Vitamin D supplementation reduces many Cardiovascular Disease markers– meta-analysis
Vitamin D Supplementation, Serum 25(OH)D Concentrations and Cardiovascular Disease Risk Factors: A Systematic Review and Meta-Analysis.
Front Cardiovasc Med. 2018 Jul 12;5:87. doi: 10.3389/fcvm.2018.00087. eCollection 2018.
Mirhosseini N1, Rainsbury J2, Kimball SM1,3.
📄 Download the PDF from VitaminDWiki
A few of the many wonderful tables
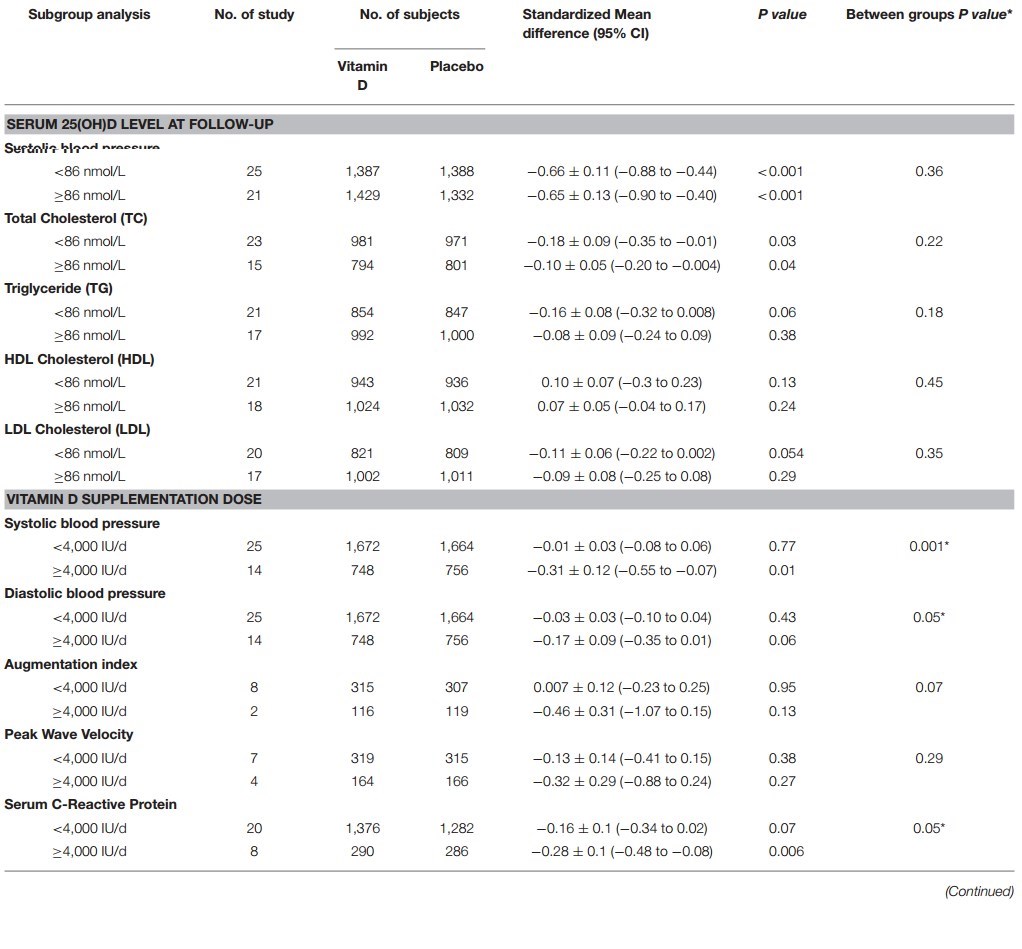

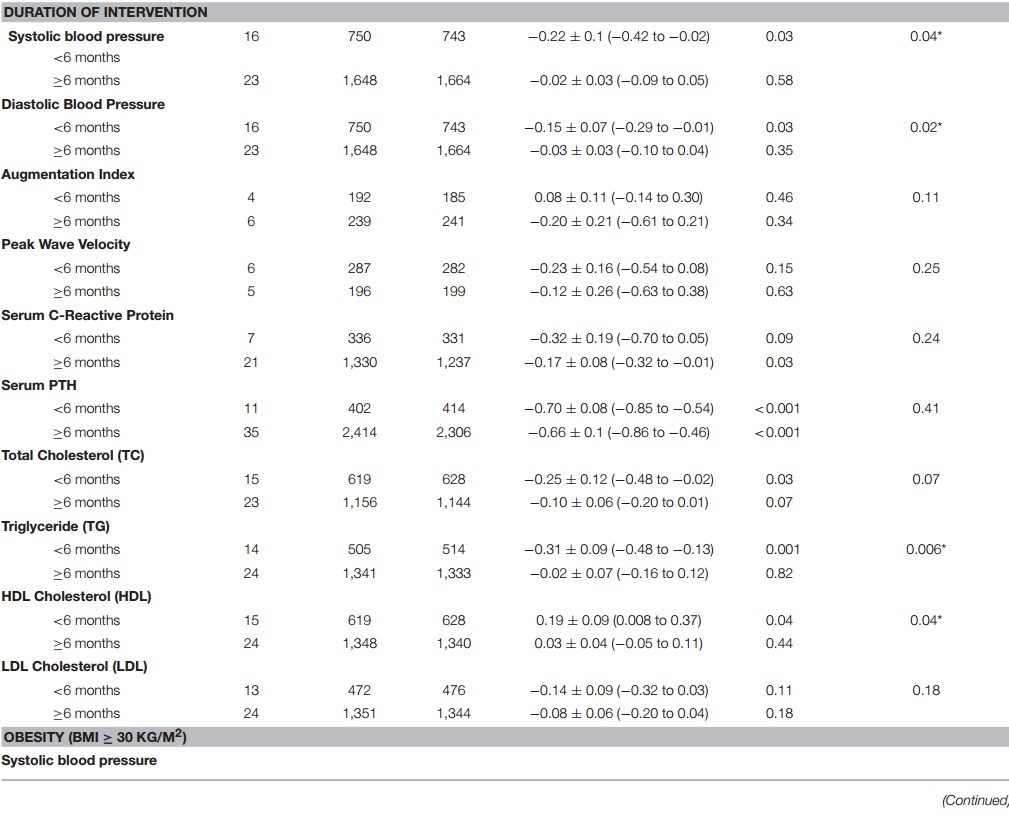
Background: Cardiovascular disease (CVD) risk factors are associated with low serum 25 hydroxyvitamin D (25(OH)D) concentrations in observational studies; however, clinical trial findings are inconsistent.
Objective: We assessed the effect of vitamin D supplementation and increased serum 25(OH)D concentrations on CVD risk factors in a systemic review and meta-analysis of randomized controlled trials (RCTs).
Design: MEDLINE, CINAHL, EMBASE, and Google Scholar were searched for RCTs that evaluated vitamin D supplementation and cardiovascular outcomes [blood pressure, parathyroid hormone (PTH), serum high-sensitivity C-reactive protein (hs-CRP), total cholesterol, high and low density lipoprotein (HDL and LDL, respectively), triglycerides, peak wave velocity (PWV) and Augmentation Index (AI)] from 1992 through 2017. Meta-analysis was based on a random-effects model and inverse variance method to calculate standardized mean difference (SMD) as effect sizes, followed by a leave-one-out method for sensitivity analysis. Risk of publication bias was assessed using Cochrane checklist and Begg funnel plots. The systematic review is registered as CRD42015025346.
Results: We identified 2341 studies from which 81 met inclusion criteria. The meta-analysis indicated a significant reduction in
systolic blood pressure (SMD = -0.102 ± 0.04 mmHg, 95% confidence interval (CI), -0.20 to -0.03),
diastolic blood pressure (SMD = -0.07 ± 0.03 mmHg, 95% CI, -0.14 to -0.006),
serum PTH (SMD = -0.66 ± 0.08 ng/L, 95% CI, -0.82 to -0.49),
hs-CRP (SMD = -0.20 ± 0.07 mg/L, 95% CI, -0.34 to -0.06),
total cholesterol (SMD = -0.15 ± 0.06 mmol/L, 95% CI, -0.25 to -0.04),
LDL (SMD = -0.10 ± 0.05 mmol/L, 95% CI, -0.20 to -0.003),
triglycerides (SMD = -0.12 ± 0.06 mmol/L, 95% CI, -0.23 to -0.003) and a significant increase in
HDL (SMD = 0.09 ± 0.04 mmol/L, 95% CI, 0.00 to 0.17)
with vitamin D supplementation. These findings remained significant in sensitivity analyses for blood pressure, lipid profile, serum PTH, and serum hs-CRP. There was no significant effect of vitamin D supplementation on PWV (SMD = -0.20 ± 0.13 m/s, 95% CI, -0.46 to 0.06, p = 0.14) and AI (SMD = -0.09 ± 0.14%, 95% CI, -0.37 to 0.19, p = 0.52) for vitamin D supplemented groups.
Conclusion: These findings suggest that vitamin D supplementation may act to protect against CVD through improving risk factors, including high blood pressure, elevated PTH, dyslipidemia, and inflammation.
