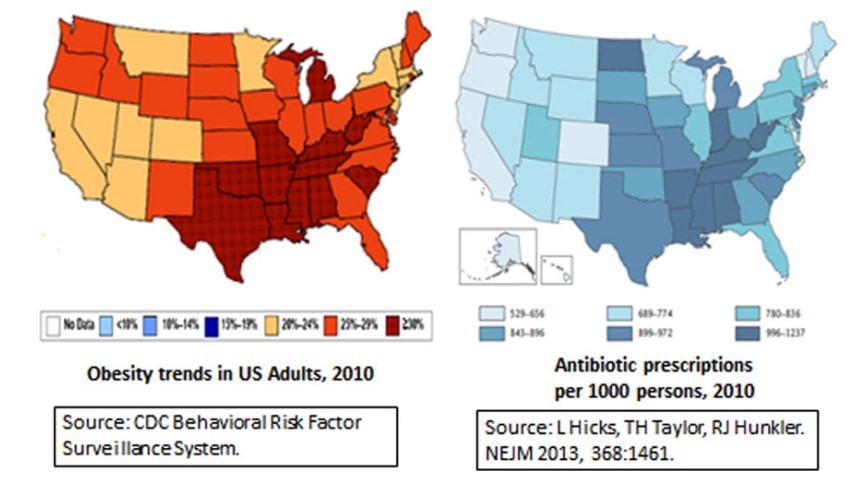
US States which get the most antibiotics are those states with the most obesity (CDC)
Obese US adults have 1/2 of the gut biotic diversity of non-obese adults (400,000 vs 800,000)
Germ-Free mice became obese when given fecal transplants from mice who had antibiotics and became obese
- This is a strong indication that the cause of the obesity was the gut microbiome
Misc. notes from the book Missing Microbes
100 Million neurons in gut (vs 100 Billion neurons in adult brain)
Author is very concerned about increased antibiotics ==> increased disease
Author is extremely concerned about antibiotic resistance ==> world-wide pandemic - far worse than any in the past 500 years
17 antibiotic courses by age 20 in the US now (varies a lot with which state you live in - see map below)
Antibiotics in US children < age 2: 1365 / 1000 (average of more than 1 per child)
Sweden banned antibiotics for farm animal weight gain in 1986
US continues to give antibiotics to new-born infant eyes - vs Sweden does not, and has no eye infection anyway
C-Section 4% in Sweden, 30% in US (go to 50% by 2020), and 80% in Rome
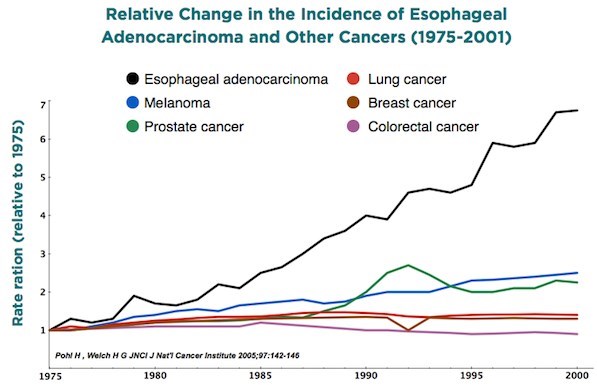
Esophageal Cancer increased 6X in 30 years (see chart on this page) - while H.pylori decreased
Currently only 6% of US children have H.pylori
GERD (Heart Burn) currently 10-20% of US - author believes it it due to reduction in H.pylori
Study found 8X more GERD if no H.pylori
GERD has suspected 2-way-link with Asthma
Modern plagues : obesity, T1 diabetes, asthma, hay fever, food allergies, esphageal reflux and cancer, celiac disease, chron’s disease, ulcerative colitits, autism, ecezma, MRAS, C-diff; also increase in C-sections
There are perhaps 10,000 species of bacteria in the adult human colon.
- There appear to be no bacteria in fetus before birth.
Author is against using antibiotics for runny nose and ear infections. 80% of upper RTI are virus – which are not treated with antibiotics
BRCA breast cancer developes earlier in women born after 1940 (had antibiotics)
C.diff infections (antibiotic resistant) now account for 250,000 hospitalizations and 14,000 deaths
- C.diff cure rate with fecal transfer 94 % , standard drug cure rate is only 31%
- And it's not far fetched to think that ( fecal transfer ) also could be used to treat obesity and a variety of immunoloic disorders, possibly including autism
MRSA infections (antibiotic resistant) now affect 2,000,000 US per year for 250,000 hospitalizations and 23,000 deaths
Author is concerned that many "contingency" organisms are totally wiped out by antibiotics - probiotics does NOT replace them ANTIBIOTIC WINTER
- 15-40% of microbial diversity is lost in otherwise normal individuals (for more loss of diversity in those who are obese, . . )
70% of kids with upper respiratory infection get an antibiotic - when the problem is typically due to a virus - which is not stopped by antibiotics
Many countries have been trying to preserve "antibiotic efficacy" for 10-20 years.
- FDA started thinking about an optional decrease in antibiotics for animals in 2013
- July 2014 update: Court ruling: FDA can allow antibiotics in animal feed NY Times
- FDA started thinking about an optional decrease in antibiotics for animals in 2013
Hardly any good trials of probiotics so far. Author anticipates probiotics will be standard care with antibiotics (10-20 years?)
Esophageal Cancer
Thoughts by Henry Lahore - admin of VitaminDWiki
- Are there societies which have had very little or perhaps no antibiotics?
- Have their disease rates increased?
What % of weight gain can be explained by the antibiotic data
Chemotherapy leads to bacterial infection – wonder if Chemo is like antibiotic – author does not seem to say
So, what might be increasing so many diseases all around the world?
- besides: Increased Antibiotics, and Decreased vitamin D?
- If not, what %. Are they synergistic?
Update Sept 2015
Blaser is heading a task force to look at alternatives. First meeting Sept 29 2015
The US Is Finally Taking Action on Antibiotic Resistance Wired Magazine
We’ll be asking questions like:
How do we curtail antibiotic use?
Can we come up with alternatives to antibiotics?
Can we have narrow spectrum antibiotics that only target harmful bacteria?
Can we develop new diagnostics to show viral versus antibacterial infections?
Association of caesarean delivery with child adiposity from age 6 weeks to 15 years.
Int J Obes (Lond). 2013 Jul;37(7):900-6. doi: 10.1038/ijo.2013.49. Epub 2013 Apr 8.
Blustein J1, Attina T, Liu M, Ryan AM, Cox LM, Blaser M J, Trasande L.
OBJECTIVES: To assess associations of caesarean section with body mass from birth through adolescence.
DESIGN: Longitudinal birth cohort study, following subjects up to 15 years of age.
SETTING AND PARTICIPANTS: Children born in 1991-1992 in Avon, UK who participated in the Avon Longitudinal Study of Parents and Children (ALSPAC) (n=10 219).
OUTCOME MEASURES: Primary outcome: standardized measures of body mass (weight-for length z-scores at 6 weeks, 10 and 20 months; and body mass index (BMI) z-scores at 38 months, 7, 9, 11 and 15 years). Secondary outcome: categorical overweight or obese (BMI: 85th percentile) for age and gender, at 38 months, 7, 9, 11 and 15 years.
RESULTS: Of the 10 219 children, 926 (9.06%) were delivered by caesarean section. Those born by caesarean had lower-birth weights than those born vaginally (-46.1 g, 95% confidence interval(CI): 14.6-77.6 g; P=0.004). In mixed multivariable models adjusting for birth weight, gender, parental body mass, family sociodemographics, gestational factors and infant feeding patterns, caesarean delivery was consistently associated with increased adiposity, starting at 6 weeks (+0.11 s.d. units, 95% CI: 0.03-0.18; P=0.005), through age 15 (BMI z-score increment+0.10 s.d. units, 95% CI: 0.001-0.198; P=0.042). By age 11 caesarean-delivered children had 1.83 times the odds of overweight or obesity (95% CI: 1.24-2.70; P=0.002). When the sample was stratified by maternal pre-pregnancy weight, the association among children born of overweight/obese mothers was strong and long-lasting. In contrast, evidence of an association among children born of normal-weight mothers was weak.
CONCLUSION: Cesarean delivery is associated with increased body mass in childhood and adolescence. Research is needed to further characterize the association in children of normal weight women. Additional work is also needed to understand the mechanism underlying the association, which may involve relatively enduring changes in the intestinal microbiome.
PMID: 23670220
Probiotics, prebiotics, and the host microbiome: the science of translation.
Ann N Y Acad Sci. 2013 Dec;1306:1-17. doi: 10.1111/nyas.12303. Epub 2013 Nov 22.
Petschow B1, Doré J, Hibberd P, Dinan T, Reid G, Blaser M , Cani PD, Degnan FH, Foster J, Gibson G, Hutton J, Klaenhammer TR, Ley R, Nieuwdorp M, Pot B, Relman D, Serazin A, Sanders ME.
Recent advances in our understanding of the community structure and function of the human microbiome have implications for the potential role of probiotics and prebiotics in promoting human health. A group of experts recently met to review the latest advances in microbiota/microbiome research and discuss the implications for development of probiotics and prebiotics, primarily as they relate to effects mediated via the intestine. The goals of the meeting were to share recent advances in research on the microbiota, microbiome, probiotics, and prebiotics, and to discuss these findings in the contexts of regulatory barriers, evolving healthcare environments, and potential effects on a variety of health topics, including the development of obesity and diabetes; the long-term consequences of exposure to antibiotics early in life to the gastrointestinal (GI) microbiota; lactose intolerance; and the relationship between the GI microbiota and the central nervous system, with implications for depression, cognition, satiety, and mental health for people living in developed and developing countries. This report provides an overview of these discussions.
© 2013 The Authors. Annals of the New York Academy of Sciences published by Wiley Periodicals, Inc. on behalf of New York Academy of Sciences.
PMID: 24266656
Probiotics, prebiotics, and the host microbiome - the science of translation – June 2013 is extracted with highlights by VitaminDWiki
PDF (Dec 2013) is attached at the bottom of this page
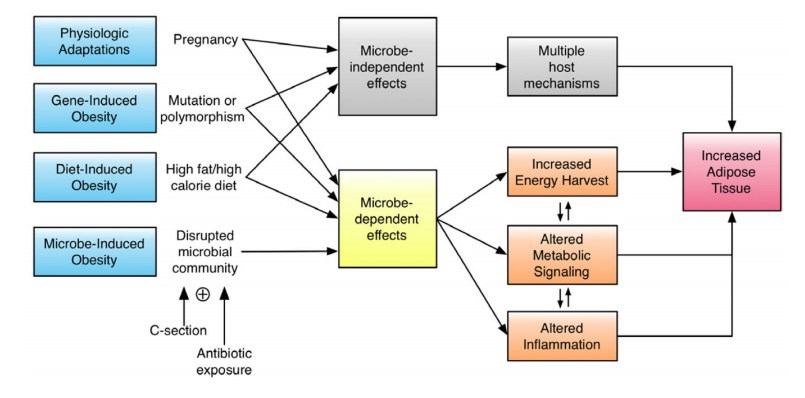
Pathways in microbe-induced obesity.
Cell Metab. 2013 Jun 4;17(6):883-94. doi: 10.1016/j.cmet.2013.05.004.
Cox LM1, Blaser M J.
Diet, host gene composition, and alterations in the intestinal microbiota can contribute to obesity. In microbe-induced obesity, metabolic changes stem from primary perturbation of the microbiota, consequent to modern changes in human biology. Microbiota disruption during early development can result in syndromes of metabolic dysfunction. We focus on the pathways involved in these interactions, particularly related to energy extraction and the role of inflammation in the metabolic phenotypes. Model physiologic systems and perturbations including gastric bypass surgery, pregnancy, and hibernation provide insight into the respective roles of the critical participants.
Copyright © 2013 Elsevier Inc. All rights reserved.
PMID: 23747247
PDF (Micro-induced is attached at the bottom of this page
A Brave New World: The Lung Microbiota in an Era of Change
Annals of the American Thoracic Society, Vol. 11, No. Supplement 1 (2014), pp. S21-S27. doi: 10.1513/AnnalsATS.201306-189MG
Leopoldo N. Segal1 and Martin J. Blaser 1
Corresponding Author: Leopoldo N. Segal, M.D., NYU School of Medicine, 462 First Avenue 7W54, New York, NY 10016. E-mail: Leopoldo.Segal@nyumc.org
The development of culture-independent techniques has revolutionized our understanding of how our human cells interact with the even greater number of microbial inhabitants of our bodies. As part of this revolution, data are increasingly challenging the old dogma that in health, the lung mucosa is sterile. To understand how the lung microbiome may play a role in human health, we identified five major questions for lung microbiome research:
(1) Is the lung sterile?
(2) Is there a unique core microbiome in the lung?
(3) How dynamic are the microbial populations?
(4) How do pulmonary immune responses affect microbiome composition? and
(5) Are the lungs influenced by the intestinal immune responses to the gut microbiome?
From birth, we are exposed to continuous microbial challenges that shape our microbiome. In our changing environment, perturbation of the gut microbiome affects both human health and disease. With widespread antibiotic use, the ancient microbes that formerly resided within us are being lost, for example, Helicobacter pylori in the stomach. Animal models show that antibiotic exposure in early life has developmental consequences. Considering the potential effects of this altered microbiome on pulmonary responses will be critical for future investigations.
Publisher has the PDF behind a $20 paywall
Antibiotic exposure and the development of coeliac disease: a nationwide case-control study.
BMC Gastroenterol. 2013 Jul 8;13:109. doi: 10.1186/1471-230X-13-109.
Mårild K1, Ye W, Lebwohl B, Green PH, Blaser MJ, Card T, Ludvigsson JF.
BACKGROUND:
The intestinal microbiota has been proposed to play a pathogenic role in coeliac disease (CD). Although antibiotics are common environmental factors with a profound impact on intestinal microbiota, data on antibiotic use as a risk factor for subsequent CD development are scarce.
METHODS:
In this population-based case-control study we linked nationwide histopathology data on 2,933 individuals with CD (Marsh stage 3; villous atrophy) to the Swedish Prescribed Drug Register to examine the association between use of systemic antibiotics and subsequent CD. We also examined the association between antibiotic use in 2,118 individuals with inflammation (Marsh 1-2) and in 620 individuals with normal mucosa (Marsh 0) but positive CD serology. All individuals undergoing biopsy were matched for age and sex with 28,262 controls from the population.
RESULTS:
Antibiotic use was associated with
CD (Odds ratio [OR] = 1.40; 95% confidence interval [CI] = 1.27-1.53),
inflammation (OR = 1.90; 95% CI = 1.72-2.10) and
normal mucosa with positive CD serology (OR = 1.58; 95% CI = 1.30-1.92).
ORs for prior antibiotic use in CD were similar when we excluded antibiotic use in the last year (OR = 1.30; 95% CI = 1.08-1.56) or restricted to individuals without comorbidity (OR = 1.30; 95% CI = 1.16 - 1.46).
CONCLUSIONS:
The positive association between antibiotic use and subsequent CD but also with lesions that may represent early CD suggests that intestinal dysbiosis may play a role in the pathogenesis of CD. However, non-causal explanations for this positive association cannot be excluded.
PMID: 23834758
PDF (coeliac disease) is attached at the bottom of this page
More H-pylori, less stroke - Sept 2013
Association between Helicobacter pylori and mortality in the NHANES III study
Gut. 2013 Sep;62(9):1262-9. doi: 10.1136/gutjnl-2012-303018. Epub 2013 Jan 8.
Chen Y1, Segers S, Blaser MJ.
OBJECTIVE:
Persistent colonisation by Helicobacter pylori, and especially by cagA-positive strains, has been related to several health outcomes with effects in opposite directions. Thus, it is important to evaluate its influence on total and category-specific mortality.
DESIGN:
We conducted prospective cohort analyses in a nationally representative sample of 9895 participants enrolled in the National Health and Nutrition Examination Survey III to assess the association of H pylori status with all-cause and cause-specific mortality. Analyses for the association of H pylori cagA positivity with mortality were conducted in 7384 subjects with data on H pylori cagA status.
RESULTS:
In older people (> 40.1 years), H pylori was not associated with all-cause mortality (HR 1.00; 95% CI 0.84 to 1.18).
There was an inverse association of H pylori status with stroke mortality (HR 0.69; 95% CI 0.44 to 1.08), and the inverse association was stronger for H pylori cagA positivity, with the HR of 0.45 (95% CI 0.27 to 0.76). H pylori was also strongly positively related to gastric cancer mortality. After we adjusted p values using the Benjamini-Hochberg false discovery rate method to account for multiple comparisons, these associations remained, and H pylori status was not related to other outcomes.
CONCLUSIONS:
Our findings suggest that H pylori has a mixed role in human health, but is not a major risk factor for all-cause mortality.
PMID: 23303440
Infant antibiotic exposures and early-life body mass.
Int J Obes (Lond). 2013 Jan;37(1):16-23. doi: 10.1038/ijo.2012.132. Epub 2012 Aug 21.
Trasande L1, Blustein J, Liu M, Corwin E, Cox LM, Blaser MJ.
OBJECTIVES:
To examine the associations of antibiotic exposures during the first 2 years of life and the development of body mass over the first 7 years of life.
DESIGN:
Longitudinal birth cohort study.
SUBJECTS:
A total of 11 532 children born at 2500 g in the Avon Longitudinal Study of Parents and Children (ALSPAC), a population-based study of children born in Avon, UK in 1991-1992.
MEASUREMENTS:
Exposures to antibiotics during three different early-life time windows (<6 months, 6-14 months, 15-23 months), and indices of body mass at five time points (6 weeks, 10 months, 20 months, 38 months and 7 years).
RESULTS:
Antibiotic exposure during the earliest time window (<6 months) was consistently associated with increased body mass (+0.105 and +0.083 s.d. unit, increase in weight-for-length Z-scores at 10 and 20 months, P<0.001 and P=0.001, respectively; body mass index (BMI) Z-score at 38 months +0.067 s.d. units, P=0.009; overweight OR 1.22 at 38 months, P=0.029) in multivariable, mixed-effect models controlling for known social and behavioral obesity risk factors. Exposure from 6 to 14 months showed no association with body mass, while exposure from 15 to 23 months was significantly associated with increased BMI Z-score at 7 years (+0.049 s.d. units, P=0.050). Exposures to non-antibiotic medications were not associated with body mass.
CONCLUSIONS:
Exposure to antibiotics during the first 6 months of life is associated with consistent increases in body mass from 10 to 38 months. Exposures later in infancy (6-14 months, 15-23 months) are not consistently associated with increased body mass. Although effects of early exposures are modest at the individual level, they could have substantial consequences for population health. Given the prevalence of antibiotic exposures in infants, and in light of the growing concerns about childhood obesity, further studies are needed to isolate effects and define life-course implications for body mass and cardiovascular risks.
PMID: 22907693
PDF (infant) is attached at the bottom of this page
Microbionome and Obesity - June 2013 video - Dr. Blaser presenting a paper at medical conference
https://www.youtube.com/watch?v=6b-fHqFhqyk
Bibliography - Blaser - NY University
http://library.med.nyu.edu/cgi-bin/facbibx.pl?AU=blasem01&YR;=2000-2015
US Recommendations on antibiotics fails to recommend reduction of farm antibiotics - Sept 2014
Their Report told of the problem on antibiotics on the farm, but the recommendations made little mention of it.
One of the 14 member of the task force was Dennis Treacy, executive vice president of meat-production giant Smithfield Foods.
Perhaps Dennis had something to do with the omission in the recommendations.
Details at White House Actions on Antibiotic Resistance: Big Steps, Plus Disappointments Wired Magazine
Includes links to both their report and their recommendations.
WHO Antibiotics Resistance 2014
📄 Download the PDF from VitaminDWiki.
📄 Download the slides PDF from VitaminDWiki.
Since 2000 Antibiotics in chicken feed only increases growth by only ~ 1%
CAFOs, Your Gut, and Mental Health Mercola March 2015
“The growth response to antibiotics may have decreased over the past 30 years for several possible reasons.
First, the growth response to antibiotics is less important when animal nutrition, hygiene, genetics, and health are optimal. The relative improvement in the growth rate resulting from supplementing the diet of pigs with antibiotics has been shown to be inversely related to the growth rate of animals not being fed antibiotics. With changes in the livestock industry over the past 30 years, all of these factors have improved.
Second, increasing levels of resistance in animals could be diminishing the overall effectiveness of AGPs, although data are lacking to evaluate this hypothesis.”
Organic Lables include
100% USDA Organic label offers excellent assurance that antibiotics have not been used at any stage of production.
"No antibiotics administered" and similar labels also offer high assurance that antibiotics have not been used, especially if accompanied by a "USDA process Verified" shield.
"Grass-fed" label coupled with USDA Organic label means no antibiotics have been used, but if the "grass-fed" label appears alone, antibiotics may have been given.
"American Grass-fed" and " Food Alliance Grass-fed" labels indicate that in addition to having been raised on grass, the animal in question received no antibiotics.
See also VitaminDWiki
Antibiotic use cut in half by elderly (over 70) after monthly 60,000 IU of vitamin D – RCT Dec 2013
Off Topic: 200,000 deaths annually due to superbugs - 10,000,000 annually in 35 years – Dec 2014
Search VitaminDWiki for ANTIBIOTIC 258 items as of July 2014
All items in category Antibiotics/probiotics and Vitamin D items
Medical use of antibiotics increased 36 percent globally in a decade – Aug 2014
- along with big increases in Antibiotic use and Autism in Australia
Hypothesis: antibiotic resistant bacteria can be controlled with vitamin D
Soft Bones, Hard Arteries, Vitamin D, Vitamin K2 and antibiotics – Sept 2012
Superbug (Clostridium difficile) 4.7X more of a problem if low vitamin D – Sept 2013
Gut microbiota, probiotics, and vitamin D: Interrelated exposures influencing allergy, asthma, and obesity? file, not web page Jan 2011
Probiotics reduced weight gain in mice for many weeks (proof of concept) – June 2014
Does Less Sun mean More Disease short introductory video - in 10 languages
Proof that Vitamin D Works 47 diseases proven to be prevented or treated (as of July 2014)
Gut Microbiota: The Neglected Endocrine Organ (vitamin D not mentioned) – July 2014 has the following
- Germ-Free mice getting microbiota from obese mice become obese
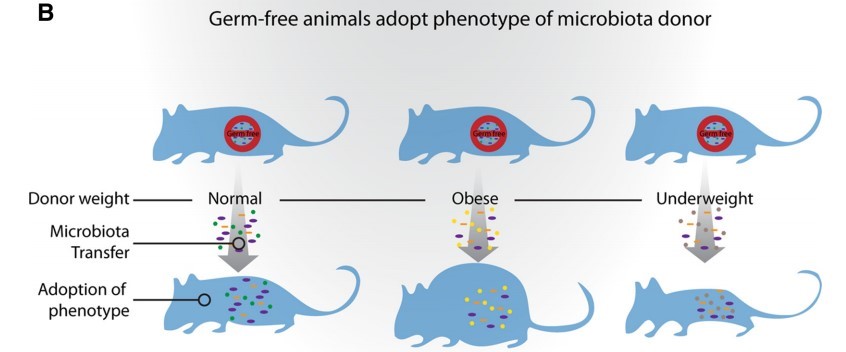
- Low-level antibiotics causes weight gain in mice (and most mammals) – Aug 2014 excellent -many charts, including the following
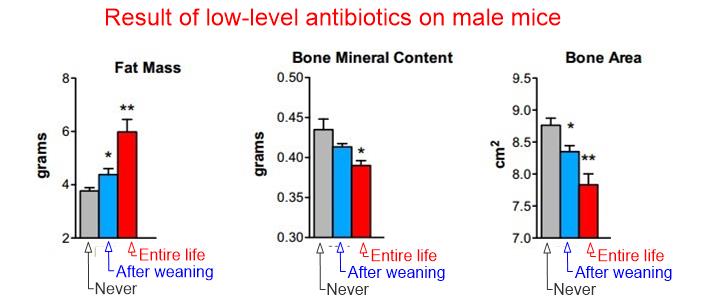
See also web
- Antibiotic Use for Farm Animals a Wiki
- The majority of drugs are fed to animals to promote their growth in factory farms.
- Antibiotic use in livestock WikiPedia
- Antimicrobials (including antibiotics and antifungals) and other drugs are used by veterinarians and livestock owners to increase the size of livestock, poultry, and other farmed animals.
- In 1950, a group of United States scientists found that adding antibiotics to animal feed increases the growth rate of livestock.
- By 2001 this practice had grown so much that a report by the Union of Concerned Scientists found that nearly 90% of the total use of antimicrobials in the United States was for non-therapeutic purposes in agricultural production.
- US - . in 2011 80% of antibiotics went to livestock production
Antibiotic resistance WikiPedia
Alliance for the Prudent Use of Antibiotics Wikipedia Formed 1981
Overuse of antibiotics is disrupting our microbiome NYT via Globe and Mail - the article which caused me to buy the book
Gut microBiota For Health - THE PLACE FOR SCIENTIFIC DEBATE a huge wealth of information
- Book mentioned: MICROBIOTA 2014 WORLD CONGRESS, October 2014, Paris
- 📄 Download the Program with highlights by VitaminDWiki.
- 📄 Download the Posters with highlighs by VitaminDWiki. with 1 poster on Vitamin D
- Mentioned: THE GUT, ITS MICROBES AND HEALTH CONFERENCE, October 8-9 2014 ,Singapore
- 📄 Summary.
- 📄 Newsletter overview of the conference.
Primal Bugs: The Hunter Gatherer Microbiome Primal Docs April 2014, excellent science
Resistant “Nightmare Bacteria” Increase Five-Fold in Southeastern U.S. Wired July 2014
- CRE detection was 0.26 cases per 100,000 patient days in 2008; in 2012, it was 1.4 per 100,000 patient-days
Technology will soon permit modeling human organ/tissue reactions to drugs - but NOT reaction of the bionome
Tonsillectomies May Trigger Weight Gain In Kids July 2014 - no mention of antibiotics used with Tonsillectomies
- Kids' weight rose over 6 % within 18 months of their surgery (and associated antibiotics)
- Mind-altering microbes: how the microbiome affects brain and behavior: Elaine Hsiao at TEDxCaltec Feb 2013
- Weight of brain = 3 lbs, weight of gut microbes = 4-6 lbs
- Antibiotics sprayed on ORGANIC apples, pears, blueberries, etc Nov 2014
- Apples which do not need antibiotics include: Jonafree, Cameo, Melrose, Empire, Red Delicious, Honeycrisp, Jonagold, Liberty, McIntosh, and Winesap
- Many organic vegetables also get low level of antibiotics from manure of animals raised with antibiotics
- Antibiotics in Meat - Scientific American
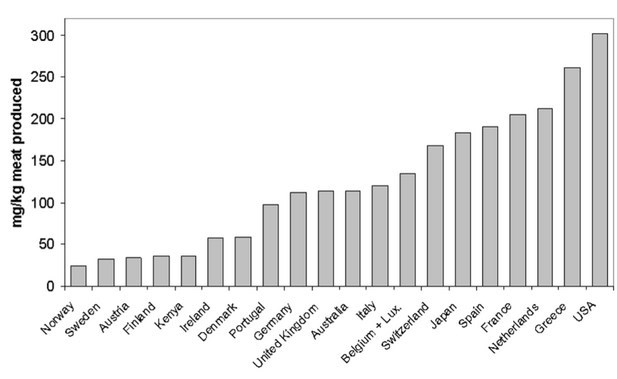
- A Dearth in Innovation for Key Drugs NYT July 2014 - which had the following timeline
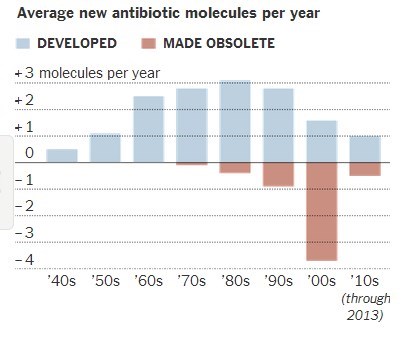
Probiotic and prebiotics treat a variety of diseases Consumer Labs - behind a paywall
The White House 2016 Budget Includes Big Funding for Antibiotic Resistance Wired Jan 2015
- $!.2 Billion mainly focued on new drugs, not decreased use of existing drugs
- Author has written http://superbugthebook.com/ in 2011
Antibiotics infographic Information is Beautiful July 2014 (nothing about vitamin D)
Why infectious bacteria are winning Dec 2015
- Excellent set of animated graphics on antibiotics, nothing about vitamin D
Does the Gut Microbiome Ever Fully Recover From Antibiotics? NYT Dec 2018
- some gut bacteria not recover in 6 monthjs
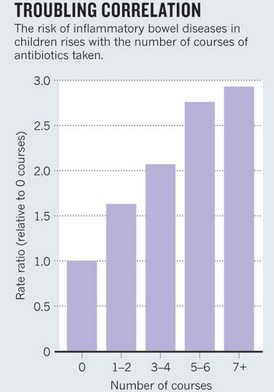
IBD vs number of antibiotics
Mercola on antibiotics
- How Your Microbiome Controls Your Health Mercola May 2014
- includes TedTalk 9 minute video on gut flora Nov 2012
Autism associated with low gut flora (due to antibiotics) – Mercola Oct 2014
Food and Drugmakers Fight Antibiotic Regulation Even As Reports of Human Risks Grow Mercola, March 2016
- lobbing by American Veterinary Medical Association (AVMA) and the Animal Health Institute (AHI) has stopped all legislation to even slow the use of antibiotics
- "Preservation of Antibiotics for Medical Treatment Act (PAMTA), which was supported by over 450 medical and consumer advocate groups7 but blocked with millions of dollars in lobbying money from meat and agricultural interests."
- cephalosporins for food-producing animals INCREASED by 57 % between 2009 through 2014.
- "Dr. Judy Stone recently reported in Forbes that she was seeing disturbing amounts of delirium, confusion and hallucinations in patients taking antibiotics, especially elderly and hospitalized patients"
- "In hospitalized patients, in particular, it’s easy to attribute new confusion to ‘sundowning’ (where elderly get confused at night) or ICU psychosis."
- Note by Henry Lahore - it happened to my 103 year-old father-in-law antibiotics both in hospital and in home
2017 update
- Should We Continue to Feed Antibiotics to Livestock? Scientific American Feb 2015
- "Currently 80 percent of all antibiotics sold in the U.S. are given to poultry and livestock"
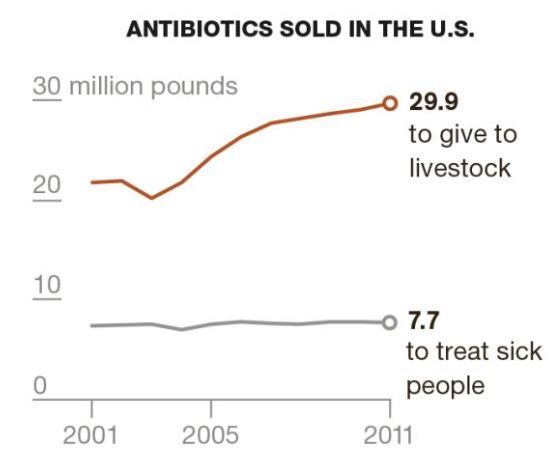
- We Will Miss Antibiotics When They’re Gone NYT Jan 2017
- No mention that only 20% of all antibiotics are actually given to humans in the US
- Talks about trying to produce even more new antibiotics.
- Currently 23,000 people a year in the US die of bacterial infection which current antibiotics cannot treat
"You must finish your course of antibiotics" - that dogma was based on ZERO studies - July 2017
The concept of finishing a course of antibiotics was based on a single person in 1941.
The British Medical Journal (July 2017) describes the origin of the myth and its consequences
The medical community went from undocumented fear of undertreatment to documented harm from overtreatment
It is OK to stop taking the antibiotics once you feel well.
📄 Download the PDF from VitaminDWiki
Big Chicken- antibiotics book - Sept 2017
Wired Mag Sept 2017
"THESE DAYS, THE only thing more American than apple pie is eating an animal raised on antibiotics. Eighty percent of antibiotics sold in the US go not to human patients, but to the nation’s plate-bound pigs, cows, turkeys, and chickens"
Videos - problems with antibiotics
Ramanan Laxminarayan: The coming crisis in antibioticsTedMed Sept 2014 - very good
What causes antibiotic resistance? - Kevin Wu TedEd Aug 2014
Statins were first developed as antibiotics
- The anti-bacterial effect of statins Dr. Grimes - 2018
- Statins were developed in the 1970's as antibacterials
- They found a far larger market in the reduction of Cholesterol - used daily by many instead of infrequently by a few
A historical perspective on the discovery of statins 2010 free PDF online
Martin Blaser news as of July 2019
- Rutgers Names New Director for Center for Advanced Biotechnology and Medicine Dec 2018
- "Blaser also will be the Henry Rutgers Chair of the Human Microbiome and professor of medicine and microbiology at the Rutgers Robert Wood Johnson Medical School. Currently, he serves as the Muriel and George Singer Professor of Medicine, professor of Microbiology and director of the Human Microbiome Program at New York University School of Medicine."
- "In addition to holding 28 U.S. patents related to his research, he has authored more than 580 original articles, with more than 100,000 citations in the scientific literature. "
- Amazon Kindle book $10
Conference of 350 people made great progress on lowering use of antibiotics - Sept 2019
Wait, There’s Hope! Here’s How Humans Might Save Antibiotics
CDC sponsored AMR Challenge in New York City
