Early Puberty if low vitamin D - many studies
Note: Vitamin D levels have been crashing in the past 40 years AND the age of puberty has also been dropping around the world
Early puberty in boys 3.9 X more likely if less than 30 ng of Vitamin D - Aug 2025
Association between vitamin D and central precocious puberty in children: Threshold effects and mediation mechanisms based on LC-MS/MS quantitation
Journal of Endocrinological Investigation 10.1007/s40618-025-02695-1 PDF behind $40 paywall
Juan Le, Wen Dai, Rui Peng & Shaoting Wang
Purpose
To investigate the association between serum 25-hydroxyvitamin D [25(OH)D] levels and central precocious puberty (CPP) in children, with emphasis on sex-specific threshold effects and mediation pathways.
Methods
This cross-sectional study enrolled 494 CPP patients (female: 413; male: 81) and 2,259 age-matched healthy controls who underwent liquid chromatography-tandem mass spectrometry (LC-MS/MS) based 25(OH)D quantification, Tanner-Whitehouse 3 bone age assessment, and hormonal profiling. Dose-response relationships were analyzed via restricted cubic splines (RCS), and causal mediation analysis with 1,000 bootstrap resamples were quantified using structural equation models.
Results
CPP patients exhibited significantly lower 25(OH)D levels than controls (median (IQR): females, 20.00 (14.00–24.20) vs. 23.40 (18.10–29.22) ng/mL, P < 0.001; males, 21.60 (16.00–27.10) vs. 23.30 (18.30–28.83) ng/mL, P = 0.033), with higher deficiency rates (females: 49.6% vs. 33.0%; males: 43.2% vs. 32.8%). RCS analysis revealed inverse 25(OH)D-CPP associations, with threshold concentrations at 35.4 ng/mL (females) and 19.5 ng/mL (males). Each 1 ng/mL increment in serum 25(OH)D was associated with 3.6% reduced risk of advanced pubic hair maturation (adjusted OR = 0.964, P = 0.009).
Sex-stratified logistic regression showed elevated CPP risks in vitamin D-insufficient/deficient groups versus sufficient counterparts:
females (OR = 2.13, P = 0.037; OR = 2.26, P = 0.030) and
males (OR = 3.89 , P = 0.059; OR = 4.71, P = 0.034).
Mediation analysis identified bone age acceleration (64.6% mediation) and gonadotropin activation (14.6%) dominated pathways in females.
Conclusion
Vitamin D demonstrated sex-dimorphic associations with CPP risk, requiring higher protective thresholds in females. Bone age acceleration and gonadotropin activation emerged as primary mediators in females. These findings advocated sex-specific vitamin D supplementation strategies for CPP prevention.
Early puberty occurs 1.53 X more often if low vitamin D – meta-analysis Dec 2023
An updated meta-analysis of the relationship between vitamin D levels and precocious puberty
Front Endocrinol (Lausanne) . 2023 Dec 5:14: doi: 10.3389/fendo.2023.1298374
Hong Cheng # 1, Dan Chen # 2, Hui Gao 3
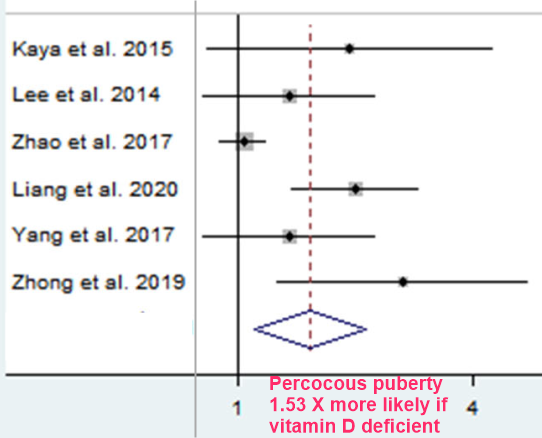
Background: Some studies have investigated the association between vitamin D levels and precocious puberty (PP) but with limited sample sizes and inconsistent conclusions across studies.
Methods: Until July 2022, a comprehensive electronic search of works of literature was conducted in MEDLINE, Web of Science, and CNKI (Chinese National Knowledge Infrastructure). A systematic review and meta-analysis of 15 case-control studies with 2145 cases and 2063 controls was conducted to explore the relationship between vitamin D and PP. Stratified analyses by year of publication, country, diagnosis category of PP, child's sex, and methods of 25(OH)D test were conducted.
Results: There was a negative correlation between 25(OH)D concentrations and PP in all study populations (SMD = -1.046, 95%CI = -1.366, -0.726). The pooled SMD remained significant in Chinese studies (SMD = -1.113, 95%CI = -0.486, -0.741), studies published before or after 2018 (SMD = -0.9832 and -1.185, 95%CI = -2.044, -1.133 and -1.755, -0.726), studies with female children (SMD = -1.114, 95%CI = -1.446, -0.781), and studies using electrochemiluminescence to detect 25(OH)D (SMD = -0.999, 95%CI = -1.467, -0.531). Vitamin D deficiency also increased the risk of PP ( OR = 1.531 , 95%CI = 1.098, 2.134). Unfortunately, heterogeneity was high in all analyses, and there was some publication bias.
Conclusion: This systematic review and meta-analysis demonstrated an association between vitamin D and precocious puberty. We recommend more high-quality studies, especially prospective cohort studies with big sample sizes or some randomized controlled intervention trials, to validate the reliability of the results.
📄 Download the PDF from VitaminDWiki
Early puberty occurs 2.25 X more often if low vitamin D - Meta-analysis May 2023
Does vitamin D have a potential role in precocious puberty? A meta-analysis
Food & Function, Issue 11, 2023
Caihong Wu,a Xingwei Zhang,b Feifei Yan,a Yani Cui,a Yuan Song,c Shoumeng Yan*d and Weiwei Cui ORCID

Background: Precocious puberty, one of the common pediatric endocrine system diseases, has been related to reduced adult height, adverse psychological outcomes and long-term health consequences. Previous findings have found that low levels of vitamin D appear to be associated with the characteristics of precocious puberty such as early menarche. However, the effect of vitamin D on precocious puberty remains controversial.
Methods: The published literature was searched from PubMed, Web of Science, Cochrane Library, MEDLINE, EMBASE, CNKI, Wan Fang and VIP databases up to October 2022. A randomized effect model was used to perform a meta-analysis to evaluate differences in vitamin D concentration between precocious puberty subjects and normal subjects, the risk of precocious puberty in subjects with low vitamin D levels, and the effect of supplementation of vitamin D on subjects with precocious puberty on medication.
Results: Our study found that precocious puberty subjects had lower serum vitamin D levels than the normal population (standardized mean difference (SMD) = −1.16 ng ml−1 and 95% confidence interval (CI) = −1.41 and −0.91 ng ml−1). Meanwhile, the lower level of vitamin D was associated with the risk of precocious puberty (odd ratio (OR) = 2.25 and 95% CI = 1.66 and 3.04). Moreover, compared with gonadotropin-releasing hormone analogue (GnRHa) intervention alone, subjects receiving GnRHa + vitamin D intervention had significantly lower luteinizing hormone (LH), follicle-stimulating hormone (FSH), and estradiol levels and bone age, and higher predicted adult height (PAH).
Conclusions: Vitamin D may have a potential role in precocious puberty and more data from large clinical trials are needed to confirm the findings.
idiopathic central precocious puberty in girls 7 X more likely if low vitamin D - July 2023
Serum 25-hydroxyvitamin D levels and the risk of idiopathic central precocious puberty in girls
Clinics (Sao Paulo) . 2023 Jul 4;78:100244. doi: 10.1016/j.clinsp.2023.100244
Dong-Mei Gan 1, Jie Fang 2, Ping-Ping Zhang 1, Yu-Dan Zhao 1, Ya-Nan Xu 1
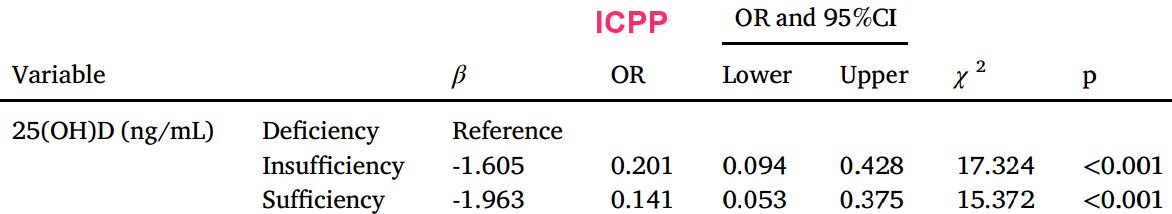
Introduction: Prior studies have found inconsistent results regarding the relationship between vitamin D status and Idiopathic Central Precocious Puberty (ICPP).
Objective: To assess the role of serum 25-hydroxyvitamin D (25 [OH]D) levels in ICPP development.
Method: The authors retrospectively collected data from 221 girls with ICPP and 144 healthy girls between January 2017 and December 2019 . The participants' serum 25(OH)D levels were measured using an automatic chemiluminescence method, and the association between serum 25(OH)D levels and the risk of ICPP was assessed using multivariate logistic regression analysis. Odds Ratios (OR) with 95% Confidence Intervals (95% CI) were calculated as effect estimates.
Results: Serum 25(OH)D levels in the ICPP group were significantly lower than those in healthy controls (p < 0.001). Multivariate analysis indicated that girls with insufficient vitamin D levels (OR = 0.201; 95% CI 0.094-0.428; p < 0.001) and sufficient vitamin D levels ( OR = 0.141 ; 95% CI 0.053-0.375; p < 0.001) both had a lower risk of ICPP than girls with vitamin D deficiency. Moreover, the authors found that the height (p = 0.014), weight (p = 0.014), breast stage (p = 0.010), mother's height (p < 0.001), and luteinizing hormone/follicle-stimulating hormone ratio (p = 0.010) in girls with ICPP could be associated with levels of vitamin D.
Conclusion: This study found that a low serum 25(OH)D level is an independent risk factor for ICPP, and several characteristics of girls with ICPP could be affected by their vitamin D status.
📄 Download the PDF from VitaminDWiki
5X increase in Precocious Puberty during early COVID lockdown- Sept 2022
Analysis of the Incidence and Risk Factors of Precocious Puberty in Girls during the COVID-19 Pandemic
Int J Endocrinol . 2022 Sep 28;2022:9229153. doi: 10.1155/2022/9229153
Dongxia Fu 1 , Tao Li 1 , Yingxian Zhang 1 , Huizhen Wang 1 , Xue Wu 1 , Yongxing Chen 1 , Bingyan Cao 2 , Haiyan Wei 1

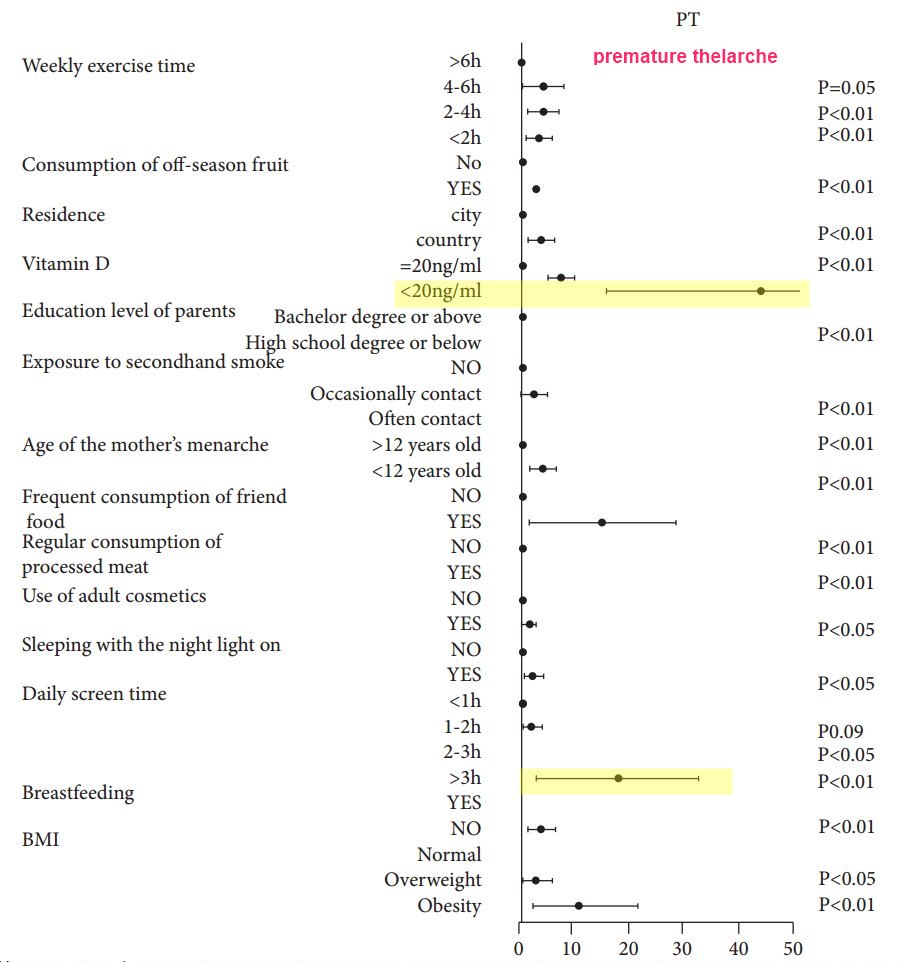
Home quarantine due to the global coronavirus disease 2019 (COVID-19) pandemic has had a significant impact on children. Lifestyle changes have led to an increase in precocious puberty (PP) among girls, and the underlying risk factors for this remain unclear. Thus, we aimed to assess the influence of environmental, genetic, nutritional, and other lifestyle factors on the risk of PP in girls. We evaluated the incidence of new-onset PP in girls during home quarantine for COVID-19 and analyzed the potential risk factors. This was a retrospective questionnaire and medical record-based study involving 22 representative medical units from 13 cities in Henan Province, China. Girls with new-onset PP (central precocious puberty, 58; premature thelarche, 58; age, 5-9 years) between February 2020 and May 2020 were included, along with 124 healthy, age-matched controls. The number of new-onset PP cases reported during the study period was compared with that reported between February and May in 2018 and 2019. Patients' families completed a questionnaire to assess potential risk factors.
There was a 5.01 - and 3.14-fold increase in the number of new-onset PP cases from 2018 to 2020 and from 2019 to 2020, respectively; the differences were statistically significant (p < 0.01).
High-risk factors for PP included
longer time spent using electronic devices,
decreased exercise time,
higher body mass index,
vitamin D deficiency,
young age (<12 years)
of mother during menarche,
consumption of fried food and processed meat,
residence in rural areas, and
consumption of off-season fruits.
Thus, we found that lifestyle changes caused due to the COVID-19 pandemic led to a significant increase in PP in girls. Management of the risk factors identified in this study may help in PP prevention.
📄 Download the PDF from VitaminDWiki
Early puberty during pandemic (perhaps just low vitamin D) - Sept 2022
NYT article wondering why earlier and earlier puberty over the past 50 years - May 2022
Puberty Starts Earlier Than It Used To (unaware of Vitamin D) - May 2022
NYT: Girls of Color Are Getting Their Periods Earlier. No One Quite Knows Why. June 2024
Menarche and Time to Cycle Regularity Among Individuals Born Between 1950 and 2005 in the US May 2024
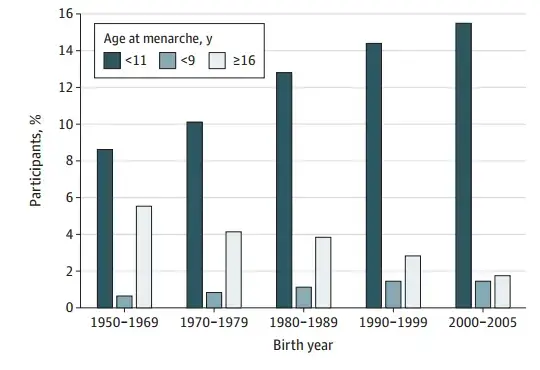
📄 Download the PDF from VitaminDWiki
Early puberty cases among girls surged during pandemic - April 2022
MDEdge no mention of lockdown ==> lower level of vitamin D
"In another study, a Turkish pediatric endocrinology clinic reported 58 cases during the first year of the pandemic, as compared with 66 total cases during the 3 previous years."
"Doctors have tied the current uptick to the stress of the pandemic and lockdowns, including reduced physical activity and increased consumption of unhealthy food, which are things linked to a higher risk of early puberty."
Early puberty 2X more likely if low vitamin D – Meta-analysis Feb 2020
The Association Between Vitamin D Levels and Precocious Puberty: A Meta-Analysis
J Pediatr Endocrinol Metab, 2020 Feb 18, DOI: 10.1515/jpem-2019-0388
Shanshan Liu 1, Xun Zhu 1, Yuanxin Wang 1, Shoumeng Yan 2, Dong Li 3, Weiwei Cui 4
The objective of this short communication was the relationship between vitamin D and precocious puberty (PP). In this study, a comprehensive search of multiple databases was performed to identify studies focused on the association between vitamin D deficiency and PP. Studies that compared serum vitamin D levels between patients with PP and controls were selected for the systematic meta-analysis. The main outcome was the mean difference in serum vitamin D levels between PP and controls. Vitamin D-deficient subjects were more likely to develop PP. Our findings suggest that PP may be linked to vitamin D deficiency. Thus, providing supplements of vitamin D to PP patients may improve their nutritional status and prevent diseases. But, the amount of vitamin D required is uncertain, so it is important to be careful when taking vitamin D supplements.
📄 Download the PDF from Sci-Hub via VitaminDWiki
Early puberty more likely if < 20 ng of Vitamin D - Aug 2018
Vitamin D status and premature adrenarche
Pediatrics International Volume 60, Issue 10, https://doi.org/10.1111/ped.13682
Onur Akın Aysun Bideci Esra Döğer Emine Demet Akbaş Aylin Kilinç Uğurlu Süleyman Tolga Yavuz Şehri Elbeğ Orhun Çamurdan Peyami Cinaz
Background: Vitamin D, an important factor in calcium‐phosphate homeostasis, has recently been suggested to play an important role in the pathogenesis of numerous chronic conditions such as hyperandrogenism. The aim of this study was to investigate the relationship between vitamin D status and premature adrenarche (PA).
Methods
A total of 71 girls with PA and 52 healthy girls, as the control group, were recruited. Axillary and/or pubic hair development before the age of 8 years was defined as PA. Bone age and anthropometric measures including height, weight, and body mass index (BMI) were obtained. 25‐Hydroxyvitamin D (25(OH)D), fasting plasma glucose and insulin were measured. Vitamin D insufficiency was defined as <20 ng/mL.
Results
The PA patients had older bone age, higher BMI standard deviation score, homeostasis model of assessment–insulin resistance (HOMA‐IR), and androgen but lower 25(OH)D than the control group. HOMA‐IR and dehydroepiandrosterone sulfate were also higher in PA patients with vitamin D insufficiency compared with those with normal vitamin D. There was a negative correlation between 25(OH)D and HOMA‐IR.
Conclusion:Low vitamin D is associated with PA; and insulin resistance may be a factor in this association.
Vitamin D deficiency and age at menarche: a prospective study - Oct 2011
Am J Clin Nutr. 2011 Oct;94(4):1020-5. Epub 2011 Aug 10.
Villamor E, Marin C, Mora-Plazas M, Baylin A.
Department of Environmental Health Sciences, University of Michigan School of Public Health, Ann Arbor, MI 48109, USA. villamor@umich.edu
BACKGROUND: Early menarche is a risk factor for cardiometabolic disease and cancer. Latitude, which influences sun exposure, is inversely related to age at menarche.
This association might be related to vitamin D, but to our knowledge it has not been investigated in prospective epidemiologic studies.
OBJECTIVE: We studied the association between vitamin D status and the occurrence of menarche in a prospective study in girls from Bogota, Colombia.
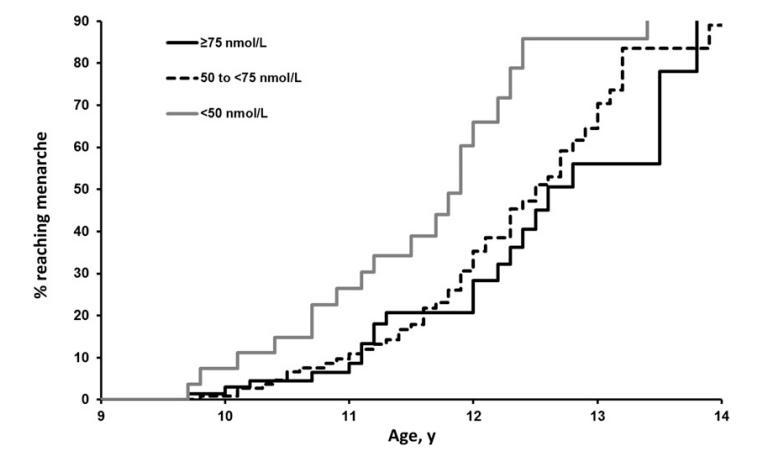
DESIGN: We measured plasma 25-hydroxyvitamin D [25(OH)D] concentrations in a random sample of 242 girls (mean ± SD age: 8.8 ± 1.6 y) and followed them for a median of 30 mo. Girls were asked periodically about the occurrence and date of menarche. Baseline 25(OH)D concentrations were categorized as <50 nmol/L (deficient), ?50 and <75 nmol/L, or ?75 nmol/L (sufficient). The incidence of menarche was compared between groups by using time-to-event analyses.
RESULTS: A total of 57% of girls in the vitamin D-deficient group reached menarche during follow-up compared with 23% of girls in the vitamin D-sufficient group (P-trend = 0.0004). The estimated mean (±SE) ages at menarche in the same groups were 11.8 ± 0.2 y and 12.6 ± 0.2 y, respectively (P = 0.0009). After adjustment for baseline age and BMI-for-age z score in a Cox proportional hazards model, the probability of menarche was twice as high in vitamin D-deficient girls than in girls who were vitamin D-sufficient (HR: 2.05; 95% CI: 1.03, 4.07; P = 0.04). Similar results were obtained in girls aged ?9 y at baseline (HR: 2.39; 95% CI: 1.14, 5.00; P = 0.02).
CONCLUSION: Vitamin D deficiency is associated with earlier menarche.
Approximately 1 year earlier if low level of vitamin D
Figure from PDF
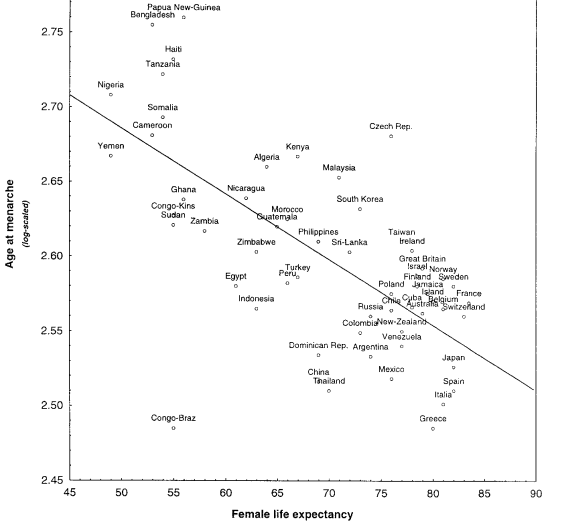
Menarche vs life expectancy
PDF is attached at the bottom of this page
Elsewhere: In 1901, menarche in US and Canada 13.9 or 14 years.
By the 1970's it had declined to 12.5 years
Now, if vitamin D deficient, it is, on average < 12 years
Early puberty increasing in obese and dark skin children (probably lower vitamin D) – Nov 2013
There was no mention of vitamin D in the article
Black girls had the earliest average onset at 8.8 years old, followed by Latino girls (9.3 years) and white and Asian girls (9.7 years).
The onset for white girls was earlier by four months than in a large study 15 years prior.
The new study found that 14 percent of instances of early puberty appeared linked to obesity,
Onset of Breast Development in a Longitudinal Cohort
Pediatrics (doi: 10.1542/peds.2012-3773)) Nov 4, 2013
BACKGROUND AND OBJECTIVES: There is growing evidence of pubertal maturation occurring at earlier ages, with many studies based on cross-sectional observations. This study examined age at onset of breast development (thelarche), and the impact of BMI and race/ethnicity, in the 3 puberty study sites of the Breast Cancer and the Environment Research Program, a prospective cohort of >1200 girls.
METHODS: Girls, 6 to 8 years at enrollment, were followed longitudinally at regular intervals from 2004 to 2011 in 3 geographic areas: the San Francisco Bay Area, Greater Cincinnati, and New York City. Sexual maturity assessment using Tanner staging was conducted by using standardized observation and palpation methods by trained and certified staff. Kaplan-Meier analyses were used to describe age at onset of breast maturation by covariates.
RESULTS: The age at onset of breast stage 2 varied by race/ethnicity, BMI at baseline, and site. Median age at onset of breast stage 2 was 8.8, 9.3, 9.7, and 9.7 years for African American, Hispanic, white non-Hispanic, and Asian participants, respectively. Girls with greater BMI reached breast stage 2 at younger ages. Age-specific and standardized prevalence of breast maturation was contrasted to observations in 2 large cross-sectional studies conducted 10 to 20 years earlier (Pediatric Research in Office Settings and National Health and Nutrition Examination Survey III) and found to have occurred earlier among white, non-Hispanic, but not African American girls.
CONCLUSIONS: We observed the onset of thelarche at younger ages than previously documented, with important differences associated with race/ethnicity and BMI, confirming and extending patterns seen previously. These findings are consistent with temporal changes in BMI.
3X more likely to be vitamin D deficient if early puberty - June 2014
Associations between serum vitamin D levels and precocious puberty in girls,
Ann Pediatr Endocrinol Metab. 2014 Jun;19(2):91-5. doi: 10.6065/apem.2014.19.2.91. Epub 2014 Jun 30.
Lee HS, Kim YJ, Shim YS, Jeong HR, Kwon E, Hwang JS.
Department of Pediatrics, Ajou University Hospital, Ajou University School of Medicine, Suwon, Korea.
PURPOSE: Vitamin D deficiency has been linked to chronic diseases, such as diabetes mellitus, obesity and autoimmune disease.
However, data on the vitamin D status and its association with precocious puberty in girls are limited.
We aimed to investigate the association between serum 25-hydroxyvitamin D (25OHD) and precocious puberty in girls.
METHODS: A total of 60 girls with central precocious puberty (CPP) and 30 control girls were enrolled. Anthropometric measurement and serum level of 25OHD were estimated for all subjects.
RESULTS: There was a significant difference in the mean serum 25OHD concentration between the precocious puberty group and the control group (17.1±4.5 ng/mL vs. 21.2±5.0 ng/mL, P<0.05). Forty-two of the 60 girls with CPP (70%) had vitamin D deficiency (defined as serum 25OHD<20 ng/mL) and 18 (30%) had vitamin D insufficiency. Of the 30 girls in the control group, vitamin D deficiency was seen in 13 subjects (43.3%), 15 subjects (50%) had vitamin D insufficiency, and 2 subjects (6.7%) had sufficient serum vitamin D (defined as serum 25OHD>30 ng/mL). Vitamin D deficient girls had a significantly higher odds ratio (OR, 3.05; 95% CI, 1.22-7.57, P=0.021).
CONCLUSION: These results showed that vitamin D levels may be associated with precocious puberty.
Further studies are required to establish the potential effect of vitamin D status on puberty.
Summary by VitaminDWiki
| precocious puberty | Control | |
| Vitamin D | 17 ng | 21 ng |
| Vitamin D Deficiency < 20 ng | 70% | 43% |
| Vitamin D Insufficiency 20-30 ng | 30% | 50% |
| Vitamin D Sufficiency ? 30 ng | 0% | 6.7% |
📄 Download the PDF from VitaminDWiki
See also VitaminDWiki
Vitamin D deficiency and pregnancy - from preconception to birth Aug 2010
Early puberty in girls 60 percent more likely if less than 32 ng of vitamin D – Aug 2017
International Variability of Ages at Menarche and Menopause April 2001. file - not web page
- Found that the probability that the age of menarche was correlated with latitude was 99.95%
- That is, the international study found that the higher the latitude, the lower the age of menarche
- It is well known that the higher the latitude, the lower the level of vitamin D
Menstruation 10 months earlier if low on vitamin D – Aug 2011
See also web
Boys Now Enter Puberty Younger, Study Suggests, but It’s Unclear Why
- New York Times Oct 2012, no mention of vitamin D
Age is now 6 to 24 months earlier than 40 years ago (12+ reasons for decrease in vitamin D in the past 40 years)
African American boys age 9, Hispanic boys age 10, white boys age 10.5 ? (Having dark skin reduces the vitamin D levels from the sun)
Heaviest boys reached puberty sooner (being overweight reduces the vitamin D level in the body)
Does vitamin D affect timing of menarche? Jan 2013 - rebuttal paper
- The association was not fully explained by differences in body mass index-for-age z-scores.
- The mechanism for the association, if real, has not been elucidated, but could potentially involve vitamin D receptor polymorphisms.
- Early menarche and vitamin D deficiency are both associated with poor health outcomes, and further exploration of their association is important for women's health.
- More Vitamin D intake may delay precocious puberty Times of India, June 2013
- Reporting on ENDO Meeting in the US
- The influence of puberty on vitamin D status in obese children and the possible relation between vitamin D deficiency and insulin resistance Jan 2015
Speculation: Obesity ==> lower Vitamin D ==> early puberty
~~ visitors to this page since it was originally made
Short URL for this page = http://is.gd/vitdpuberty
