Overview Stroke and vitamin D
Summary - strokes, as with many other diseases:
2000+ IU of vitamin D daily will provide some stroke prevention
Increased Magnesium or Omega-3 appear prevent strokes
10,000+ IU of vitamin D daily will provide some treatment and prevention
loading dose of >100,000 IU followed by maintence dose of >5,000 IU daily cost effectively can reduce the impact of a stroke
need larger doses if person is in a high risk group
- examples include elderly, dark skin, live far from equator, obese, avoid the sun, ...
Overview Stroke and vitamin D category has items
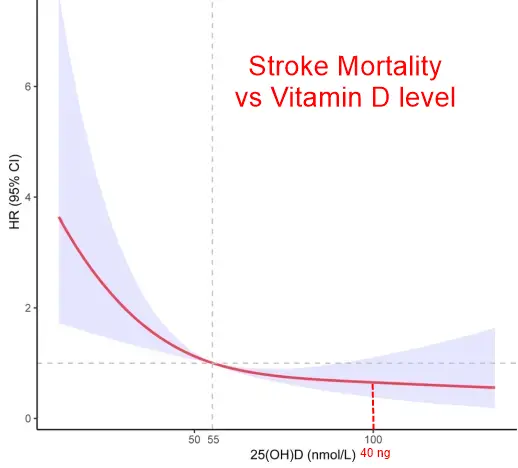
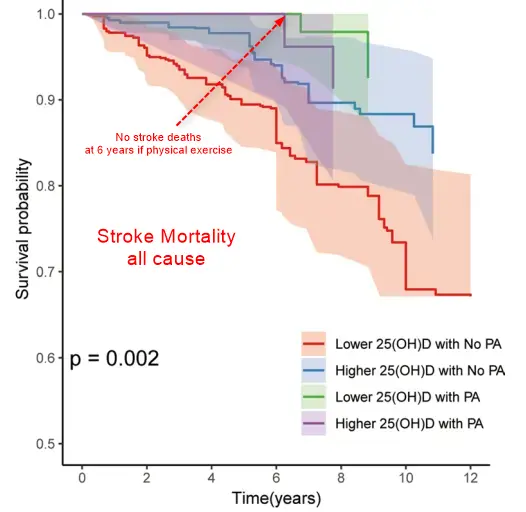
Stroke mortality 2.6 X less if high Vitamin D, 3.5 X less if physical exercise, and 7.5 X less if both - Jan 2025
Combined 25-hydroxyvitamin D concentrations and physical activity on mortality in US stroke survivors: findings from the NHANES
Nutr J . 2025 Jan 13;24(1):5. doi: 10.1186/s12937-025-01076-x.
Junqi Liao # 1 2, Jingyi Chen # 1 2, Huimin Wu 1 2, Qing Zhu 1 2, Xiaogang Tang 1 2, Li Li 1 2, Aimei Zhang 1 2, Peiyi Mo 1 2, Yan Liu 1 2, Xinyi Yang 1 2, Yang Han 3, Zhaoyao Chen 1 2, Wenlei Li 4 5, Yuan Zhu 6 7, Minghua Wu 8 9 10
Background: 25-hydroxyvitamin D [25(OH)D] concentrations and physical activity (PA) are linked and both are associated with changes in mortality. We examined the association of 25(OH)D and PA with all-cause or cause-specific mortality risk in stroke survivors.
Methods: The analysis included 677 stroke survivors from National Health and Nutrition Examination Survey (NHANES) 2007-2008 to 2017-2018. Independent and joint associations of 25(OH)D, PA and mortality among stroke survivors were analyzed using weighted Cox regression.
Results: We identified 133 all-cause deaths [major adverse cardiovascular events (MACE), 34; non-MACE, 79] with a median follow-up of 5.8 years (interquartile, 2.8-8.9 years). In a range of adjusted models, high 25(OH)D was observed with lower all-cause mortality compared to low 25(OH)D (HR, 0.376; 95% CI, 0.233-0.607) and non-MACE (HR, 0.265; 95% CI, 0.143-0.490) mortality was consistently associated. At the same time, compared with no PA, PA was associated with a lower all-cause (HR, 0.280; 95%CI, 0.107-0.733) and non-MACE (HR, 0.266; 95%CI, 0.087-0.810) was associated with a lower risk of death. In addition, pooled analyses showed that stroke survivors with high 25(OH)D and PA had the lowest risk of all-cause death (HR, 0.132; 95%CI, 0.038-0.460) and non-MACE (HR, 0.092; 95%CI, 0.023-0.363), there is an additive interaction between 25(OH)D and PA in non-MACE.
Conclusion: In conclusion, this study found that combining high 25(OH)D levels and PA showed an enhanced protective effect which demonstrated a synergistic effect between them in reducing mortality among stroke survivors. These findings provide new ideas and possibilities for the prevention and treatment of cardiovascular and cerebrovascular diseases, offering a reference for development of clinical practice guidelines in the future.
📄 Download the PDF from VitaminDWiki
Google Scholar had 184,000 hits for Stroke AND Vitamin D as of Oct 2024
A systematic review and meta-analysis of the linkage between low vitamin D and the risk as well as the prognosis of stroke - June 2024 FREE PDF
Association between Vitamin D and Short-Term Functional Outcomes in Acute Ischemic Stroke - Nov 2023 - FREE PDF
A systematic review examining the effect of vitamin D supplementation on functional outcomes post-stroke - May 2023 FREE PDF
The relationship of vitamin D deficiency with severity and outcome of acute stroke - Dec 2021 [FREE PDF](https://doi.org/10.2478/rjim-2021-0013%20)
Low vitamin D levels and the long-term functional outcome of stroke up to 5 years - Sept 2021 📄 PDF attached
Does vitamin D administration play a role in outcome of patients with acute ischemic stroke? A randomized controlled trial - Jan 2021📄 PDF attached
The Evaluation of the Neuroprotective Effect of a Single High-Dose Vitamin D3 in Patients with Moderate Ischemic Stroke - 📄 PDF attached
- 600,000 IU injection
Vitamin D supplementation, cardiac events and stroke: A systematic review and meta-regression analysis - June 2020📄 PDF attached
Vitamin D Supplementation and Post-Stroke Rehabilitation: A Randomized, Double-Blind, Placebo-Controlled Trial - June 2019 📄 PDF attached
Stroke mortality 3X worse among seniors with less than 26 ng of vitamin D – June 2014

See also at VitaminDWiki
Strokes result in many years of disability (Vitamin D can help) GBD – March 2019
Twice as many fatal strokes among whites who were low on vitamin D – Jan 2012
Too much and too little Calcium both increase death after strokes – Jan 2011
0.4 year of the 5 year life penalty for having black skin = fatal stroke
Stroke Meta-analyses
This count and list are automatically updated
{category}
Stroke Interventions
This count and list are automatically updated
{category}
5+ VitaminDWiki Stroke pages have RCT in the title
The list is automatically updated
{LIST()}
Depression lead to Strokes (VitaminDWiki notes that both are related to low vitamin D)
Article about Brigham Women's Hospital Study which was published in Stroke
"women with a history of depression had a 29 percent higher risk of stroke , even after considering other stroke risk factors."
"The study included more than 80,000 female nurses between the ages of 54 to 79 years old from 2000-06 without a prior history of stroke. "
"More than 1000 cases of stroke were documented among the women during the six years."
CLICK HERE for abstract Aug 2011
(VitaminDWiki notices that the principal author has published many other papers on cardiovascular problems and low vitamin D levels. Kathryn M. Rexrode krexrode@partners.org)
See in VitaminDWiki No longer depressed, but risk of stroke is still 1.7X higher (did not consider low vitamin D) – May 2015
Stroke patients with low vitamin D were 10X more likely to become depressed – Aug 2014
Stroke patients with low vitamin D were 10X more likely to become depressed – Aug 2014
Magnesium in water also associated with a reduction in stroke - 2012
100 mg more Magnesium in water associated with 8 percent reduction in stroke – Feb 2012
Independent evidence shows that Vitamin D and Magnesium both reduce strokes.
Expect that they would do well together - perhaps more than 2X the benefit
Excessive IRON increases Stroke incidence and death by about 20% - April 2025
📄 Report by Perplexity AI Deep Research - April 2025
📄 Mercola April "A simple blood test, called a serum ferritin test, can tell you your iron levels. You want your ferritin below 100 ng/mL, and ideally between 35 and 45 ng/mL."
Rusting from the inside - Mercola Video - 11 minutes
- See in VitaminDWiki Overview Iron Supplements and Vitamin D
Stroke 50 % more likely if low vitamin D - Meta-analysis May 2012
25-Hydroxyvitamin D Levels and the Risk of Stroke. A Prospective Study and Meta-analysis
Qi Sun, MD, ScD qisun@hsph.harvard.edu ; An Pan, PhD; Frank B. Hu, MD, PhD; JoAnn E. Manson, MD, DrPH; Kathryn M. Rexrode, MD, MPH
From the Departments of Nutrition (Q.S., A.P., F.B.H.) and Epidemiology (F.B.H., J.E.M.), Harvard School of Public Health, Boston, MA; and the Channing Laboratory (Q.S., F.B.H., J.E.M.) and the Division of Preventive Medicine (J.E.M., K.M.R.), the Department of Medicine, Brigham and Women's Hospital and Harvard Medical School, Boston, MA.
Background and Purpose—Despite evidence suggesting that vitamin D deficiency may lead to elevated cardiovascular disease risk, results regarding the association of 25-hydroxyvitamin D (25[OH]D) levels with stroke risk are inconclusive. We aimed to examine this association in a prospective study in women and to summarize all existing data in a meta-analysis.
Methods—We measured 25(OH)D levels among 464 women who developed ischemic stroke and an equal number of control subjects who were free of stroke through 2006 in the Nurses' Health Study (NHS). We searched MEDLINE and EMBASE for articles published through March 2011 that prospectively evaluated 25(OH)D levels in relation to stroke.
Results—After multivariable adjustment for lifestyle and dietary covariates, lower 25(OH)D levels were associated with an elevated risk of ischemic stroke in the NHS: the OR (95% CI) comparing women in the lowest versus highest tertiles was 1.49 (1.01–2.18; Ptrend=0.04). We found 6 other prospective studies that examined 25(OH)D in relation to stroke outcomes. After pooling our results with these prospective studies that included 1214 stroke cases in total, low 25(OH)D levels were associated with increased risk of developing stroke outcomes in comparison to high levels: the pooled relative risk (95% CI) was 1.52 (1.20–1.85; I2=0.0%, Pheterogeneity=0.63). In 2 studies that explicitly examined ischemic stroke, this association was 1.59 (1.07–2.12; I2=0.0%, Pheterogeneity=0.80).
Conclusions—These data provide evidence that low vitamin D levels are modestly associated with risk of stroke.
Maintaining adequate vitamin D status may lower the risk of stroke in women.
Hypertension (blood pressure) increases incidence of strokes
Overview Hypertension and vitamin D at VitaminDWki
-
- 70% of strokes related to high blood pressure
- "High blood pressure is the single most important controllable stroke risk factor, especially in the elderly."
Strokes occur 25% more often in the Spring - when the vitamin D blood levels are the lowest
Incidence of Stroke and Season of the Year: Evidence of an Association
Am J Epidemiol 2000;152:558–64.
Evidence of seasonal variation in the incidence of stroke is inconsistent. This may be a likely consequence of one or more methodological shortcomings of the studies investigating this issue, including inappropriate analytic models, insufficient length of time, small sample size, and a regional (vs. national) focus. The authors' objective was to ascertain whether an association exists between season of the year and the incidence of stroke by using a methodological approach designed to overcome these limitations.
The authors used a longitudinal study design involving 72,779 veterans hospitalized for stroke at any Veterans Affairs hospital nationally during the years 1986–1995.
These data were analyzed by using time series methods.
There was clear evidence of a seasonal occurrence for stroke in general.
This seasonal effect was found for ischemic stroke, but not for hemorrhagic stroke.
The peak occurrence was in mid-May.
Neither the region (i.e., climate) nor the race of the patient substantially modified the seasonal trend. An explanation for this pattern remains to be determined.
Ischemic Stroke
VitaminDWiki Ischemic Stroke and Vitamin D - many studies
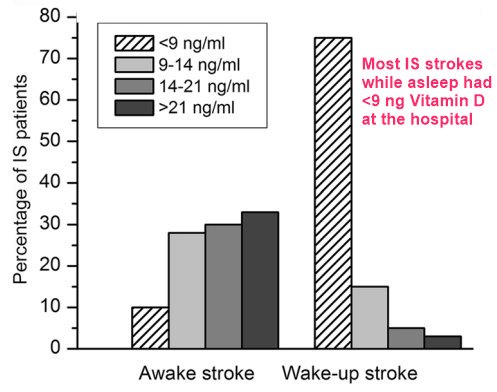
Ischemic Stroke while asleep is associated with <9 ng Vitamin D - June 2022
Surrogate biomarkers of outcome for wake-up ischemic stroke
BMC Neurol . 2022 Jun 9;22(1):215. doi: 10.1186/s12883-022-02740-z.
Pablo Hervella 1 2, María Luz Alonso-Alonso 3, María Pérez-Mato 4, Manuel Rodríguez-Yáñez 5, Susana Arias-Rivas 5, Iria López-Dequidt 5, José M Pumar 3 6, Tomás Sobrino 7, Francisco Campos 8, José Castillo 3, Ramón Iglesias-Rey 9 10
Background: Wake-up ischemic stroke (IS) has been usually excluded from acute stroke therapy options for being outside of the safe treatment window. We identified risk factors, and clinical or molecular biomarkers that could be therapeutic targets for wake-up stroke prevention, thus hopefully leading to a decrease in its mortality and disability in medium to long-term outcome.
Methods: 4251 ischemic stroke (IS) patients from a prospectively registered database were recruited; 3838 (90.3%) had known onset-symptom time, and 413 (9.7%) were wake-up strokes. The main endpoint was to analyze the association between different serum biomarkers with wake-up IS episodes and their progression. Leukocytes count, serum levels of C-reactive protein, fibrinogen, interleukin 6 (IL-6), and vitamin D were analyzed as inflammation biomarkers; N-terminal pro-B-type Natriuretic-Peptide and microalbuminuria, used as atrial/endothelial dysfunction biomarkers; finally, glutamate levels as excitotoxicity biomarker. In addition, demographic, clinical and neuroimaging variables associated with the time-evolution of wake-up IS patients and functional outcome at 3 months were evaluated. Good and poor functional outcome were defined as mRS ≤2 and mRS > 2 at 3 months, respectively.
Results: Wake-up IS showed a poorer outcome at 3-months than in patients with known on-set-symptom time (59.1% vs. 48.1%; p < 0.0001). Patients with wake-up IS had higher levels of inflammation biomarkers; IL-6 levels at admission (51.5 ± 15.1 vs. 27.8 ± 18.6 pg/ml; p < 0.0001), and low vitamin D levels at 24 h (5.6 ± 5.8 vs. 19.2 ± 9.4 ng/ml; p < 0.0001) are worthy of attention. In a logistic regression model adjusted for vitamin D, OR was 15.1; CI 95%: 8.6-26.3, p < 0.0001. However, we found no difference in vitamin D levels between patients with or without clinical-DWI mismatch (no: 18.95 ± 9.66; yes: 17.84 ± 11.77 ng/mL, p = 0.394). No difference in DWI volume at admission was found (49.3 ± 96.9 ml in wake-up IS patients vs. 51.7 ± 98.2 ml in awake IS patients; p = 0.895).
Conclusions: Inflammatory biomarkers are the main factors that are strongly associated with wake-up IS episodes. Wake-up IS is associated with lower vitamin D levels. These data indicate that vitamin D deficiency could become a therapeutic target to reduce wake-up IS events.
📄 Download the PDF from VitaminDWiki
Stroke is more severe and disabling if vitamin D is lower - April 2021
The Relationship of Vitamin D Deficiency with Severity and Outcome of Acute Stroke
Rom J Intern Med. 2021 Apr 13. doi: 10.2478/rjim-2021-0013
Reza Ebrahimi Rad 1, Mohammadreza Zarbakhsh 2, Samira Sarabi 3
Background: There are currently conflicting results regarding the link between vitamin D deficiency and increased risk for stroke and its poor prognosis. The present study aimed to assess the relationship between vitamin D deficiency and prognosis of acute stroke.
Methods: This bi-center cross-sectional study was performed on 140 consecutive patients who referred to two general hospitals in Iran with the diagnosis of acute stroke. The levels of 25-hydroxy vitamin D were evaluated by Electrochemiluminescence (ECL) technique. Clinical severity of stroke on admission as well as on discharge time were evaluated using the National Institutes of Health Stroke Scale (NIHSS) or Modified Rankin (mRS) tools.
Results: Mean serum level of vitamin D was 25.51 ± 18.87 ng/mL, ranging from 3.0 to 98.6 ng/ml. There was a significant difference between the two groups (with and without vitamin D deficiency) in terms of stroke severity and disability, as reflected by mRS (P=0.003) and NIHSS evaluation (14.24 ± 9.23 versus 9.73 ± 7.36, P=0.003). Also, regarding patients' clinical condition, the mean NIHSS score in those with deficient and normal levels of vitamin D was 14.24 ± 9.23 and 9.73 ± 7.36, respectively with NIHSS score > 5 in 76.1% and 61.5%, respectively (P = 0.003).
Conclusion: According to the results of study, vitamin D status can be related to the severity of stroke. However, considering the cross-sectional design of our study, it could not point out the causality between vitamin D deficiency and acute stroke and further studies are warranted. It is not possible to draw any conclusions in terms of causality. Further studies are required in order to assess the relationship between the serum vitamin D levels and stroke severity.
4X more likely to have a good function after a stroke if have a high vitamin D level - May 2014
Prognostic Value of Serum 25-Hydroxyvitamin D in Patients with Stroke.
Neurochem Res. 2014 May 1.
Wang Y1, Ji H, Tong Y, Zhang ZB.

We aimed to evaluate the association between 25-hydroxyvitamin D [25(OH) D] levels and both clinical severity at admission and outcome at discharge in patients with acute ischemic stroke (AIS). From June 2012 to October 2013, consecutive first-ever AIS patients admitted to the Department of Emergency of The Fourth Affiliated Hospital of Harbin Medical University, China were identified. Clinical information was collected. Serum 25(OH) D levels were measured at baseline. Stroke severity was assessed at admission using the National Institutes of Health Stroke Scale (NIHSS) score. Functional outcome was evaluated at discharge using the modified Rankin scale (m-Rankin). Multivariate analyses were performed using logistic regression models. During the study period, 326 patients were diagnosed as AIS and were included in the analysis. Serum 25(OH) D levels reduced with increasing severity of stroke as defined by the NIHSS score. There was a negative correlation between levels of 25(OH) D and the NIHSS (r = - 0.389, P = 0.000). In multivariate analyses, serum 25(OH) D level was an independent prognostic marker of discharge favorable functional outcome and survival [odds ratio 3.96 (2.85-7.87) and 3.36 (2.12-7.08), respectively, P = 0.000 for both, adjusted for NHISS, other predictors and vascular risk factors] in patients with AIS. Serum 25(OH) D levels are a predictor of both severity at admission and favorable functional outcome in patients with AIS. Additional research is needed on vitamin D supplementation to improve the outcome of post-stroke patients.
📄 Download the PDF from sci-hub via VitaminDWiki
More likely to have a stroke if < 20 ng of vitamin D - Community living seniors
Vitamin D deficiency and incident stroke risk in community-living black and white adults Jan 2016
8.5 X more likely if black, 1.6X more likely if white - but racial difference was not statistically significant
Vitamin D and Stroke: Promise for Prevention and Better Outcome - 2015
Current Vascular Pharmacology, Jan 2014 free PDF online
Table 1. Association of Vitamin D Deficiency with Risk Factors for Cerebrovascular Events
Indirect
Hypertension
Diabetes mellitus
Metabolic syndrome
Atherosclerosis
Direct
Limitation of Antithrombotic Effects
Enhancement of platelet aggregation
Up-regulation of tissue factor gene
Down-regulation of antithrombin gene
Down-regulation of thrombomodulin gene
Limitation of Neuroprotective Effects
Biosynthesis of neurotrophic factors:
Nerve growth factor
Glial cell line derived neurotrophic factor (GDNF)
Biosynthesis of neurotransmitters
Brain detoxification pathways:
Expression of inducible nitric oxide synthase (iNOS)
Intracellular glutathione levels
Gamma-GT levels
Modulation of neuronal death:
- Regulation of L-Type calcium channels (L-VSCC) in hippocampal neurons
7 Stroke Symptoms 1 Month before it Happens - May 2024
0:00 - Intro
0:53 - 1: Silent High Blood Pressure
1:34 - 2: Extreme Fatigue
2:20 - 3: Vision Problems
2:58 - 4: Sudden Severe Headache
3:51 - 5: Numbness or Weakness
4:29 - 6: Speech Difficulties
4:55 - 7: Neurological Problems
5:24 - Two main types of strokes: Ischemic and Hemorrhagic
5:30 - Ischemic Stroke
5:48 - Hemorrhagic Stroke
Association between Vitamin- D Deficiency and Stroke - A Comparative Study - 2017
Charts of Vitamin D levels for the two types of strokes
📄 Download the PDF from VitaminDWiki
Hemorrhagic Stroke
--
Reasons for better hemorrhagic stroke outcome if higher Vitamin D - Aug 2021
Nutritional Supplementation of Naturally Occurring Vitamin D to Improve Hemorrhagic Stroke Outcomes
Front Neurol. 2021 Jul 30;12:670245. doi: 10.3389/fneur.2021.670245
Rani Ashouri 1, Madison Fangman 1, Jordan Brielmaier 1, Zoe A Fields 1, Natalie Campo 1, Sylvain Doré 1 2
📄 Download the PDF from VitaminDWiki
Vitamin D deficiency, if left untreated, is associated with bone disorders, cardiovascular damage, and an increased risk of ischemic stroke. While there are various nutritional options for the natural intake of vitamin D, we hope to elucidate the potential mechanisms dietary vitamin D may play in hemorrhagic stroke pathology. This scoping review outlines findings from studies relevant to the biochemical activity of vitamin D, the impact of vitamin D deficiency on hemorrhagic stroke outcomes, and the potential benefit of nutritional vitamin D on hemorrhagic stroke outcomes. Here, we analyze the relevant factors that can lead to vitamin D deficiency, and subsequently, a higher risk of hemorrhagic stroke incidence with worsened subsequent outcomes.
The neuroprotective mechanisms through which vitamin D works to attenuate hemorrhagic stroke onset and post-stroke outcomes have not yet been thoroughly examined.
However, researchers have proposed several potential protective mechanisms, including
reduction of blood brain barrier disturbance by inhibiting the production of reactive oxygen species,
mitigation of inflammation through a reduction of levels of proinflammatory cytokines, and
prevention of cerebral vasospasm and
delayed cerebral ischemia following subarachnoid hemorrhage and intracerebral hemorrhage.
While more research is needed and there are limitations to vitamin D supplementation, vitamin D as a whole may play a significant role in the dynamics of hemorrhagic stroke. Further research should focus on expanding our understanding of the neuroprotective capacity and mechanisms of vitamin D, as well as how vitamin D supplementation could serve as an effective course of treatment of hemorrhagic strokes.
Quick review of Hemorrhagic Stroke - June 2017
Vitamin D - maybe, Vitamin C - maybe, Cholesterol - maybe, Omega-3 - YES
- There has been some Hemorrhagic Stroke research: https://academic.oup.com/aje/article-lookup/doi/10.1093/aje/kwp227
- There was not enough data to show that vitamin D was significant - but the trend indicated a 40% reduction
- https://www.ncbi.nlm.nih.gov/pubmed/22627988 PDF online
- "We found no significant associations between dietary vitamin D and hemorrhagic stroke."
- How LOW Cholesterol Can Harm Your Health Green Medical Information, Sept 2012
- Cholesterol Is Needed To Prevent Hemorrhagic Stroke:
- The Role of Omega-3 Polyunsaturated Fatty Acids in Stroke - 2016
Omega-3 and vitamin C both PREVENT Hemorrhagic Stroke- Life Extension 2015
Omega-3 Good After Heart Attacks And For Hemorrhagic Stroke Prevention 2015
2 studies of Hemorrhagic stroke treatment with Vitamin D - July 2024
Nutritional Supplementation of Naturally Occurring Vitamin D to Improve Hemorrhagic Stroke Outcomes - July 2021 FREE PDF
Vitamin D Enhances Hematoma Clearance and Neurologic Recovery in Intracerebral Hemorrhage - May 2022 FREE PDF
Stroke prevention guidelines - 80% of strokes can be prevented, Vitamin D ignored - Oct 2024
2024 Guideline for the Primary Prevention of Stroke: A Guideline From the American Heart Association/American Stroke Association
