Overview Lung cancer and vitamin D
Lung Cancer: Role of Vitamin D, Vitamin D-Dependent Proteins, and Vitamin D Receptor - June 2024
Exploring the Role of Vitamin D, Vitamin D-Dependent Proteins, and Vitamin D Receptor Gene Variation in Lung Cancer Risk
Int. J. Mol. Sci. 2024, 25, 6664. https://doi.org/10.3390/ijms25126664
Tudor Ciocarlie 4, Alexandru Catalin Motofelea 2,*, Nadica Motofelea 3, Alina Gabriela Dutu 4, Alexandra Craciun 4, Dan Costachescu 5, Ciprian loan Roi 6, Ciprian Nicolae Silaghi 4 and Andreea Crintea 4
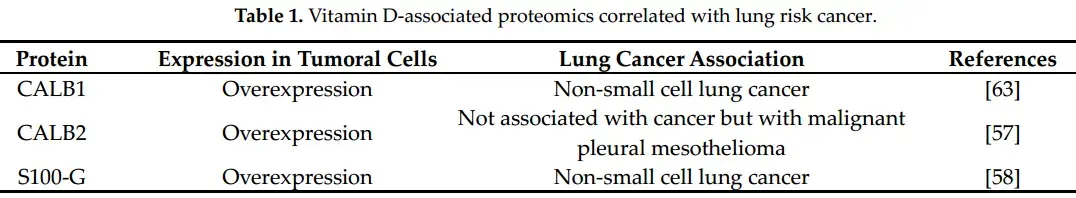
Lung cancer has an unfavorable prognosis with a rate of low overall survival, caused by the difficulty of diagnosis in the early stages and resistance to therapy. In recent years, there have been new therapies that use specific molecular targets and are effective in increasing the survival chances of advanced cancer. Therefore, it is necessary to find more specific biomarkers that can identify early changes in carcinogenesis and allow the earliest possible treatment. Vitamin D (VD) plays an important role in immunity and carcinogenesis. Furthermore, the vitamin D receptor (VDR) regulates the expression of various genes involved in the physiological functions of the human organism. The genes encoding the VDR are extremely polymorphic and vary greatly between human populations.
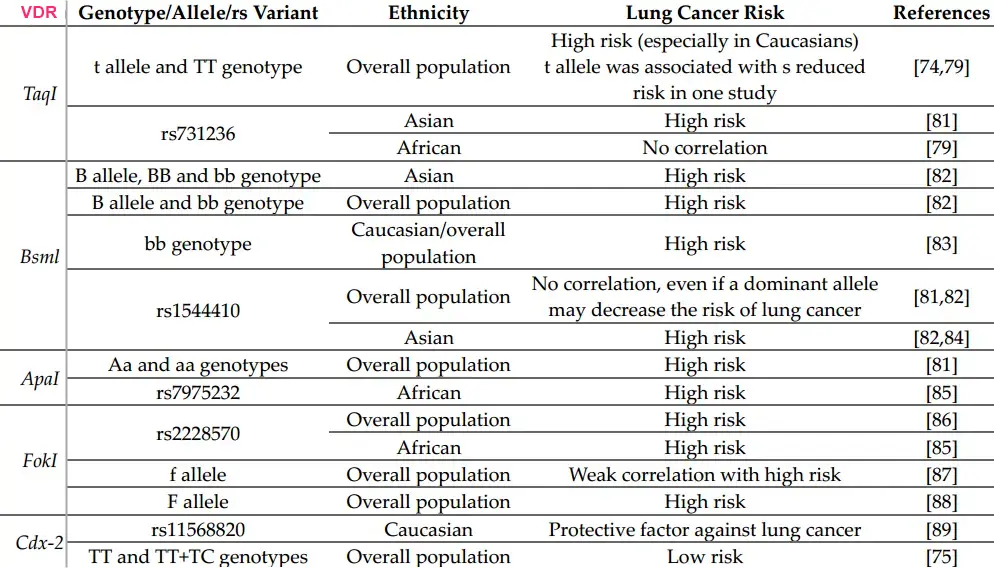
To date, there are significant associations between VDR polymorphism and several types of cancer, but the data on the involvement of VDR polymorphism in lung cancer are still conflicting. Therefore, in this review, our aim was to investigate the relationship between VDR single-nucleotide polymorphisms in humans and the degree of risk for developing lung cancer. The studies showcased different gene polymorphisms to be associated with an increased risk of lung cancer; TaqI, ApaI, BsmI, FokI, and Cdx2. In addition, there is a strong positive correlation between VD deficiency and lung cancer development. Still, due to a lack of awareness, the assessment of VD status and VDR polymorphism is rarely considered for the prediction of lung cancer evolution and their clinical applicability, despite the fact that studies have shown the highest risk for lung cancer given by TaqI gene polymorphisms and that VDR polymorphisms are associated with more aggressive cancer evolution.
📄 Download the PDF from VitaminDWiki
Has Lung Cancer, like many other cancers,COVID, etc. learned how to protect itself from Vitamin D by altering the VDR?
Cost of CT scans and Vitamin D for a 20% reduction in lung cancer deaths
CT: early detection: Cost $800/year
Vitamin D prevention: Cost $ 5/year
- Note: no proof for Vitamin D and lung cancer as of May 2014, but proof for many other cancers and diseases
- Cancer patients 64% less likely to die if have a high level of vitamin D – Dec 2011
- Vitamin D would also prevent many other forms of Cancer and health problems
Estimation of the cost of CT scan per pack
Assume same number years of smoking at CT scanning
Assume 400 packs per year (> the minimum of 32/year)
Cost of scan to the public per pack = $2
See also Lung cancer decreased by 7.5% for every 1260 feet in altitude
Yet another reason to think that Lung Cancer might be reduced with vitamin D
Life Extension Magazine March 2007 - Vitamin D and Cancers such as Lung Cancer
Prevention of Lung Cancer: Future Perspective with Natural Compounds
See also VitaminDWiki
Smoking reduces vitamin D - many studies an overview
One third of lung disease patients in China had less than 4ng of vitamin D – May 2012
Low vitamin D strongly related to death due to tobacco cancer, but not others – March 2013
Cancer patients 64% less likely to die if have high level of vitamin D – Dec 2011 has the following chart
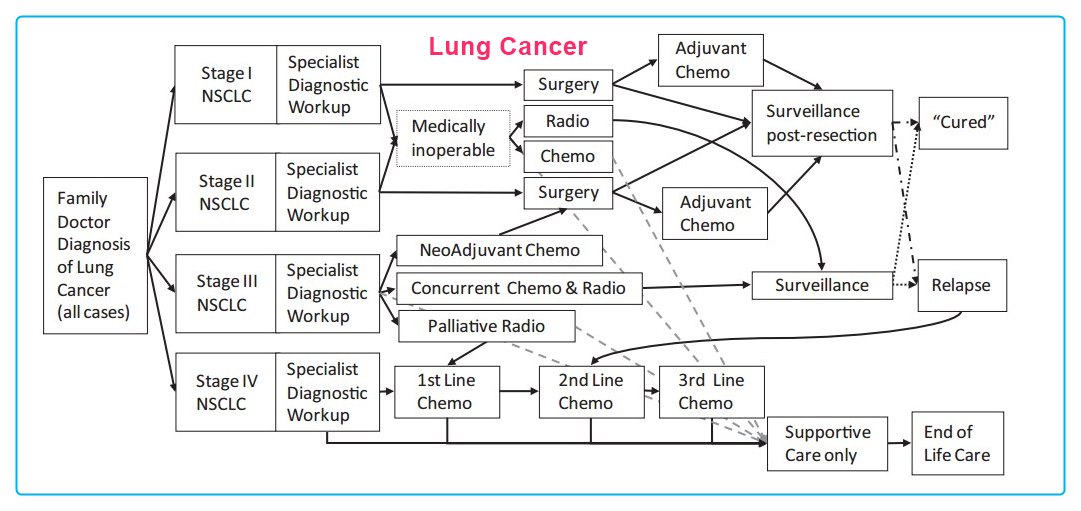
PubMed for Lung Cancer and vitamin D includes
Vitamin D status and the risk of lung cancer: a cohort study in Finland free PDF, small study - helped women, but not men
-
- Lower levels of UVB irradiance were independently associated with higher incidence rates of lung cancer in 111 countries.
Cancer intervention trials using Vitamin D
Lung Cancer 4X less for some races (smoking 10 cig. per day) - Aug 2018
Tobacco biomarkers and genetic/epigenetic analysis to investigate ethnic/racial differences in lung cancer risk among smokers
Smoking changes gene activation to different amount in different races

📄 Download the PDF from VitaminDWiki
Lung Cancer factoids from The Body by Bill Bryson, 2019
80 percent of all men smoked by the late 1940s—but very few of them developed lung cancer.
The upshot was that by the late 1950s the average smoker was taking in more tar and nicotine than he had before filters were invented.
American Medical Association took 15 years to endorse the surgeon general’s finding.
- can anticipate getting change from AMA about Vitamin D will take decades - Comment by founder of VitaminDWiki
As late as 1973, Nature ran an editorial backing women’s smoking during pregnancy on the grounds that it calmed their stress.
Nearly one-third of people below the poverty line (in the US) still smoke, and the habit continues to account for one-fifth of all deaths.
Why is the number of lung cancers in people who have never smoked increasing?
-
" “If lung cancer in never-smokers were a separate entity, it would be in the top 10 cancers in the U.S.” for both incidence and mortality."
"A 2019 study in South Korea diagnosed lung cancer in 0.45% of never-smokers, compared to 0.86% of smokers. "
- but the US never screens for lung cancer in never-smokers
Perhaps many cancers are increasing: toxins, poor food, less vitamin D, radon, family history of lung cancer . . .
20 non-smoking cases of lung cancer - Claude AI April 2024
Environmental Exposures
Radon Gas The #1 cause of lung cancer in non-smokers. A naturally occurring radioactive gas that seeps from soil and rock into buildings. Responsible for ~21,000 deaths/year in the U.S. Exposure is invisible and odorless — home testing is the only way to detect it.
Asbestos Fibrous minerals once widely used in insulation, flooring, and construction. Inhaled fibers lodge permanently in lung tissue, causing inflammation and DNA damage. Particularly dangerous in combination with smoking (synergistic risk). Linked especially to mesothelioma, a rare lung/chest lining cancer.
Air Pollution (Outdoor) Fine particulate matter (PM2.5) and nitrogen dioxide from traffic, industry, and wildfires are classified as Group 1 carcinogens by the IARC. Estimated to cause ~200,000+ lung cancer deaths globally per year.
Indoor Air Pollution Burning of biomass fuels (wood, coal, dung) for cooking/heating — a major cause in developing countries, especially among women. Also includes secondhand tobacco smoke.
Occupational Hazards
Certain jobs carry elevated risk due to chronic inhalation of carcinogens:
- Silica dust (mining, quarrying, sandblasting)
- Diesel exhaust (truck drivers, railroad workers)
- Chromium, nickel, cadmium (metalworking, electroplating)
- Beryllium (aerospace, nuclear industries)
- Coal dust and coke oven emissions
- Arsenic (smelting, pesticide manufacturing)
- Formaldehyde and vinyl chloride
Genetic & Hereditary Factors
- Family history of lung cancer raises personal risk ~2x, even after controlling for smoking.
- Mutations in genes like EGFR, KRAS, ALK, RET, and ROS1 can drive lung cancer development independently.
- People with certain inherited conditions (e.g., Li-Fraumeni syndrome, BRCA2 mutations) have elevated susceptibility.
- Some ethnic groups (e.g., East Asian women) have higher rates of EGFR-mutated lung adenocarcinoma with no smoking history.
Pre-existing Lung Conditions
- COPD (chronic obstructive pulmonary disease) — significantly elevated risk even in non-smokers
- Pulmonary fibrosis — chronic scarring creates a pro-carcinogenic environment
- Previous lung infections (TB, pneumonia) — especially associated with adenocarcinoma arising in scar tissue
- Lung adenomatosis / atypical adenomatous hyperplasia — precancerous lesions
Radiation Exposure
- Medical imaging — high cumulative CT scan doses over a lifetime
- Occupational radiation — uranium miners, nuclear plant workers
- Therapeutic radiation to the chest (e.g., for breast cancer or lymphoma) can increase risk years later
Dietary & Lifestyle Factors
- Beta-carotene supplements — paradoxically, high-dose supplementation increases lung cancer risk in high-risk individuals (CARET trial)
- Arsenic in drinking water — a well-established carcinogen
- Low fruit and vegetable intake — associated with modestly elevated risk
- Heavy alcohol use — some evidence of independent contribution
Emerging/Less-Established Factors
- Marijuana smoke — contains carcinogens similar to tobacco; evidence accumulating but not yet conclusive
- E-cigarettes/vaping — long-term cancer risk unknown but concerning
- Hormone factors — some evidence that estrogen may promote lung adenocarcinoma in women
- Chronic lung inflammation from any cause
Key Takeaway
Roughly 10–20% of lung cancers occur in lifetime never-smokers, making it effectively the 5th or 6th most common cancer death on its own. In never-smokers, the most common culprits are radon, secondhand smoke, air pollution, and genetic mutations — with adenocarcinoma being the predominant histological type. Vitamin D deficiency has also been studied as a risk modifier, with lower levels associated with worse outcomes and possibly higher incidence.
Related in VitaminDWiki
Click on a tag below
