COVID-19 Long haul - excellent graph - systematic review
Assessment of the Frequency and Variety of Persistent Symptoms Among Patients With COVID-19 A Systematic Review
JAMA Netwoh< Open. 2021;4(5):e2111417. doi:10.1001/jamanetworkopen.2021.11417
Tahmina Nasserie, MPH; Michael Hittle, BS; Steven N. Goodman, MD, MHS, PhD
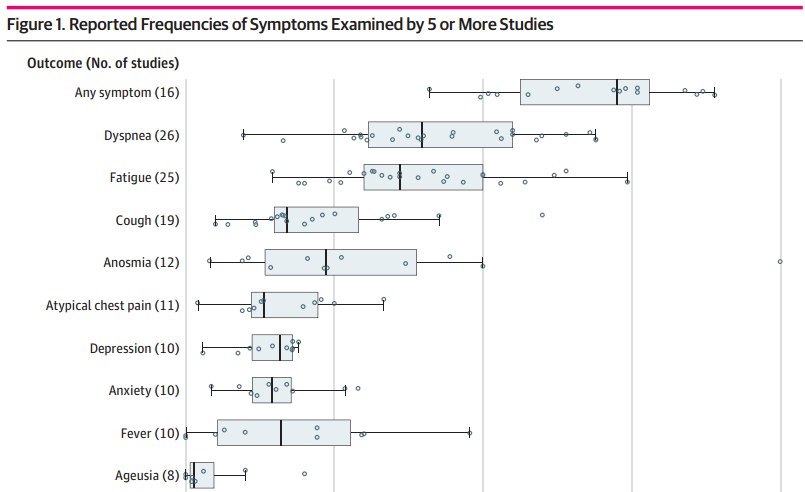
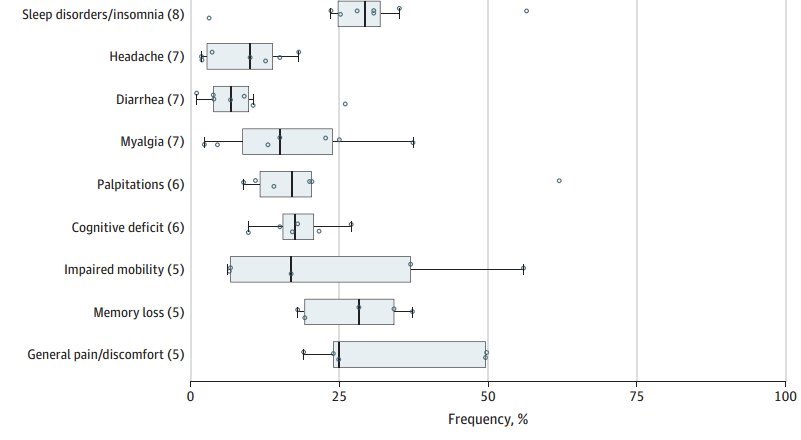
The horizontal bar extends from the first to the third quartile, the interquartile range (IQR).
The whiskers extend from the upper and lower quartiles to the largest value within 1.5 IQRs of that quartile.
The width of the box represents the IQR.
The vertical bar represents the median value for the outcome.
The circles represent point estimates from each study.
Circles beyond the whiskers are considered outliers.
📄 Download the PDF from VitaminDWiki
Key Points
Question What are the frequency and variety of persistent symptoms after COVID-19 infection?
Findings In this systematic review of 45 studies including 9751 participants with COVID-19, the median proportion of individuals who experienced at least 1 persistent symptom was 73%; symptoms occurring most frequently included shortness of breath or dyspnea, fatigue or exhaustion, and sleep disorders or insomnia. However, the studies were highly heterogeneous and needed longer follow-up and more standardized designs.
Meaning This systematic review found that COVID-19 symptoms commonly persisted beyond the acute phase of infection, with implications for health- associated functioning and quality of life; however, methodological improvements are needed to reliably quantify these risks.
IMPORTANCE Infection with COVID-19 has been associated with long-term symptoms, but the frequency, variety, and severity of these complications are not well understood. Many published commentaries have proposed plans for pandemic control that are primarily based on mortality rates among older individuals without considering long-term morbidity among individuals of all ages. Reliable estimates of such morbidity are important for patient care, prognosis, and development of public health policy.
OBJECTIVE To conduct a systematic review of studies examining the frequency and variety of persistent symptoms after COVID-19 infection.
EVIDENCE REVIEW A search of PubMed and Web ofScience was conducted to identify studies published from January 1, 2020, to March 11,2021, that examined persistent symptoms after COVID-19 infection. Persistent symptoms were defined as those persisting for at least 60 days after diagnosis, symptom onset, or hospitalization or at least 30 days after recovery from the acute illness or hospital discharge. Search terms included COVID-19, SARS-CoV-2, coronavirus, 2019-nCoV, longterm, after recovery, long-haul, persistent, outcome, symptom, follow-up, and longitudinal. All English-language articles that presented primary data from cohort studies that reported the prevalence of persistent symptoms among individuals with SARS-CoV-2 infection and that had clearly defined and sufficient follow-up were included. Case reports, case series, and studies that described symptoms only at the time of infection and/or hospitalization were excluded. A structured framework was applied to appraise study
quality.
FINDINGS A total of 1974 records were identified; of those, 1247 article titles and abstracts were screened. After removal of duplicates and exclusions, 92 full-text articles were assessed for eligibility; 47 studies were deemed eligible, and 45 studies reporting 84 clinical signs or symptoms were included inthe systematic review. Of 9751 total participants, 5266 (54.0%) were male; 30 of 45 studies reported mean or median ages younger than 60 years. Among 16 studies, most of which comprised participants who were previously hospitalized, the median proportion of individuals experiencing at least 1 persistent symptom was 72.5% (interquartile range [IQR], 55.0%-80.0%). Individual symptoms occurring most frequently included shortness of breath or dyspnea (26 studies; median frequency, 36.0%; IQR, 27.6%-50.0%), fatigue or exhaustion (25 studies; median frequency, 40.0%; IQR, 31.0%-57.0%), and sleep disorders or insomnia (8 studies; median 29.4%, IQR, 24.4%-33.0%). There were wide variations in the design and quality of the studies, which had implications for interpretation and often limited direct comparability and combinability. Major design differences included patient populations, definitions of time zero (ie, the beginning of the follow-up interval), follow-up lengths, and outcome definitions, including definitions of illness severity.
CONCLUSIONS AND RELEVANCE This systematic review found that COVID-19 symptoms commonly persisted beyond the acute phase of infection, with implications for health-associated functioning and quality of life. Current studies of symptom persistence are highly heterogeneous, and future studies need longer follow-up, improved quality, and more standardized designs to reliably quantify risks.
{include}
