Blood vessels not helped by small vitamin D doses – meta-analysis
Effect of vitamin D supplementation on endothelial function – An updated systematic review with meta-analysis and meta-regression
Nutrition, Metabolism and Cardiovascular Diseases, Vol 29, Issue 12, Dec 2019, Pages 1261-1272, https://doi.org/10.1016/j.numecd.2019.08.005
📄 Download the PDF from Sci-Hub via VitaminDWiki
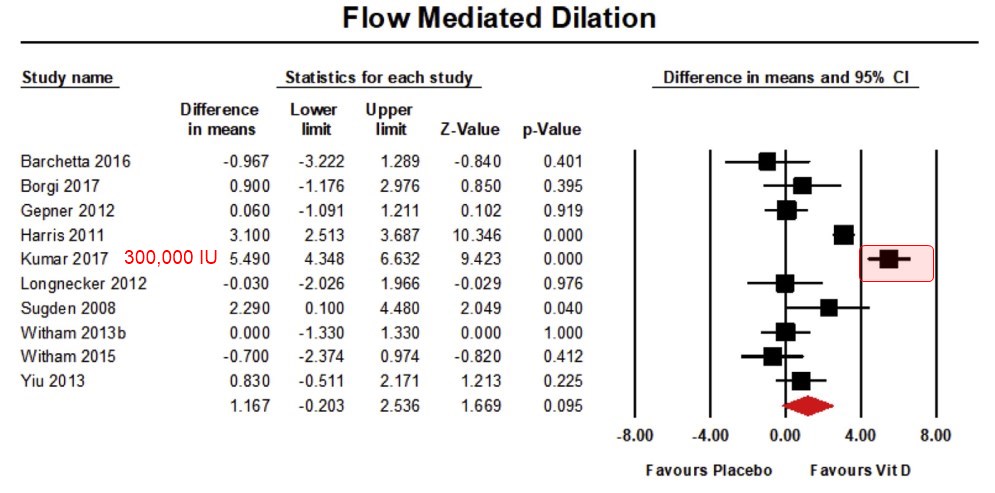
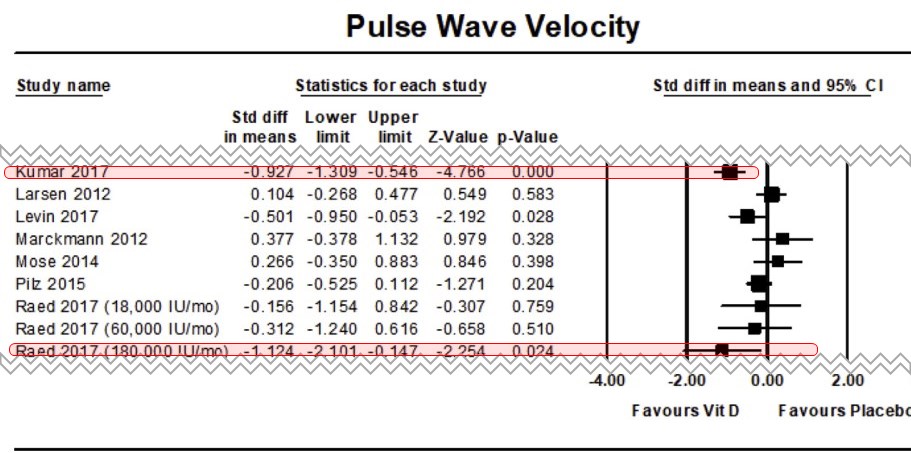
Highlighted the few studies which used enough vitamin D to make a difference
Note: Unfortunately most meta-analyses ignore dose sizes
Note: The founder of VitaminDWiki owns a pulse wave velocity meter which uses his iPad for analysis and display
His arteries have Pulse Wave Velocities of a person 20 years younger.
Background and aims
Atherogenesis and endothelial dysfunction contribute to cardiovascular risk and vitamin D has been implemented in endothelial repair. This systematic review, meta-analysis and meta-regression aims to establish the effect of vitamin D supplementation on endothelial function.
Methods and Results
To conduct the systematic review we searched the Cochrane Library of Controlled Trials, PubMed, ProQuest and EMBASE for randomized controlled trials that investigated the effects of vitamin D supplementation on flow-mediated dilation (FMD%), pulse wave velocity (PWV), and central augmentation index (AIx). Meta-analysis was based on a random effects model and inverse-variance methods to calculate either mean difference (MD) or standardized mean difference (SMD) as effects sizes. This was followed by meta-regression investigating the effect of baseline vitamin D concentrations, vitamin D dosing and study duration. Risk of bias was assessed using the JADAD scale and funnel plots.
We identified 1056 studies of which 26 studies met inclusion criteria for quantitative analysis. Forty-two percent of the 2808 participants had either deficient or insufficient levels of vitamin D. FMD% (MD 1.17% (95% CI −0.20, 2.54), p = 0.095), PWV (SMD −0.09 m/s (95% CI −0.24, 0.07), p = 0.275) and AIx (SMD 0.05% (95% CI −0.1, 0.19), p = 0.52) showed no improvement with vitamin D supplementation. Sub-analysis and meta-regression revealed a tendency for AIx and FMD% to increase as weekly vitamin doses increased; no other significant relationships were identified.
Conclusions
Vitamin D supplementation showed no improvement in endothelial function. More evidence is required before recommendations for management of endothelial dysfunction can be made.
