Myopia may be related to low vitamin D
Many studies have found Myopia associated with Vitamin D and some of its cofactors - Mg and Zinc
Possibly: Less vitamin D ( or cofactors which increase Vitamin D getting to cells)
==> less muscle tone ==> eye muscle not as strong
The rest of this page are studies of Vitamin D/Sun and Myopia
Myopia 2X more likely if both parents had myopia (genetics?)
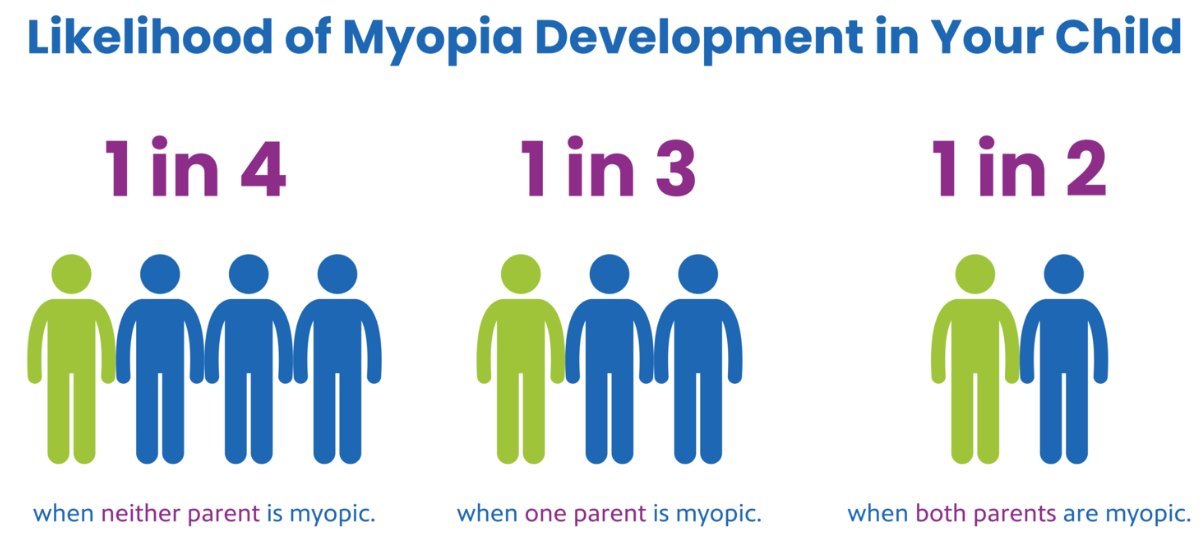
Potential candidate: Vitamin D Receptor gene
Google Search of Myopia & "Vitamin D" 4,800 hits June 2022 - 3 examples
Time outdoors, blood vitamin D status and myopia: a review - Oct 2020 📄 PDF
Vitamin D and its pathway genes in myopia: systematic review and meta-analysis - Dec 2018 📄 PDF
Spectrum of Darkness, Agent of Light: Myopia, Keratoconus, Ocular Surface Disease, and Evidence for a Profoundly Vitamin D-dependent Eye - June 2018 📄 PDF
Myopia 3 percent less likely per extra 1 ng vitamin D – May 2018
Risk factors for high myopia in Koreans: The Korea national health and nutrition examination survey.
Curr Eye Res. 2018 May 2. doi: 10.1080/02713683.2018.1472286.
Hwang HS1, Chun MY2, Kim JS3, Oh B4, Yoo SH5, Cho BJ1.
1 Department of Ophthalmology , Hallym University College of Medicine, Chuncheon Sacred Heart Hospital , Chuncheon , Korea.
2 Department of Global Medical Science , Sungshin Women's University , Seoul , Korea.
3 Department of Ophthalmology , Yonsei University College of Medicine , Seoul , Korea.
4 Department of Family Medicine , SMG-SNU Boramae Medical Center , Seoul , Korea.
5 Department of Medical Humanities and Ethics , Hanyang University College of Medicine , Seoul , Korea.
PURPOSE: To investigate risk factors for high myopia in the general Korean population.
METHODS:
In this nationwide population study, the dataset of the Korea National Health and Nutrition Examination Survey 2008-2012 was analyzed. The study cohort included 11,703 participants, aged 25-49 years, who underwent neither refractive nor cataract surgery. The association between demographic, socioeconomic, behavioral, and systemic variables and high myopia were investigated.
RESULTS:
The mean participant age was 37.9 ± 6.8 years old, and the prevalence of high myopia ≤-6.0 diopters (D) was 7.0 ± 0.3% in the study population. The right eyes (-1.76 ± 0.03 D) were more myopic than the left eyes (-1.70 ± 0.03 D; P < 0.001). In multivariate logistic regression analysis, high myopia was associated with age (odds ratio [OR], 0.97 per 1 year-increase) and female sex (OR, 1.24). Other identified risk factors included education level ≥university graduation (OR, 1.91), the presence of hypertension (OR, 1.69), and serum glucose level (OR, 1.01 per 1 mg/dL). Sunlight exposure of ≥5 hours a day (OR, 0.67) and
serum 25-hydroxyvitamin D level (OR, 0.97 per 1 ng/mL) showed protective effect against high myopia.
CONCLUSION:
High myopia is associated with younger age, female sex, high education level, longer sunlight exposure, and some other systemic conditions.
PMID: 29718719 DOI: 10.1080/02713683.2018.1472286
Myopia 2X more likely if have less than 20 ng of vitamin D – June 2014
Myopia is associated with lower vitamin D status in young adults.
Invest. Ophthalmol. Vis. Sci. June 26, 2014 IOVS-14-14589
Seyhan Yazar1,*, Alex W. Hewitt2, Lucinda J Black3, Charlotte M McKnight4, Jenny A. Mountain5, Justin C Sherwin6, Wendy H Oddy7, Minas Coroneo8, Robyn M Lucas9 and David A. Mackey10
↵* Centre for Ophthalmology and Visual Science, University of Western Australia, Lions Eye Institute, Perth, 6009, Australia seyhanyazar@gmail.com
Purpose: To investigate the association between serum vitamin D levels and myopia in young adults.
Methods: A total of 946 individuals participating in the 20-year follow-up of the Western Australian Pregnancy Cohort (Raine) Study were included in this study. Ethnicity, parental myopia and education status were ascertained by self-reported questionnaire. A comprehensive ophthalmic examination was performed, including post-cycloplegic autorefraction and conjunctival UV autofluorescence photography. Serum 25-hydroxyvitamin D3 (25(OH)D3) concentrations were determined using mass spectrometry. The association between serum 25(OH)D3 concentrations and prevalent myopia was determined using multivariable logistic regression. Myopia was defined as mean spherical equivalent ≤ -0.5 diopters.
Results: Of the 946 participants, 221 (23.4%) had myopia (n=725 non-myopic). Myopic subjects had lower serum 25(OH)D3 concentrations compared to non-myopic participants (median 67.6 nmol vs. 72.5 nmol, p=0.003). In univariable analysis, lower serum 25(OH)D3 concentration was associated with higher risk of having myopia (odds ratio [OR] for <50nmol/L vs. ≥50nmol/L: 2.63; 95CI% 1.71 - 4.05; p <0.001). This association persisted after adjustment for potential confounders, including age, sex, ethnicity, parental myopia, education status and ocular sun-exposure biomarker score (Adjusted OR 2.07; 95%CI 1.29-3.32; p=0.002).
Conclusions: Myopic participants had significantly lower 25(OH)D3 concentrations. The prevalence of myopia was significantly higher in individuals with vitamin D deficiency compared to the individuals with sufficient levels. Longitudinal studies are warranted to investigate whether higher serum 25(OH)D3 concentration is protective against myopia or whether it is acting as a proxy for some other biologically effective consequence of sun exposure.
Publisher wants $15 for the PDF
Myopia (in chickens) reduced by flashing light (myopia may not be due to low vitamin D)

Intermittent Episodes of Bright Light Suppress Myopia in the Chicken More than Continuous Bright Light
Weizhong Lan , Marita Feldkaemper, Frank Schaeffel
PLOS ONE Published: October 31, 2014DOI: 10.1371/journal.pone.0110906
Purpose: Bright light has been shown a powerful inhibitor of myopia development in animal models. We studied which temporal patterns of bright light are the most potent in suppressing deprivation myopia in chickens.
Methods: Eight-day-old chickens wore diffusers over one eye to induce deprivation myopia. A reference group (n = 8) was kept under office-like illuminance (500 lux) at a 10:14 light:dark cycle. Episodes of bright light (15 000 lux) were super-imposed on this background as follows. Paradigm I: exposure to constant bright light for either 1 hour (n = 5), 2 hours (n = 5), 5 hours (n = 4) or 10 hours (n = 4). Paradigm II: exposure to repeated cycles of bright light with 50% duty cycle and either 60 minutes (n = 7), 30 minutes (n = 8), 15 minutes (n = 6), 7 minutes (n = 7) or 1 minute (n = 7) periods, provided for 10 hours. Refraction and axial length were measured prior to and immediately after the 5-day experiment. Relative changes were analyzed by paired t-tests, and differences among groups were tested by one-way ANOVA.
Results: Compared with the reference group, exposure to continuous bright light for 1 or 2 hours every day had no significant protective effect against deprivation myopia. Inhibition of myopia became significant after 5 hours of bright light exposure but extending the duration to 10 hours did not offer an additional benefit. In comparison, repeated cycles of 1:1 or 7:7 minutes of bright light enhanced the protective effect against myopia and could fully suppress its development.
Conclusions: The protective effect of bright light depends on the exposure duration and, to the intermittent form, the frequency cycle. Compared to the saturation effect of continuous bright light, low frequency cycles of bright light (1:1 min) provided the strongest inhibition effect. However, our quantitative results probably might not be directly translated into humans, but rather need further amendments in clinical studies.
📄 Download the PDF from VitaminDWiki
See also VitaminDWiki
Tears often have 25 % higher levels of vitamin D than does blood
Myopia boom (still no mention of vitamin D) – Nature April 2015 has the following trend chart

15+ Vitamin D pages with "Myopia" in title
{LIST()}
See also web
- Time outdoors and myopia: a case for vitamin D? Optometry Times July 2013, same author as two studies on this page
- Take-Home Message The CLEERE study followed approximately 5,000 children over time to determine what factors were different between those who became myopic and those who remained emmetropic. Study investigators recently reported that myopic children engage in more near work than emmetropic children, although near work did not cause the myopia. It appears, however, that time spent outdoors lowers the risk of becoming myopic.
High myopia strongly associated with lowest vitamin D level - April 2014
Low serum 25-hydroxyvitamin D is associated with myopia in Korean adolescents.
Invest Ophthalmol Vis Sci. 2014 Apr 3;55(4):2041-7. doi: 10.1167/IOVS.13-12853.
Choi JA1, Han K, Park YM, La TY.
1Department of Ophthalmology, St. Vincent's Hospital, College of Medicine, the Catholic University of Korea, Seoul, Korea.
PURPOSE:
To assess the relationship between serum level of 25-hydroxyvitamin D (25(OH)D) and refractive error in Korean adolescents.
METHODS:
A total of 2038 adolescent aged 13 to 18 years, who participated in the Korea National Health and Nutrition Examination Survey (KNHANES) from 2008 to 2011 underwent refractive examination using an autorefractor. Serum 25(OH)D concentration and other potential risk factors were examined. Multivariate regression analysis was performed to investigate the association between serum 25(OH)D and spherical equivalent (SE).
RESULTS:
Among the participants, 80.1% had myopia (-0.5 diopters [D] or more myopic) and 8.9% had high myopia (-6.0 D or more myopia).
Age, total energy/Ca intake, area of residence, parental income, and smoking experience were significantly different among groups according to SE (All, P < 0.05).
The age-adjusted distribution of SE according to serum 25(OH)D concentration showed a positive relationship (r = 0.067, P = 0.012).
The myopia group had a significant positive relationship between SE and serum 25(OH)D tertile concentration (P = 0.020), whereas the nonmyopia group did not have any significant relationship (P = 0.599).
In multiple linear regression analyses, SE was significantly associated with low serum 25(OH)D concentration after adjustment for area of residence, parental income, total energy intake, dietary Ca intake, milk consumption, and smoking experience (P = 0.047).
The prevalence of high myopia was significantly associated with the lowest tertile of serum 25(OH)D concentration after adjustment for the confounding factors (P = 0.017).
CONCLUSIONS:
Low serum 25(OH)D concentration was associated with myopia prevalence in Korean adolescents.
This relationship was particularly notable in adolescents with high myopia.
PMID: 24699557
Publisher wants $15 for the PDF
Blood levels of vitamin D in teens and young adults with myopia.
Optom Vis Sci. 2011 Mar;88(3):377-82. doi: 10.1097/OPX.0b013e31820b0385.
Mutti DO, Marks AR.
The Ohio State University College of Optometry, Columbus, Ohio 43210-1280, USA. mutti.2@osu.edu
PURPOSE: Longitudinal data suggest that time outdoors may be protective against myopia onset. We evaluated the hypothesis that time outdoors might create differences in circulating levels of vitamin D between myopes and non-myopes.
METHODS: Subjects provided 200 μl of peripheral blood in addition to survey information about dietary intakes and time spent in indoor or outdoor activity. The 22 subjects ranged in age from 13 to 25 years. Myopes (n = 14) were defined as having at least -0.75 diopter of myopia in each principal meridian and non-myopes (n = 8) had +0.25 diopter or more hyperopia in each principal meridian. Blood level of vitamin D was measured using liquid chromatography/mass spectroscopy.
RESULTS: Unadjusted blood levels of vitamin D were not significantly different between myopes ( 13.95 ± 3.75 ng/ml) and non-myopes ( 16.02 ± 5.11 ng/ml, p = 0.29) nor were the hours spent outdoors (myopes = 12.9 ± 7.8 h; non-myopes = 13.6 ± 5.8 h; p = 0.83). In a multiple regression model, total sugar and folate from food were negatively associated with blood vitamin D, whereas theobromine and calcium were positively associated with blood vitamin D. Myopes had lower levels of blood vitamin D by an average of 3.4 ng/ml compared with non-myopes when adjusted for age and dietary intakes (p = 0.005 for refractive error group, model R = 0.76). Gender, time outdoors, and dietary intake of vitamin D were not significant in this model.
CONCLUSIONS: The hypothesis that time outdoors might create differences in vitamin D could not be evaluated fully because time outdoors was not significantly related to myopia in this small sample. However, adjusted for differences in the intake of dietary variables, myopes appear to have lower average blood levels of vitamin D than non-myopes. Although consistent with the hypothesis above, replication in a larger sample is needed.
PMID: 21258262

📄 Download the PDF from VitaminDWiki
VDR problems associated with 2X increase risk of Myopia - 2011
Vitamin D Receptor (VDR) and Group-specific Component (GC, Vitamin D Binding Protein) Polymorphisms in Myopia.
Invest Ophthalmol Vis Sci. 2011 Feb 25
Mutti DO, Cooper ME, Dragan E, Jones-Jordan LA, Bailey MD, Marazita ML, Murray JC, Zadnik K; the CLEERE Study Group.
The Ohio State University, College of Optometry, Columbus, OH 43210;
Purpose. Epidemiologic evidence indicates that time outdoors reduces the risk of myopia onset, suggesting a possible role for vitamin D. We conducted a case-control study to determine whether single nucleotide polymorphisms (SNPs) within VDR at 12q13.11 and GC at 4q12-13 were associated with myopia.
Methods. The primary analysis was conducted on 81 white adult control subjects between 18 and 50 years of age with a spherical equivalent refractive error between +0.50 D and +2.00 D in both eyes and less than 1.50 D of astigmatism. Affected myopic subjects were 289 unrelated white adults at least 18 years of age with at least --0.75 D myopia in both principal meridians of both eyes.
Results. One SNP within VDR was significantly associated with myopia in the multivariate analysis of the primary sample (rs2853559: odds ratio = 1.99, p = 0.003). In a subsample of less severely myopic white cases between -0.75 D and -4.00 D, three SNPs within VDR were significantly associated in a multivariate model after adjustment for multiple comparisons (rs2239182: odds ratio = 2.17, p = 0.007; rs3819545: odds ratio = 2.34, p = 0.003; rs2853559: odds ratio = 2.14, p = 0.0035), accounting for 12% of model variance over age alone.
Conclusions: Polymorphisms within VDR appear to be associated with low to moderate amounts of myopia in white subjects. Future studies should determine whether this finding can be replicated and should explore the biological significance of these variations with respect to myopia.
PMID: 21357399 📄 Download the PDF from VitaminDWiki
Myopia: a world tour
- US 1971-1972: 25%, by 1999-2004: 41.6%.
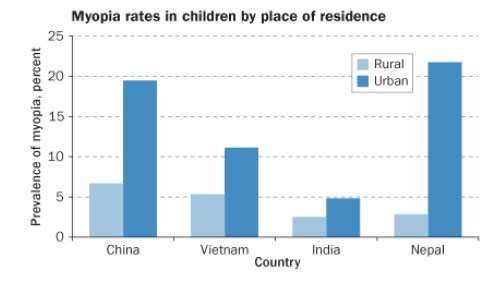
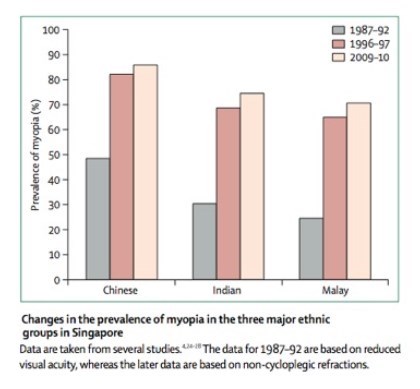
Extra 40 minutes outdoors daily: 30% incidence of myopia vs 40% if not outdoors - RCT 2015
Effect of Time Spent Outdoors at School on the Development of Myopia Among Children in China. A Randomized Clinical Trial
JAMA . 2015;314(11):1142-1148. doi:10.1001/jama.2015.10803.
Mingguang He, MD, PhD1,2; Fan Xiang, MD, PhD1,3; Yangfa Zeng, MD1; Jincheng Mai, BSc4; Qianyun Chen, MSc1; Jian Zhang, MSc1; Wayne Smith, MD, PhD5; Kathryn Rose, PhD6,7; Ian G. Morgan, PhD1,8
Objective To assess the efficacy of increasing time spent outdoors at school in preventing incident myopia.
Design, Setting, and Participants Cluster randomized trial of children in grade 1 from 12 primary schools in Guangzhou, China, conducted between October 2010 and October 2013.
Interventions For 6 intervention schools (n = 952 students), 1 additional 40-minute class of outdoor activities was added to each school day, and parents were encouraged to engage their children in outdoor activities after school hours, especially during weekends and holidays. Children and parents in the 6 control schools (n = 951 students) continued their usual pattern of activity.
Main Outcomes and Measures The primary outcome measure was the 3-year cumulative incidence rate of myopia (defined using the Refractive Error Study in Children spherical equivalent refractive error standard of ≤−0.5 diopters [D]) among the students without established myopia at baseline. Secondary outcome measures were changes in spherical equivalent refraction and axial length among all students, analyzed using mixed linear models and intention-to-treat principles. Data from the right eyes were used for the analysis.
Results There were 952 children in the intervention group and 951 in the control group with a mean (SD) age of 6.6 (0.34) years. The cumulative incidence rate of myopia was 30.4% in the intervention group (259 incident cases among 853 eligible participants) and 39.5% (287 incident cases among 726 eligible participants) in the control group (difference of −9.1% [95% CI, −14.1% to −4.1%]; P < .001). There was also a significant difference in the 3-year change in spherical equivalent refraction for the intervention group (−1.42 D) compared with the control group (−1.59 D) (difference of 0.17 D [95% CI, 0.01 to 0.33 D]; P = .04). Elongation of axial length was not significantly different between the intervention group (0.95 mm) and the control group (0.98 mm) (difference of −0.03 mm [95% CI, −0.07 to 0.003 mm]; P = .07).
Conclusions and Relevance Among 6-year-old children in Guangzhou, China, the addition of 40 minutes of outdoor activity at school compared with usual activity resulted in a reduced incidence rate of myopia over the next 3 years. Further studies are needed to assess long-term follow-up of these children and the generalizability of these findings.
Trial Registration clinicaltrials.gov Identifier: NCT00848900
