Chronic Hives treated by Vitamin D - many studies
Chronic Urticaria treated by Vitamin D: 50K or 60K weekly - review July 2025
📄 Download the PDF from VitaminDWiki
Hives (Urticaria) 7X more likely if vitamin D deficient; supplementation helps – meta-analysis April 2021
Hives treated by 28,000 IU of Vitamin D weekly – RCT Aug 2020
The effect of vitamin D add-on therapy on the improvement of quality of life and clinical symptoms of patients with chronic spontaneous urticaria
📄 Download the PDF from VitaminDWiki
Hives treated by 60,000 IU of Vitamin D every two weeks – RCT May 2020
Effect of vitamin D supplementation on clinical outcome and biochemical profile in South Indian population with vitamin D-deficient chronic urticarial – A randomized, double-blind placebo-controlled trial
Clinica Chimica Acta, Volume 504, May 2020, Pages 1-6, https://doi.org/10.1016/j.cca.2020.01.003
Highlights
Chronic urticaria (CU) is a debilitating inflammatory skin disease.
This study assessed the effect of vitamin D supplementation on outcomes in CU.
A decrease in UAS7 and medication usage was seen in the intervention group, compared with placebo.
Vitamin D supplementation led to decreased systemic inflammation, hence improving disease course and quality of life in CU.
Background
Chronic urticaria (CU) is a debilitating inflammatory skin disease. Prior studies have shown reduced concentrations of vitamin D in CU and there are limited reports of potential beneficial role for vitamin D supplementation in the treatment of subjects with CU. We assessed the effect of vitamin D supplementation in vitamin D deficient CU patients on the clinical outcome and inflammatory markers in South Indian patients with CU.
Methods
This randomized controlled trial involved 120 vitamin-D-deficient CU patients. Urticaria activity score (UAS7) and autologous plasma skin test (APST) status were assessed in all cases. CU patients were supplemented with vitamin D with a dose of 60,000 IU fortnightly for a period of 12 weeks, and those in the placebo arm received matched placebo. Five milliliters of blood was drawn from all study subjects at baseline and after 12 weeks to assess inflammatory markers.
Results
We observed a significant reduction in UAS7 scores after 12 weeks in the vitamin D treated group in comparison to that of placebo. We also noted a significant reduction of the inflammatory cytokines in the vitamin D-treated group.
Conclusion
Supplementation with vitamin D among patients with vitamin D deficient CU significantly decreases disease severity which is probably mediated through the reduction of systemic inflammation.
📄 Download the PDF from Sci-Hub via VitaminDWiki
Hives treatment augmented by 60,000 IU Vitamin D weekly – RCT June 2015
Hives treatment augmented by 60,000 IU Vitamin D weekly – RCT June 2015, which has the following chart.

Beneficial role for supplemental vitamin D3 treatment in chronic urticaria: a randomized study.
Ann Allergy Asthma Immunol. 2014 Feb 5. pii: S1081-1206(14)00012-X. doi: 10.1016/j.anai.2014.01.010.
Rorie A 1, Goldner WAS 2, Lyden E3, Poole JA 4.
1Pulmonary, Critical Care, Sleep, and Allergy Division, Department of Medicine, College of Medicine, University of Nebraska Medical Center, The Nebraska Medical Center, Omaha, Nebraska.
2Diabetes, Endocrinology and Metabolism Division, Department of Medicine, College of Medicine, University of Nebraska Medical Center, The Nebraska Medical Center, Omaha, Nebraska.
3Department of Biostatistics, College of Public Health; University of Nebraska Medical Center, The Nebraska Medical Center, Omaha, Nebraska.
4Pulmonary, Critical Care, Sleep, and Allergy Division, Department of Medicine, College of Medicine, University of Nebraska Medical Center, The Nebraska Medical Center, Omaha, Nebraska. japoole@unmc.edu.
BACKGROUND: Observational reports have linked vitamin D with chronic urticaria, yet no randomized controlled trial has been conducted.
OBJECTIVE: To determine whether high-dose vitamin D supplementation would decrease Urticaria Symptom Severity (USS) scores and medication burden in patients with chronic urticaria.
METHODS: In a prospective, double-blinded, single-center study, 42 subjects with chronic urticaria were randomized to high (4,000 IU/d) or low (600 IU/d) vitamin D3 supplementation for 12 weeks.
All subjects were provided with a standardized triple-drug therapy (
cetirizine,
ranitidine, and
montelukast)
and a written action plan. Data on USS scores, medication use, blood for 25-hydroxyvitamin D, and safety measurements were collected.
RESULTS: Triple-drug therapy decreased total USS scores by 33% in the first week. There was a further significant decrease (40%) in total USS scores in the high, but not low, vitamin D3 treatment group by week 12. Compared with low treatment, the high treatment group demonstrated a trend (P = .052) toward lower total USS scores at week 12, which was driven by significant decreases in body distribution and the number of days with hives . Beneficial trends for sleep quality and pruritus scores were observed with high vitamin D3. Serum 25-hydroxyvitamin D levels increased with high vitamin D3 supplementation, but there was no correlation between 25-hydroxyvitamin D levels and USS scores. There was no difference in allergy medication use between groups. No adverse events occurred.
CONCLUSION: Add-on therapy with high-dose vitamin D3 (4,000 IU/d) could be considered a safe and potentially beneficial immunomodulator in patients with chronic urticaria.
Vitamin D deficiency 2.5 X more likely with hives - April 2015
Vitamin D deficiency in chronic idiopathic urticaria
Iran J Allergy Asthma Immunol. 2015 Apr;14(2):222-7.
Movahedi M1, Tavakol M2, Hirbod-Mobarakeh A3, Gharagozlou M1, Aghamohammadi A4, Tavakol Z5, Momenzadeh K6, Nabavi M7, Dabbaghzade A1, Mosallanejad A8, Rezaei N9.
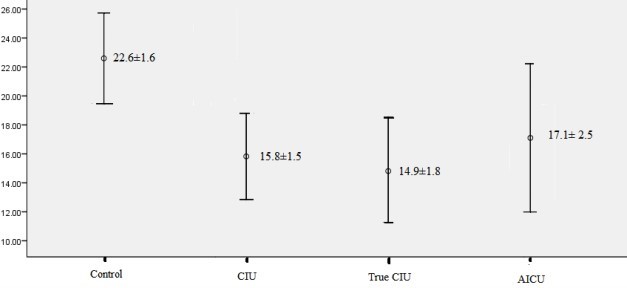
Chronic urticaria is the most common skin disease, characterized by chronic cutaneous lesions which severely debilitate patients in several aspects of their everyday life. Vitamin D is known to exert several actions in the immune system and to influence the function and differentiation of mast cells, central role players in the pathogenesis of chronic idiopathic urticaria. This study was performed to evaluate the relationship between vitamin D levels and susceptibility to chronic idiopathic urticaria. One hundred and fourteen patients with chronic idiopathic urticaria were recruited in this study along with one hundred and eighty-seven sex-matched and age-matched healthy volunteers as the control group. For each patient, the urticaria activity score was calculated, and autologous serum skin test was done. Vitamin D metabolic status was measured in serum as 25 hydroxyvitamin D using the enzyme immunoassay method. Patients with chronic idiopathic urticaria significantly showed lower levels of vitamin D. Vitamin D deficiency was significantly associated with increased susceptibility to chronic idiopathic urticaria. There was a significant positive correlation between vitamin D levels and urticaria activity score. This study showed that patients with chronic idiopathic urticaria had reduced levels of vitamin D, while vitamin D deficiency could increase susceptibility to chronic idiopathic urticaria.
Clipped from results
Patients with CIU and particularly with true CIU, significantly showed lower levels of 25 (OH)D in
comparison with the control group (p=0.005) (Figure 1). However, considering AICU patients separately,
there were no significant differences in vitamin D levels between them and the control group (p=0.11). Vitamin
D deficiency was significantly associated with increased susceptibility to CIU (p=0.001). Individuals
with vitamin D deficiency showed a 2.4-fold (95%CI: 1.4-4) risk of having CIU. In addition, vitamin D
deficiency significantly increased susceptibility to true CIU (p=0.001, OR=2.7 , 95%CI: 1.4-5.1). However,
a slightly significant difference was detected between the controls and the AICU patients regarding vitamin D
deficiency (p=0.048, OR=2.04, 95%CI: 0.99-4.2)(Table 2).
📄 Download the PDF from VitaminDWiki
Chronic Urticaria helped by 300,000 IU of vitamin D monthly Aug 2015
Does the replacement of vitamin D reduce the symptom scores and improve the quality of life in patients with chronic urticaria?
J Dermatolog Treat. 2015 Aug 21:1-19.
Topal IO1, Kocaturk Goncu OE, Gungor S, Durmuscan M, Sucu V, Yıldırmak S.
BACKGROUND:
Vitamin D plays a key role in the immune responses generated by lymphocytes and antigen-presenting cells. Decreased vitamin 25-hydroxyvitamin D (25(OH)D) levels have been implicated in several allergic disorders, and the association between 25(OH)D levels and chronic urticaria (CU) symptom scores has been in a few studies. This study was performed to assess the effects of vitamin D supplementation on the symptoms and quality of life scores in chronic spontaneous urticaria and on vitamin D levels in CSU patients in comparison with controls.
PATIENTS AND METHODS:
Fifty-eight CSU patients and forty-five controls were included in the study. The patients were divided into two groups according to the severity of the disease; mild/moderate and severe urticaria. Serum 25-hydroxyvitamin D (25(OH)D) concentrations were measured in the serum of CSU patients and compared with the control groups. In patients with 25(OH)D concentrations lower than 30 µg/L, 300.000 IU/month of vitamin D3 supplementation was added to standard therapy. The clinical improvement was evaluated after 3 months with urticaria activity score (UAS4) and Chronic Urticaria Quality of Life Questionnaire (CU-Q2oL).
RESULTS:
Serum 25(OH)D concentration was significantly lower in the CSU group compared to healthy subjects (p<0.001). The prevalence of vitamin D deficiency (< 20 (µg/L) and insufficiency (< 30 µg/L) was significantly higher in CSU patients than in control groups. In addition, 25(OH)D concentrations were significantly lower in both mild-moderate and severe CSU patients than those of the controls (P=0.011 and p<0.001, respectively). Ninety-eight percent of patients (25(OH)D < 30 µg/L) were treated with vitamin D3 (300.000 IU/month-1) supplementation, and after 12 weeks, these patients showed significant improvements in UAS4 and CU-Q2oL scores.
CONCLUSION:
This study supports the contributing and beneficial effects of vitamin D in the treatment of chronic urticaria. Replacement of vitamin D may provide improvement in both the severity of symptoms and quality of life scores in these patients.
📄 Download the PDF from VitaminDWiki
Chronic Urticaria alternative treatments include vitamin D - March 2023
THE ROLE OF ADJUVANT THERAPY IN THE MANAGEMENT OF CHRONIC URTICARIA
Review Actas Dermosifiliogr . 2023 Mar 3;S0001-7310(23)00171-0. doi: 10.1016/j.ad.2023.02.015
W Keumala Budianti 1, S Mahri 1, D Almira 2
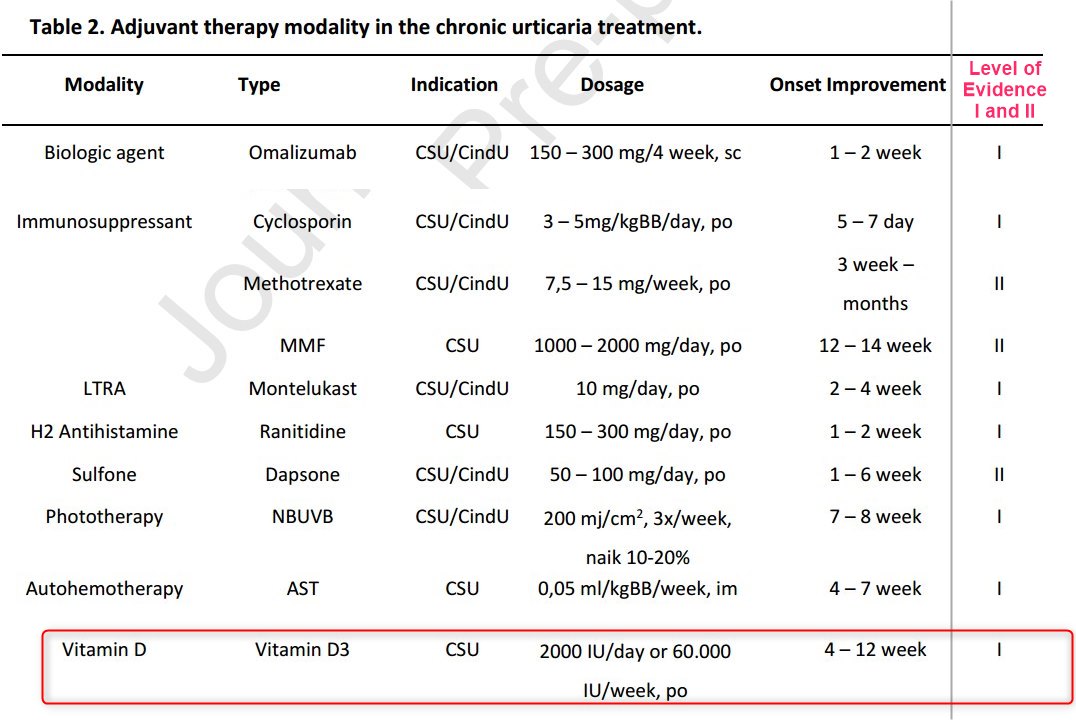
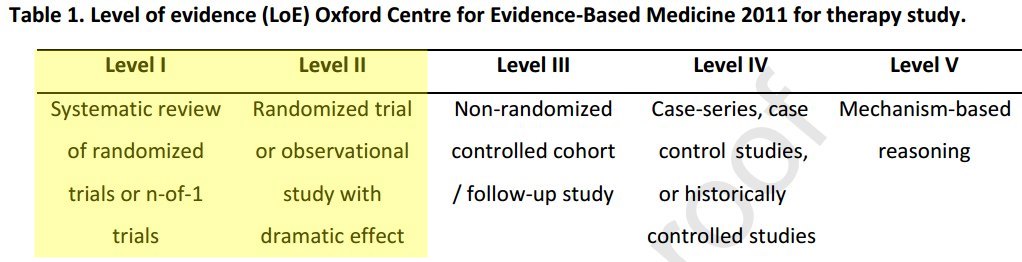
Levels of Evidence

Recent guideline on the management of urticaria recommends second-generation H1-antihistamine as the first-line therapy, with dose increases of up to fourfold if inadequately controlled. However, the treatment of chronic spontaneous urticaria (CSU) is often disappointing, so additional adjuvant therapies are needed to increase the effectiveness of first-line therapy, especially in patients who are refractory to the increase of antihistamine doses. Recent studies recommend various adjuvant therapy modalities for CSU, such as biological agents, immunosuppressants, leukotriene receptor antagonists, H2-antihistamine, sulfones, autologous serum therapy, phototherapy, vitamin D , antioxidants, and probiotics. This literature review was made to determine the effectiveness of various adjuvant therapies in managing CSU.
📄 Download the PDF from VitaminDWiki
CIU = chronic idiopathic urticaria
4+ VitaminDWiki pages have HIVES OR URTICARIA in the title
The list is automatically updated
{LIST()}
See also web
- Vitamin D Blog: Help for Hives? MedPageToday
- ‘’ In the first week, both groups saw a 33% decrease in symptoms. But only the high-dose vitamin D group saw a further reduction in symptoms (40%) by the end of the study.’’
- High dose = 4,000 IU vitamin D daily
- UNMC study: Vitamin D provides relief for those with chronic hives Press Release
- “It was not a cure, but it showed benefits when added to anti-allergy medications. Patients taking the higher dose had less severe hives — they didn’t have as many hives and had a decrease in the number of days a week they had hives.
- In the study, patients had suffered from five to 20 years with severe hives . Some had been on therapy, and others none.
