Interactions between Magnesium, Vitamin D, and Calcium
Essential Nutrient Interactions: Does Low or Suboptimal Magnesium Status Interact with Vitamin D and/or Calcium Status?
American Society for Nutrition. Adv Nutr 2016;7:25–43; doi:10.3945/an.115.008631.
Andrea Rosanoff,3* Qi Dai,4 and Sue A Shapses5
3Cente.r for Magnesium Education and Research, Pahoa, HI; 4Vanderbilt Epidemiology Center, Department of Medicine, School of Medicine, Vanderbilt University, Nashville, TN; and 5Rutgers University, New Brunswick, NJ
 The items in both categories of Magnesium and Calcium are listed here:
{category}
The items in both categories of Magnesium and Calcium are listed here:
{category}
📄 Download the PDF from VitaminDWiki
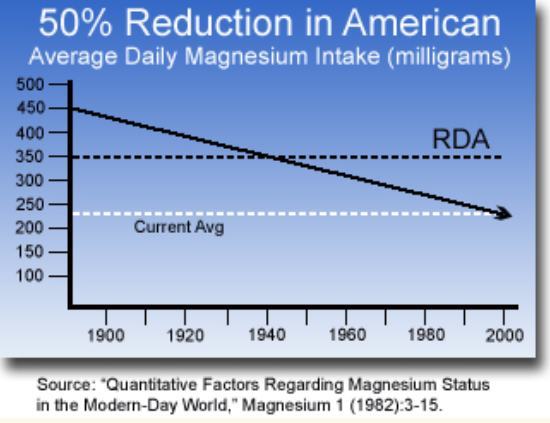
Although much is known about magnesium, its interactions with calcium and vitamin D are less well studied. Magnesium intake is low in populations who consume modern processed-food diets. Low magnesium intake is associated with chronic diseases of global concern [e.g., cardiovascular disease (CVD), type 2 diabetes, metabolic syndrome, and skeletal disorders], as is low vitamin D status. No simple, reliable biomarker for whole-body magnesium status is currently available, which makes clinical assessment and interpretation of human magnesium research difficult. Between 1977 and 2012,
US calcium intakes increased at a rate 2-2.5 times that of magnesium intakes , resulting in a dietary calcium to magnesium intake ratio of >3.0. Calcium to magnesium ratios <1.7 and >2.8 can be detrimental, and optimal ratios may be ~2.0. Background calcium to magnesium ratios can affect studies of either mineral alone. For example, US studies (background Ca:Mg >3.0) showed benefits of high dietary or supplemental magnesium for CVD, whereas similar Chinese studies (background Ca:Mg <1.7) showed increased risks of CVD. Oral vitamin D is widely recommended in US age-sex groups with low dietary magnesium. Magnesium is a cofactor for vitamin D biosynthesis, transport, and activation; and vitamin D and magnesium studies both showed associations with several of the same chronic diseases. Research on possible magnesium and vitamin D interactions in these human diseases is currently rare. Increasing calcium to magnesium intake ratios, coupled with calcium and vitamin D supplementation coincident with suboptimal magnesium intakes, may have unknown health implications. Interactions of low magnesium status with calcium and vitamin D, especially during supplementation, require further study.
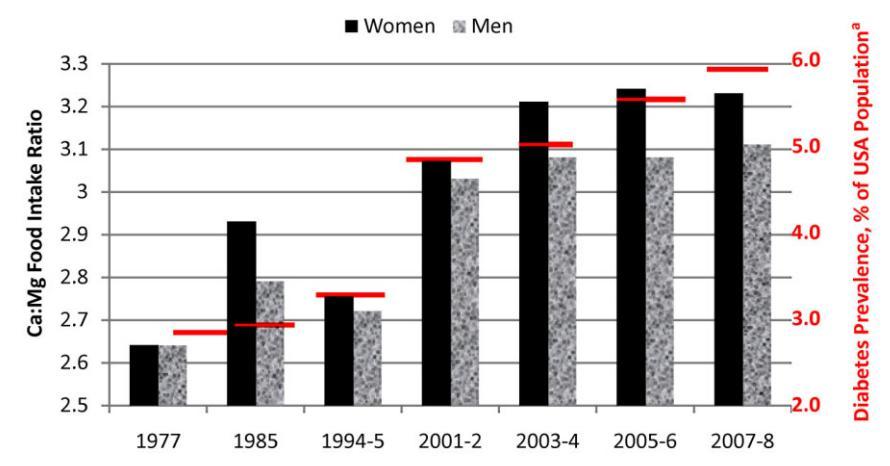
Increased Ca/Mg ratio over time, especially for women figure 2
Introduction
The role of magnesium in health physiology and metabolism has been well studied; however, its interactions with calcium and vitamin D, especially when magnesium is inadequate, are less well known. This lack of data is in contrast with the extensive literature on interactions of vitamin D with calcium. This article reviews general intakes of and assessment issues for dietary magnesium and explores interactions of magnesium with the nutrients calcium and vitamin D.
Magnesium
Health effects of inadequate magnesium intake
Magnesium status is low in populations who consume modern processed-food diets that are high in refined grains, fats, and sugars (1). Low magnesium status may lead to chronic diseases (Table 1) (2-36). For example, studies have linked low magnesium status to a greater risk of metabolic syndrome (MetS) 6 (24, 27-31), type 2 diabetes (T2D) (17, 37, 38), cardiovascular disease (CVD) (7, 8, 39), skeletal disorders (32, 34, 36, 40-42), chronic obstructive pulmonary disease (43-47), and possibly some cancers (48-51). Low magnesium status has also been associated with depression (52-55) and decreased cognition (56, 57). These diseases have large human and financial costs, as reported in the Global Burden of Disease Study (58). Therefore, there is a need to explore the consequences of suboptimal magnesium status in populations consuming modern processed-food diets.
Something wrong with text extraction – lots of text is missing here
Magnesium physiology
In human adults, whole-body magnesium content is ~24 g (1 mol). Approximately half of this magnesium is present in bone and the other half is found in soft tissue, with <1% present in blood. Serum magnesium represents ~0.3% of whole-body magnesium (73). Although the measurement of serum magnesium is useful in medical diagnoses of clinically severe magnesium deficiency (74), it may not reliably represent whole-body magnesium status. The healthy human body tightly regulates blood magnesium concentrations, maintaining a “normal” range even in times of low dietary magnesium intakes and/or excessive magnesium excretion. Both bone and soft tissue intracellular magnesium concentrations may be depleted (or depleting) while serum/plasma magnesium concentrations remain in the “healthy” range (75). Pig studies in the 1970s (76) showed that magnesium-deficient pigs had reduced intracellular magnesium from soft tissues and erythrocytes as well as reduced bone magnesium content, although serum magnesium remained at the normal concentration. This magnesium physiology appears to be similar in humans (75). Thus, in populations who have chronically low dietary magnesium intakes and high dietary calcium to magnesium ratios, such as in the United States (discussed later in this review), people who are nonsymptomatic with normal serum magnesium concentrations may have dangerously low tissue magnesium concentrations and decreasing bone magnesium content. This condition has been termed “chronic latent magnesium deficit” (CLMD) (75) and is further considered later in this review.
Magnesium status assessment
There is currently no simple, reliable biomarker for whole- body magnesium status, and the challenges of assessing magnesium status can impede the interpretation of human magnesium research. The currently available forms of assessment are described below.
Magnesium load retention test as a biomarker . The magnesium retention test is cumbersome but is considered the most reliable research indicator of whole-body magnesium status. In this test, an intramuscular or intravenous infusion of magnesium (the magnesium “load”) is given to a subject, followed by urine collection for $24 h. The percentage of the magnesium load excreted in the urine is measured, and the percentage of the magnesium load retained by the body during the length of the urine collection is calculated. Subjects who are magnesium replete are expected to retain small percentages of the magnesium load, whereas subjects with magnesium deficits are expected to show larger retention percentages.
FIGURE 2 Increasing calcium to magnesium ratios in US women (A) and men (B) from food alone (all adults) and from food plus supplements (supplement users only). Data are from the USDA Agricultural Research Service Food Surveys for 1977 and 1985 (63, 64), 1994-1995 (65), and 2001-2012 (59, 66-70). In US adults, 23% of women and 22% of men use dietary supplements that contain magnesium (59). A calcium to magnesium ratio >2.8 interacts with a functional polymorphism in colorectal neoplasia risk (71).
Researchers use different retention percentages to define “magnesium deficit” with these load tests (77-81) (Table 2). In addition to its poorly defined cutoffs and its cumbersome nature, the magnesium load retention test cannot be used in patients with chronic kidney disease or in individuals with critical illnesses (82).
Serum magnesium and CLMD . The largest data source for serum magnesium reference ranges is derived from a 19711974 US study in 15,820 presumably healthy individuals aged 1-74 y (83), a population who may not have been fully magnesium replete (75). Serum magnesium clinical reference ranges in the United States are not evidence based and may include a subpopulation of unknown size with CLMD. The lower serum magnesium range for healthy individuals has been questioned because some studies suggested that the currently accepted lower range correlates with negative health outcomes. The criterion for low “normal” serum magnesium as a definition for hypomagnesemia varies widely in studies (Table 2) as well as among clinical laboratories, ranging from as low as 0.6 mmol/L to as high as 0.75 mmol/L (83-85, FH Nielsen, unpublished data, 2015) (Table 3). Increasing the low-normal boundary of serum magnesium to a range of 0.80-0.85 mmol/L to better accommodate the CLMD subpopulation has been suggested (75, 84, 86).
Magnesium load retention vs. serum magnesium as a biomarker . Data from a small (n = 16) study in Wales reported both individual serum magnesium and magnesium load retention test results for hospitalized patients (77). The study showed that differentiation between depletion and nondepletion (via the magnesium load retention test) was meaningful only when a serum magnesium value of $0.85 mmol/L was used as the cutoff to define hypomagnesemia (77). Serum magnesium may not be a reliable marker of magnesium status in clinical settings or research studies partly because the accepted “normal range” in North America is not evidence based. For example, individuals in the serum magnesium range from 0.6 or 0.7 up to 0.84 mmol/L are labeled “normomagnesemic” and are thus assumed to be non-magnesium depleted when, in fact, a large portion of these persons might more accurately be designated as magnesium depleted. Well-designed studies comparing results of individual magnesium load retention tests with serum magnesium concentrations are needed to fully explore whether increasing the lower cutoff is warranted.
Value of serum magnesium as a biomarker . Additional research is needed on the proper use of serum magnesium as a biomarker of magnesium status and the possible impact of CLMD. Studies are needed to address whether there are physiologic changes to bone or soft tissue that are associated with low magnesium intakes but normal serum magnesium concentrations. In addition, proton pump inhibitors are widely prescribed and these medications significantly increase the risk of hypomagnesemia in the general population (87). Recent analysis of human magnesium balance studies suggests that serum magnesium may represent long-term, severely magnesium-deficient status, because it does not respond as rapidly or as flexibly to magnesium intake as does urinary magnesium (FH Nielsen, unpublished data, 2015). At this time, serum magnesium values can be considered a useful, but not an absolutely reliable, indicator of whole-body magnesium status when interpreting human magnesium research.
Urinary magnesium . Urinary magnesium increases with high magnesium diets and/or oral magnesium supplementation and remains low during times of low magnesium intake (88, 89). A study by Joosten et al. showed that urinary magnesium excretion is an indicator of intestinal magnesium absorption and is thus a potential marker of CVD risk (90) that is perhaps more reliable than serum magnesium (2, 89).
Calcium
Magnesium interactions with calcium
In humans, it has long been known that hypomagnesemia often presents with hypocalcemia (91) and that calcium intake affects magnesium retention and vice versa (see below). Intricate interactions of magnesium and calcium are basic to all living cells and some are quite early on the evolutionary scale (92). For example, it was shown in the amoeba almost a century ago (93) that magnesium prevents calcium entry into the cell when calcium is present in excess. In addition, magnesium prevents calcium exit during calcium-deficient conditions and “in the presence of magnesium, less calcium is required for optimum movement” (93) in these one-celled animals. These basic cellular calcium-magnesium interactions are at work in human cells (94, 95), in which the imbalance of these 2 essential minerals can give rise to cellular phenotypes manifesting the physiologic symptoms of modern chronic diseases (96).
Change in calcium intake may affect magnesium balance and vice versa
Two comprehensive reviews of pre-1970 human studies on the impact of calcium intake on magnesium balance showed that with magnesium intakes <4 mg • kg"1 • d"1, there was magnesium loss regardless of calcium intake; however, when magnesium intakes were $5 mg • kg" 1 • d" \ increases in calcium intake resulted in less magnesium retention (97, 98). Note that the current adult DRIs for magnesium are based on intakes of 4.3 mg • kg" 1 • d"1 to maintain balance in healthy adults (60), and human studies found this factor to be 2.36 mg • kg"1 • d"1 (95% CI: 1.58, 3.38 mg • kg"1 • d"1) (99). Calcium intakes as high as 2-2.5 g/d caused lower magnesium absorption in 2 small, earlier studies (100, 101). In a study in teenaged girls, magnesium balance was negative with calcium intakes of 1800 mg/d; however, compared with positive magnesium balance results with 800 mg calcium/d, the differences in magnesium absorption, excretion, and balance were not significant in this small crossover trial (n = 5) (102). In a randomized clinical trial conducted in New Zealand menopausal women, researchers observed that the consumption of milk high in calcium or supplementation (1200 mg calcium) with or without magnesium significantly increased magnesium urinary excretion during the 8 h of consumption (103). Another trial in Thai menopausal women found that supplementation with 750 mg calcium for 3 mo led to a 15% increase in urinary excretion of magnesium, but the increase was not significant (104). A third trial conducted in women aged 24-34 y in The Netherlands found that 400 mg calcium in the form of salts or in cheese increased urinary excretions of magnesium (105). Although these findings are not entirely consistent and no dietary magnesium intakes were measured, these clinical trials indicate that high calcium supplementation may affect urinary magnesium excretion in women aged $24 y.
With regard to magnesium intakes affecting calcium balance, earlier studies showed that healthy adults with both low magnesium and low calcium intakes had a negative calcium balance, which was attenuated and reversed when magnesium intake improved (97, 98). More recently, a randomized trial of magnesium supplementation, conducted in Ireland, found that increasing magnesium intake from 11 mmol/d (264 mg/d) to ~22 mmol/d (528 mg/d) for 28 d did not increase urinary excretion of calcium among women aged 20-28 y (106). Another randomized trial conducted in women aged ~40 y in South Africa also found that magnesium supplementation at 250 mg/d (10.3 mmol/d) did not change urinary excretion of calcium, but it reduced fractional absorption of calcium by 23.5%, which was not caused by direct competition between the 2 minerals (107). However, a third trial conducted in men aged 21-42 y in Japan found that supplementation of 250 mg magnesium (as MgO) significantly elevated the urinary excretion of calcium (108). Note that the Japanese population has a low calcium to magnesium ratio (109).
High calcium to magnesium ratios in the United States
Over the past $30 y in the United States, both dietary calcium and magnesium intakes have increased. However, calcium intakes increased at a rate 2-2.5 times that of dietary magnesium intakes, giving rise to an increasing calcium to magnesium ratio in this population (Figure 2). This trend appears to have either reversed or leveled off during 20112012, but further surveys are needed to determine which trend, if either, is occurring. Compared with the increases in mean magnesium intakes in US adults (increases of 15.5% and 25% for men and women, respectively; see above) from 1977 to 2011-2012, mean calcium intakes from these same surveys (59, 63-70) showed increases of 37% in men (from 815 to 1117 mg calcium/d; r = 0.92, P = 0.0005) and 51% in women (from 570 to 862 mg calcium/d; r = 0.95, P = 0.0001). As a result, the mean calcium to magnesium ratio in US adults increased significantly between 1977 and 2012 (for men: r = 0.92, P = 0.0005; for women: r = 0.89, P = 0.001); in 2001, the mean calcium to magnesium ratio increased from <3.0 to >3.0 for both men and women (Figure 2). Increases in mean calcium and magnesium intakes were 3-6 and 1.5-3 times the increases in kilocalories, respectively (17% for women and 6% for men). This high calcium to magnesium ratio appears to be exacerbated by supplement usage, especially in women (110).
Impact of calcium to magnesium ratios on disease outcomes
Traditional advice is to maintain dietary calcium to magnesium ratios close to 2.0 for optimal health outcomes in humans (111) came from knowledgeable speculation that was not supported by any experimental evidence. In 2007, a colorectal neoplasia study by Dai et al. (71) provided evidence for an optimal dietary calcium to magnesium ratio (i.e., <2.8). In this case-control study (n = 2204), the risk of colorectal adenoma was reduced only in subjects with a calcium to magnesium ratio <2.8, although this risk decreased with increasing total magnesium intakes regardless of confounders. Among those with a calcium to magnesium ratio >2.8, total magnesium intake was not related to risk, although increasing total calcium intake showed a trend toward greater risk. Thus, total calcium intakes may be related to a reduced risk of colorectal adenoma only when calcium to magnesium ratios are <2.8. Dai et al. also found a nutrient-gene interaction [i.e., transient receptor potential melastatin 7 (TRPM7) with dietary Ca:Mg] in relation to the risk of both colorectal adenoma and hyperplastic polyps. TRPM7 is a newly identified gene that is essential to magnesium homeostasis, and the Thr14821le rs8042919 polymorphism in the TRPM7 gene is functional. Individuals with the 14821le allele and calcium to magnesium ratios >2.8 had a 60% greater risk of colorectal adenoma and an 85% increased risk of hyperplastic polyps than those without the 14821le allele in the TRPM7 gene (71).
A follow-up randomized clinical trial in 930 subjects (112) found that long-term calcium treatment (1200 mg/d over a 4-y period) significantly reduced colorectal adenoma recurrence risk but only when the baseline calcium to magnesium ratio was <2.6 (RR: 0.68; 95% CI: 0.52, 0.90). By contrast, calcium supplementation had no effect among subjects when the calcium to magnesium ratio was >2.6 (RR: 0.98; 95% CI: 0.75, 1.2). This effect modification by the calcium to magnesium ratio cannot solely be attributed to the baseline dietary intake of calcium or magnesium (112). These results show that the interpretation of studies measuring either calcium or magnesium intake alone is difficult, especially because food sources of calcium and magnesium are positively correlated (113).
Opposite influence of low calcium to magnesium ratios on health outcomes
Just as a calcium to magnesium ratio >2.6-2.8 can result in a detrimental effect, baseline calcium to magnesium ratios <2.0 may also have a detrimental effect. The Shanghai Women’s Health Study and the Shanghai Men’s Health Study are 2 population-based cohorts with >130,000 participants. These studies were conducted in a Chinese population in whom magnesium intakes are comparable to the US population; however, the median calcium to magnesium ratio (~1.7) is much lower than the calcium to magnesium ratio in the US population ($3.0) (114). In this population with very low calcium to magnesium ratios, magnesium intakes at or above RDA levels were associated with an increased risk of total mortality in both women and men. This is in contrast with US studies undertaken with a high background calcium to magnesium ratio ($3.0), which showed decreased mortality when magnesium intakes were increased by 200-375 mg/d (7, 13, 115, 116).
Furthermore, in the Chinese studies, among those with calcium to magnesium ratios >1.7, a magnesium intake $320 mg/d was significantly associated with reduced risks of total mortality and mortality due to ischemic heart disease (IHD) among men and mortality due to all cancers among women. By contrast, when calcium to magnesium ratios were #1.7, magnesium intake $320 mg/d was significantly related to increased risks of all-cause mortality and mortality due to CVD and colorectal cancer among women.
In addition, one study measuring both serum calcium and magnesium found that elevated serum magnesium was significantly associated with a lower risk of high-grade prostate cancer (OR: 0.26; 95% CI: 0.09, 0.85), whereas an elevated serum calcium to magnesium ratio was associated with an increased risk of high-grade prostate cancer (OR: 2.81; 95% CI: 1.24, 6.36) adjusted for serum calcium and magnesium (50). Another study with an examination of serum concentrations of calcium, magnesium, and phosphorus in a large population of whites and African Americans (27%) indicated that when serum magnesium is low and calcium and phosphorus are higher, this leads to a greater risk of heart failure (117). With the use of NHANES data, a recent study found that women who met the RDA for both magnesium and calcium had the greatest reduced odds of MetS (OR: 0.59; 95% CI: 0.45, 0.76). In men, meeting the RDA showed no association with MetS, but those with intakes in the highest quartile for magnesium ($386 mg/d) and calcium ($1224 mg/d) had lower odds of MetS (OR: 0.74; 95% CI: 0.59, 0.93) (118).
In skeletal studies, magnesium depletion was associated with decreased osteoblastic and increased osteoclastic activity (40), lower bone mineral density (BMD) (32, 34, 36), and fragility. Most studies suggest that magnesium intake favorably alters BMD. In a study by Orchard et al. (33) that used data from the Women’s Health Initiative, a lower magnesium intake was associated with lower BMD of the hip and whole body, as expected; however, this did not translate into an increased risk of hip or total fractures. In the same study, excess magnesium appeared to be detrimental to bone and fracture risk of the forearm and wrist. The authors speculated that greater physical activity, made more likely by increased magnesium intakes, was responsible for this unexpected result. It would have been interesting to see whether calcium intakes and calcium to magnesium ratios might have further explained this detrimental outcome of higher magnesium intakes (33).
Together, these findings suggest that any magnesium or calcium effect is dependent on the intake amount of calcium or magnesium, respectively, and thus on the calcium to magnesium ratio. Furthermore, dietary intake studies of either magnesium or calcium alone may be unwittingly confounded by the unmeasured calcium or magnesium. These findings are relevant to the US population (and other populations experiencing an increased Ca:Mg) because the calcium to magnesium ranges that show these modifying effects (i.e., <1.7 in the Chinese study and >2.6-2.8 in the US studies) are well below the current mean calcium to magnesium ratio in US adults, which was 3.1-3.2 in 2007-2008 (119) and increased to 3.3-3.4 in 2009-2010 (Figure 2) from food intakes alone (i.e., not including supplements).
It appears that too much or too little of either calcium or magnesium might not be beneficial and there may be an optimal range of human calcium and magnesium intake. Studies in this area might expand our knowledge of when supplementation with magnesium or calcium is helpful or detrimental. Long-term exposure to a diet with a high calcium to magnesium ratio, which is common in the United States, may lead to public health concerns and requires further study.
Vitamin D
Magnesium interactions with vitamin D
There has been a recent surge of positive studies for several human health issues with vitamin D in the peer-reviewed literature, giving rise to medical prescriptions for and over-the-counter sales of high doses of vitamin D to increase serum vitamin D concentrations. With early studies showing an effect of magnesium on vitamin D status in patients with clinically diagnosed magnesium deficiency (23, 120-125), it is important to review the possible effects of both nutrients on one another in a general population with largely suboptimal magnesium intake (see above).
Vitamin D Status
Vitamin D deficiency causes rickets in children and osteomalacia in adults (126). Many epidemiologic studies suggest that low vitamin D status may also be associated with allcause mortality (127-129) and with the risk of nonskeletal chronic diseases such as T2D (130-132), CVD (133, 134), and colorectal cancer (135-137). However, findings have not been entirely consistent (138-141). Large-scale clinical trials of vitamin D supplementation are ongoing (138, 139, 142). Despite food fortification and dietary supplementation, low vitamin D status (<20 mg/L or <50 nmol/L; Table 3) is still relatively common in the United States (143). In addition, there is large interindividual variation in serum 25-hydroxyvitamin D [25(OH)D] concentrations that is unexplained by dietary intake of vitamin D and sun exposure alone (144, 145).
Magnesium is a cofactor in several steps of vitamin D biosynthesis and activation
Magnesium, the second most abundant intracellular cation, plays a critical role in the synthesis and metabolism of parathyroid hormone (PTH) and vitamin D (123, 146, 147). Previous studies showed that the activities of 3 major enzymes that determine 25(OH)D concentrations, 25-hydroxylase, 1a-hydroxylase, and 24-hydroxylase (123, 147, 148), as well as vitamin D binding protein (VDBP) (123), are magnesium dependent. Magnesium deficiency leads to reduced 1,25- dihydroxyvitamin D [1,25(OH)2D] and impaired PTH response (123) and has been implicated in magnesium- dependent, vitamin D-resistant rickets (146). In 2 case studies of vitamin D-resistant rickets, magnesium supplementation substantially reversed the resistance to vitamin D treatment (146), whereas intramuscular infusion of vitamin D as high as 600,000 IU alone did not lead to any improvement in biochemical features of advanced vitamin D deficiency (i.e., serum calcium, magnesium, phosphorus, and alkaline phosphatase; serum vitamin D was not measured) (146). On the other hand, 2 small clinical studies with no placebo arm conducted in magnesium-deficient patients (123, 149) found that magnesium infusion alone led to a nonsignificant increase in both 25(OH)D and 1,25(OH)2D (123), whereas magnesium infusion plus oral vitamin D as 25(OH)D substantially increased both serum 25(OH)D and 1,25(OH)2D (149). Thus, these findings showed no effect for a high dose of vitamin D alone or magnesium infusion alone; however, there was a substantial increase in serum 25(OH)D due to vitamin D supplementation with magnesium infusion. Taken together, these findings suggest that a possible interaction between magnesium and vitamin D influences vitamin D status (150), but these findings should be tested in a large clinical trial.
Effects of interaction between nutritional magnesium status and serum vitamin D on disease outcomes
On the basis of this biological plausibility, one recent NHANES study found that a high intake of total, dietary, or supplemental magnesium was independently and significantly associated with reduced risks of both vitamin D deficiency and insufficiency in the general population (150). In addition, an inverse association between total magnesium intake and vitamin D insufficiency primarily appeared among populations at high risk of vitamin D insufficiency, such as overweight/obese individuals and African Americans. Furthermore, this study also found inverse associations of serum 25(OH)D with mortality (particularly CVD and colorectal cancer) that were modified by high magnesium intake (i.e., the inverse associations were primarily present when the magnesium intake was above the median).
The critical role of magnesium in the synthesis of VDBP, PTH, 25(OH)D, and 1,25(OH)2D may partially explain why these inverse associations between serum 25(OH)D and the risk of all-cause mortality and mortality due to colorectal cancer and CVD primarily existed among those with magnesium intakes above the median. High magnesium intakes may increase the availability of 1,25(OH)2D by activating the synthesis of 25(OH)D and 1,25(OH)2D and increasing the transfer to target tissues by elevating VDBP. This explanation is supported by 2 case studies reported by Reddy and Sivakumar (146), in which magnesium supplementation substantially reversed the resistance to vitamin D treatment in magnesium-deficient patients.
A previous clinical study found that parenteral magnesium treatment without vitamin D replacement in 23 magnesium-deficient patients led to a normalizing of VDBP. The study also reported a 12% increase in serum 25(OH)D and a 30% increase in serum 1,25(OH)2D; however, neither of these changes was significant (123). In a subsequent study in 5 magnesium-deficient patients, intramuscular treatment with magnesium alone did not significantly increase serum 25(OH)D, but magnesium infusion together with a pharmacologic dose of 25(OH)D substantially increased both serum 25(OH)D and 1,25(OH)2D among patients with magnesium deficiency (149). One interpretation is that magnesium treatment does not affect 25(OH)D status (123, 149). However, it is also possible that several factors may have contributed to the nonsignificant increase in 25(OH)D status. First, the patients with magnesium deficiency who participated in these previous studies had low concentrations of 25(OH)D and 1,25(OH)2D as well as previtamin D3 and vitamin D3 (cholecalciferol) as a result of limited sunlight exposure, underlying disease, and/or lack of oral supplementation. Therefore, concentrations of25(OH)D and 1,25(OH)2D did not substantially increase during short-term magnesium repletion because pre-vitamin D3 was not available in sufficient amounts. Second, a modest increase in the conversion of 25(OH)D to 1,25(OH)2D resulted in a reduction in 25(OH)D concentrations (147). Finally, the sample size in these 2 studies may have been too small to show a significant moderate effect of magnesium treatment on vitamin D status.
Similar health effects of vitamin D and magnesium studies
Vitamin D and magnesium studies have shown similar associations in several aspects of human health (151) (Table 1). In these areas of human disease, vitamin D and magnesium may potentially confound each other or a possible interaction between the 2 may exist. However, almost all studies in these areas measured either vitamin D or magnesium status, not both. This may hamper interpretation of the results. For example, results of studies examining associations between magnesium intake and risk of stroke (6, 152) and IHD (116, 152) have been inconsistent. A meta-analyses of prospective studies found that magnesium intake was related to a significantly reduced risk of stroke; however, this inverse association was weak (an 8% reduction in risk per 100-mg magnesium/d increment) and only 1 of the 7 cohorts included in the meta-analysis found a significant inverse association (6). Likewise, a prospective cohort study showed that magnesium intake was nonsignificantly inversely associated with IHD, with a pooled RR of 0.86 (95% CI: 0.67, 1.10) for the highest quintile (mean magnesium intake: 433 mg/d) vs. the lowest quintile (mean magnesium intake: 255 mg/d) of intake category (152). However, it must be noted that 255 mg magnesium/d was found to be adequate for healthy human adults in a series of metabolic unit magnesium balance studies (99). Similar to these findings in studies on stroke and IHD, several studies evaluated the associations between magnesium intake and the risk of colorectal adenoma and cancer and the results were also not entirely consistent (48, 71, 153, 154). All of these studies examined associations of disease with magnesium intake only, without considering any interaction with vitamin D. The significant interactions between serum vitamin D and magnesium intakes in relation to mortality due to CVD and colorectal cancer might help to explain such inconsistencies.
Although findings on the potential interaction between vitamin D and magnesium have been promising, only one recent study, to our knowledge, examined the interaction between vitamin D and magnesium in the general population (150). Deng et al. (150) found that magnesium intake may contribute to vitamin D status and that associations between serum vitamin D and mortality risk may be modified by magnesium intake. Because there is currently only one available study, it is difficult to discern whether these 2 micronutrients act independently or synergistically. Future studies are warranted to replicate the findings of Deng et al. and to explore the biochemical basis and molecular mechanisms that would explain these findings.
Areas in need of study on the interaction between magnesium, calcium, and vitamin D
Normal vitamin D metabolism requires Mg2+ for its synthesis and metabolism of parathyroid hormone and vitamin D (see above).
The following questions require further exploration:
Does low magnesium status affect this activation?
Does the calcium to magnesium ratio affect this activation?
Does low magnesium status result in low serum 25(OH)D concentrations?
Is there an impact of the calcium to magnesium ratio on serum 25(OH)D concentrations?
When discerning clinical, biochemical, or physiologic effects of low serum vitamin D, are these effects all or partly due to a low magnesium status or a high calcium to magnesium ratio?
Do clinical aspects of magnesium deficit or suboptimal status really derive at least partially from low serum vitamin D associated with low magnesium status or a high calcium to magnesium ratio?
Does vitamin D supplementation affect magnesium status in any manner?
Seelig (97, 98) reviewed earlier studies on animals, summarizing that vitamin D supplements improved both calcium and magnesium absorption but also increased magnesium excretion and therefore decreased magnesium retention. In one well-controlled human study (155), added vitamin D caused a decrease in magnesium retention, as predicted by animal studies. This area requires further study.
Dietary phosphorus interacts with each of the 3 above- described nutrients (magnesium, calcium, and vitamin D) and dietary intakes of phosphorus in US adults are well above the RDA of 700 mg/d. Phosphorus intakes in the United States have remained relatively stable, as have magnesium intakes, compared with the substantial increase in calcium intakes since 1977. Not much is known about the interaction of magnesium with phosphorus; however, because phosphorus is closely linked to calcium, it is possible that phosphorus nutrition affects a population with low magnesium dietary intakes. Indeed, Lutsey et al. (117) found that lower serum magnesium coupled with high serum calcium and phosphorus was a risk factor for heart failure. Interactions of phosphorus with magnesium, calcium, and vitamin D are areas for future study.
Conclusions
The essential micronutrients magnesium, calcium, and vitamin D are each associated with chronic diseases of global concern, including CVD, T2D, MetS, and skeletal disorders.
Dietary intakes of magnesium in the US population are low, and dietary calcium intakes in US adults increased 2-2.5 times more than dietary magnesium intakes between 1977 and 2010. Oral vitamin D has recently been recommended and is widely available. Despite these changes in intakes, research on the interactions between these 3 essential nutrients has been sparse.
Measuring magnesium status presents challenges, but magnesium intake is low in populations who consume a modern processed-food diet, including individuals in the United States. High calcium intakes can exacerbate the onset of low magnesium status and vice versa .
Studies showed that a calcium to magnesium intake ratio <2.8 is critical for optimal health , supporting a long-held but non-evidence-based recommendation that the calcium to magnesium ratio should be close to 2.
Increasing calcium intakes in the United States since 1977 have resulted in a calcium to magnesium ratio >3.0 since 2000, coinciding with increasing rates of T2D and colorectal cancer. US studies assessing oral magnesium therapy or dietary magnesium intakes showed beneficial effects of dietary magnesium in CVD, T2D, and cancers, although similar studies in populations with lower calcium to magnesium ratios ($1.7) reported the opposite, showing the impact that background dietary calcium and/or magnesium can have on studies of either calcium or magnesium alone.
Low vitamin D status is associated with chronic diseases of global concern, as is low magnesium status. Magnesium is a cofactor for vitamin D biosynthesis, transport, and activation . Interactions between magnesium intake and serum vitamin D contributing to the risk of CVD and colorectal cancer were recently indicated. However, epidemiologic data on possible interactions of these 2 micronutrients in human health and disease are very limited. Thus, additional studies are warranted. Increasing calcium to magnesium ratios coupled with oral calcium and vitamin D supplement recommendations in the face of suboptimal magnesium intakes maybe affecting health via unstudied impacts of interactions between magnesium, calcium, and vitamin D.
References
Seelig M, Rosanoff A. Are we really low in magnesium? In: Seelig M, Rosanoff A, editors. The magnesium factor. New York: Avery, Penguin; 2003. p. 211-8.
Joosten MM, Gansevoort RT, Mukamal KJ, van der Harst P, Geleijnse JM, Feskens EJ, Navis G, Bakker SJ; Prevend Study Group. Urinary and plasma magnesium and risk of ischemic heart disease. Am J Clin Nutr 2013;97:1299-306.
Khan AM, Lubitz SA, Sullivan LM, Sun JX, Levy D, Vasan RS, Magnani JW, Ellinor PT, Benjamin EJ, Wang TJ. Low serum magnesium and the development of atrial fibrillation in the community: the Framingham Heart Study. Circulation 2013;127:33-8.
Misialek JR, Lopez FL, Lutsey PL, Huxley RR, Peacock JM, Chen LY, Soliman EZ, Agarwal SK, Alonso A. Serum and dietary magnesium and incidence of atrial fibrillation in whites and in African Americans— Atherosclerosis Risk in Communities (ARIC) study. Circ J 2013; 77:323-9.
Del Gobbo LC, Song Y, Poirier P, Dewailly E, Elin RJ, Egeland GM. Low serum magnesium concentrations are associated with a high prevalence of premature ventricular complexes in obese adults with type 2 diabetes. Cardiovasc Diabetol 2012;11:23.
Larsson SC, Orsini N, Wolk A. Dietary magnesium intake and risk of stroke: a meta-analysis of prospective studies. Am J Clin Nutr 2012;95: 362-6.
Del Gobbo LC, Imamura F, Wu JH, de Oliveira Otto MC, Chiuve SE, Mozaffarian D. Circulating and dietary magnesium and risk of cardiovascular disease: a systematic review and meta-analysis ofprospective studies. Am J Clin Nutr 2013;98:160-73.
Qu X, Jin F, Hao Y, Li H, Tang T, Wang H, Yan W, Dai K. Magnesium and the risk of cardiovascular events: a meta-analysis of prospective cohort studies. PLoS One 2013;8:e57720.
Nie ZL, Wang ZM, Zhou B, Tang ZP, Wang SK. Magnesium intake and incidence of stroke: meta-analysis of cohort studies. Nutr Metab Cardiovasc Dis 2013;23:169-76.
Alghamdi AA, Al-Radi OO, Latter DA. Intravenous magnesium for prevention of atrial fibrillation after coronary artery bypass surgery: a systematic review and meta-analysis. J Card Surg 2005;20:293-9.
Shiga T, Wajima Z, Inoue T, Ogawa R. Magnesium prophylaxis for arrhythmias after cardiac surgery: a meta-analysis of randomized controlled trials. Am J Med 2004;117:325-33.
Reffelmann T, Ittermann T, Dorr M, Volzke H, Reinthaler M, Petersmann A, Felix SB. Low serum magnesium concentrations predict cardiovascular and all-cause mortality. Atherosclerosis 2011;219:280-4.
Chiuve SE, Sun Q, Curhan GC, Taylor EN, Spiegelman D, Willett WC, Manson JE, Rexrode KM, Albert CM. Dietary and plasma magnesium and risk of coronary heart disease among women. J Am Heart Assoc 2013;2:e000114.
Booth JV, Phillips-Bute B, McCants CB, Podgoreanu MV, Smith PK, Mathew JP, Newman MF. Low serum magnesium level predicts major adverse cardiac events after coronary artery bypass graft surgery. Am Heart J 2003;145:1108-13.
Ishimura E, Okuno S, Yamakawa T, Inaba M, Nishizawa Y. Serum magnesium concentration is a significant predictor of mortality in maintenance hemodialysis patients. Magnes Res 2007;20:237-44.
Singhi SC, Singh J, Prasad R. Hypo- and hypermagnesemia in an Indian pediatric intensive care unit. J Trop Pediatr 2003;49:99-103.
Dong JY, Xun P, He K, Qin LQ. Magnesium intake and risk of type 2 diabetes: meta-analysis of prospective cohort studies. Diabetes Care 2011;34:2116-22.
Larsson SC, Wolk A. Magnesium intake and risk of type 2 diabetes: a meta-analysis. J Intern Med 2007;262:208-14.
Sales CH, Pedrosa LF, Lima JG, Lemos TM, Colli C. Influence of magnesium status and magnesium intake on the blood glucose control in patients with type 2 diabetes. Clin Nutr 2011;30:359-64.
Agrawal P, Arora S, Singh B, Manamalli A, Dolia PB. Association of macrovascular complications of type 2 diabetes mellitus with serum magnesium levels. Diabetes Metab Syndr 2011;5:41-4.
Sharma A, Dabla S, Agrawal RP, Barjatya H, Kochar DK, Kothari RP. Serum magnesium: an early predictor of course and complications of diabetes mellitus. J Indian Med Assoc 2007;105:16, 8, 20.
Chambers EC, Heshka S, Gallagher D, Wang J, Pi-Sunyer FX, Pierson RN Jr. Serum magnesium and type-2 diabetes in African Americans and Hispanics: a New York cohort. J Am Coll Nutr 2006;25:509-13.
Saggese G, Federico G, Bertelloni S, Baroncelli GI, Calisti L. Hypomagnesemia and the parathyroid hormone-vitamin D endocrine system in children with insulin-dependent diabetes mellitus: effects of magnesium administration. J Pediatr 1991;118:220-5.
Solati M, Ouspid E, Hosseini S, Soltani N, Keshavarz M, Dehghani M. Oral magnesium supplementation in type II diabetic patients. Med J Islam Repub Iran 2014;28:67.
Song Y, He K, Levitan EB, Manson JE, Liu S. Effects of oral magnesium supplementation on glycaemic control in type 2 diabetes: a meta-analysis of randomized double-blind controlled trials. Diabet Med 2006;23:1050-6.
Yang CY, Chiu HF, Cheng MF, Tsai SS, Hung CF, Tseng YT. Magnesium in drinking water and the risk of death from diabetes mellitus. Magnes Res 1999;12:131-7.
He K, Liu K, Daviglus ML, Morris SJ, Loria CM, Van Horn L, Jacobs DR Jr., Savage PJ. Magnesium intake and incidence of metabolic syndrome among young adults. Circulation 2006;113:1675-82.
Huang JH, Lu YF, Cheng FC, Lee JN, Tsai LC. Correlation of magnesium intake with metabolic parameters, depression and physical activity in elderly type 2 diabetes patients: a cross-sectional study. Nutr J 2012;11:41.
Guerrero-Romero F, Rodriguez-Moran M. Low serum magnesium levels and metabolic syndrome. Acta Diabetol 2002;39:209-13.
Rodriguez-Moran M, Guerrero-Romero F. Oral magnesium supplementation improves the metabolic profile of metabolically obese, normal-weight individuals: a randomized double-blind placebo- controlled trial. Arch Med Res 2014;45:388-93.
Dibaba DT, Xun P, Fly AD, Yokota K, He K. Dietary magnesium intake and risk of metabolic syndrome: a meta-analysis. Diabet Med 2014a;31:1301-9.
Tucker KL, Hannan MT, Chen H, Cupples LA, Wilson PW, Kiel DP. Potassium, magnesium, and fruit and vegetable intakes are associated with greater bone mineral density in elderly men and women. Am J Clin Nutr 1999;69:727-36.
Orchard TS, Larson JC, Alghothani N, Bout-Tabaku S, Cauley JA, Chen Z, Lacroix AZ, Wactawski-Wende J, Jackson RD. Magnesium intake, bone mineral density, and fractures: results from the Women’s Health Initiative Observational Study. Am J Clin Nutr 2014;99:926-33.
Ryder KM, Shorr RI, Bush AJ, Kritchevsky SB, Harris T, Stone K, Cauley J, Tylavsky FA. Magnesium intake from food and supplements is associated with bone mineral density in healthy older white subjects. J Am Geriatr Soc 2005;53:1875-80.
New SA, Robins SP, Campbell MK, Martin JC, Garton MJ, Bolton- Smith C, Grubb DA, Lee SJ, Reid DM. Dietary influences on bone mass and bone metabolism: further evidence of a positive link between fruit and vegetable consumption and bone health? Am J Clin Nutr 2000;71:142-51.
Stendig-Lindberg G, Tepper R, Leichter I. Trabecular bone density in a two year controlled trial of peroral magnesium in osteoporosis. Magnes Res 1993;6:155-63.
Hopping BN, Erber E, Grandinetti A, Verheus M, Kolonel LN, Maskarinec G. Dietary fiber, magnesium, and glycemic load alter risk of type 2 diabetes in a multiethnic cohort in Hawaii. J Nutr 2010;140:68-74.
Hruby A, McKeown N, Song Y, Djousse L. Dietary magnesium and genetic interactions in diabetes and related risk factors: a brief overview of current knowledge. Nutrients 2013;5:4990-5011.
Guasch-Ferre M, Bullo M, Estruch R, Corella D, Martinez-Gonzalez MA, Ros E, Covas M, Aros F, Gomez-Gracia E, Fiol M, et al. Dietary magnesium intake is inversely associated with mortality in adults at high cardiovascular disease risk. J Nutr 2014;144:55-60.
Rude RK, Singer FR, Gruber HE. Skeletal and hormonal effects of magnesium deficiency. J Am Coll Nutr 2009;28:131-41.
Sojka JE, Weaver CM. Magnesium supplementation and osteoporosis. Nutr Rev 1995;53:71-4.
New SA, Bolton-Smith C, Grubb DA, Reid DM. Nutritional influences on bone mineral density: a cross-sectional study in premenopausal women. Am J Clin Nutr 1997;65:1831-9.
Aziz HS, Blamoun AI, Shubair MK, Ismail MM, DeBari VA, Khan MA. Serum magnesium levels and acute exacerbation of chronic obstructive pulmonary disease: a retrospective study. Ann Clin Lab Sci 2005;35:423-7.
Bhatt SP, Khandelwal P, Nanda S, Stoltzfus JC, Fioravanti GT. Serum magnesium is an independent predictor of frequent readmissions due to acute exacerbation of chronic obstructive pulmonary disease. Re- spir Med 2008;102:999-1003.
Fiaccadori E, Del Canale S, Coffrini E, Melej R, Vitali P, Guariglia A, Borghetti A. Muscle and serum magnesium in pulmonary intensive care unit patients. Crit Care Med 1988;16:751-60.
Kurys E, Kurys P, Kuzniar A, Kieszko R. Analysis of antioxidant enzyme activity and magnesium level in chronic obstructive pulmonary disease (COPD). Ann Univ Mariae Curie Sklodowska Med 2001;56:261-6.
Ruljancic N, Popovic-Grle S, Rumenjak V, Sokolic B, Malic A, Mihanovic M, Cepelak I. COPD: magnesium in the plasma and polymorphonuclear cells of patients during a stable phase. COPD 2007;4:41-7.
Chen GC, Pang Z, Liu QF. Magnesium intake and risk of colorectal cancer: a meta-analysis of prospective studies. Eur J Clin Nutr 2012; 66:1182-6.
Ko HJ, Youn CH, Kim HM, Cho YJ, Lee GH, Lee WK. Dietary magnesium intake and risk of cancer: a meta-analysis of epidemiologic studies. Nutr Cancer 2014;66:915-23.
Dai Q, Motley SS, Smith JA Jr., Concepcion R, Barocas D, Byerly S, Fowke JH. Blood magnesium, and the interaction with calcium, on the risk of high-grade prostate cancer. PLoS One 2011;6:e18237.
Everett CJ, King DE, Wells BJ, Frithsen IL, Mainous AG III. Serum magnesium and cancer mortality. In: Bernhardt NE, Kasko AM, editors. Nutrition for the middle aged and elderly. Hauppauge (NY): Nova Science Publishers; 2008. p. 271-84.
Barragan-Rodriguez L, Rodriguez-Moran M, Guerrero-Romero F. Depressive symptoms and hypomagnesemia in older diabetic subjects. Arch Med Res 2007;38:752-6.
Derom ML, Sayon-Orea C, Martinez-Ortega JM, Martinez-Gonzalez MA. Magnesium and depression: a systematic review. Nutr Neurosci 2013;16:191-206.
Tarleton EK, Littenberg B. Magnesium intake and depression in adults. J Am Board Fam Med 2015;28:249-56.
Yary T, Aazami S, Soleimannejad K. Dietary intake of magnesium may modulate depression. Biol Trace Elem Res 2013;151:324-9.
Ozawa M, Ninomiya T, Ohara T, Hirakawa Y, Doi Y, Hata J, Uchida K, Shirota T, Kitazono T, Kiyohara Y. Self-reported dietary intake of potassium, calcium, and magnesium and risk of dementia in the Japanese: the Hisayama Study. J Am Geriatr Soc 2012;60:1515-20.
Slutsky I, Abumaria N, Wu LJ, Huang C, Zhang L, Li B, Zhao X, Govindarajan A, Zhao MG, Zhuo M, et al. Enhancement of learning and memory by elevating brain magnesium. Neuron 2010;65:165-77.
Lozano R, Naghavi M, Foreman K, Lim S, Shibuya K, Aboyans V, Abraham J, Adair T, Aggarwal R, Ahn SY, et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380:2095-128. Erratum in: Lancet 2013;381(9867):628.
USDA Agricultural Research Service. What we eat in America, NHANES 2011-2012. Table 37: Total nutrient intakes: percent reporting and mean amounts of selected vitamins and minerals from food and beverages and dietary supplements, by gender and age, in the United States, 2011-2012. Magnesium [cited 2015 Jan 1]. Available from:
- http://www.ars.usda.gov/ SP2UserFiles/Place/80400530/pdf/1112/Table37SUPGEN11.pdf.
Institute of Medicine. Dietary Reference Intakes for calcium, phosphorus, magnesium, vitamin D, and fluoride. Washington (DC): National Academies Press; 1997.
Moshfegh A, Goldman JD, Ahuja J, Rhodes D, LaComb R. What we eat in America, NHANES 2005-2006: usual nutrient intakes from food and water compared to 1997 Dietary Reference Intakes for vitamin D, calcium, phosphorus, and magnesium. 2009 [cited 2015 May 11]. Available from: http://www.ars.usda.gov/SP2UserFiles/Place/12355000/pdf/0506/usualnutrientintakevitDcaphosmg_2005-06.pdf.
Rosanoff A, Weaver CM, Rude RK. Suboptimal magnesium status in the United States: are the health consequences underestimated? Nutr Rev 2012;70:153-64.
USDA Human Nutrition Information Service. CSFII Nationwide Food Consumption Survey Continuing Survey of Food Intakes by Individuals; men 19-50 years, 1 day; report no. 85-3. 1985 [cited 2012 Jul 10]. Available from: http://www.ars.usda.gov/SP2UserFiles/Place/80400530/pdf/8586/csfii851daymen_doc.pdf.
USDA Human Nutrition Information Service. CSFII Nationwide Food Consumption Survey Continuing Survey of Food Intakes by Individuals; women 19-50 years and their children 1-5 years, 1 day; report no. 85-1. 1985 [cited 2012 Jul 10]. Available from: http://www.ars.usda.gov/SP2UserFiles/Place/80400530/pdf/8586/csfii851daydoc.pdf.
Wilson JW, Enns CW, Goldman JD, Tippett KS, Mickle SJ, Cleveland LE, Chahil PS. Data tables: combined results from USDA’s 1994 and 1995 Diet and Health Knowledge Survey [online]. 1997 [cited 2012 Jul 10]. Available from: http://www.barc.usda.gov/bhnrc/foodsurvey/home.htm; http://www.ars.usda.gov/Services/docs.htm?docid=14531.
USDA Agricultural Research Service. Nutrient intakes from food compared to Dietary Reference Intakes. Table 1. Mean amounts by gender and age: individuals 2 years and over (excluding breast-fed children), MEC sampling weights NHANES, 2001-2002 [cited 2012 Feb 29]. Available from: http://www.ars.usda.gov/SP2UserFiles/ Place/80400530/pdf/0102/usualintaketables2001-02.pdf.
USDA Agricultural Research Service. Table 1. Nutrient intakes from food: mean amounts consumed per individual, one day, NHANES 2003-2004. 2007 [cited 2012 Feb 29]. Available from: http://www.ars.usda.gov/SP2UserFiles/Place/80400530/pdf/0304/Table1NIF.pdf.
USDA Agricultural Research Service. Table 1. Nutrient intakes from food: mean amounts consumed per individual, one day, NHANES 2005-2006. 2008 [cited 2012 Feb 29]. Available from: http://www.ars. usda.gov/SP2UserFiles/Place/80400530/pdf/0506/Table1NIF_05.pdf.
USDA Agricultural Research Service. Table 1. Nutrient intakes from food: mean amounts consumed per individual, one day, NHANES 2007-2008. 2010 [cited 2012 Feb 29]. Available from: http://www.ars.usda.gov/SP2UserFiles/Place/80400530/pdf/0708/Table1NINGEN07.pdf.
USDA Agricultural Research Service. What we eat in America, NHANES 2009-2010, individuals 2 years and over (excluding pregnant and/or lactating females and breast-fed children), day 1 food and supplement intake data, weighted. 2012 [cited 2014 Oct 15]. Available from: http://www.ars.usda.gov/SP2UserFiles/Place/80400530/pdf/0910/Table39SUPINC09.pdf.
Dai Q, Shrubsole MJ, Ness RM, Schlundt D, Cai Q, Smalley WE, Li M, Shyr Y, Zheng W. The relation of magnesium and calcium intakes and a genetic polymorphism in the magnesium transporter to colorectal neoplasia risk. Am J Clin Nutr 2007;86:743-51.
Marier JR. Magnesium content of the food supply in the modern-day world. Magnesium 1986;5:1-8.
Elin RJ. Laboratory tests for the assessment of magnesium status in humans. Magnes Trace Elem 1991;10:172-81.
Wong ET, Rude RK, Singer FR, Shaw ST Jr. A high prevalence of hypomagnesemia and hypermagnesemia in hospitalized patients. Am J Clin Pathol 1983;79:348-52.
Elin RJ. Assessment of magnesium status for diagnosis and therapy. Magnes Res 2010;23:S194-8.
Nuoranne P. On the reliability of the magnesium serum value as an indicator of body magnesium status. Nord Vet Med 1978;30:71-3.
Arnold A, Tovey J, Mangat P, Penny W, Jacobs S. Magnesium deficiency in critically ill patients. Anaesthesia 1995;50:203-5.
Saur PM, Zielmann S, Roth AT, Frank L, Warneke G, Radke A, Ensink FB, Kettler D. [Diagnosis of magnesium deficiency in intensive care patients.] Anasthesiol Intensivmed Notfallmed Schmerzther 1996;31: 37-41 (in German).
Hebert P, Mehta N, Wang J, Hindmarsh T, Jones G, Cardinal P. Functional magnesium deficiency in critically ill patients identified using a magnesium-loading test. Crit Care Med 1997;25:749-55.
Ryzen E, Elbaum N, Singer FR, Rude RK. Parenteral magnesium tolerance testing in the evaluation of magnesium deficiency. Magnesium 1985;4:137-47.
Danielson BG, Johansson G, Ljunghall S. Magnesium metabolism in healthy subjects. Scand J Urol Nephrol Suppl 1979;49-73.
Seelig MS. Magnesium deficiency in the pathogenesis of disease, early roots of cardiovascular,skeletal, and renal abnormalities. New York and London: Plenum Medical Book Co.; 1980.
Lowenstein FW, Stanton MF. Serum magnesium levels in the United States, 1971-1974. J Am Coll Nutr 1986;5:399-414.
Elin RJ. Re-evaluation of the concept of chronic, latent, magnesium deficiency. Magnes Res 2011;24:225-7.
Ross AC, Taylor CL, Yaktine AL, Del Valle H. Dietary Reference Intakes for calcium and vitamin D. Washington (DC): National Academies Press; 2011.
Elin R. Laboratory evaluation of chronic latent magnesium deficiency. In: Rayssiguier Y, Mazur A, Durlach J, editors. Advances in magnesium research: nutrition and health. Eastleigh (United Kingdom): John Libbey & Company Ltd.; 2001. p. 233-9.
Kieboom BC, Kiefte-de Jong JC, Eijgelsheim M, Franco OH, Kuipers EJ, Hofman A, Zietse R, Stricker BH, Hoorn EJ. Proton pump inhibitors and hypomagnesemia in the general population: a population- based cohort study. Am J Kidney Dis 2015;66(5):775-82.
Shils M. Magnesium. In: Shils M, Olson J, Shike M, Ross A, editors. Modern nutrition in health and disease. Baltimore (MD): Williams & Wilkins; 1999. p. 169-92.
Larsson SC. Urinary magnesium excretion as a marker of heart disease risk. Am J Clin Nutr 2013;97:1159-60.
Joosten MM, Gansevoort RT, Mukamal KJ, Kootstra-Ros JE, Feskens EJM, Geleijnse JM, Navis G, Bakker SJL. Urinary magnesium excretion and risk of hypertension: the prevention of renal and vascular end-stage disease study. Hypertension 2013;61:1161-7.
Rude RK. Magnesium metabolism and deficiency. Endocrinol Metab Clin North Am 1993;22:377-95.
Rubin H. Central roles of Mg2+ and MgATP2- in the regulation of protein synthesis and cell proliferation: significance for neoplastic transformation. Adv Cancer Res 2005;93:1-58.
Pantin CFA. On the physiology of amoeboid movement. IV. The action of magnesium. Br J Exp Biol 1925-26;3:297-312.
Resnick LM. Cellular calcium and magnesium metabolism in the pathophysiology and treatment of hypertension and related metabolic disorders. Am J Med 1992;93:11S-20S.
Resnick LM. Cellular ions in hypertension, insulin resistance, obesity, and diabetes: a unifying theme. J Am Soc Nephrol 1992;3:S78-85.
Resnick LM. Ionic basis of hypertension, insulin resistance, vascular disease, and related disorders: the mechanism of “syndrome X”. Am J Hypertens 1993;6:123S-34S.
Seelig MS. The requirement of magnesium by the normal adult. Am J Clin Nutr 1964;14:242-90.
Seelig MS. Human requirements of magnesium; factors that increase needs. In: Durlach J, ed. 1er Symposium International sur le Deficit Magnesique en Pathologie Humaine [First International Symposium on Magnesium Deficiency in Human Pathology]. Vittel: SGEMV, 1971:11-38 (in French).
Hunt CD, Johnson LK. Magnesium requirements: new estimations for men and women by cross-sectional statistical analyses of metabolic magnesium balance data. Am J Clin Nutr 2006;84:843-52.
Amiot D, Hioco D, Durlach J. Frequence du deficit magnesique chez le sujet normal et dans diverses osteopathies. [Frequency of magnesium deficit in the normal subjects and in various steopathies]. J Med Be- sancon 1969;5:371-8 (in French).
Clarkson EM, Warren RL, McDonald SJ, de Wardener HE. The effect of a high intake of calcium on magnesium metabolism in normal subjects and patients with chronic renal failure. Clin Sci 1967;32: 11-8.
Sojka J, Wastney M, Abrams S, Lewis SF, Martin B, Weaver C, Peacock M. Magnesium kinetics in adolescent girls determined using stable isotopes: effects of high and low calcium intake. Am J Physiol 1997;273:R710-5.
Green JH, Booth C, Bunning R. Impact of supplementary high calcium milk with additional magnesium on parathyroid hormone and biochemical markers of bone turnover in postmenopausal women. Asia Pac J Clin Nutr 2002;11:268-73.
Domrongkitchaiporn S, Ongphiphadhanakul B, Stitchantrakul W, Pia- seu N, Chansirikam S, Puavilai G, Rajatanavin R. Risk of calcium oxalate nephrolithiasis after calcium or combined calcium and calcitriol supplementation in postmenopausal women. Osteoporos Int 2000;11: 486-92.
Karkkainen MU, Wiersma JW, Lamberg-Allardt CJ. Postprandial parathyroid hormone response to four calcium-rich foodstuffs. Am J Clin Nutr 1997;65:1726-30.
Doyle L, Flynn A, Cashman K. The effect of magnesium supplementation on biochemical markers of bone metabolism or blood pressure in healthy young adult females. Eur J Clin Nutr 1999;53:255-61.
Basso LE, Ubbink JB, Delport R, Spies J, Vermaak WJ. Effect of magnesium supplementation on the fractional intestinal absorption of 45CaCl2 in women with a low erythrocyte magnesium concentration. Metabolism 2000;49:1092-6.
Kato Y, Yamaguchi S, Yachiku S, Nakazono S, Hori J, Wada N, Hou K. Changes in urinary parameters after oral administration of potassium- sodium citrate and magnesium oxide to prevent urolithiasis. Urology 2004;63:7-11; discussion: 2.
Sei M, Nakamura H, Miyoshi T. Nutritional epidemiological study on mineral intake and mortality from cardiovascular disease. Tokushima J Exp Med 1993;40:199-207.
Burnett-Hartman AN, Fitzpatrick AL, Gao K, Jackson SA, Schreiner PJ. Supplement use contributes to meeting recommended dietary intakes for calcium, magnesium, and vitamin C in four ethnicities of middle-aged and older Americans: the Multi-Ethnic Study of Atherosclerosis. J Am Diet Assoc 2009;109:422-9.
Durlach J. Recommended dietary amounts of magnesium: Mg RDA. Magnes Res 1989;2:195-203.
Dai Q, Sandler R, Barry E, Summers R, Grau M, Baron J. Calcium, magnesium, and colorectal cancer. Epidemiology 2012;23:504-5.
Ma J, Folsom AR, Melnick SL, Eckfeldt JH, Sharrett AR, Nabulsi AA, Hutchinson RG, Metcalf PA. Associations of serum and dietary magnesium with cardiovascular disease, hypertension, diabetes, insulin, and carotid arterial wall thickness: the ARIC study. Atherosclerosis Risk in Communities Study. J Clin Epidemiol 1995;48: 927.
Dai Q, Shu XO, Deng X, Xiang YB, Li H, Yang G, Shrubsole MJ, Ji B, Cai H, Chow WH, et al. Modifying effect of calcium/magnesium intake ratio and mortality: a population-based cohort study. BMJ Open 2013;3:e002111.
Chiuve SE, Korngold EC, Januzzi JL Jr., Gantzer ML, Albert CM. Plasma and dietary magnesium and risk of sudden cardiac death in women. Am J Clin Nutr 2011;93:253-60.
Zhang W, Iso H, Ohira T, Date C, Tamakoshi A. Associations of dietary magnesium intake with mortality from cardiovascular disease: the JACC study. Atherosclerosis 2012;221(2):587-95.
Lutsey PL, Alonso A, Michos ED, Loehr LR, Astor BC, Coresh J, Folsom AR. Serum magnesium, phosphorus, and calcium are associated with risk of incident heart failure: the Atherosclerosis Risk in Communities (ARIC) Study. Am J Clin Nutr 2014;100:756-64.
Moore-Schiltz L, Albert JM, Singer ME, Swain J, Nock NL. Dietary intake of calcium and magnesium and the metabolic syndrome in the National Health and Nutrition Examination (NHANES) 2001-2010 data. Br J Nutr 2015;14(6):1-12.
Rosanoff A. Rising Ca:Mg intake ratio from food in USA Adults: a concern? Magnes Res 2010;23:S181-93.
Carpenter TO. Disturbances of vitamin D metabolism and action during clinical and experimental magnesium deficiency. Magnes Res 1988;1:131-9.
Medalle R, Waterhouse C, Hahn TJ. Vitamin D resistance in magnesium deficiency. Am J Clin Nutr 1976;29:854-8.
Rosler A, Rabinowitz D. Magnesium-induced reversal of vitamin-D resistance in hypoparathyroidism. Lancet 1973;1:803-4.
Rude RK, Adams JS, Ryzen E, Endres DB, Niimi H, Horst RL, Haddad JG Jr., Singer FR. Low serum concentrations of 1,25-dihydroxyvitamin D in human magnesium deficiency. J Clin Endocrinol Metab 1985;61:933-40.
Seelig MS. Vitamin D and cardiovascular, renal, and brain damage in infancy and childhood. Ann N Y Acad Sci 1969;147:539-82.
Seelig MS. Vitamin D—riskvs benefit. J Am Coll Nutr 1983;2:109-10.
Holick MF. Resurrection of vitamin D deficiency and rickets. J Clin Invest 2006;116:2062-72.
Zittermann A, Iodice S, Pilz S, Grant WB, Bagnardi V, Gandini S. Vitamin D deficiency and mortality risk in the general population: a meta-analysis of prospective cohort studies. Am J Clin Nutr 2012; 95:91-100.
Schottker B, Haug U, Schomburg L, Kohrle J, Perna L, Muller H, Holleczek B, Brenner H. Strong associations of 25-hydroxyvitamin D concentrations with all-cause, cardiovascular, cancer, and respiratory disease mortality in a large cohort study. Am J Clin Nutr 2013;97:782-93.
Melamed ML, Michos ED, Post W, Astor B. 25-Hydroxyvitamin D levels and the risk of mortality in the general population. Arch Intern Med 2008;168:1629-37.
Pittas AG, Nelson J, Mitri J, Hillmann W, Garganta C, Nathan DM, Hu FB, Dawson-Hughes B; Diabetes Prevention Program Research Group. Plasma 25-hydroxyvitamin D and progression to diabetes in patients at risk for diabetes: an ancillary analysis in the Diabetes Prevention Program. Diabetes Care 2012;35:565-73.
Mitri J, Muraru MD, Pittas AG. Vitamin D and type 2 diabetes: a systematic review. Eur J Clin Nutr 2011;65:1005-15.
Pittas AG, Lau J, Hu FB, Dawson-Hughes B. The role of vitamin D and calcium in type 2 diabetes: a systematic review and meta-analysis. J Clin Endocrinol Metab 2007;92:2017-29.
Sun Q, Shi L, Rimm EB, Giovannucci EL, Hu FB, Manson JE, Rexrode KM. Vitamin D intake and risk of cardiovascular disease in US men and women. Am J Clin Nutr 2011;94:534-42.
Leu M, Giovannucci E. Vitamin D: epidemiology of cardiovascular risks and events. Best Pract Res Clin Endocrinol Metab 2011;25: 633-46.
Reddy V, Sivakumar B. Magnesium-dependent vitamin-D-resistant rickets. Lancet 1974;1:963-5.
Risco F, Traba ML. Influence of magnesium on the in vitro synthesis of 24,25-dihydroxyvitamin D3 and 1 alpha, 25-dihydroxyvitamin D3. Magnes Res 1992;5:5-14.
Risco F, Traba ML. Possible involvement of a magnesium dependent mitochondrial alkaline phosphatase in the regulation of the 25-hydroxyvitamin D3-1 alpha-and 25-hydroxyvitamin D3-24R- hydroxylases in LLC-PK1 cells. Magnes Res 1994;7:169-78.
Fuss M, Bergmann P, Bergans A, Bagon J, Cogan E, Pepersack T, Van Gossum M, Corvilain J. Correction of low circulating levels of 1,25- dihydroxyvitamin D by 25-hydroxyvitamin D during reversal of hypo- magnesaemia. Clin Endocrinol (Oxf) 1989;31:31-8.
Deng X, Song Y, Manson JE, Signorello LB, Zhang SM, Shrubsole MJ, Ness RM, Seidner DL, Dai Q. Magnesium, vitamin D status and mortality: results from US National Health and Nutrition Examination Survey (NHANES) 2001 to 2006 and NHANES III. BMC Med 2013;11:187.
Ross AC, Manson JE, Abrams SA, Aloia JF, Brannon PM, Clinton SK, Durazo-Arvizu RA, Gallagher JC, Gallo RL, Jones G, et al. The 2011 report on Dietary Reference Intakes for calcium and vitamin D from the Institute of Medicine: what clinicians need to know. J Clin Endocrinol Metab 2011;96:53-8.
Song Y, Manson JE, Cook NR, Albert CM, Buring JE, Liu S. Dietary magnesium intake and risk of cardiovascular disease among women. Am J Cardiol 2005;96:1135-41.
Wark PA, Lau R, Norat T, Kampman E. Magnesium intake and colorectal tumor risk: a case-control study and meta-analysis. Am J Clin Nutr 2012;96:622-31.
Qu X, Jin F, Hao Y, Zhu Z, Li H, Tang T, Dai K. Nonlinear association between magnesium intake and the risk of colorectal cancer. Eur J Gastroenterol Hepatol 2013;25:309-18.
Chu HI, Liu SH, Hsu HC, Choa HC, Cheu SH. Calcium, phosphorus, nitrogen, and magnesium metabolism in normal young Chinese adults. Chin Med J 1941;59:1-33.
