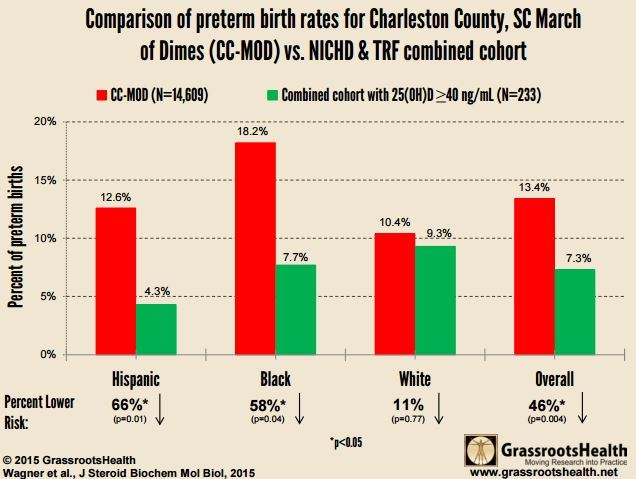
Preterm birth rate reduced 57 percent by Vitamin D
Post-hoc analysis of vitamin D status and reduced risk of preterm birth in two vitamin D pregnancy cohorts compared with South Carolina march of dimes 2009-2011 rates.
J Steroid Biochem Mol Biol. 2015 Nov 7. pii: S0960-0760(15)30124-2. doi: 10.1016/j.jsbmb.2015.10.022. [Epub ahead of print]
Wagner CL1, Baggerly C2, McDonnell S2, Baggerly KA3, French CB2, Baggerly L2, Hamilton SA4, Hollis BW5.
Note that most of the benefit was to women of color - who typically have low vitamin D levels
1 Medical University of South Carolina Children's Hospital, Charleston, SC, United States. Electronic address: wagnercl@musc.edu.
2 GrassrootsHealth, Encinitas, CA, United States.
3 Department of Bioinformatics and Computational Biology, The University of Texas MD Anderson Cancer Center, Houston, TX, United States.
4 Eau Claire Cooperative Health Centers, Columbia, SC, United States.
5 Medical University of South Carolina Children's Hospital, Charleston, SC, United States.
BACKGROUND:
Two vitamin D pregnancy supplementation trials were recently undertaken in South Carolina: The NICHD (n=346) and Thrasher Research Fund (TRF, n=163) studies. The findings suggest increased dosages of supplemental vitamin D were associated with improved health outcomes of both mother and newborn, including risk of preterm birth (<37 weeks gestation). How that risk was associated with 25(OH)D serum concentration, a better indicator of vitamin D status than dosage, by race/ethnic group and the potential impact in the community was not previously explored. While a recent IOM report suggested a concentration of 20 ng/mL should be targeted, more recent work suggests optimal conversion of 25(OH)D to 1,25(OH)2D takes place at 40 ng/mL in pregnant women.
OBJECTIVE:
Post-hoc analysis of the relationship between 25(OH)D concentration and preterm birth rates in the NICHD and TRF studies with comparison to Charleston County, South Carolina March of Dimes (CC-MOD) published rates of preterm birth to assess potential risk reduction in the community.
METHODS:
Using the combined cohort datasets (n=509), preterm birth rates both for the overall population and for the subpopulations achieving 25(OH)D concentrations of ≤20 ng/mL, >20 to <40 ng/mL, and ≥40 ng/mL were calculated; subpopulations broken down by race/ethnicity were also examined. Log-binomial regression was used to test if an association between 25(OH)D serum concentration and preterm birth was present when adjusted for covariates; locally weighted regression (LOESS) was used to explore the relationship between 25(OH)D concentration and gestational age (weeks) at delivery in more detail. These rates were compared with 2009-2011CC-MOD data to assess potential risk reductions in preterm birth.
RESULTS:
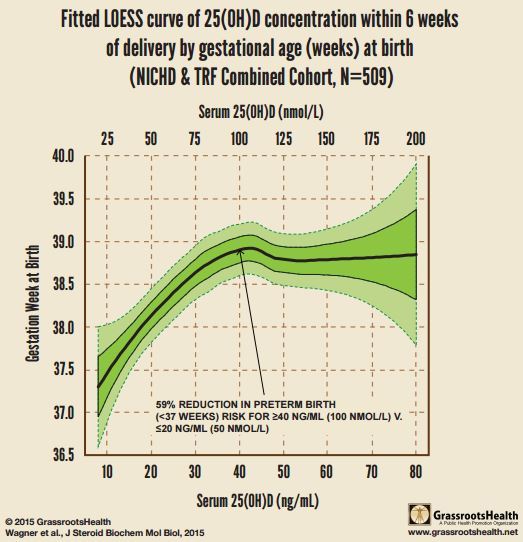
Women with serum 25(OH)D concentrations ≥40 ng/mL (n=233) had a 57% lower risk of preterm birth compared to those with concentrations ≤20 ng/mL [n=82; RR=0.43, 95% confidence interval (CI)=0.22,0.83]; this lower risk was essentially unchanged after adjusting for covariates (RR=0.41, 95% CI=0.20,0.86). The fitted LOESS curve shows gestation week at birth initially rising steadily with increasing 25(OH)D and then plateauing at ∼40 ng/mL. Broken down by race/ethnicity, there was a
79% lower risk of preterm birth among Hispanic women with 25(OH)D concentrations ≥40 ng/mL (n=92) compared to those with 25(OH)D concentrations ≤20 ng/mL (n=29; RR=0.21, 95% CI=0.06,0.69) and a
45% lower risk among Black women (n=52 and n=50; RR=0.55, 95% CI=0.17,1.76).
There were too few white women with low 25(OH)D concentrations for assessment (n=3). Differences by race/ethnicity were not statistically significant with 25(OH)D included as a covariate.
Copyright © 2015. Published by Elsevier Ltd.
PMID: 26554936
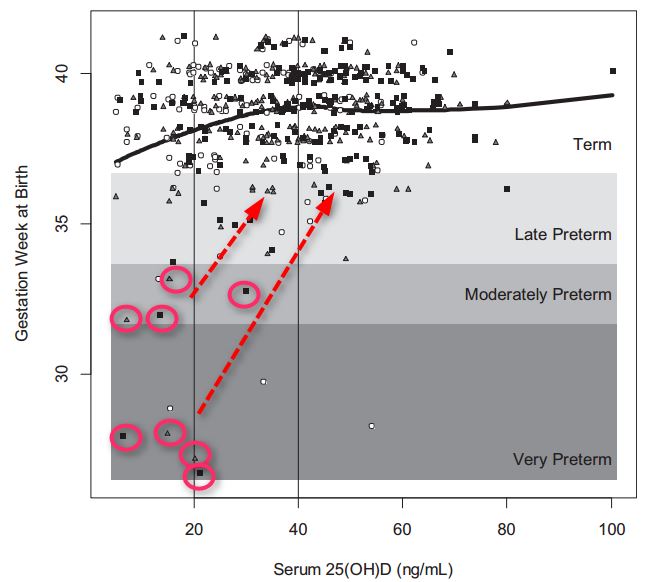
Notice the moderate and very preterms- poor response to 4,000 IU of Vitamin D by several women (black squares)
Suspect that these poor responses could have been avoided if more vitamin D and/or cofactors which increase the response had been give to high-risk women - such as obese
Fig. 1. 25(OH)D concentration within 6 weeks of delivery by gestational age (weeks) at birth (NICHD & TRF, N = 509).
Term birth is 37 weeks of gestation; late preterm birth is 34 to <37 weeks; moderately preterm is 32 to <34 weeks; and very preterm is <32 weeks.
White circles represent women assigned to the control group (400 IU/day);
gray triangles represent women assigned to the 2000 IU/day treatment group; and
solid black squares represent women assigned to the 4000 IU/day treatment group.
Black line represents fitted LOESS curve.
📄 Download the PDF from VitaminDWiki
See also VitaminDWiki
Healthy pregnancies need lots of vitamin D has the following summary
{include}
Intervention during Pregnancy studies on VitaminDWiki
{category}
