Juvenile Idiopathic Arthritis is strongly associated with low vitamin D – many studies
Juvenile idiopathic arthritis and Lupus have low bone mineral density (associated with low vitamin D) - July 2025
Autoimmun Rev. 2025 Jul 19:103886. doi: 10.1016/j.autrev.2025.103886
The assessment and management of bone health in pediatric-onset rheumatological diseases from early age to adulthood: A critical overview
Raffaele Di Taranto 1, Andrea Amati 2, Chiara Crotti 1, Francesco Baldo 3, Stefania Costi 3, Achille Marino 3, Massimo Varenna 1, Roberto Caporali 4, Cecilia Beatrice Chighizola 5
Despite the advancements achieved in modern rheumatology, patients with pediatric-onset rheumatological diseases are still exposed to systemic and/or articular inflammation and corticosteroid treatment, all exerting detrimental effects on the growing skeleton together with the reduced body weight and scarce physical activity that rheumatological patients usually experience. The assessment of bone mass in pediatric subjects carries computational limitations: Dual energy X-ray Absiorptiometry (DXA) underestimates bone mineral density (BMD) especially in case of smaller bone, an instance that occurs frequently in children with rheumatologic conditions due to the high rate of short stature or pubertal delay. The rates of low BMD in juvenile idiopathic arthritis (JIA) patients range between 3 % and 34 %, being higher in systemic and polyarticular JIA; patients with juvenile onset systemic lupus erythematosus (jSLE) present a low BMD in approximately 1/3 of cases. Such reduction in BMD presents early on disease course, persists with aging but might be reversed by rheumatological treatment. In pediatric populations, the term osteoporosis should be reserved to children with clinically relevant fractures, favoring "low BMD for chronological age". The prevalence of vertebral fractures ranges between 10 % and 30 % in JIA, peaking in female JIA patients aged 10-15 years, and between 21.4 % and 52 % in jSLE. While calcium and vitamin D supplementation should be optimized in all pediatric patients with rheumatological conditions, bisphosphonates should be reserved to subjects with fragility fractures; the prescription for primary fracture prevention in glucocorticoid-treated children is recommended only in case of a dosage <0.1 mg/kg/day for at least 3 months.
Can vitamin D be an adjuvant therapy for juvenile rheumatic diseases? - Aug 2023
Rheumatol Int. 2023 Aug 11. doi: 10.1007/s00296-023-05411-5
Maciej K Stawicki 1, Paweł Abramowicz 1, Gabriela Sokolowska 2, Sebastian Wołejszo 1, William B Grant 3, Jerzy Konstantynowicz 4
Vitamin D, known for its essential role in calcium and bone homeostasis, has multiple effects beyond the skeleton, including regulation of immunity and modulation of autoimmune processes. Several reports have shown suboptimal serum 25 hydroxyvitamin D [25(OH)D] levels in people with different inflammatory and autoimmune rheumatic conditions, and an association between 25(OH)D levels, disease activity and outcomes. Although most available data pertain to adults, insights often are extended to children. Juvenile rheumatic diseases (JRDs) are a significant health problem during growth because of their complex pathogenesis, chronic nature, multisystemic involvement, and long-term consequences. So far, there is no definitive or clear evidence to confirm the preventive or therapeutic effect of vitamin D supplementation in JRDs, because results from randomized controlled trials (RCTs) have produced inconsistent outcomes. This review aims to explore and discuss the potential role of vitamin D in treating selected JRDs. Medline/PubMed, EMBASE, and Scopus were comprehensively searched in June 2023 for any study on vitamin D supplementary role in treating the most common JRDs.
We used the following keywords: "vitamin D" combined with the terms
"juvenile idiopathic arthritis",
"juvenile systemic scleroderma",
"juvenile systemic lupus erythematosus",
"juvenile inflammatory myopathies",
"Behcet disease",
"periodic fever syndromes" and
"juvenile rheumatic diseases".
Observational studies have found that serum 25(OH)D concentrations are lower in juvenile idiopathic arthritis, juvenile systemic lupus erythematosus, juvenile systemic scleroderma, Behcet disease and proinflammatory cytokine concentrations are higher. This suggests that vitamin D supplementation might be beneficial, however, current data are insufficient to confirm definitively the complementary role of vitamin D in the treatment of JRDs. Considering the high prevalence of vitamin D deficiency worldwide, children and adolescents should be encouraged to supplement vitamin D according to current recommendations. More interventional studies, especially well-designed RCTs, assessing the dose-response effect and adjuvant effect in specific diseases, are needed to determine the potential significance of vitamin D in JRDs treatment.
📄 Download the PDF from VitaminDWiki
Vitamin D Supplementation in Patients with Juvenile Idiopathic Arthritis – April 2022
Chao-Yi Wu 1,2,Huang-Yu Yang 2,3ORCID,Shue-Fen Luo 4,Jing-Long Huang 1,2,5 andJenn-Haung Lai 4,6,*ORCID
Nutrients 2022, 14(8), 1538; https://doi.org/10.3390/nu14081538
Vitamin D has been implicated in the pathogenesis of skeletal disorders and various autoimmune disorders. Vitamin D can be consumed from the diet or synthesized in the skin upon ultraviolet exposure and hydroxylation in the liver and kidneys. In its bioactive form, vitamin D exerts a potent immunomodulatory effect and is important for bone health. Juvenile idiopathic arthritis (JIA) is a collection of inflammatory joint diseases in children that share the manifestation of inflamed synovium, which can result in growth arrest, articular deformity, bone density loss, and disability. To evaluate the potential effect of vitamin D on JIA disease manifestations and outcomes, we review the role of vitamin D in bone metabolism, discuss the mechanism of vitamin D in modulating the innate and adaptive immune systems, evaluate the clinical significance of vitamin D in patients with JIA, and summarize the supplementation studies.
📄 Download the PDF from VitaminDWiki
Concluding Remarks
JIA is the leading rheumatic disorder driven by a dysregulated innate and adaptive immune system in children. While current treatments provide notable improvements in the control of systemic inflammation and the relieve of symptoms in JIA, issues in long-term bone health and concerns for medication-related side effects, infection, and malignancy, for example, have led to the search for a cost-effective therapy or nutrient supplementation with limited side effects. Vitamin D is an essential hormone in altering calcium homeostasis and modulating bone health. Its deficiency can result in osteomalacia and rickets in humans [8,9]. Beyond its endocrine activity, vitamin D is capable of enhancing the immunomodulatory activities of monocytes and macrophages, and suppressing the proinflammatory cytokines produced by lymphocytes as summarized above [10-12]. Considering the prevalence of vitamin D insufficiency among patients with JIA and its ability to alter bone mineralization and immune modulation, rising interests have led to the research of vitamin D supplementation in JIA.
Clinical significance of vitamin D in patients with JIA has been documented. Data from limited randomized controlled trials, however, did not support the therapeutic effect of vitamin D supplementation in suppressing disease activity or improving bone mineralization. Heterogeneity between studies in terms of the study population, vitamin D supplementation regimen, outcome measurements, and definitions of vitamin D deficiency is perhaps the most obvious problem. Moreover, as trials were conducted across 30 years in different geographic locations, with various ethnic backgrounds, under diverse qualities of diet, sun exposure, and clothing style, it is hard to draw a conclusion based on the available information at present.
Further studies are needed to better evaluate the potential efficacy of vitamin D treatment in JIA. First, larger controlled trials are recommended as sample sizes from existing JIA supplementation studies were small. These trials do not allow for stratification based on baseline vitamin D concentration, JIA subtypes, disease activity, medication, diet quality, sun exposure, and other factors. Next, given the high prevalence of vitamin D deficiency and because vitamin D is noted to be safe for adults in doses of up to 4000 IU/day [117], trials should supply sufficient vitamin D to correct deficiencies.
In conclusion, mechanistic and epidemiologic data support a role for vitamin D in promoting bone health and modulating disease status in JIA. However, additional evidence is needed to clarify the efficacy of vitamin D supplementation in patients with JIA and determine the optimal level of vitamin D for these patients.
VITAMIN D AND ITS CLINICAL SIGNIFICANCE IN JUVENILE IDIOPATHIC ARTHRITIS – June 2017
Otilia Marginean1,2 Andrea Somogyi Militaru3, Oana Belei1,2 Raluca Corina Tamasanu1, Ioana Mozos4,5 ioanamozos@yahoo.de, Mirabela Dima6, Giorgiana Flavia Brad1,2 Niculina Mang1, Teofana Otilia Bizerea1 11st Pediatric Clinic.’’Victor Babe§” University of Medicine and Pharmacy, Timisoara, Romania
Vitamin D is known especially for its bone effects. Juvenile idiopathic arthritis (JIA) is one of the most common rheumatic diseases in childhood. It was the aim of the present study to evaluate vitamin D status in patients with JIA and to assess the relationship between vitamin D levels and disease activity. A total of 44 patients with JIA, diagnosed according to the International League Against Rheumatism (ILAR) criteria and a control group (n=13), matched for age and sex, with no musculoskeletal complaints, were evaluated. Disease activity was assessed, X-ray was performed in clinically active joints, with disease duration more than 6 months and vitamin D level was measured. Significant lower values were obtained for vitamin D in JIA patients compared to the healthy controls, especially in patients
📄 Download the PDF from VitaminDWiki
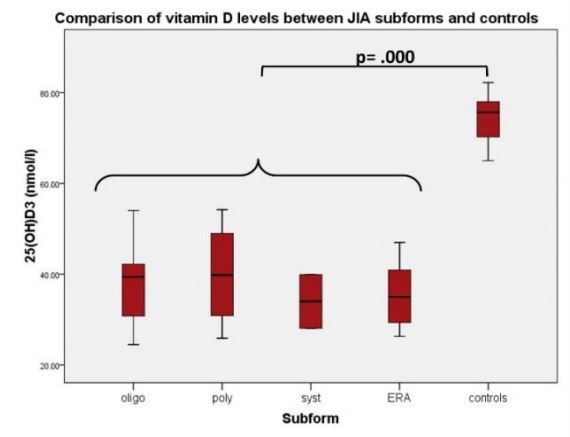
Determinants of Vitamin D Levels in Children, Adolescents, and Young Adults with Juvenile Idiopathic Arthritis - Aug 2014
J Rheumatol. 2014 Aug 1. pii: jrheum.131421
Stagi S, Bertini F, Cavalli L, Matucci-Cerinic M, Brandi ML, Falcini F.

OBJECTIVE:
Deficiency of 25-hydroxyvitamin D [25(OH)D] is reported to be common in patients with rheumatoid arthritis (RA); data in patients with juvenile idiopathic arthritis (JIA) are inconsistent. We assessed serum 25(OH)D in children, adolescents and young adults with JIA, in order to identify the risk factors for vitamin D deficiency in patients with JIA.
METHODS:
We evaluated 152 patients with JIA: 115 female, 37 male, mean age 16.2 ± 7.4 yrs; evaluated by onset type, 96 had oligoarticular, 35 polyarticular, 7 systemic, and 14 enthesitis-related arthritis (ERA). Patients were compared with a control group matched for sex and age. All patients and controls underwent laboratory tests of plasma 25(OH)D, parathyroid hormone (PTH), calcium, phosphorus, and bone alkaline phosphatase levels, and dual-energy x-ray absorptiometry examination.
RESULTS:
Patients with JIA showed significantly reduced 25(OH)D levels compared to controls (p < 0.001), even divided into subtypes (
oligoarticular, p < 0.05;
polyarticular, p < 0.005;
systemic, p < 0.001;
ERA, p < 0.005).
Patients with active disease and/or frequent relapses had significantly reduced 25(OH)D levels compared to patients with no active disease and no frequent flares (p < 0.005, respectively). Nevertheless, JIA patients had significantly higher PTH levels compared to controls (p < 0.0001). JIA patients with 25(OH)D deficiency showed a significantly lower bone mineral apparent density than those with normal 25(OH)D levels (p < 0.001).
CONCLUSION:
JIA patients have reduced 25(OH)D and higher PTH values. This may explain at least in part why JIA patients, despite more effective current drugs, do not achieve bone-normal condition over time. JIA patients with more severe disease could require higher supplementation of vitamin D to maintain normal 25(OH)D serum levels. Longterm studies are needed to investigate the relationship between serum 25(OH)D levels and disease activity in JIA.
📄 Download the PDF from VitaminDWiki
Vitamin D and different types of JIA types - May 2025
Subtype-specific profiles and predictive factors for early evaluation of vitamin D levels in newly diagnosed active juvenile idiopathic arthritis
8+ VitaminDWiki pages with both JUVENILE/CHILD AND ARTHRITIS/ARTHRITIC/LUPUS in the title
This list is automatically updated
{LIST()}
- Juvenile Rheumatoid Arthritis associated with low vitamin D, but how low – meta-analysis Jan 2013 shows rarity of JIA
VitaminDWiki - Rheumatoid Arthritis category
{include}
Note: Arthritis is associated with less D in cells (poor Vitamin D Receptor) (10+ studies)
You can measure a good level of vitamin D in the blood, but have little Vitamin D in the cells
studies in both categories Rehumatoid Artiritis and Vitamin D Receptor
This list is automatically updated
{category}
VitaminDWiki - Vitamin D Receptor activation can be increased in 14 ways
Omega-3, Magnesium, Zinc, Quercetin, non-daily Vit D, Curcumin, intense exercise, Butyrate Ginger, Essential oils, etc
Note: The founder of VitaminDWiki uses 10 of the 14 known VDR activators
Note: Weekly dosing gets more D into cells if poor VDR
