Statins and Vitamin D - many studies
Taking statins extends your life by 4 days, taking Vitamin D extends your life by 4 YEARS - Aug 2021
How Much Longer Do You Live on Statins?
| Statins | 4 days |
| vs. Exercise your whole life | 150 days |
| vs. Stopping smoking | 270 days |
| vs. a Diet packed with fruits, vegetables, and nuts | 800 days? |
| vs. Vitamin D | 1400+ days |
Are Doctors Misleading Patients About Statin Risks and Benefits? 5-minute video
" In a large clinical study, 3 percent of patients not taking the statin drug had a heart attack within a certain amount of time, compared to 2 percent taking the drug"
If doctors inform patients only about the relative risk reduction, for example, telling patients a pill with cut their risk of heart attacks by 34 percent, 9 out of 10 agree to take it. Give them the same information framed as absolute risk reduction, though, “1.4 percent fewer patients had heart attacks,” and those agreeing to take the drug drops to only 4 out of 10.
"; anti-statin spin could be like only 3 percent fewer heart attacks compared to a 1,267 percent higher risk of breast cancer.
Another "number needed to treat" - Vitamin D
Number of children needed to be treated by Vitamin D to prevent Infuenza = 13
Number of people with < 10 ng of vitamin D needed to prevent influenza = 4
Deep Research on Statins and Vitamin D - this wepage and the web - Perplexity AI Feb 2025
Executive Summary
The relationship between statins and vitamin D has emerged as a critical area of investigation due to the widespread use of statins for cardiovascular disease (CVD) prevention and the high prevalence of vitamin D deficiency globally. This report synthesizes evidence from clinical trials, observational studies, and meta-analyses to explore the bidirectional interactions between statins and vitamin D. Key findings include statins' modest cardiovascular benefits (1.3% absolute risk reduction in heart attacks)1, their association with musculoskeletal side effects, and the role of vitamin D in mitigating statin-induced myopathy. Paradoxically, while observational studies suggest vitamin D supplementation improves statin tolerance[VDW] 5 11, randomized controlled trials (RCTs) such as the VITAL study found no significant benefit 2 13. Mechanistic insights reveal that statins may alter vitamin D metabolism via cytochrome P450 enzymes, with lipophilic statins like atorvastatin reducing vitamin D levels [VDW] 6, whereas others like rosuvastatin increase them 7 17. Clinical recommendations emphasize individualized approaches, considering vitamin D status in patients with statin-associated muscle symptoms (SAMS), though evidence remains contentious.
[VDW] = PDF of this 📄 webpage on Feb 19, 2025 Follow the link for lots more information
US has the highest senior statin usage rates globally (nearly half of those >75) - Sept 2025
LDL cholesterol ranks 46th out of 48 factors in predicting CVD events - so why use statins - Feb 2025
1 of 12 questions in The Clot Thickens: The enduring mystery of heart disease (2021) Unbekoming Substack]
The Great Statin Scam - A Midwestern Doctor Dec 2024
over a trillion dollars have now been spent on Stains
"Statins are also one of the most frequent causes of pharmaceutical injuries
- (e.g., they are notorious for causing muscle, nerve, or liver damage and significant cognitive impairment)."
Pfizer's trial of their statin found (but was NOT disclosed to doctors) Of their 2,503 patients tested with Lipitor, seven experienced transient global amnesia attacks and four others experienced other forms of severe memory disturbances, for a total of 11 cases out of 2,503 test patients. This is a ratio of 4.4 cases of severe cognitive loss to result from every 1000 patients that took the drug.
- Not one word of warning of this was transmitted to the thousands of physicians who soon would be dispensing the drug.
High dose statins increase risk of Diabetes by 36% - Aug 2024
New Study Confirms What We've Known About Statins for 15 Years Mercola
People taking statins should supplement with both CO-Q10 and Vitamin K2 - Dec 2023
"With over a million annual heart failure hospitalizations in the United States, the condition is often referred to as an epidemic—and it may be that “statin drug therapy is a major contributing factor,” according to the review."
1.3% absolute risk reduction by statins - meta-analysis March 2023
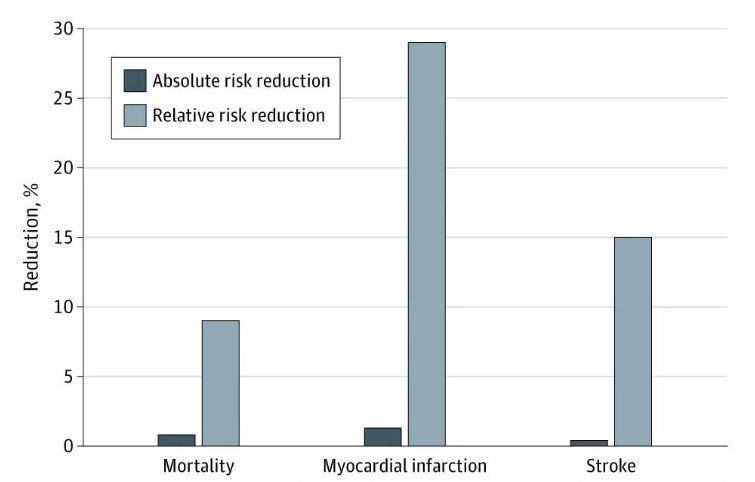
Evaluating the Association Between Low-Density Lipoprotein Cholesterol Reduction and Relative and Absolute Effects of Statin Treatment A Systematic Review and Meta-analysis* JAMA
Meta-analysis of 21 statin trials
Our analysis showed that trial participants taking a statin for an average of 4.4 years showed a 29% RELATIVE Risk Reduction in heart attacks, but the Absolute Risk Reduction was only 1.3%.
{FONT( size="18")}* 📄 Download the PDF from VitaminDWiki *{FONT}
Statin-Associated Muscle Symptoms decreased with Vitamin D - trial Nov 2022
Effects of Vitamin D Supplementation in Patients with Statin-Associated Muscle Symptoms and Low Vitamin D Levels **Metab Syndr Relat Disord. 2022 Nov 7. doi: 10.1089/met.2021.0127 PDF is behind a paywall
Claudio Carallo 1 , Alessandro Capozza 1 , Agostino Gnasso 1
 ** - - - - Have been unable to find out how much vitamin D was given
** - - - - Have been unable to find out how much vitamin D was given
Background: Statin therapy is a cornerstone of cardiovascular disease treatment and prevention. Unfortunately, 7%-29% of statin-treated patients complain of **muscular fatigue, cramps, and/or pain (statin-associated muscle symptoms [SAMS]). In recent years, the important role of vitamin D in muscle health maintenance has been highlighted. In addition, hypovitaminosis D is very prevalent and might be a reversible risk factor for SAMS occurrence.
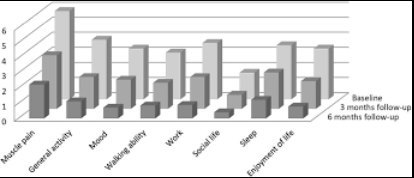
Methods: In our controlled intervention study, patients suffering from both SAMS and hypovitaminosis D underwent vitamin D replacement for 6 months. SAMS intensity and its impact on the quality of life were evaluated with a questionnaire during follow-up. A subgroup of patients who were not at the low-density lipoprotein cholesterol (LDL-C) target attempted a statin rechallenge after 3 months. Control subjects, with SAMS only, were not treated.
Results: Blood vitamin D levels reached 261% of baseline values.
Pain intensity was reduced by 63%, and
All life quality indicators improved.
At follow-up, percentage variations in SAMS intensity and in vitamin D levels were inversely related (r = 0.57, P = 0.002). In a multiple regression analysis, this association was found to be independent. Among the rechallenge subgroup,* 75% successfully tolerated high-intensity statins during the follow-up *. The parameters of interest were unchanged in control subjects.
Conclusions: In our findings, the amount of increase in vitamin D concentrations is directly related to SAMS improvement. Although randomized studies are needed, 25(OH)D levels can be measured and eventually supplemented in all patients suffering from SAMS, and this can be done together with a statin rechallenge after 3 months for patients who are not at the LDL-C target.
Register: The study protocol was registered with the* EudraCT clinical trial register *[ID: 2019-003250-83] in date April 8, 2020.
Found: The reason statins can make your muscles sore or weak - June 2023
* America’s Most Popular Drug Has a Puzzling Side Effect. We Finally Know Why* Poor gene: "enzyme is known as HMG-CoA reductase"
- "Many patients—some 5 percent in clinical trials, and up to 30 percent in observational studies—experience sore and achy muscles, especially in the upper arms and leg"
$400/month Cholesterol-Lowering Drug Reduces Absolute Risk of Heart Attack by 1.1% - March 2023
TrialSiteNews Bempedoic acid, brand name Nexletol,
The cost for Nexletol oral tablet 180 mg is around $426 for a supply of 30 tablets, - daily
25 VitaminDWiki pages containing "STATIN" in the title as of Feb 2025
Statin pain reduces Vitamin D levels by 4 ng - Meta-analysis July 2021
Statin pain reduces Vitamin D levels by 4 ng ( 9 studies) - Meta-analysis July 2021
Statins do cause pain - but it takes months for the pain to appear and disappear - Dr. Greger, May 2021
The trials (almost all of which were funded by statin manufacturers) looking for pain appearance in a short time did not detect it.
In the real world, pain is detected.
- "Three-quarters may flat out stop taking them, or sometimes up to nearly 90 percent discontinue treatment"
Lipophilic statins double the risk of dementia - July 2021
Statins Double Risk of Dementia, Are Linked to COVID Deaths Mercola July 2021
lipophilic statin examples: atorvastatin (Lipitor), simvastatin (Zocor), Fluvastatin (Lescol), and lovastatin (Altoprev),** The brain is up to 30% cholesterol. Statins reduce cholesterol
Are We Being Misled About the Benefits and Risks of Statins? - Greger Sept 2025
“your chance to avoid a nonfatal heart attack during the next 2 years is about 97% without treatment, but you can increase it to about 98% by taking a Crestor [a statin] every day.”
Dr. Greger has 200+ Statins videos
14% of UK adults are taking statins - new Statin Nation Book 2018* Alternative take on statins, fat and cholesterol is an intriguing read ** A Statin Nation: Damaging millions in a brave new post-health world *Dec 2018
Previous book with the same title by another author* Statin Nation: The Ill-Founded War on Cholesterol, What Really Causes Heart Disease and the Truth About the Most Overprescribed Drugs in the World *---
36% of heart patients have still prescribed Statins - strangely, a higher % if morning appointment - May 2021* Assessment of Primary Care Appointment Times and Appropriate Prescribing of Statins for At-Risk Patients *JAMA Network Open. 2021;4(5):e219050. doi:10.1001/jamanetworkopen.2021.9050
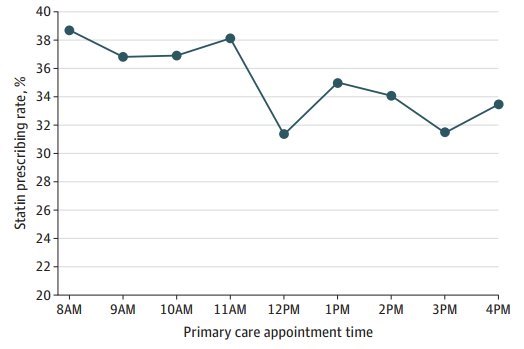
Do doctors remember dogma better in the morning?
Vitamin D blocked the simvastatin decline in exercise performance - RCT Dec 2017* Vitamin D supplementation improves simvastatin-mediated decline in exercise performance: A randomized double-blind placebo-controlled study. *J Diabetes. 2017 Dec;9(12):1100-1106. Doi 10.1111/1753-0407.12541. Epub 2017 Jun 28.
Singla M1, Rastogi A1, Aggarwal AN2, Bhat OM3, Badal D4, Bhansali A1.
| {BOX( title="VitaminDWiki" class="border" bg="#FFFAE2" width="700px")}* Three arms of Randomized Controlled 12 week trial with T2DM * | |||
|---|---|---|---|
| Cardiorespiratory fitness | Muscle mitochondrial content | ||
| 40 mg daily, simvastatin | -8.4% | -3.6% | |
| 40 mg daily, simvastatin + 60,000 IU Vitamin D weekly |
-0.6% | * 7.1% | |
| 60,000 IU Vitamin D weekly | * 16.7% |
{BOX}
BACKGROUND:
The aim of the present study was to determine the effect of vitamin D supplementation on simvastatin-mediated changes in cardiorespiratory fitness and skeletal muscle mitochondrial content after exercise in adults with type 2 diabetes mellitus (T2DM).
METHODS:
Vitamin D-deficient T2DM patients aged 25-50 years performed moderate-intensity aerobic exercise for 12 weeks and were randomized to receive simvastatin 40 mg daily plus vitamin D 60 000 units once weekly or vitamin D 60 000 units once weekly. The primary outcomes were cardiorespiratory fitness (peak oxygen consumption) and skeletal muscle mitochondrial content (citrate synthase activity in the vastus lateralis) following simvastatin and/or vitamin D replacement therapy.
RESULTS:
Twenty-eight patients completed the study. C decreased by 8.4% (P < 0.05) following 12 weeks of simvastatin therapy. Vitamin D supplementation blunted the decline in cardiorespiratory fitness to 0.6% (P < 0.05 for between-group difference in change from baseline).
Similarly, skeletal muscle mitochondrial content decreased by 3.6% with simvastatin but improved by 12.1% on supplementation with vitamin D, although the between-group difference was not significant. Vitamin D alone increased cardiorespiratory fitness and mitochondrial content by 7.1% (P < 0.05) and 16.7%, respectively.
CONCLUSIONS:
Simvastatin tends to cause deterioration in exercise-associated cardiorespiratory fitness and skeletal muscle mitochondrial content in adults with T2DM, which is blunted by vitamin D supplementation.
People taking statins have 1.5 ng more Vitamin D (after adjustment) - July 2020
The Effect of Statins on Serum Vitamin D Concentrations Among Older Adults
Cureus. 2020 Jul 1;12(7):e8950. doi: 10.7759/cureus.8950.
Carlos H Orces 1, Martha Montalvan 2 3 4, Daniel Tettamanti 5 6 7
Background Randomized and observational studies have previously reported inconsistent results for the direct association between statin therapy and 25 hydroxyvitamin D [25(OH)D] levels. Thus, the present study aimed to examine the relationship between statin use and 25(OH)D and its metabolites concentrations in a large nationally representative sample of older adults.
Methods This study was conducted using data from the National Health and Nutrition Examination Survey. Participants were asked to show the medication containers of all the products used in the previous 30 days, and the prescription of statins was defined on the three-level nested therapeutic classification scheme of Cerner Multum's Lexicon. General linear models adjusted for potential confounders were created to compare 25(OH)D concentrations between older adults taking statins and those who did not.
Results A total of 6,261 participants with a mean age of 69.5 years comprised the study sample. Of those, 40.2% were taking statins with a median length of therapy of 5 years.* Adjusted mean 25(OH)D3 and 25(OH)D levels were 3.3 and 4.4 nmol/L higher among participants taking statins than those who did not *, respectively. Moreover, this association was consistently seen regardless of the duration of therapy and particularly in subjects taking simvastatin, atorvastatin, or rosuvastatin. In subgroup analyses according to BMI categories and vitamin D intake, higher 25(OH)D levels were also seen among statin users. By contrast, this association was attenuated among those with a daily vitamin D between 400 and 800 and >800 IU.
Conclusion Older adults on statin therapy had significantly higher serum 25(OH)D concentrations. Additional research should be conducted to define the mechanism of this association and determine if the pleiotropic effects attributed to statins may be mediated by vitamin D.
See also VitaminDWiki
Statins with low vitamin D increased chance of musculoskeletal pain by 2X – Jan 2015 < 15 ng
Theories on the interaction between statins and vitamin D – 2012
Rosuvastatin given for renal problem resulted in increased vitamin D levels – RCT Dec 2012
Statin pain associated with 10 ng less vitamin D – meta-analysis Oct 2014
Off topic: US and NZ permit drug advertising on TV, none permit tobacco advertising
The statin Crestor dramatically increases levels of vitamin D in the blood – Jan 2012
One statin decreased vitamin D levels but the other did not – March 2010
Statin-induced Myalgias corrected with 100,000 weekly Vitamin D
Statins associated with 14X increase in Polymyalgia Rheumatica (a new disease) – Aug 2012
[tiki-download_file.php?fileId=155]
Statin pain eliminated by taking 50,000 IU vitamin D weekly – July 2011
Statin use increased probability of diabetes by 48 percent – perhaps via vitamin D Jan 2012
Approximately 1 in every 4 adult Americans over 45 currently using statins to "prevent heart disease."
Breast cancer 2X more likely if have taken statins for 10 years – July 2013
If you must take statins and want to avoid hardening of arteries, take vitamin K2 – RCT May 2015
The statin Crestor dramatically increases levels of vitamin D in the blood – Jan 2012
Antibiotics and Vitamin D are associated with many of the same diseases
- Statins were first developed as antibiotics
Statin intolerance reduced as the level of vitamin D is raised - July 2015
about 53% are no longer statin intolerant if > 30ng of vitamin D
about 90% are no longer statin intolerant if 54 ng of vitamin D* 📄 Download a letter to the editor from VitaminDWiki *---
490+ Statins and Vitamin D studies in PubMed* PubMed as of Jan 2025 ** Statin Intolerance: A Review and Update - March 2023 doi: 10.1016/j.eprac.2023.03.004 PDF is behind a paywall
Association Between Vitamin D Supplementation and Statin-Associated Muscle Symptoms: A Systematic Review - June 2022 https://doi.org/10.1007/s40292-022-00526-5 PDF is behind a paywall
- "We found that vitamin D supplementation was associated with improved statin tolerance in 509 out of 606 (83.9%) patients across the 7 studies"
Effects of Vitamin D Supplementation in Patients with Statin-Associated Muscle Symptoms and Low Vitamin D Levels. - Dec 2022 doi: 10.1089/met.2021.0127 PDF is behind a paywall
Vitamin D Supplementation During Statin Rechallenge in Patients With a History of Intolerance.- June 2021
The Effect of Statins on Serum Vitamin D Concentrations Among Older Adults July 2020 FREE PDF
Effects of vitamin D supplementation on adherence to and persistence with long-term statin therapy: Secondary analysis from the randomized, double-blind, placebo-controlled ViDA study.- July 2018
Impact of vitamin D status on statin-induced myopathy. Free PDF doi: 10.1016/j.jcte.2016.11.002 Dec 2016
Statin Use and 25-Hydroxyvitamin D Blood Level Response to Vitamin D Treatment of Older Adults.- June 2017
Is there really a relationship between serum vitamin D (25OHD) levels and the musculoskeletal pain associated with statin intake? A systematic review. April 2016 full free text
Safety of 50,000-100,000 Units of Vitamin D3/Week in Vitamin D-Deficient, Hypercholesterolemic Patients with Reversible Statin Intolerance. March 2016 full free text
21% less vitamin D in those taking statins - 3 RCT Feb 2017* Statin Use and 25-Hydroxyvitamin D Blood Level Response to Vitamin D Treatment of Older Adults. *J Am Geriatr Soc. 2017 Feb 27. doi: 10.1111/jgs.14784.
Bischoff-Ferrari HA1,2, Fischer K1,2, Orav EJ3, Dawson-Hughes B4, Meyer U1,2, Chocano-Bedoya PO1,2, Meyer OW1,2, Ernst R1,2, Schietzel S1,2, Eberli F5, Staehelin HB6, Freystätter G1,2, Roas S1, Theiler R1,2, Egli A1,2, Wilson NM1,2.
OBJECTIVES: To determine whether statin use alters the response of 25-hydroxyvitamin D (25(OH)D) level to vitamin D treatment.
DESIGN: Pooled analysis.
SETTING: Three double-blind randomized controlled trials that tested different doses of vitamin D.
PARTICIPANTS: Participants of three trials (N = 646; mean age 76.3 ± 8.4, 65% female).
MEASUREMENTS: In all three trials, 25(OH)D status and statin use were assessed repeatedly over time (baseline, 6 and 12 months). Repeated-measures analysis was used to compare 25(OH)D responses to vitamin D treatment at baseline and 6 and 12 months of statin users and nonusers, controlling for age, sex, body mass index, Charlson Comorbidity Index, vitamin D dose, trial, and season.
RESULTS: At baseline, 17.5% were statin users, and 65% were vitamin D deficient (25(OH)D < 20 ng/mL). Baseline 25(OH)D levels did not differ significantly between groups at baseline (18.8 for statin users, 17.2 ng/mL for nonusers, P = .07), but according to the longitudinal analyses, the total increase over 12 months in 25(OH)D concentration was significantly lower in statin users (13.1 ng/L) than nonusers (15.9 ng/mL; 21.4% difference; P = .009).* CONCLUSION: Of persons aged 60 and older at high risk of vitamin D deficiency, statin users had a 21.4% smaller increase in 25(OH)D serum concentrations over time than nonusers, independent of vitamin D dose and other covariates. PMID: 28240766 DOI: 10.1111/jgs.14784 Publisher will rent the PDF for $6 *---
Do statins increase the level of vitamin D in the blood in the short term?* Question: Is this a direct effect, or is it due to statins reducing cholesterol, which is needed to produce vitamin D from the skin, but cholesterol is not needed if the vitamin D is taken as a supplement * Some people appear to think that vitamin D could serve the same function as statins at a much lower cost and much lower risk. Note: one statin is the top-selling US prescription drug - with more sales than the next two top-selling drugs **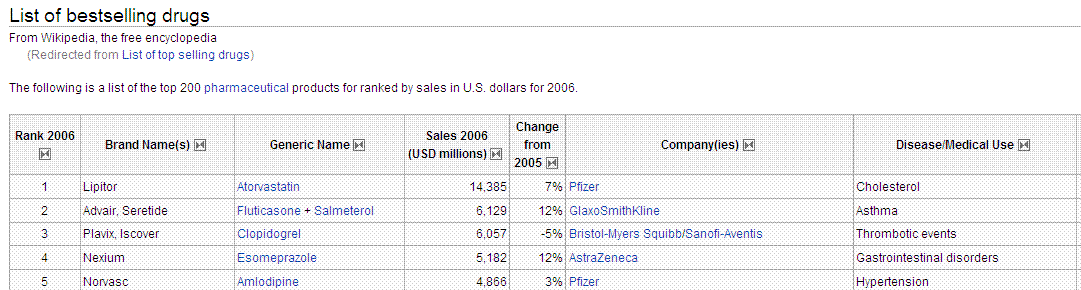
See also Web
Evidence shows Calcium supplementation is useless for the bones and dangerous for the heart. MINA Nov 2016
- "excess calcium in their coronary artery and who take statins have a 17-fold higher risk of heart attacks than do those with lower arterial calcium levels"
New York Times Article March 2012
About 1 in 200 on statins get diabetes
about 4 in 200 on statins do not get a heart attack (if not had one before)
with 200 million taking statins in the US,* this amounts to 200,000 more people getting diabetes ** New statin guidelines: Everyone 40 and older should be considered for the drug therapy Nov 2016
The U.S. Preventive Services Task Force, as reported by Washington Post
"The new guidelines, published in JAMA, suggests that people ages 40 to 75 who have one or more risk factors — such as high cholesterol, high blood pressure, diabetes, or smoking that put them at a 10 percent or greater risk of having a heart attack or stroke in the next 10 years — should be on statins"
FDA warning Feb 2012 Statins associated with"
- Diabetes, *Muscle loss, *Memory loss
Consumer Alert: 300+ Health Problems Linked To Statin Drugs Green Medical Information April 2012
Statins double diabetes rates Mercola July 2019
Do YOU Take Any of These 11 Dangerous Cholesterol Drugs? Mercola Aug 2012
over 900 studies proving the adverse effects of statins. If You Take Statins, You MUST Take CoQ10
appropriate sun exposure normalizes your cholesterol levels and prevents heart disease
The Many Health Benefits of Coenzyme Q10 and Ubiquinol Mercola June 2016
Some people do not have the gene which turns CoQ10 into Ubiquinol - interview with transcript
Can Red Yeast Rice Supplements Help Manage Your Cholesterol Levels? Mercola Feb 2018
Red yeast rice has fewer side effects than statins
Enhancement of vitamin D levels by statins Endocrine conference June 2013
Patients who were taking statins were significantly more likely to have vitamin D levels at or above 30ng/ml (X2=5.5, p=0.02) than patients not on a statin
Low vitamin D levels associated with statin induced muscle pain Vitamin D Council] March 2013
PLOS ONE free full-text study; 21% more likely if low vitamin D
Cholesterol drug users may use pills as a license to overeat April 2014
US statin users were eating about the same number of calories as non-users by 2009-2010.
Statins: proven and associated harms May 2014 details, with RCT references
2X more likely to have pain with a statin if vitamin D <15 ng
New York Times Nov 2015 - no mention of vitamin D
A Systematic Review and Meta-analysis of 7 Studies with 2416 Patients 2014
statin-induced myalgia is associated with -9.4 ng less vitamin D (7 studies, 2400 people - see table below
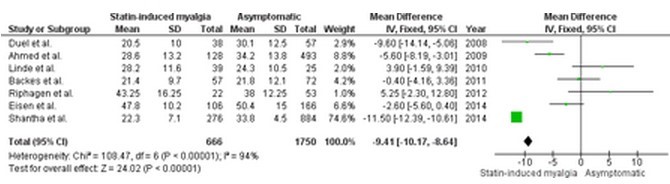
Statins & Muscle Pain Dean - April 2016
Comment on Medscape article on Statins
75% of those over 50 years old will be on statins!
10–20% have reported muscle-related side effects – pain and/or weakness
She recommends Magnesium
Double-blind RCT with/without Statins - no change in reporting of pain Lancel May 2017
PDF31075-9/fulltext) costs $31.50
Short comment about stains and vitamin by Dr who wrote book about Statin Problems
1% to 5% of statin users get muscle pain - perhaps associated with depletion of vitamin D
1. Vitamin D reduces Statin pain - review April 2019 <strong>Vitamin D Supplementation to Treat Statin-Associated Muscle Symptoms: A Review.</strong> Sr Care Pharm. 2019 Apr 1;34(4):253-257. doi 10.4140/TCP.n.2019.253.
Lowe K, Kubra KT, He ZY, Carey K.
For the past 15 years, cardiovascular disease (CVD) has been the leading cause of death for both men and women in the United States and worldwide. With an aging population, there has been increasing use of statin therapy to reduce the risk of CVD. However, statin-associated muscle symptoms (SAMS) remain an obstacle to this treatment, leading to discontinuation and nonadherence to statin therapy. Signs and symptoms of SAMS include muscle pain, tenderness, and increased serum creatine kinase. Despite the idiopathic pathophysiology of SAMS, some studies have shown an association between vitamin D deficiency and SAMS; the use of vitamin D supplements can lead to relief of these symptoms. The purpose of this review was to critique evidence for the association between low serum vitamin D and SAMS and the use of vitamin D supplementation for treatment.
1. Benefits of Chocolate on the Heart and all-cause mortality (vs. statins) - 2012
Green Med Info April 2012
Great many health benefits of chocolate documented -
Regarding just the heart: Chocolate appears to be better than statins.
1. Statin Health problems - GreenMedInfo - 2015, 2019 <strong>nothing about vitamin D</strong> <strong><a href="https://www.greenmedinfo.com/blog/cracking-cholesterol-myth-how-statins-harm-body-and-mind">2019 update</a></strong> <strong>* <a href="http://www.greenmedinfo.com/blog/cracking-cholesterol-myth-how-statins-harm-body-and-mind">Cracking the Cholesterol Myth: How Statins Harm The Body and Mind</a></strong> * A new study finds the chemical war against cholesterol using statin drugs was justified through statistical deception and the cover-up of over 300 adverse health effects documented in the biomedical literature
| Muscle damage 80 studies | Nerve damage 54 studies | * Liver damage 32 studies |
| Endocrine disruption: 16 studies | Cancer-promoting: 9 studies | Diabetes-promoting: 8 studies |
| Cardiovascular-damaging: 15 studies | Birth defect Causing 11 studies |
The JUPITER trial of Crestor vs. placebo resulted in increased fatal heart attacks in the treatment group, which were obscured by combing fatal and nonfatal infarctions.
The HPS study had a 26% dropout rate prior to the beginning of the trial, so those with significant side effects were functionally excluded from the study.
In at least four trials, statistically significant increases in cancer incidence were found, and handily dismissed by all authors as insignificant because they claimed "no known potential biological basis" is known.
A low serum cholesterol level has also been found to serve as a biological marker of major depression and suicidal behavior,
suicidal ideation among adults with mood disorders was more than 2.5-times greater in those taking statins
"So, the next time you hear of a doctor recommending a cholesterol-lowering intervention, tell him you'll take that 1% risk and spare yourself cancer, cognitive dysfunction, myopathy, and diabetes" Aug 2016 Video Statin Drugs Linked to 300+ Adverse Effects ---
- If you really must take statins and they cause pain, vitamin D will relieve the pain - 2015
50,000 or 100,000 IU of vitamin** D2per week relieved statin pain 📄 Download the PDF from VitaminDWiki * ConsumerLabs has a nice summary of this as well as many other vitamin D studies behind a subscription paywall
Their paywall is very much worth the price. They review a huge number of supplements
I have subscribed for over a decade
1. 80% of the people who should take statins have decided not to (TOO many side effects?) - 2015
Eight in 10 Primary-Prevention Patients Skip Statins, Dutch Study Finds Medscape
70,000 participants in the LifeLines cohort study
Conclusion of the report - doctors need to insist that the patients actually take the statins
1. Statins associated with low vitamin D - Dec 2015 <strong>Statin therapy and Vitamin D</strong> Int J Basic Clin Pharmacol. 2015; 4(6): 1113-1117<a href="https://doi.org/10.18203/2319-2003.ijbcp20151342">[doi: 10.18203/2319-2003.ijbcp20151342</a>](https://doi.org/10.18203/2319-2003.ijbcp20151342)
Arunkumar Radhakrishnan, A. Ruckmani, M. Abishek, S. Govindaraju.
Background: Statins are well-known drugs used in dyslipidemia and cardiac disorders for several years. Recently, it has been reported that long-term use of statins reduces serum vitamin D levels. When statins are administered to patients with low vitamin D, more muscular side effects have been reported. On the contrary, a few studies report that statins might increase vitamin D levels competing with its metabolism. Hence, this study was conducted to evaluate the association between statins and vitamin D.
Methods: 125 participants who fulfilled the selection criteria were enrolled in the study. 65 subjects belonged to the control group and 60 to the statin group. The blood sample was collected for Vitamin D estimation. The results were correlated with a demographic profile, the nature of statin, and the muscular side effects and compared with the control group.
Results: The mean vitamin D level in the statin group was 15.82 ng/ml±11.51 and 20.57 ng/ml±7.007 in the control group. The difference was found to be statistically significant. 13.85% in the control group and 10% in the statin group had sufficient vitamin D levels. 18.33% and 36.92 % had insufficient levels, and 71.67% and 49.23% had a deficiency in the statin and control groups, respectively. Myalgia was reported by 30 among 60 subjects (50%) in the statin group and 5 among 65 subjects (7.69%) in the control group.
Conclusion: The present study has shown that statin therapy is associated with low vitamin D levels and that this could contribute to the increased incidence of myalgia in the statin group.** 📄 Download the PDF from VitaminDWiki---
1. Statin intolerance ==> statin tolerance after adding lots of vitamin D - March 2016</strong> ID: 86: SAFETY OF 50,000-100,000 UNITS OF VITAMIN D3 PER WEEK IN VITAMIN D DEFICIENT, HYPERCHOLESTEROLEMIC PATIENTS WITH STATIN INTOLERANCE **Journal of Investigative Medicine
V Jetty, G Duhon, P Shah, M Prince, K Lee, M Goldenberg, A Kumar, CJ Glueck, P Wang
DOI: 10.1136/jim-2016-000120.39 Published 22 March 2016
Background In ∼85–90% of statin-intolerant patients, vitamin D deficiency (serum 25 (OH) D <32 ng/ml) is a reversible cause of statin intolerance, usually requiring 50,000 to 100,000 units of vitamin D/week continuously to normalize serum vitamin D, and thus successfully allow reinstitution of statins which previously could not be tolerated because of myalgia-myositis.
Specific Aim In 274 statin-intolerant patients, all with low entry serum vitamin D (<32 ng/ml, median 21 ng/ml), we assessed safety and efficacy of vitamin D supplementation (50,000–100,000 units/week) over treatment periods of 3 months (n=274), 3 and 6 months (n=161), 3, 6, and 9 months (n=58), and 3, 6, 9, and 12 months (n=22).
Results In the 385 patients with a 3-month follow-up, taking mean 61,000 and median 50,000 IU of vitamin D3/week, median serum vitamin D rose from 20 to 42 ng/ml (p<0.0001); vitamin D became high (>100 ng/ml) but not toxic-high (>150 ng/ml) in 4 patients (1.0%) (101, 102, 106, 138 ng/ml). Median serum calcium was unchanged from entry (9.6 mg/dl) to 9.6 at 3 months. On vitamin D supplementation, the trend of change in serum calcium from normal-to-high or from high to normal did not significantly differ (McNemar S=1.0, p=0.32), and there was no significant trend in change of the calculated glomerular filtration rate (eGFR) from entry to follow-up (McNemar S=2.6, p=0.11).
In the 161 patients with 3 and 6-month follow-up, taking mean 67,000 and median 50,000 IU of vitamin D3/week, median entry serum vitamin D rose from 21 to 42 to 44 ng/ml (p<0.0001), serum vitamin D was high (>100 but <150 ng/ml) in 2 patients at 3 months (1.2%, 101, 102 mg/ml) and in 3 (1.9%) at 6 months (101, 140, 140 ng/ml). Median serum calcium was unchanged from entry (9.7 mg/dl) at 3 and 6 months (9.7, 9.6 mg/dl, p>0.05). On vitamin D supplementation, the change in serum calcium from normal-to-high or high-to-normal was no significant trend (McNemar S=0.7, p=0.41), and no trend in change of eGFR (McNemar S=1.3, p=0.26).
In the 58 patients with 3, 6, and 9-month follow-up on mean and median 71,000 and 100,000 IU of D3/week, median entry vitamin D rose from 20 to 37, 41, and 44 ng/ml (p<0.0001), with 1 (1.7%, 102 ng/ml), 2 (3.5%, 140, 140 ng/ml), and 0 (0%) patients high. Median serum calcium was unchanged from entry, median 9.7, 9.8, 9.6, and 9.6 mg/dl. On vitamin D supplementation, the trend of change in serum calcium from normal-to-high or high-to-normal was not significant (McNemar S=1.8, p=0.18), and no trend in change of eGFR (McNemar S=2, p=0.16).
In the 22 patients with follow-up at 3, 6, 9, and 12 months on mean and median 70,000 and 75,000 IU of D3/week, median serum vitamin D rose from 20 to 37, to 41, to 44, and to 43 ng/ml (p<0.0001), with 1 (5%, 102 ng/ml) high, 2 (9%, 140, 140) high, 0 (0%) high, and 1 (5%, 126 ng/ml) high. Serum calcium was unchanged, median at entry 9.6, and then at 3, 6, 9, and 12 months 9.7, 9.7, 9.5, and 9.7 mg/ml. At entry, serum calcium was normal in 21, none high, and one became high at 12-month follow-up. The trend of change in eGFR was insignificant, McNemar S=1.0, p=0.32.
When serum D rose above 100 ng/ml in the few cases, as above, it fell into the normal range within 2 weeks by reducing the vitamin D dose by 50%.
Conclusions When 50,000–100,000 units of vitamin D/week are given to reverse statin intolerance in statin-intolerant patients with low entry vitamin D (<32 ng/ml), it appears to be safe over up to 1-year follow-up, without toxic high serum vitamin D levels >150 ng/ml, and levels rarely >100 ng/ml, and without changes in serum calcium or eGFR.
1. Atorvastatin decreases D levels via CPY3A4; parvastatin increases D levels via CYP27A1 - 2016 <strong><a href="http://www.atherosclerosis-journal.com/article/S0021-9150(16">The mechanism of statin-induced modulation of vitamin D metabolism</a>30525-1/abstract) Sept 2016</strong> Behind $36 paywall http://dx.doi.org/10.1016/j.atherosclerosis.2016.07.224
1. Those with Statin pain were 3 times more likely to have levels of low vitamin D – Nov 2016 <strong>Impact of Vitamin D Status on Statin-Induced Myopathy</strong> J of Clinical and Translational Endocrinology DOI: http://dx.doi.org/10.1016/j.jcte.2016.11.002
Krista D. Riche, Justin Arnall, Kristin Rieser, Honey E. East, Daniel M. Riche** 📄 Download the PDF from VitaminDWiki * *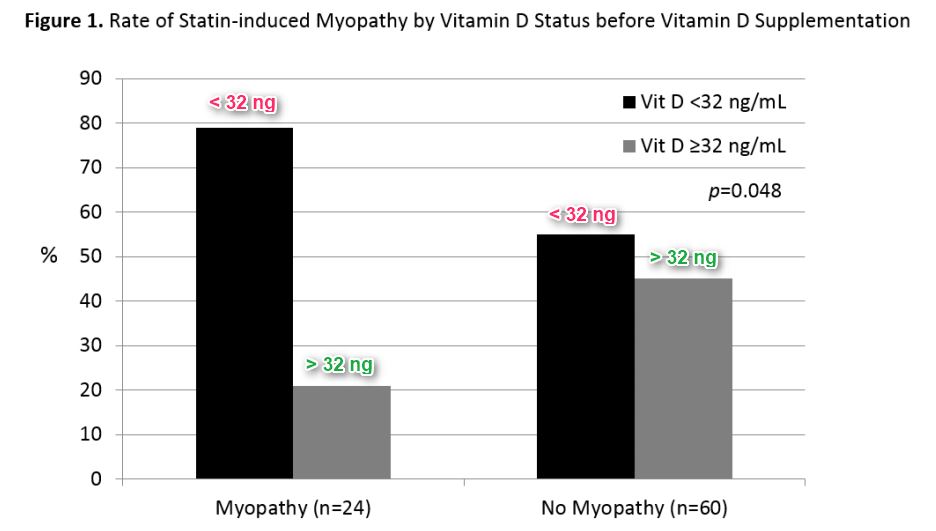 Highlights •Vitamin D status plays an important role in the consideration of statin-induced myopathy.
Highlights •Vitamin D status plays an important role in the consideration of statin-induced myopathy.
•Correction of vitamin D deficiency ( 20 ng/mL) can improve statin tolerance rates.
1. 15% more likely to continue to take statins if they have a monthly 100,000 IU Vitamin D supplement - RCT April 2018 <strong>Effects of vitamin D supplementation on adherence and persistence with long-term statin therapy: Secondary analysis from the randomized, double-blind, placebo-controlled ViDA study</strong> Atherosclerosis, online 7 April 2018, https://doi.org/10.1016/j.atherosclerosis.2018.04.009
Zhenqiang Wua, Carlos A. Camargo Jr.b, Kay-Tee Khaw, Debbie Waayera, Carlene M.M. Lawesa, Les Toopd, Robert Scragga, ,Highlights •Long-term use of statins lowers cholesterol and prevents cardiovascular disease.
•Adherence to taking statins is compromised by adverse effects such as myalgia.
•Adherence and persistence to statin use were assessed in a vitamin D trial.
•Monthly vitamin D3 supplementation improved persistence in taking statins.
Results: Overall, 2494 participants were on long-term statins at follow-up (vitamin D = 1243, placebo = 1251). Compared with placebo, monthly vitamin D supplementation did not improve the proportion with adherence (risk ratio: 1.01, p=0.62) but improved the persistence probability of taking all statins after 24 months (hazard ratio: 1.15, p=0.02). In further analyses, significant differences were observed in the adherence to simvastatin, the first-line statin therapy.
Conclusions: Monthly vitamin D supplementation improved persistence with taking statins over a 24-month measurement period in older adults on long-term statin therapy, especially for participants on simvastatin. The role of vitamin D supplementation as an adjunct therapy for patients on long-term statins merits further investigation.
1. JAMA is finally questioning Statins - 2016 <strong><a href="http://jamanetwork.com/journals/jama/issue/316/19">Nov 15 2016 - JAMA</a> is finally questioning Statins</strong> <strong>Four of the papers in that issue (Free online PDFs)</strong> * What to Believe and Do About Statin-Associated Adverse Effects
Statins for Primary Prevention in Older Adults - Uncertainty and the Need for More Evidence
Evolving Approaches for Statins in Primary Prevention- Progress, but Questions Remain
* Statins for Primary Prevention - The Debate Is Intense, but the Data Are Weak * "The evidence for treating asymptomatic persons with statins does not appear to merit a grade B or even a grade C recommendation.”
“Benefits of any preventive therapy accrue according to the risk of disease (greater benefit in higher-risk patients). The harms of therapy usually distribute equally overall risk levels. Thus, persons at low risk have little chance of benefit but equal chance of harms and thus are more likely to have net harm.”
“Other studies have estimated that closer to 20% of statin users have muscle problems.”
“The decision aid [available from the Mayo Clinic website] shows that of 100 people who take a statin for 5 years, only 2 of 100 will avoid a myocardial infarction, and 98 of the 100 will not experience any benefit.”
“At the same time, 5 to 20 of the 100 will experience muscle aches, weakness, fatigue, cognitive dysfunction, and increased risk of diabetes.”
“The rate of statin use for primary prevention among persons older than 79 years had increased from 8.8% in 2000 to 34.1% in 2012.”
The number needed to treat is 244 for the target group and is much worse for younger women and the elderly.
- Dr. Grimes's comment on JAMA and BMJ Statin studies
Dr.Grime's blog post on the JAMA articles - he has been outspoken about Statins problems and the importance of Cholesterol for many years.
A 10-year study of statins in Europe concluded: “…. the apparent lack of association we observed between CHD mortality and statin utilization….”
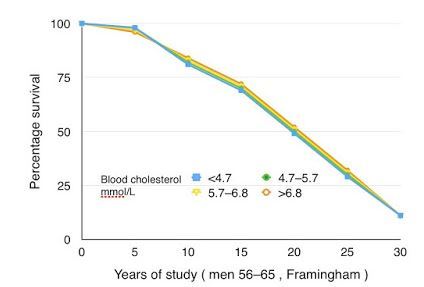
Very small benefit to taking statins - and only to those who had heart problems - June 2017
"Soon after the height of the epidemic in 1970–1980, there was a reduction of deaths in those who received statins, in WOSCOPS from 4% deaths at five years in controls to 3% in those treated. This means that just one man in 100 without a history of CHD who took (prava)statin for five years did not die. Statins are of no value in the elderly - Blog post-Sept 2017 [http://www.drdavidgrimes.com/2017/09/statins-are-of-no-value-in-elderly.html|Dr. Grimes blog post
1. Red yeast rice as good a statin (RCT May 2017) - without the side effects <strong><a href="https://www.ncbi.nlm.nih.gov/pubmed/28521773">Red yeast rice induces less muscle fatigue symptom than simvastatin in dyslipidemic patients: a single center randomized pilot trial.</a></strong> ** <span style="color:#00F;"><i class="fas fa-file-pdf" style="margin-right: 0.3em;"></i><a href="https://d378j1rmrlek7x.cloudfront.net/attachments/pdf/red-yeast-rice.pdf">Download the PDF from VitaminDWiki</a></span><strong> * Good Review of <a href="https://www.consumerlab.com/reviews/_/Red_Yeast_Rice/#whatitis">Red Yeast Rice supplements by ConsumerLabs</a> - June 2017 </strong>Consumer Labs found a 300 to 1 range in the active ingredient between the supplements
Nature's Plus and HPF Cholestene had good amounts
1. Statins were developed as antibiotics, and it was later noticed that statins reduce cholesterol
50X market for a drug taken daily than if only taken about 1/50 of the year
1. See also <a href="/pages/cholesterol/">Cholesterol</a> in VitaminDWiki
1. Magnesium is better than statins in many ways - 2004 <strong>Comparison of mechanism and functional effects of magnesium and statin pharmaceuticals</strong> ** [Chart from Grassroots Health](http://campaign.r20.constantcontact.com/render?m=1102722411090&ca;=db0ea5b4-f32a-4a36-81df-c94ca651f583) 2019 **<img src="https://d378j1rmrlek7x.cloudfront.net/attachments/jpg/mg-statin-rosanoff.jpg" alt="image" width="600">
102 references to the 2004 study as of Aug 2019
{FONT( size="16")}** 📄 Download the PDF from VitaminDWiki__{FONT}
1. There have been <span style="color:#00F;"><!-- {SQL(db=>vitamind)}SELECT hits FROM tiki_pages WHERE page_id=444{SQL} --></span> visits to this page
