Vitamin D Pregnancy Protocol in a US hospital (40 ng)
Vitamin D Testing and Treatment Protocol
MUSC Department of Ob-Gyn, Maternal-Fetal Medicine Division
South Carolina
BACKGROUND:
A rapidly evolving body of literature, including sentinel studies done by Carol Wagner and colleagues here at MUSC, has documented both the perinatal and child health benefits of achieving therapeutic 25-0H Vitamin D levels (> 40 ng/ml) during pregnancy. Simultaneously, we are aware that almost 80% of our obstetrical population and virtually 100% of our African-American obstetrical population have 25-0H Vitamin D levels that fall below this therapeutic threshold.
Studies by Wagner as well as others have demonstrated significant reductions in the rate of preterm birth among pregnant women who achieve 25-0H Vitamin D levels greater than 40 ng/ml via prenatal supplementation. Vitamin D deficiency and appropriate supplementation may both explain and help improve the high rates of premature birth in our community and region. Other potential perinatal benefits include the possibility of reducing the incidences of Gestational Diabetes, pre-eclampsia, depression and postpartum depression.
Perinatal supplementation and achievement of therapeutic maternal 25-0H Vitamin D levels has also been associated with improved neonatal and childhood immune function. This improved immune function has translated into reduced risks of upper respiratory infection, bronchitis, ear infections and pneumonia. A soon to be published prospective randomized trial will demonstrate a significant reduction in childhood asthma among the children of women who achieve therapeutic Vitamin D levels during pregnancy.
Figure 1. illustrates the potential disease incidence prevention associated with increasing the 25-0H Vitamin D level to > 40 ng/ml. The recommended range for 25-0H Vitamin D is between 40-60 ng/ml.
PROTOCOL:
A 25-0H Vitamin D level will be obtained routinely as part of the New OB prenatal blood work.
If the 25-0H Vitamin D level is < 40 ng/ml you can begin supplementation with 4000-5000 IU of Vitamin D per day.
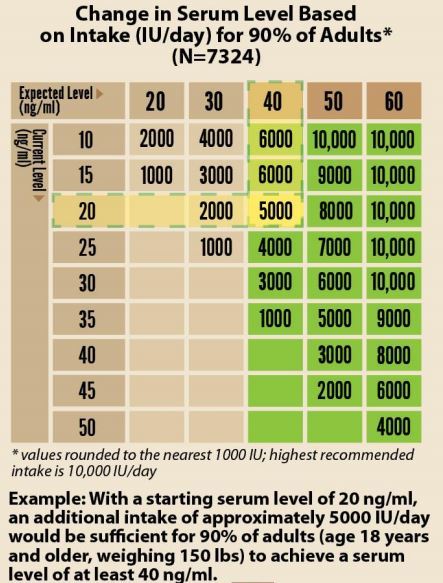
More specific supplementation dosing can be achieved with the use of Figure 2. which provides a recommended daily dose of 25-0H Vitamin D based on the initial starting level and anticipating a goal of > 40 ng/ml.
Using the chart in Figure 2. to get 90% of the patients from an initial level of 20 ng/ml (many are even lower) to a level of 45 ng/ml, the likely required daily dose will be 5000 IU / day.
GrassrootsHealth through the Protect Our Children NOW! project has provided free Vitamin D (5000 IU capsules) for your patients that they can obtain by taking their prescription to the Rutledge Tower Pharmacy to have it filled.
The 25-0H Vitamin D level should be rechecked along with the routine Glucola screen at 24-28 weeks gestation. Vitamin D dosing adjustments can be made based on this mid-trimester measurement.
The 25-0H Vitamin D level should be checked a third time at 34-36 weeks gestation along with the third trimester CBC and / or STD blood work. A further dosage adjustment can be made at that time if required.
The 25-0H Vitamin D level is covered by insurance as part of the prenatal panel. Follow up testing is also covered if "Vitamin D Deficiency" is added to the problem list if the Vitamin D level is < 40 ng/ml.
TOXICITY:
Vitamin D toxicity is an uncertain entity and rarely encountered. Most labs will identify a 25-0H Vitamin D level of > 100-120 ng/ml as being potentially toxic. Toxicity is typically defined by elevations of the serum or urinary calcium levels and potentially kidney stones. We have not encountered any Vitamin D levels that high either before or after supplementation. Nor have we encountered any side effects attributed to Vitamin D supplementation. This experience includes several high dose Vitamin D supplementation trials by Dr. Wagner. Published literature shows no toxicity under 200 ng/ml and 30,000 IU/day. This greatly exceeds any dosing regimen we would have.
It is important to perform follow up Vitamin D testing as there can be significant individual variation in the response to Vitamin D supplementation.
MANAGEMENT TIPS:
Obviously not all patients show up in the first trimester for their initial prenatal visit. Additionally, at MUSC we see a number of women referred at later gestational ages due to high risk conditions. Many of these women will have already had their prenatal blood work performed.
If these women are seen later in pregnancy, please obtain a 25-0H Vitamin D level if not already performed. Based on results, initiate aggressive supplementation as soon as possible. With daily supplementation maternal Vitamin D levels can normalize as quickly as 2 months . Vitamin D is believed to prevent preterm birth through its anti-inflammatory and immune modulating properties. Therefore, supplementation even in just the third trimester is still beneficial.
Another inevitable issue is when and how to initiate supplementation. Selecting a dose based on measured Vitamin D levels is ideal, but misses the opportunity to discuss and initiate treatment at that first prenatal visit. That missed opportunity becomes more problematic when it is remembered that 80% of all our patients and 100% of our African- American patients are Vitamin D deficient (<40 ng/ml).
What I do is inform my patients of the above reality and prescribe 2000 IU of 25-0H Vitamin D capsules. I recommend that my patient take 2 / day (4000 IU) until their Vitamin D level is available. If worse than anticipated I can increase my advisory to 3 / day and if better than anticipated I can decrease to 1/day. If the level is > 40 ng/ml, I advise that she take one supplement every other day. If the patient decides to get the free supplements from Rutledge Tower Pharmacy (5000 IU/capsule) I advise them to take 1/day until her Vitamin D level is available. At that point supplementation can be doubled if severely deficient or cut down to once every 2 or 3 days if levels are better than expected.
PROJECT FOLLOW-UP:
In a collaboration between MUSC and GrassrootsHealth we will use electronic medical records and perinatal outcome summary data to assess the uptake and impact of the Vitamin D testing and supplementation program on Obstetrical outcomes at MUSC.
As a greater number of obstetrical patients are tested for Vitamin D deficiency and appropriately supplemented to achieve levels > 40 ng/ml we expect to see measurable reductions in our institution's preterm delivery rate as well as potentially other perinatal measures.
Figure F1
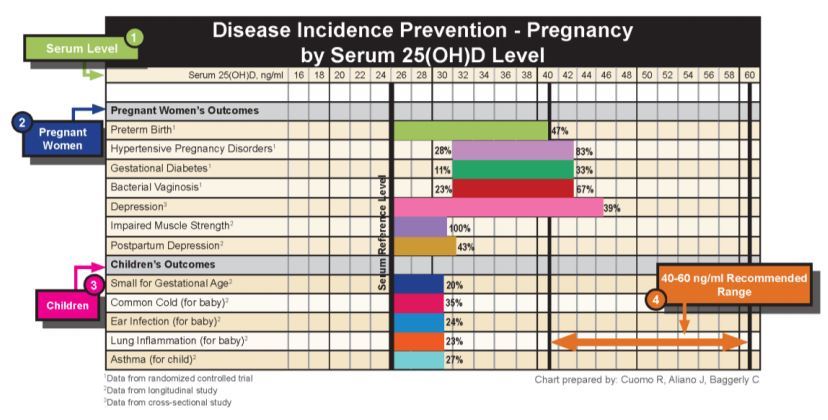
Figure F2
(signed) Dr. Rodger Newman, Professor and Maas Endowed Chair of Reproductive Sciences
📄 Download the Protocol PDF from VitaminDWiki
This is a great first protocol
Future protocols should also address
- Get Vitamin D levels high as soon as possible (loading dose: 1 week, vs 8+ weeks)
- With daily dosing an 8 week delay is too long
- Cofactors (Magnesium, Omega-3, etc.)
- To balance the increased vitamin D
- To improve health during and after pregnancy
- Other forms/types of vitamin D are needed if:
- Dislike/unable to take capsules
- Have a gut problem
- Have a liver or kidney problem
- Unlikely to take the supplement daily (poor compliance)
- Vegeterian
- Start with more vitamin D if person is likely to be deficient
- Dark Skinned
- Obese
- Indoors a lot
- Wear concealing clothing
- One or more Vitamin D diseases in person or in family
- which is a indication of poor vitamin D genes
Season - if at high latitude
Start earlier in pregnancy - before conception is great
Encourage vitamin D after pregnancy- for both mom and infant
See also VitaminDWiki
Healthy pregnancies need lots of vitamin D has the following summary
{include}
and
One pill every two weeks gives you all the vitamin D most adults need
Vitamin D is being used to prevent premature births – Baggerly interview – Dec 2015
Ensure a healthy pregnancy and infant with as little as $20 of Vitamin D
Near the end of pregnancy 50,000 IU vitamin D weekly was great – RCT April 2013
Many groups of pregnant women are at high risk of being vitamin D deficient – Jan 2013
Overview Vitamin D Dose-Response
Reasons for low response to vitamin D
Healthy in Seven Days - Loading dose of Vitamin D – book 2014
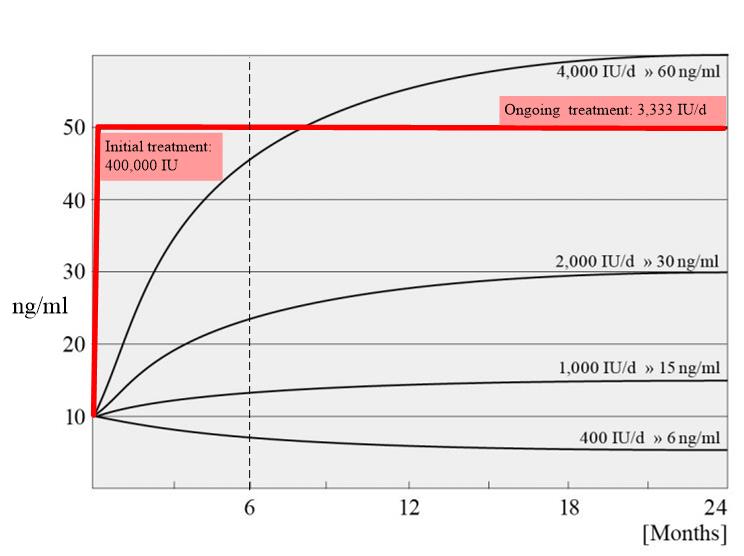
Restocking vitamin D quickly gets you to a good level during pregnancy (from the book: Healthy in Seven Days)
The articles in Pregnancy AND Intervention are here:
{category}
