Preterm birth 3X more likely if low vitamin D
Vitamin D plasma concentrations in pregnant women and their preterm newborns.
BMC Pregnancy Childbirth. 2018 Oct 22;18(1):412. doi: 10.1186/s12884-018-2045-1.
Kassai MS1, Cafeo FR2, Affonso-Kaufman FA2, Suano-Souza FI3,4, Sarni ROS1.
📄 Download the PDF from VitaminDWiki
BACKGROUND:
Vitamin D deficiency is a global public health issue. More than half of pregnant women are affected by vitamin D insufficiency/deficiency. Studies suggest an association between low vitamin D concentrations during pregnancy with intrauterine growth restriction and prematurity. This study aimed to describe the concentrations of 25(OH)D (25-hydroxyvitamin D) of mothers who delivered preterm newborns compared to women with full-term pregnancy deliveries, as well as to relate 25(OH)D blood concentrations of mothers with those of their newborns.
METHOD:
This cross-sectional study was conducted with 66 mothers who had given birth to preterm babies and their preterm newborns (PTNB, < 32 weeks), and 92 women who had given birth at the full-term of their pregnancy and their newborns (FTNB). Data were collected on the characteristics of mothers (gestational age, diseases, and habits) and newborns (anthropometry and adequacy for gestational age). Ten milliliters of blood were drawn from the mothers and the umbilical cord of newborns at birth to identify the 25(OH)D, parathyroid hormone, calcium, phosphorus, and alkaline phosphatase concentrations.
RESULTS:
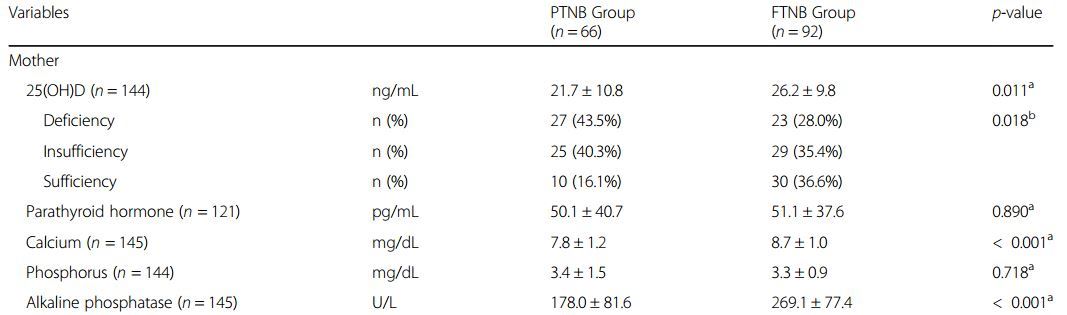
Mothers in the PTNB group had significantly lower mean 25(OH)D blood levels (21.7 ± 10.8 ng/mL vs. 26.2 ± 9.8 ng/mL; p = 0.011) and were three times more likely to have insufficiency when compared to mothers in the FTNB group (OR = 2.993; 95%CI 1.02-8.74). Newborns in the PTNB group also had lower 25(OH)D concentrations compared to FTNB group (25.9 ± 13.9 ng/dL vs. 31.9 ± 12.3 ng/dL; p = 0.009). There was a directly proportional correlation between mother and newborn umbilical cord 25(OH)D concentrations in PTNB (r = 0.596; p < 0.001) and FTNB (r = 0.765; p < 0.001).
CONCLUSION:
Mothers who delivered preterm babies and their preterm newborns had lower 25(OH)D concentrations compared to women who had given birth at the full-term of their pregnancy. In both groups, 25(OH)D concentrations of the mothers correlated directly with those of the newborns, and this correlation was higher in the full-term birth group. Nevertheless, the recommended universal vitamin D supplementation in pregnant women to curb the risk of preterm birth is still incipient. More studies are required to clarify the particularities of vitamin D metabolism further and define the adequate 25(OH)D concentrations throughout pregnancy.
VitaminDWiki - Preterm births are VERY costly – Feb 2017 contains
{include}
VitaminDWiki Pregnancy pages with PRETERM of PRE-TERM in title (61 as of May 2022)
This list is automatically updated
{LIST()}
