Vitamin D restricted in getting to cells by genes, obesity, etc
Sunlight exposure is just one of the factors which influence vitamin D status.
Photochem Photobiol Sci. 2017 Jan 31. doi: 10.1039/c6pp00329j. [Epub ahead of print]
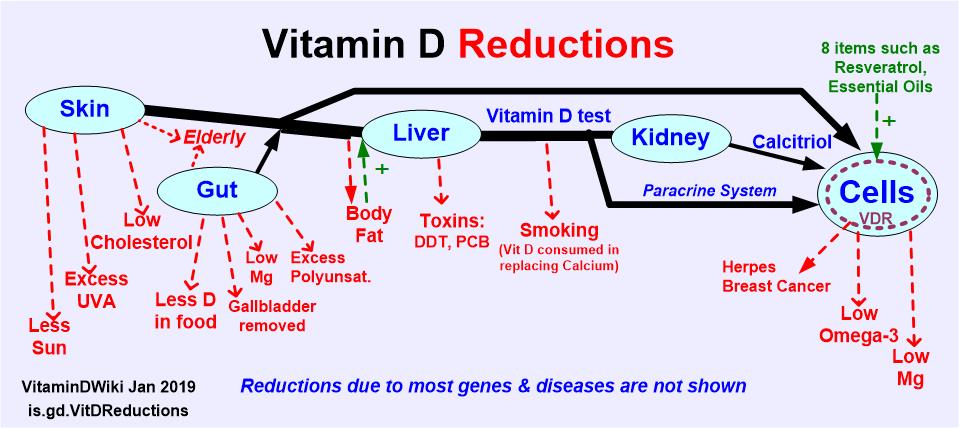 ::Click on chart for details::
Items in both of the categories of Genetics AND Obesity
{category}
::Click on chart for details::
Items in both of the categories of Genetics AND Obesity
{category}
Abboud M1, Rybchyn MS2, Rizk R3, Fraser DR4, Mason RS2.
1Physiology, School of Medical Sciences, Sydney Medical School, Australia. rebecca.mason@sydney.edu.au and Bosch Institute for Medical Research, Australia and College of Sustainability Sciences and Humanities-Zayed University, Abu Dhabi, United Arab Emirates.
2Physiology, School of Medical Sciences, Sydney Medical School, Australia. rebecca.mason@sydney.edu.au and Bosch Institute for Medical Research, Australia.
3Department of Health Services Research, CAPHRI School of Public Health and Primary Care, Maastricht University, Maastricht, 6200 MD Maastricht, The Netherlands.
4Faculty of Veterinary Science, University of Sydney, Sydney, NSW 2006, Australia.
Studies on the determinants of vitamin D status have tended to concentrate on input - exposure to ultraviolet B radiation and the limited sources in food. Yet, vitamin D status, determined by circulating concentrations of 25-hydroxyvitamin D (25(OH)D), can vary quite markedly in groups of people with apparently similar inputs of vitamin D.
There are small effects of polymorphisms in the genes for key proteins involved in vitamin D production and metabolism, including
7-dehydrocholesterol reductase, which converts 7-dehydrocholesterol, the precursor of vitamin D, to cholesterol,
CYP2R1, the main 25-hydroxylase of vitamin D,
GC, coding for the vitamin D binding protein which transports 25(OH)D and other metabolites in blood and
CYP24A1, which 24-hydroxylates both 25(OH)D and the hormone, 1,25-dihydroxyvitamin D.
25(OH)D has a highly variable half-life in blood. There is evidence that the half-life of 25(OH)D is affected by calcium intake and some therapeutic agents.
Fat tissue seems to serve as a sink for the parent vitamin D, which is released mainly when there are reductions in adiposity.
Some evidence is presented to support the proposal that skeletal muscle provides a substantial site of sequestration of 25(OH)D, protecting this metabolite from degradation by the liver, which may help to explain why exercise, not just outdoors, is usually associated with better vitamin D status.
PMID: 28139795 DOI: 10.1039/c6pp00329j
Publisher wants £ 42 for the PDF
