Irritable Bowel Syndrome and Vitamin D - many studies
18+ VitaminDWiki pages with IBS etc. in the title
This list is automatically updated
{LIST()}
IBS helped in many ways by Vitamin D (better if had used gut-friendly forms) – meta-analysis Jan 2025
Impact of vitamin D supplementation on symptom severity and quality of life in patients with irritable bowel syndrome: A meta-analysis
Shuang Qi 1, Meng Zhao 2, Yinuo Sun 2, Sunaina Boro 3, Bhawna Arora 4, Sanjay Rastogi 5
Adv Clin Exp Med. 2025 Jan 24. doi: 10.17219/acem/191463
Background: Vitamin D supplementation could offer irritable bowel syndrome (IBS) patients significant improvements in terms of symptom severity and overall quality of life (QoL). Yet, the potential benefits and risks associated with vitamin D supplementation still require additional investigation.
Objectives: We aimed to evaluate the impact of vitamin D supplementation on IBS using a systematic review and meta-analysis.
Material and methods: A comprehensive search was carried out utilizing 4 electronic databases (PubMed, Embase, Scopus, and Cochrane Library) to identify articles published in English-language peer-reviewed journals. The odds ratios (ORs), risk ratios (RRs) and mean differences (MDs), along with their respective 95% confidence intervals (95% CIs), were computed. Heterogeneity was evaluated using the appropriate p-value and Cochrane Q and I2 statistics. For the analysis, RevMan 5.3 was utilized.
Results: Nine randomized controlled trials involving a total of 780 participants were included in this study. Vitamin D supplementation, in adolescents and young adults with IBS, improves the IBS symptoms severity score, QoL and serum 25(OH)D levels compared to controls.
We obtained an
OR of 2.34 (95% CI: 1.56-3.50) for change in the IBS severity scoring system (IBS-SSS),
OR = 2.51 (95% CI: 1.71-3.70) for change in QoL,
low risk of any adverse events (RR 0.49 (95% CI: 0.35-0.69)), and
substantial changes in serum 25(OH)D level (MD = 11.29 (95% CI: 7.13-15.45)).
Results were statistically significant (p < 0.05).
Conclusion: Vitamin D supplementation could lead to better IBS management with a low risk of adverse events.
📄 Download the PDF from VitaminDWiki
Role of in vitamin D in irritable bowel syndrome - April 2023
World J Clin Cases. 2023 Apr 26; 11(12): 2677–2683. doi: 10.12998/wjcc.v11.i12.2677
Xiao-Lan Yu, Qi-Qi Wu, Lian-Ping He, and Yong-Feng Zheng
Irritable bowel syndrome (IBS) is a common chronic functional gastrointestinal disorder affecting 10%-22% of adults. Its development is closely related to the gut microbiota, and the inflammatory and immune responses triggered by the gut microbiota can lead to IBS. Vitamin D (VD) effectively treats IBS with fewer side effects by improving gut microbiota, immune regulation, and anti-inflammatory effects. In the future, it is necessary to carry out epidemiological studies on the relationship between VD and IBS, clinical studies on the efficacy of supplementing VD to improve IBS, and animal studies on the mechanism of VD improving IBS. Therefore, this paper discussed the relationship between VD and IBS.
Core Tip: Irritable bowel syndrome (IBS) is a common chronic functional gastrointestinal disorder affecting 10%-22% of adults. Its development is related to the gut microbiota, and the inflammatory and immune responses triggered by the gut microbiota can lead to IBS.
Vitamin D (VD) is effective in treating IBS by
improving gut microbiota,
immune regulation, and
anti-inflammatory effects.
It is necessary to carry out epidemiological studies on the relationship between VD and IBS, clinical studies on the efficacy of supplementing VD to improve IBS, and animal studies on the mechanism of VD improving IBS. This paper discussed the relationship between VD and IBS.
📄 Download the PDF from VitaminDWiki
IBS quality of life improved somewhat when add some standard vitamin D for a short time - meta-analysis Sept 2024
The effects of vitamin D intake and status on symptom severity and quality-of-life in adults with irritable bowel syndrome (IBS): a systematic review and meta-analysis
Crit Rev Food Sci Nutr 2024 Sep 5:1-14. doi: 10.1080/10408398.2024.2400603
Kelly C Cara 1, Salima F Taylor 1, Haya F Alhmly 1 2, Taylor C Wallace 1 3 4
Vitamin D levels did not increase much (small dose, short time, not a gut-friendly form of vitamin D)
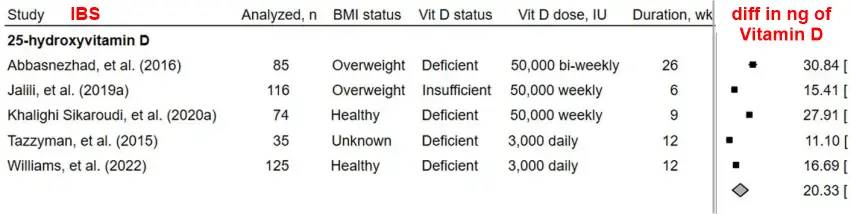
Importance: Many individuals with irritable bowel syndrome (IBS) have insufficient or deficient serum 25-hydroxyvitamin D [25(OH)D] status; however, it is not clear if improved vitamin D nutritional status through higher intake can improve symptom severity and quality of life.
Objective: This systematic review and meta-analysis aimed to identify if changes in vitamin D intake or status affect symptom severity and quality of life in adults with IBS.Data Sources: MEDLINE®, Cochrane Central Register of Controlled Trials, Global Health, EMBASE, and Web-of-Science databases were systematically searched for relevant articles to August 12, 2024, in the English language.Study Selection: Clinical trials, prospective observational studies, and Mendelian randomization (MR) analyses reporting the effect of vitamin D intake or status on IBS-related outcomes were included.Data Extraction and Synthesis: Article review and data extraction were conducted by 2 authors following the PRISMA guidelines. Random effects meta-analyses and the Nutrition Quality Evaluation Strengthening Tools to assess risk of bias were employed for randomized controlled trials.Main Outcome(s) and Measure(s): Primary outcomes included measures of serum 25(OH)D status, symptom severity, and quality of life.
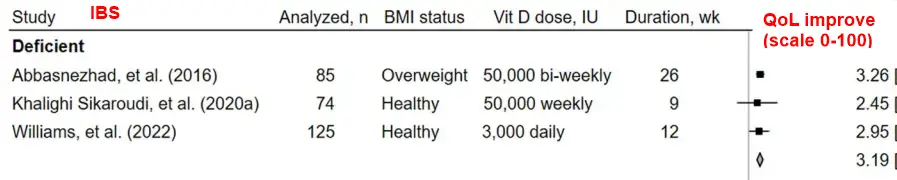
Results: 12 studies from 15 articles were included (n = 7 RCTs; n = 3 single-arm interventions; n = 2 MR). Seven study populations had deficient (<20 ng/mL) and three had insufficient (21-29 ng/mL) baseline serum 25(OH)D status. RCTs measured changes in serum 25(OH)D after 6-26 wks with 3,000 IU daily to 50,000 IU bi-weekly vitamin D dosages. Meta-analyses of low risk-of-bias RCTs revealed increased 25(OH)D levels in groups treated with oral vitamin D compared to placebo (n = 5; Pooled mean difference [95% CI]: 20.33 [1[2.91, 27.74] ng/mL; I2 = 97.9%). Quality of life scores improved significantly in deficient populations (n = 3; 3.19 [2.14, 4.24]; I2 = 0.0%).
Non-significant decreased trends in IBS symptom severity were shown across populations (n = 6: -25.89 [-55.26, 3.48]; I2 = 92.8%).
Conclusion: Moderate level evidence indicate vitamin D supplementation may improve status in adults with IBS and quality of life in those with deficient status at baseline.
📄 Download the PDF from VitaminDWiki
Expect far more QoL improvment if had used gut-friendly Vitamin D - with larger doses and for longer duration
Overview Gut and vitamin D contains gut-friendly information
{include}
VitaminDWiki - Vitamin D interactions with poor gut (Celiac, IBD, and Bariatric surgery) – several studies
VitaminDWiki – Overview Gut and vitamin D has
{include}
VitaminDWiki – Gut category listing contains
{include}
18,700 items in Google Scholar search for VITAMIN D and IBS - includes 6+ meta-analyses
Google Scholar Jan 2025
A Systematic Review and Meta-Analysis of Vitamin D Intakes and Status in Adults With Irritable Bowel Syndrome - July 2024 FREE PDF
The Role of the Gastrointestinal Microbiome and Vitamin D Intake in Inflammatory Bowel Disease - June 2024 FREE PDF
Vitamin D3 And Irritable Bowel Syndrome: Review - June 2024 FREE PDF
Role of in vitamin D in irritable bowel syndrome - April 2023 FREE PDF
Vitamin D improves irritable bowel syndrome symptoms: A meta-analysis - June 2023 FREE PDF
A systematic review and meta-analysis of diet and nutrient intake in adults with irritable bowel syndrome - Oct 2023 FREE PDF
Vitamin D Deficiency (VDD) and Benefits of Supplementation in Veterans with IBS-D - Aug 2023 FREE PDF
Vitamin D supplementation for irritable bowel syndrome: A systematic review and meta-analysis - April 2022 https://doi.org/10.1111/jgh.15852 📄 Download the PDF from VitaminDWiki
The Effect of Vitamin D Supplementation on the Severity of Symptoms and the Quality of Life in Irritable Bowel Syndrome Patients: A Systematic Review and Meta-Analysis of Randomized Controlled Trials - June 2022 https://doi.org/10.3390/nu14132618 📄 Download the PDF from VitaminDWiki
Asked Chat-GPT to compare IBS with IBD
Irritable Bowel Syndrome ( IBS ) and Inflammatory Bowel Disease ( IBD ) are both chronic conditions that affect the digestive system, but they are distinct in their underlying causes, symptoms, and treatments. Here’s a comparison:
Nature of the Condition:
IBS : It is a functional disorder, which means the symptoms are not associated with any visible signs of damage or disease in the digestive tract. It affects how the bowel functions.
IBD : It is an autoimmune disease that involves chronic inflammation of the digestive tract.
There is visible inflammation and damage to the digestive tract.
Common Forms:
IBS : It doesn't have different forms but can be classified based on the predominant symptom
( IBS-D for diarrhea predominant, IBS-C for constipation predominant, IBS-M for mixed).
IBD : Common forms are Crohn's disease and ulcerative colitis .
Symptoms:
IBS : Abdominal pain, bloating, gas, diarrhea, constipation, mucus in the stool. The pain is often relieved by a bowel movement.
IBD : Abdominal pain, cramping, diarrhea, weight loss, fatigue, reduced appetite, blood in the stool, joint pain, and fevers.
Cause:
IBS : The exact cause is not known but it is thought to be related to a combination of abnormal gastrointestinal tract movements, increased sensitivity to pain, and possibly an imbalance of gut bacteria.
IBD : It is believed to be caused by an abnormal immune response, where the immune system attacks the cells of the digestive tract. Genetics, environmental factors, and an imbalance of gut bacteria are also thought to play a role.
Diagnosis:
IBS : Usually diagnosed based on symptoms and exclusion of other diseases. There are no specific laboratory tests to diagnose IBS .
IBD : Can be diagnosed through blood tests, stool tests, endoscopy, and imaging studies which show inflammation and damage in the digestive tract.
Treatment:
IBS : Treatment focuses on relieving symptoms. This may include changes in diet, medications to treat diarrhea or constipation, and stress reduction.
IBD : Treatment aims to reduce inflammation. This often involves medications such as anti-inflammatory drugs, immune system suppressors, and sometimes surgery to remove damaged portions of the digestive tract.
Complications:
IBS : It generally doesn’t cause complications but can significantly impact quality of life.
IBD : Can lead to serious complications such as strictures, abscesses, malnutrition, and increased risk of colon cancer.
Prevalence:
IBS : Is more common compared to IBD .
IBD : Less common but tends to be more severe.
It's important to note that although they have similarities in symptoms, IBS and IBD are fundamentally different. Proper diagnosis and management are crucial for both conditions. Always consult a healthcare provider for advice and information regarding diagnosis and treatment.
