Preterm birth associated with many genes, including the Vitamin D Receptor again
Transcriptome Analysis of Early Pregnancy Vitamin D Status and Spontaneous Preterm Birth
PLoS One, 15 (1), e0227193 2020 Jan 29 eCollection 2020, DOI: 10.1371/journal.pone.0227193
Aishwarya P Yadama 1, Hooman Mirzakhani 1, Thomas F McElrath 2, Augusto A Litonjua 3, Scott T Weiss 1
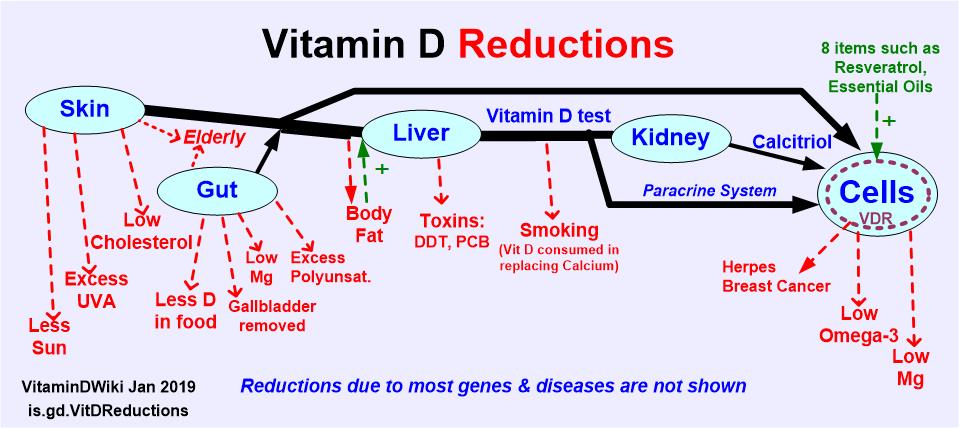 click on chart for details
click on chart for details
📄 Download the PDF from VitaminDWiki
Vitamin D Receptor is directly or indirectly connected to Spontaneous Preterm Birth genes
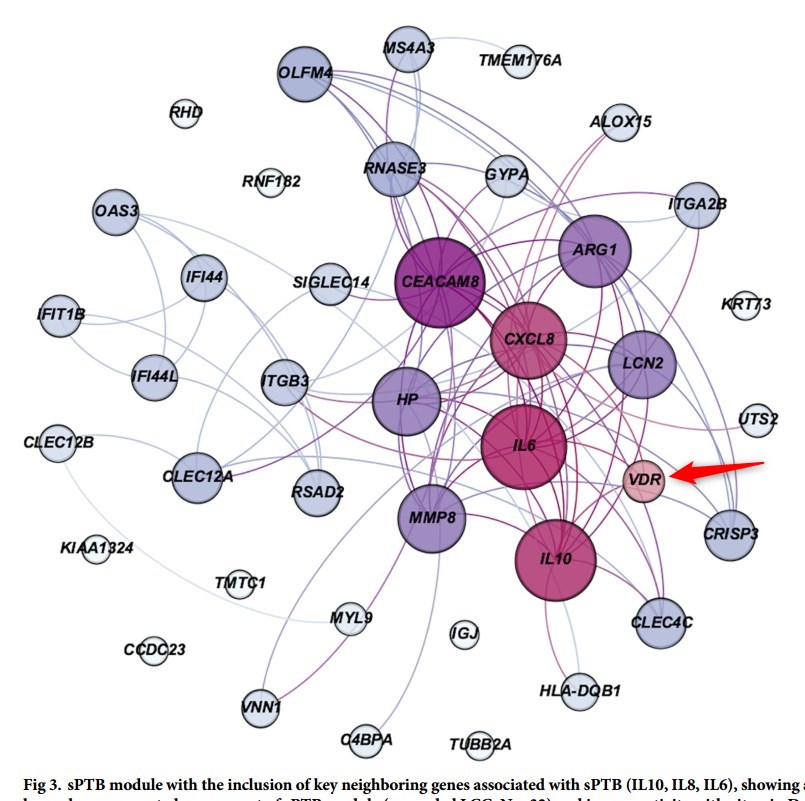
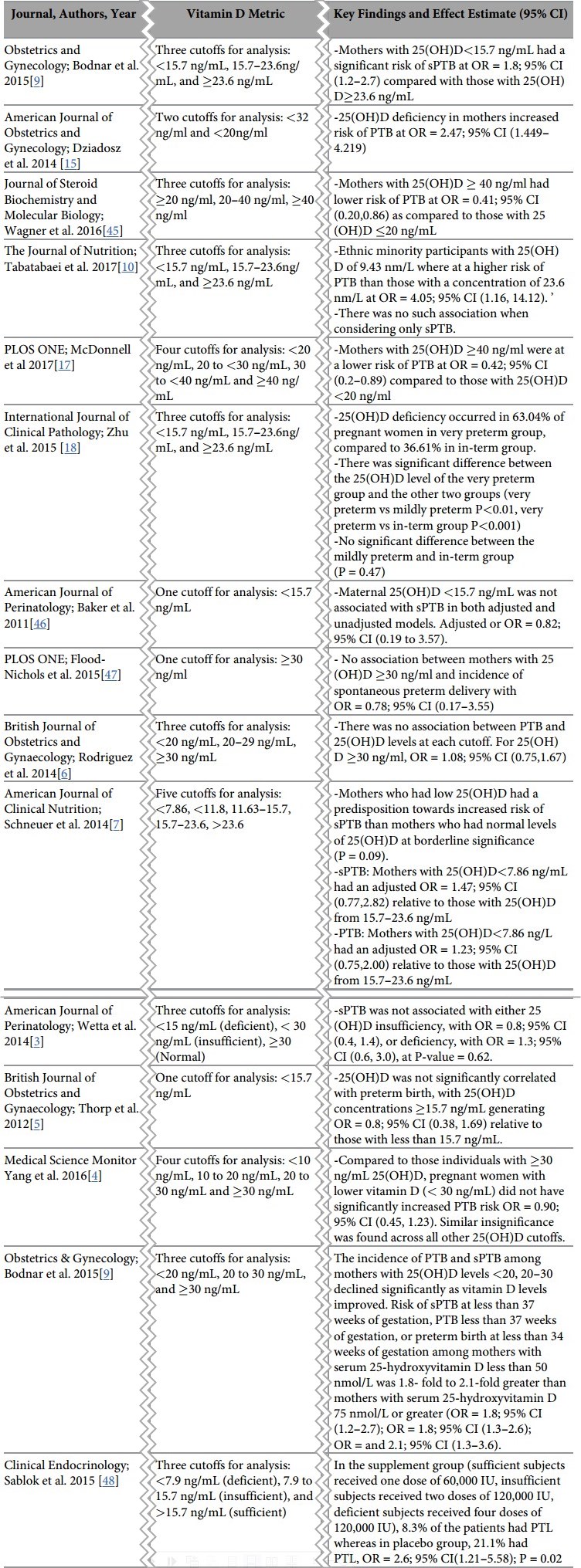
Background: We conducted a literature review on the studies that investigated the relationship of preterm birth, including spontaneous preterm birth (sPTB), with vitamin D status. Overall, these studies demonstrated that the incidence of sPTB was associated with maternal vitamin D insufficiency in early pregnancy. However, the potential mechanisms and biological pathways are unknown.
Objectives: To investigate early pregnancy gene expression signatures associated with both vitamin D insufficiency and sPTB. We further constructed a network of these gene signatures and identified the common biological pathways involved.
Study design: We conducted peripheral blood transcriptome profiling at 10-18 weeks of gestation in a nested case-control cohort of 24 pregnant women who participated in the Vitamin D Antenatal Asthma Reduction Trial (VDAART). In this cohort, 8 women had spontaneous preterm delivery (21-32 weeks of gestation) and 17 women had vitamin D insufficiency (25-hydroxyvitamin D < 30 ng/mL). We separately identified vitamin D-associated and sPTB gene signatures at 10 to 18 weeks and replicated the overlapping signatures in the mid-pregnancy peripheral blood of an independent cohort with sPTB cases.
Result: At 10-18 weeks of gestation, 146 differentially expressed genes (25 upregulated) were associated with both vitamin D insufficiency and sPTB in the discovery cohort (FDR < 0.05). Of these genes, 43 (25 upregulated) were replicated in the independent cohort of sPTB cases and controls with normal pregnancies (P < 0.05). Functional enrichment and network analyses of the replicated gene signatures suggested several highly connected nodes related to inflammatory and immune responses.
Conclusions: Our gene expression study and network analyses suggest that the dysregulation of immune response pathways due to early pregnancy vitamin D insufficiency may contribute to the pathobiology of sPTB.
