Response to infant 2,000 IU Vitamin D daily was in 194 ng, monthly dosing was 20% less – RCT
Daily vs. monthly oral vitamin D3 for treatment of symptomatic vitamin D deficiency in infants: a randomized controlled trial
J Pediatr Endocrinol Metab . 2023 May 18. doi: 10.1515/jpem-2023-0146 PDF is behind paywall
Anupriya Gora 1, Preeti Singh 2, Ekta Debnath 3, Rajeev Kumar Malhotra 4, Anju Seth 2
Objectives: Compare the efficacy and safety of daily vs. monthly oral vitamin D3 in treating symptomatic vitamin D deficiency in infants.
Methods: 90 infants with symsptomatic vitamin D deficiency were randomized into Daily (D) [46 infants] and Bolus (B) [44 infants] groups to receive oral vitamin D3, daily (2000 IU/day) and bolus (60,000 IU/month) for three months respectively. Both groups received daily oral calcium @50 mg/kg/day. Serum calcium (Ca), phosphate (P), alkaline phosphatase (ALP), 25-hydroxy cholecalciferol [25(OH)D], parathyroid hormone (PTH) levels, urine calcium: creatinine ratio and radiological score were assessed at baseline, 4 and 12 weeks. At the end of 12 weeks, 78 infants were available for evaluation of efficacy and safety of both regimens.
Results: Both regimens led to a statistically significant increase in Ca and P levels and fall in ALP and PTH levels from baseline to 4 and 12 weeks of therapy, with no inter-group difference. Infants in group D had statistically significant higher mean 25(OH)D levels as compared to group B at 4 weeks (group D 130.89 ± 43.43 nmol/L, group B - 108.25 ± 32.40 nmol/L; p - 0.012) and 12 weeks (group D - 193.69 ± 32.47 nmol/L, group B - 153.85 ± 33.60 nmol/L; p<0.001). Eight infants [group D - 6/41 (14.6 %); group B - 2/37 (5.4 %), p=0.268] developed mild asymptomatic hypercalcemia without hypercalciuria at 12 weeks that corrected spontaneously within a week.
Conclusions: Both daily and monthly oral vitamin D3 in equivalent doses are efficacious and safe for treating symptomatic vitamin D deficiency in infants.
Results summary
78 total infants RCT for 12 weeks
| Daily | Monthly bolus |
| 2,000 IU | 60,000 IU |
| 194 ng | 154 ng |
Not mentioned: Infant age, BMI, breastfeeding or mother's supplementation
VitaminDWiki - Infrequent is often be better than daily
- Better than Daily category listing has items along with related searches
More often than monthly (includes chart)
Vitamin D every 25 days may be BETTER than daily – RCT May 2018
Vitamin D dosing - weekly may be better than daily – video Aug 2018
Take vitamin D3 daily or weekly has the following chart
- This chart unrealistically assumes 100% compliance for daily dosing
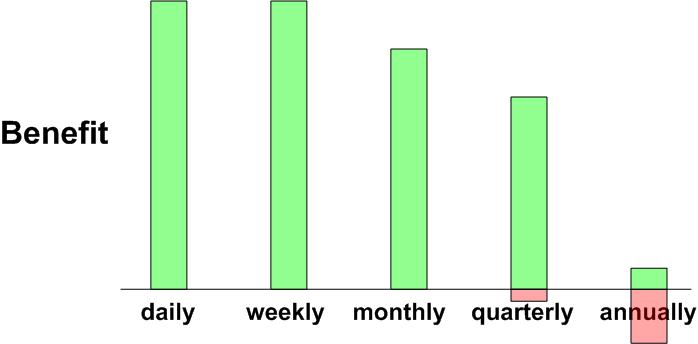 chart was made ~2013
chart was made ~2013
Study on this page must have had an untypically high compliance rate
VitaminDWiki - studies in both categories Infant-Child and any dosing interval
This list is automatically updated
{category}
VitaminDWiki - studies in both categories Infant-Child and nom daily dosing
This list is automatically updated
{category}
VitaminDWiki – Infant-Child category has items and contains
{include}
{include}
VitaminDWiki - Weekly, Monthly Vitamin D are typically better than daily - many studies
Study References
Creo, AL, Thacher, TD, Pettifor, JM, Strand, MA, Fischer, PR. Nutritional rickets around the world: an update. Paediatr Int Child Health 2017;37:84–98. https://doi.org/10.1080/20469047.2016.1248170 . - DOI
Jiang, Z, Pu, R, Li, N, Chen, C, Li, J, Dai, W, et al.. High prevalence of vitamin D deficiency in Asia: a systematic review and meta-analysis. Crit Rev Food Sci Nutri 2021:1–10. https://doi.org/10.1080/10408398.2021.1990850 . - DOI
Surve, S, Chauhan, S, Amdekar, Y, Joshi, B. Vitamin D deficiency in children: an update on its prevalence, therapeutics and knowledge gap s. Indian J Nutr 2017;4:167.
Mehrotra, P, Marwaha, RK, Aneja, S, Seth, A, Singla, BM, Ashraf, G, et al.. Hypovitaminosis d and hypocalcemic seizures in infancy. Indian Pediatr 2010;47:581–6. https://doi.org/10.1007/s13312-010-0131-1 . - DOI
Maiya, S, Sullivan, I, Allgrove, J, Yates, R, Malone, M, Brain, C, et al.. Hypocalcaemia and vitamin D deficiency: an important, but preventable, cause of life-threatening infant heart failure. Heart 2008;94:581–4. https://doi.org/10.1136/hrt.2007.119792 . - DOI
Munns, CF, Shaw, N, Kiely, M, Specker, BL, Thacher, TD, Ozono, K, et al.. Global consensus recommendations on prevention and management of nutritional rickets. J Clin Endocrinol Metab 2016;101:394–415. https://doi.org/10.1159/000443136 . - DOI
Holick, MF, Binkley, NC, Bischoff-Ferrari, HA, Gordon, CM, Hanley, DA, Heaney, RP, Endocrine Society , et al.. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 2011;96:1911–30. https://doi.org/10.1210/jc.2011-0385 . - DOI
From Indian Academy of Pediatrics ‘Guideline for Vitamin D and Calcium in Children’ Committee , Khadilkar, A, Khadilkar, V, Chinnappa, J, Rathi, N, Khadgawat, R, Balasubramanian, S, et al.. Prevention and treatment of vitamin D and calcium deficiency in children and adolescents: Indian Academy of pediatrics (IAP) guidelines. Indian Pediatr . 2017;54:567–73. https://doi.org/10.1007/s13312-017-1070-x . - DOI
Gupta, P, Dabas, A, Seth, A, Bhatia, VL, Khadgawat, R, Kumar, P, et al.. Indian Academy of pediatrics revised (2021) guidelines on prevention and treatment of vitamin D deficiency and rickets. Indian Pediatr 2022;59:142–58. https://doi.org/10.1007/s13312-022-2448-y . - DOI
Tan, JK, Kearns, P, Martin, AC, Siafarikas, A. Randomised controlled trial of daily versus stoss vitamin D therapy in Aboriginal children. J Pediatr Child Health 2015;51:626–31. https://doi.org/10.1111/jpc.12781 . - DOI
Emel, T, Dogan, DA, Erdem, G, Faruk, O. Therapy strategies in vitamin D deficiency with or without rickets: efficiency of low-dose stoss therapy. J Pediatr Endocrinol Metab 2012;25:107–10. https://doi.org/10.1515/jpem-2011-0368 . - DOI
Tannous, P, Fiscaletti, M, Wood, N, Gunasekera, H, Zurynski, Y, Biggin, A, et al.. Safety and effectiveness of stoss therapy in children with vitamin D deficiency. J Paediatr Child Health 2020;56:81–9. https://doi.org/10.1111/jpc.14497 . - DOI
Wadia, U, Soon, W, Chivers, P, Thambiran, A, Burgner, D, Cherian, S, et al.. Randomised controlled trial comparing daily versus depot vitamin D3 therapy in 0-16-year-old newly settled refugees in western Australia over a period of 40 weeks. Nutrients 2018;10:348. https://doi.org/10.3390/nu10030348 . - DOI
Chow, SC, Shao, J, Wang, H, editors. Sample size calculations in clinical research , 2nd ed. USA: Chapman & Hall/CRC Biostatistics Series; 2008.
Kumar, N, Shekhar, C, Kumar, P, Kundu, AS. Kuppuswamy’s socioeconomic status scale––updated for 2007. Indian J Pediatr 2007;74:1131–2.
Thacher, TD, Fischer, PR, Pettifor, JM, Lawson, JO, Manaster, BJ, Reading, JC. Radiographic scoring method for the assessment of the severity of nutritional rickets. J Trop Pediatr 2000;46:132–9. https://doi.org/10.1093/tropej/46.3.132 . - DOI
Lo, SF. Reference intervals for laboratory tests and procedures. In: Kleigman, RM, Behrman, RE, Jenson, HB, Stanton, BP, editors. Nelson text book of pediatrics , 20th ed. Philadelphia: Saunders Elsevier; 2011:3464–72 pp.
Balasubramanian, S. Vitamin D deficiency in breastfed infants & the need for routine vitamin D supplementation. Indian J Med Res 2011;133:250–2.
Najada, AS, Habashneh, MS, Khader, M. The frequency of nutritional rickets among hospitalized infants and its relation to respiratory diseases. J Trop Pediatr 2004;50:364–8. https://doi.org/10.1093/tropej/50.6.364 . - DOI
Aggarwal, V, Seth, A, Marwaha, RK, Sharma, B, Sonkar, P, Singh, S, et al.. Management of nutritional rickets in Indian children: a randomized controlled trial. J Trop Pediatr 2013;59:127–33. https://doi.org/10.1093/tropej/fms058 . - DOI
Saluja, RK, Dewan, P, Gomber, S, Madhu, SV, Bhat, S, Gupta, P. Low dose depot oral vitamin D3 v. daily oral vitamin D3 for treating nutritional rickets: a randomized clinical trial. Br J Nutr 2022;127:1778–83. https://doi.org/10.1017/S0007114521002713 . - DOI
Talaat, IM, Kamal, NM, Alghamdi, HA, Alharthi, AA, Alshahrani, MA. A randomized clinical trial comparing three different replacement regimens of vitamin D in clinically asymptomatic pediatrics and adolescents with vitamin D insufficiency. Ital J Pediatr 2016;42:106. https://doi.org/10.1186/s13052-016-0314-z . - DOI
Hollis, BW, Wagner, CL. Clinical review: the role of the parent compound vitamin D with respect to metabolism and function: why clinical dose intervals can affect clinical outcomes. J Clin Endocrinol Metab 2013;98:4619–28. https://doi.org/10.1210/jc.2013-2653 . - DOI
Vieth, R, Chan, PC, MacFarlane, GD. Efficacy and safety of vitamin D3 intake exceeding the lowest observed adverse effect level. Am J Clin Nutr 2001;73:288–94. https://doi.org/10.1093/ajcn/73.2.288 . - DOI
Gordon, CM, Williams, AL, Feldman, HA, May, J, Sinclair, L, Vasquez, A, et al.. Treatment of hypovitaminosis D in infants and toddlers. J Clin Endocrinol Metab 2008;93:2716–21. https://doi.org/10.1210/jc.2007-2790 . - DOI
Pappa, HM, Mitchell, PD, Jiang, H, Kassiff, S, Filip-Dhima, R, DiFabio, D, et al.. Treatment of vitamin D insufficiency in children and adolescents with inflammatory bowel disease: a randomized clinical trial comparing three regimens. J Clin Endocrinol Metab 2012;97:2134–42. https://doi.org/10.1210/jc.2011-3182 . - DOI
Mittal, M, Yadav, V, Khadgawat, R, Kumar, M, Sherwani, P. Efficacy and safety of 90,000 IU versus 300,000 IU single dose oral vitamin D in nutritional rickets: a randomized controlled trial. Indian J Endocrinol Metab 2018;22:760–5. https://doi.org/10.4103/ijem.ijem8418 . - DOI
Mittal, H, Rai, S, Shah, D, Madhu, SV, Mehrotra, G, Malhotra, RK, et al.. 300,000 IU or 600,000 IU of oral vitamin D3 for treatment of nutritional rickets: a randomized controlled trial. Indian Pediatr 2014;51:265–72. https://doi.org/10.1007/s13312-014-0399-7 . - DOI
Harnot, J, Verma, S, Singhi, S, Sankhyan, N, Sachdeva, N, Bharti, B. Comparison of 300,000 and 600,000 IU oral vitamin-D bolus for vitamin-D deficiency in young children. Indian J Pediatr 2017;84:111–6. https://doi.org/10.1007/s12098-016-2233-9 . - DOI
Shakiba, M, Sadr, S, Nefei, Z, Mozaffari-Khosravi, H, Lotfi, MH, Bemanian, MH. Combination of bolus dose vitamin D with routine vaccination in infants: a randomized trial. Singapore Med J 2010;51:440–5.
Shakiba, M, Pahloosye, A, Mirouliaei, M, Islami, Z. Comparison of two regimens of vitamin D supplementation for vitamin D-deficient neonate s. Singapore Med J 2014;55:266–70. https://doi.org/10.11622/smedj.2014070 . - DOI
Huynh, J, Lu, T, Liew, D, Doery, JC, Tudball, R, Jona, M, et al.. Vitamin D in newborns. A randomised controlled trial comparing daily and single oral bolus vitamin D in infants. J Paediatr Child Health 2017;53:163–9. https://doi.org/10.1111/jpc.13338 . - DOI
Lewis, RD, Laing, EM, Hill Gallant, KM, Hall, DB, McCabe, GP, Hausman, DB, et al.. A randomized trial of vitamin D3 supplementation in children: dose-response effects on vitamin D metabolites and calcium absorption. J Clin Endocrinol Metab 2013;98:4816–25. https://doi.org/10.1210/jc.2013-2728 . - DOI
EFSA Panel on Dietetic Products, Nutrition and Allergies (NDA) . Scientific opinion on the tolerable upper intake level of vitamin D. EFSA J 2012;10:45.
Zittermann, A, Pilz, S, Berthold, HK. Serum 25-hydroxyvitamin D response to vitamin D supplementation in infants: a systematic review and meta-analysis of clinical intervention trials. Eur J Nutr 2020;59:359–69. https://doi.org/10.1007/s00394-019-01912-x . - DOI
McKenna, MJ, Murray, BF. Vitamin D dose response is underestimated by endocrine society’s clinical practice guideline. Endocr Connect 2013;2:87–95. https://doi.org/10.1530/ec-13-0008 . - DOI
