Atrial Fibrillation decreased by Vitamin D or Magnesium - many studies
Atrial Fibrillation DECREASED by Vitamin D or Magnesium
Atrial Fibrillation INCREASED by Calcium or high-dose Omega-3
23+ VitaminDWiki pages with AFIB or FIBRILLATION in title
This list is automatically updated
{LIST()}
- - - - See also 4 Cardiovascular diseases are associated with little vitamin D getting to cells – May 2023
5% less likely to get AFIB if 10 ng higher Vitamin D - Maga-analysis Sept 2023
Vitamin D, vitamin D supplementation and atrial fibrillation risk in the general population: updated systematic review and meta-analysis of prospective studies
Front Nutr. 2023 Sep 21:10:1246359. doi: 10.3389/fnut.2023.1246359
Xiaoli Ding 1, Jiying Lai 2, Hehui Zhang 2, Zongwen Guo 2
Background: Since the association of vitamin D with atrial fibrillation (AF) risk is still unclear, we conducted this updated meta-analysis of prospective studies to identify the relationship between vitamin D or vitamin D supplementation and AF in the general population.
Methods: We conducted a comprehensive search of multiple databases up to May 2023 for studies reporting vitamin D and AF. The hazard ratios (HRs) with 95% confidence intervals (CIs) were pooled by a random-effects model.
Results: A total of seven studies were included in this meta-analysis. Vitamin D deficiency (<20 ng/ml) was associated with increased AF incidence (HR: 1.12, 95% CI: 1.005-1.25). The HR was not significant with vitamin D insufficiency (20-30 ng/ml; HR: 1.09, 95% CI: 0.98-1.21). Each 10 ng/ml increase in serum vitamin D was associated with a significantly decreased AF incidence (HR: 0.95, 95% CI: 0.93-0.97). Two studies reported the effect of vitamin D supplements on AF incidence but reached inconsistent results.
Conclusions: Vitamin D deficiency or insufficiency was associated with an increased risk of AF in the general population. The role of vitamin D supplementation in AF prevention needs further investigation.
📄 Download the PDF from VitaminDWiki
23% less likely for seniors to get AFIB if 10 ng higher Vitamin D – 13 studies – 2019
The relationship between vitamin D and risk of atrial fibrillation: a dose-response analysis of observational studies
Nutrition Journal volume 18, Article number: 73 (2019)
Xiao Liu, Wei Wang, Zhaochong Tan, Xin Zhu, Menglu Liu, Rong Wan & Kui Hong
Background
The relationship between serum vitamin D and atrial fibrillation (AF) or postoperative atrial fibrillation (POAF) in patients undergoing coronary artery bypass graft (CABG) is still debated. It is also unclear whether there is a dose-response relationship between circulating vitamin D and the risk of AF or POAF.
Methods
The Cochrane Library, PubMed, and Embase databases were searched for relevant studies. We used a “one-stage approach” with a restricted cubic spline model to summarize the dose-specific relationships between serum vitamin D and AF. Relative risk (RR) was used to measure the effects in this meta-analysis.
Results
In total, 13 studies were included with a total of 6519 cases of AF among 74,885 participants. Vitamin D deficiency (< 20 ng/ml) was associated with increased risks of AF (RR: 1.23, 95% CI: 1.05–1.43). In the dose-response analysis, the summary RR for a 10 ng/ml increased in vitamin D was 0.88 (95% CI: 0.78–0.98) and there was no evidence of a non-linear association, P non-linearity = 0.86.
In the age subgroup, high vitamin D (per 10 ng/ml increase) reduced the risk of AF in the
older group (> 65 years) (RR = 0.68, 95% CI = 0.52–0.89)
but not among young individuals (< 65 years) (RR = 0.87, 95% CI = 0.72–1.06).
In addition, a strong association was found between a 10 ng/ml increased in vitamin D and POAF incident in the patient after CABG (RR: 0.44, 95% CI: 0.24–0.82).
Conclusion
Our dose-response meta-analysis suggested serum vitamin D deficiency was associated with an increased risk of AF in the general population and POAF in patients after CABG. Further studies are needed to explore the age difference in the association between serum vitamin D level and the risk of AF and whether vitamin D supplements will prevent AF.
📄 Download the PDF from VitaminDWiki
Risk of Atrial Fibrillation Decreases if Vitamin D or Magnesium Increase - GRH Sept 2022
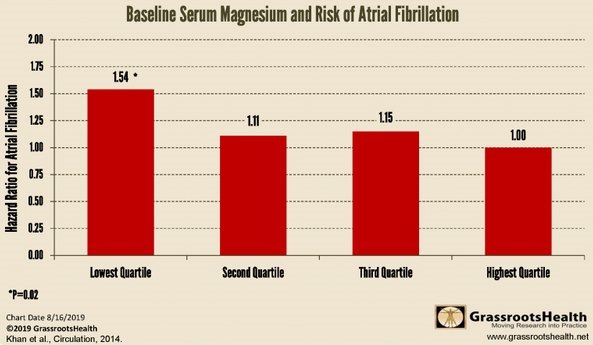
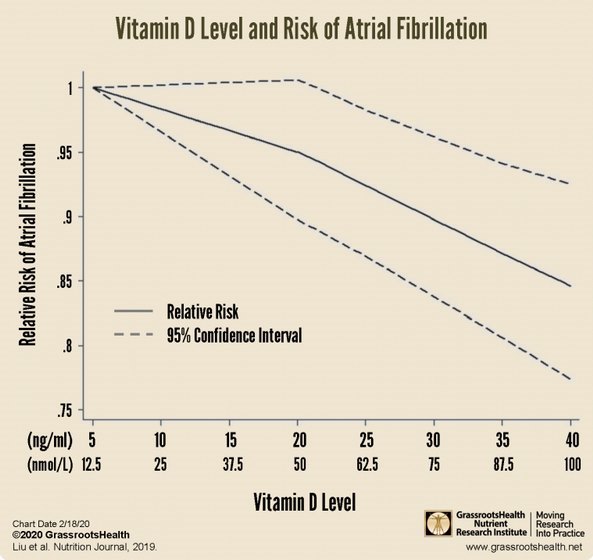
Risk of Atrial Fibrillation Decreases as Vitamin D and Magnesium Levels Increase - GRH Sept 2022
Includes the following graphs
The Pathogenesis of Cardiac Arrhythmias in Vitamin D Deficiency - May 2022
Biomedicines 2022, 10(6), 1239; https://doi.org/10.3390/biomedicines10061239
by Maria Barsan 1ORCID,Anca Monica Brata 2,*,Abdulrahman Ismaiel 3ORCID,Dinu Iuliu Dumitrascu 4,Andrei-Vlad Badulescu 5ORCID,Traian Adrian Duse 5ORCID,Stefana Dascalescu 5,Stefan Lucian Popa 3ORCID,Simona Grad 3,Lucian Muresan 6ORCID,Carmen Maria Maerescu 7,Gabriel Cismaru 8 andVlad Dumitru Brata 5ORCID
The global prevalence of vitamin D deficiency is more than 20%, and the main causes include insufficient intake, reduced absorption, abnormal metabolism, or resistance to its effects. The levels of serum vitamin D appear to influence cardiovascular risk, and the mechanism involved is linked to the transient outward current and the ultrarapid delayed rectifier K+ current densities, activated through the nuclear vitamin D receptor and Akt pathway. A significant number of studies have correlated vitamin D deficiency with an increased risk of developing cardiac arrhythmias and sudden cardiac death. For this reason, the purpose of this review is to analyze the relation between vitamin D deficiency and the pathogenesis of cardiac arrhythmias. Atrial fibrillation, increased QT interval, and QT dispersion were the most common findings associated with vitamin D deficiency. Due to the heterogeneity among existing studies, further research is necessary to confirm the existing data and to analyze its relationship with other types of arrhythmias
📄 Download the PDF from VitaminDWiki
High-Dose Omega-3 increases risk of atrial fibrillation - meta-analysis July 2021
Omega-3 fatty acids supplementation and risk of atrial fibrillation: an updated meta-analysis of randomized controlled trials
European Heart Journal - Cardiovascular Pharmacotherapy, Vol 7, Issue 4, July 2021, Pages e69–e70, https://doi.org/10.1093/ehjcvp/pvab008
Marco Lombardi, Salvatore Carbone, Marco Giuseppe Del Buono, Juan Guido Chiabrando, Giovanni Maria Vescovo, Massimiliano Camilli, Rocco Antonio Montone, Rocco Vergallo, Antonio Abbate, Giuseppe Biondi-Zoccai ...
📄 Download the PDF from VitaminDWiki
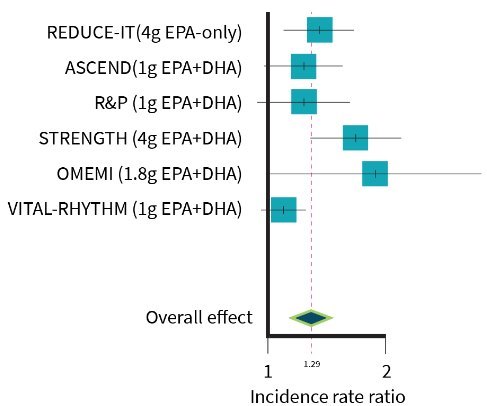
Editorial: High-Dose Omega-3 Fatty Acids and Atrial Fibrillation
Omega-3 Fatty Acids and Atrial Fibrillation - Editorial
AMA. 2021;325(11):1063. doi:10.1001/jama.2021.2909 FREE PDF
Gregory Curfman, MD1
In 2019, the global market for omega-3 fatty acids reached $4.1 billion, and it is expected to double by 2025.1 These impressive expenditures reflect the worldwide popularity of these products and the belief by many that omega-3 fatty acids are beneficial to their health. Although the health benefits of these products remain questionable, it is important for consumers who take them to understand their potential risks. In this issue of JAMA, the VITAL Rhythm Study2 examined the risk of atrial fibrillation (AF), the most common cardiac arrhythmia, with intake of omega-3 fatty acids.
In the past 2 years, 4 randomized clinical trials have provided data on the risk of AF with omega-3 fatty acid intake. In the STRENGTH trial,3 13 078 high-risk patients with cardiovascular disease were randomized to receive a high dose, 4 g/d, of a carboxylic acid formulation of omega-3 fatty acids (a combination of eicosapentaenoic acid [EPA] and docosahexaenoic acid [DHA]) or corn oil. After a median of 42 months, there was no significant difference between the 2 randomized groups in the primary composite cardiovascular end point, but there was an increase in risk of developing AF in the omega-3 fatty acids group compared with the corn oil group (2.2% vs 1.3%; hazard ratio, 1.69; 95% CI, 1.29-2.21; P < .001).
In the REDUCE-IT trial,4 8179 participants were randomized to a high dose (4 g/d, as in STRENGTH) of an omega-3 fatty acid preparation consisting of purified EPA (icosapent ethyl) or mineral oil. After a median follow-up of 4.9 years, icosapent ethyl resulted in a 25% relative reduction in the primary composite cardiovascular end point compared with mineral oil. As in STRENGTH, there was a significant increase in risk of AF with omega-3 fatty acids compared with mineral oil (5.3% vs 3.9%; P = .003).
In a third clinical trial, OMEMI,5 1027 older patients who had had a recent myocardial infarction were randomized to receive an intermediate dose, 1.8 g/d, of omega-3 fatty acids (a combination of EPA and DHA) or corn oil. After 2 years, there was no significant difference between the 2 groups in the primary composite cardiovascular end point, but 7.2% of the omega-3 fatty acids group vs 4.0% of the corn oil group developed AF (hazard ratio, 1.84; 95% CI, 0.98-3.45; P = .06).
In the VITAL Rhythm Study,2 published in this issue of JAMA, 12 542 participants were randomized to receive a standard dose of omega-3 fatty acids, 840 mg/d (a combination of EPA and DHA) and 12 557 to receive placebo. After a median of 5.3 years, the incidence of AF was 7.2 per 1000 person-years in those taking omega-3 fatty acids vs 6.6 per 1000 person-years in those taking placebo (hazard ratio, 1.09; 95% CI, 0.96-1.24; P = .19).
Considered together, the data from the 4 trials suggest, but do not prove, that there may be a dose-related risk of AF with omega-3 fatty acid intake. At a dose of 4.0 g/d, there was a highly statistically significant increase in risk (nearly a doubling). With an intermediate dose of 1.8 g/d, the increase in risk (hazard ratio, 1.84) did not achieve statistical significance, and with a standard daily dose of 840 mg/d, there was no apparent increase in risk (although the data were consistent with as much as a 24% increase in risk). Patients who choose to take omega-3 fatty acids, especially in high doses, should be informed of the risk of AF and followed up for the possible development of this common and potentially hazardous arrhythmia.
Cardiovascular category in VitaminDWiki
Starts with
{include}
Cardiovascular and Magnesium studies
{category}
Cardiovascular and Calcium studies
{category}
CLIFF NOTES FOR ATRIAL FIBRILLATION - May 2024
lots on Magnesium. He has another substack post just on Magnesium
