Rheumatoid Arthritis sometimes helped by very high dose vitamin D2 – 1935
THE TREATMENT OF RHEUMATOID ARTHRITIS WITH LARGE DOSES OF VITAMIN D - A CRITICAL EVALUATION
NATHAN R. ABRAMS, M.D., WALTER BAUER, M.D. BOSTON
In 1935 Dreyer and Reed 1 reported that they had previously observed 2 marked clinical improvement in the rheumatoid arthritis of two patients during the time they were receiving massive doses of vitamin D for hay fever. This original report and other reports by the same authors 3 have resulted in an increasing interest in the value of vitamin D in the treatment of rheumatoid arthritis as shown by subsequent reports.4
📄 Download the PDF from VitaminDWiki
Knowing that generalized décalcification is a common and at times an early manifestation of rheumatoid arthritis, one might be led to suspect that the chance observation of Dreyer and his co-workers 5 indicated that certain patients with rheumatoid arthritis suffer from some type of disease of calcium and phosphorus
If such were the case, then this chance observation might be of étiologie as well as of therapeutic significance. However, detailed studies of the calcium and phosphorus metabolism of patients with rheumatoid arthritis have failed to reveal metabolic changes of sufficient degree to allow one to conclude that the generalized décalcification is secondary to a primary disturbance of calcium and phosphorus metabolism.3 This being true, one might conclude a priori that any improvement noted in patients following the administration of vitamin D was not the result of correcting a previously existing alteration of the calcium and phosphorus metabolism. An additional reason for doubting that such is not the modus operandi of massive doses of vitamin D is suggested by our failure to observe any material alteration in the course of the disease in patients receiving from 5,000 to 15,000 U. S. P. units of vitamin D daily for as long as from six to thirty months. This dose of vitamin D, although not adequate for the cure of all diseases of calcium and phosphorus deficiency, is sufficiently large to correct a good percentage of them.
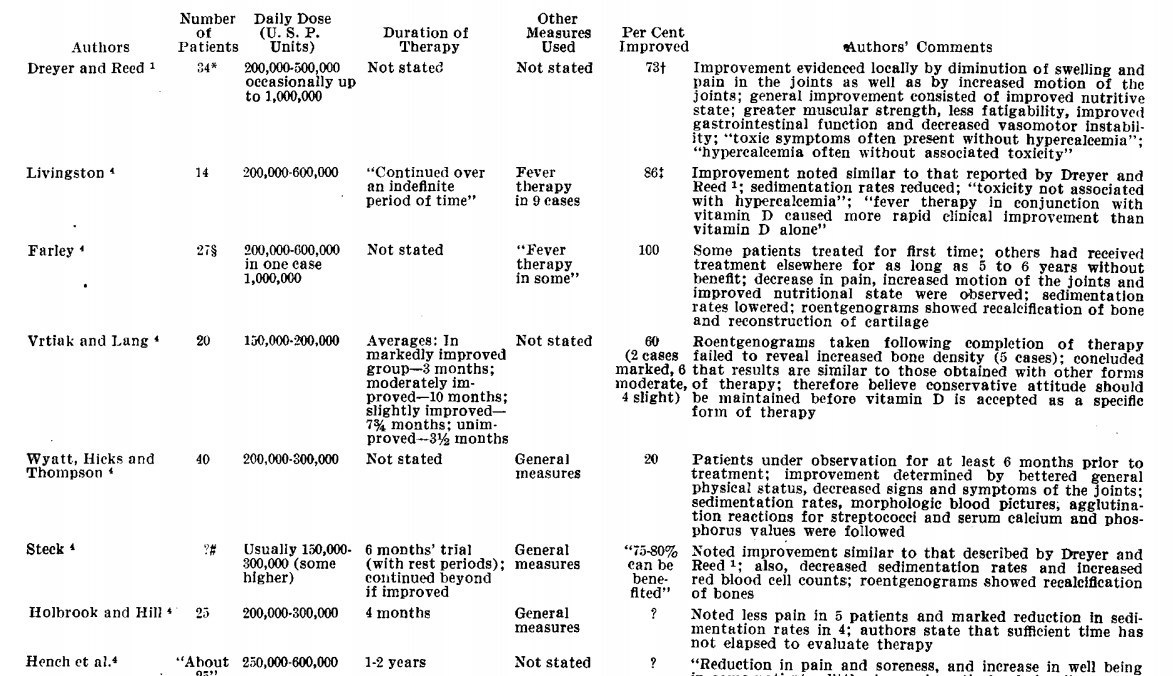
Irrespective of the aforementioned facts, Dreyer and Reed 1 reported improvement in twenty-five of thirty- four patients with rheumatoid arthritis treated with large doses of vitamin D, and others have reported equally encouraging results. Some reports have been less enthusiastic. Other workers11 have stated that further trial with this form of therapy is necessary before any final conclusions are drawn concerning its efficacy. The results obtained by previous workers are briefly summarized in table 1.
METHOD OF STUDY
Because of the therapeutic and étiologie significance that might be attached to the foregoing reports concerning a chronic disease of unknown etiology, it was deemed necessary to evaluate as critically as possible the therapeutic effectiveness of massive doses of vitamin D in the treatment of patients with rheumatoid arthritis. Since rheumatoid arthritis is a chronic disease of years’ duration, characterized by remissions and relapses of varying length and degree, the course of the disease may vary considerably from patient to patient. Therefore, in a study of this type, designed to determine the therapeutic effectiveness of a particular form of therapy, one must of necessity require that each person serve as his own control. Only in this way can one determine whether or not the therapy has altered the course of the disease. If this precaution is not taken, one will all too frequently conclude that the observed improvement is the result of the therapy employed, whereas it may represent nothing more than a natural fluctuation in the course of the disease. This manner of controlled study can best be accomplished by choosing only those patients whose clinical course has been known for months or years on a constant regimen prior to the institution of any so-called specific form of therapy. Equally important in this type of study is an adequate follow-up period on the same constant regimen employed prior to the institution of the form of therapy being studied. If each patient studied is so controlled, then one is best able to conclude whether the observed improvement or alteration in the course of the disease during and after treatment represents a therapeutic effect, a chance remission or the natural course of the disease. In all fairness to the form of therapy being studied, one should choose patients whose disease process is reversible. Any therapeutic measure employed in the treatment of rheumatoid arthritis should effect clinical improvement with great regularity in most patients before one has the right to suspect that one is dealing with a specific therapeutic therapy was being employed. It is extremely difficult to draw conclusions from much of the data presented in the reports concerning the therapeutic effectiveness of large doses of vitamin D in rheumatoid arthritis because the patients were not rigidly controlled and the degree of improvement was not accurately recorded.
We have observed eighteen patients with typical rheumatoid arthritis prior to, during and after the administration of large doses of vitamin D. Only five (66, 90, 286, 328 and J. H.) of the eighteen patients were hospitalized during the period of treatment. From table 2 one notes that in all instances the arthritis was in a stationary or progressive state prior to the insti-
agent. In studies of this type it is equally important to record improvement as accurately as possible by every available method. This is best accomplished by recording separately subjective, objective and laboratory evidence of improvement as well as grading the final result on the basis of all three. This method of appraisal enables one to evaluate more accurately any psychic effect, such as is so frequently encountered in patients with chronic disease following the institution of any new form of therapy.
Failure to consider these many facts in times past has been responsible for many premature therapeutic and étiologie claims, the inspiring of false hope in patients at great financial expense and at times progression of the disease because a good general regimen was not adhered to during the time the new form of tution of vitamin D therapy. It will be further noted that the duration of the arthritis, its severity and the extent of involvement varied from patient to patient. The observed therapeutic effects are recorded separately as subjective improvement, objective improvement, fluctuation in weight and alteration in the corrected sedimentation rate as well as the total end result. Determinations of fasting serum calcium, serum phosphorus and serum phosphatase were made every four to eight weeks in order to establish how often hypercalcemia resulted and whether or not suspected toxic symptoms occurred at the same time. Vitamin D in the form of Drisdol (1 drop = 250 U. S. P. units) was administered for a short time to the first five patients in the series. These and the remaining patients subsequently received a more concentrated preparation, crystalline vitamin D in propylene glycol (1 drop =1,000 U. S. P. units) or in sesame oil (1 drop == 25,000 U. S. P. units). One third or one fourth of the total daily dose was administered with each meal, and the fourth (when given) was taken at bedtime. All preparations were administered in milk, because Lewis has shown that the antirachitic vitamin dissolved in propylene glycol is better utilized in the medium of milk than in the medium of corn oil. Throughout the period of study all patients were kept on a constant therapeutic regimen consisting of a high vitamin, high caloric diet (unless overweight), regular rest periods, daily physical therapeutic measures, vitamin B in the form of yeast and a constant ration of acetylsalicylic acid. No new therapy was added during the period of observation.
RESULTS
Subjective Improvement. As can be seen from tables 2 and 3, if one were to judge solely on the basis of subjective improvement one might conclude that a good percentage of the patients with rheumatoid arthritis were benefited by vitamin D therapy. Subjective improvement, consisting of increased strength and feeling of well being, less of the myasthenia gravis- like fatigability and a reduction of pain and stiffness was reported by twelve of the eighteen patients. In four instances such improvement was short lived, being experienced only during the first few weeks of therapy. In the other eight cases such improvement was present throughout the period of treatment. In one instance it was marked, in another moderate, and in six slight. Such improvement was not maintained more than a few weeks following the discontinuance of vitamin D therapy.
Objective Improvement. When evidence of improvement is judged on the basis of objective changes, one notes from tables 2 and 4 that only five of the eighteen patients experienced benefit from vitamin D therapy . These five patients had also experienced subjective improvement. In four the objective improvement was slight; in one it was marked. From table 2 it will be seen that the patient (286) in whom improvement was marked received large doses of vitamin D on two different occasions and each time experienced marked objective as well as subjective improvement. The improvement observed each time consisted of marked reduction of soft tissue swelling, disappearance or marked reduction of effusions of the knee joints and an increase in motion of the joints. In the other three cases the improvement was less marked and consisted of slight reduction of the soft tissue swelling and increase in motion of the joints. In one case (66) involvement of the new joints occurred during therapy. Two patients (F. D. and C. M.) experienced marked remissions and exacerbations of signs and symptoms in the joints during the period of treatment, yet the dosage of vitamin D was kept constant throughout this time.
Weight Gam.—Improvement as measured by an appreciable weight gain (5 or more pounds) was observed in five patients (32, 120, 286, 328 and F. D.). Two of these patients (120 and 286) had noted subjective and objective improvement. Such beneficial effects were most marked in patient 286, who gained a total of 21 pounds (9.5 Kg.). Patients 32 and 328 had noted only subjective improvement, whereas Mrs. F. D. had exacerbations and remissions of both subjective and objective change.
Effect on the Sedimentation Rate.—From experience ro date, the corrected erythrocyte sedimentation rate 12 has proved to be the most reliable laboratory test for determining the activity of rheumatoid arthritis. This one objective laboratory test was performed at regular intervals before, during and after vitamin D therapy in order to determine whether the encountered variations in the sedimentation rate paralleled the observed clinical course of the disease.
In order to be consistent in judging when a decrease in the corrected sedimentation rate was significant, it was found necessary to follow some arbitrary rule.
Table 3.—Subjective Improvement
The one described here was finally adopted. In cases in which the sedimentation rate had varied between 0.5 and 1 mm. per minute a decreased rate was not considered significant unless it had fallen 0.15 mm. or more below the previously recorded rate. When the sedimentation rate had varied between 1 and 1.5 mm. per minute, a decrease of 0.2 mm. or more was considered significant. In cases in which the rate had been 1.5 mm. or more per minute a reduction was not considered significant unless it exceeded 0.3 mm. per minute.
In order to conserve space and yet give the reader some idea as to the changes observed in the curves of the sedimentation rate of each patient during the pretreatment, treatment and follow-up periods, the maximal-minimal variations for each patient are presented in table 2. Detailed curves of the sedimentation rate of four patients are presented in the accompanying chart. From the chart and table 2 one notes that alterations in the curves of the sedimentation rate were observed in only seven of the eighteen patients, but in only five was it significant. In cases 120 and 286 (as seen in the chart and in table 2) subjective and objective improvement took place at the same time. In case 286 a reduction in the sedimentation rate and clinical improvement were noted each time vitamin D was administered. In two other patients only subjective improvement was noted. The fifth patient, showing a lowered sedimentation rate, experienced no clinical improvement. Eleven of the remaining thirteen patients showed no significant alteration in the curve of the sedimentation rate. The sedimentation rates of the other two patients were increased, although both patients had considered themselves subjectively improved during the first weeks of therapy.
The observed changes in the sedimentation rates are difficult to interpret. That they cannot be of great significance is attested by the fact that both subjective and objective improvement was observed in only two of the eighteen cases studied. In fourteen cases the degree of variation encountered was as great in the pretreatment and follow-up periods as it was in the therapy period. In the chart, the variations in the curves of the sedimentation rates of the two patients who improved subjectively and objectively are compared with those of two patients who did not. These illustrated curves of the sedimentation rate serve to stress the fact that judging clinical improvement is extremely difficult even when a purely objective laboratory test is employed as the measuring stick. For instance, in case 120 the lowest sedimentation rate observed in the period of therapy was no lower than had been observed in the pretreatment period. One further observes that the sedimentation rate had begun to rise before vitamin D was discontinued. Although the changes observed in cases 120 and 286 may very well have been the result of vitamin D therapy, there is no denying the fact that they may represent, at least in part, the natural fluctuations that one frequently observes in patients receiving no specific therapy. Certainly one is not justified in drawing conclusions concerning improvement based on the sedimentation rate unless a significant sustained lowering takes place with some regularity in most patients during the period of therapy. Not having observed such an effect with any regularity in the eighteen cases studied, one is forced to conclude that vitamin D does not have any beneficial effect on the clinical course of rheumatoid arthritis as judged by the curve of the sedimentation rate. It was interesting to note that the greatest reductions in sedimentation rates frequently occurred at the time of the hypercalcemia. Such drops in the sedimentation rate were usually transient even though the hypercalcemia persisted. Variations of this type were encountered as often in those patients who did not experience clinical improvement as in those who did. This type of change in the sedimentation rate is probably directly related to the hypercalcemia and serves as further evidence that the variations in the sedimentation rates of erythrocytes cannot be ascribed to any one factor.
Final Result and Duration of Improvement.—The improvement noted always took place slowly. The best clinical and laboratory results were observed in case 286. These were observed each time vitamin D was administered but were never sudden or dramatic. The patient was hospitalized throughout each course of vitamin D therapy. The beneficial results in this case as in the others were short lived. During the follow-up study it was noted that the arthritis gradually became as severe as it had been in the pretreatment period.
Such changes were obvious in a few weeks. The other three patients who had experienced subjective and objective improvement fared no better. In the fourteen cases not materially influenced by vitamin D the arthritis ran the same pretreatment course during and after the period of administration of vitamin D. Results such as these serve to emphasize the fact that follow-up studies are needed.
HYPERCALCEMIA AND VITAMIN D TOXICITY
The pretreatment calcium, phosphorus and phosphatase values of all eighteen patients were normal, indicating as have previous studies that the calcium and phosphorus metabolism of rheumatoid arthritic patients as judged by the blood examination is normal. In sixteen of the eighteen patients hypercalcemia developed at some time during the period of vitamin D therapy. From table 2 it will be noted that hypercalcemia was noted only on one or two occasions in nine of the eighteen patients. In five instances (32, 41, 120, 127 and 229) there were no significant associated symptoms of toxicity, and the serum calcium returned to normal without alteration of the dose of vitamin D.
In cases 40, 221, 286 and F. D. either vitamin D was discontinued or the dose was reduced because of the degree of hypercalcemia or the severity of the toxic symptoms. In the other seven cases fasting serum calcium values varying from 11.2 to 16 mg. per hundred cubic centimeters persisted for weeks (from three to twenty-five) unless the dose of vitamin D was reduced or the drug discontinued. In most instances such values for hypercalcemia were not encountered until the dose was maintained between 160,000 and 200,000 U. S. P. units daily. However, a hypercalcemia of from 11.2 to 14.2 mg. per hundred cubic centimeters was observed in patient 335 for a period of twenty-five weeks, during which time the daily dose of vitamin D never exceeded 60,000 U. S. P. units. We were unable to exceed a dose of 200,000 U. S. P. units daily of the crystalline vitamin D in propylene glycol administered in milk without encountering toxic symptoms. Although the patients did tolerate larger doses of the crystalline vitamin D-sesame oil preparation, in no instance could we exceed a dose of 300,000 U. S. P. units daily without encountering serious toxic symptoms or hypercalcemia.
The toxic symptoms observed were similar to those previously described,20 consisting of anorexia, nausea, vomiting, epigastric distress or pain, diarrhea, headache, drowsiness, polyuria, polydipsia and nocturia. In some instances these symptoms were sufficiently marked to be alarming. Both the toxic symptoms and hypercalcemia often persisted for several weeks following discontinuance of the vitamin D therapy. An increased fasting serum phosphorus was observed on only two occasions. In these two instances values of 5.1 and 5.5 mg. per hundred cubic centimeters were observed with serum calcium values of 11.3 and 16.6 mg. In only one case did the serum phosphatase rise above a value of 5 Bodansky units. In this single instance a value of 6.5 units was observed with a normal serum calcium and phosphorus (10.2 and 3.4 mg. per hundred cubic centimeters respectively). As can be seen from table 2, the degree of hypercalcemia, its duration and the severity of the associated toxic symptoms were in no way related to the observed subjective and objective changes.
COMMENT
From the results observed in this series of patients with rheumatoid arthritis treated with large doses of vitamin D it is impossible to conclude that such therapy materially influences the course of the disease . Certainly the results are too disappointing to allow one to entertain the thought that one might be dealing with a specific therapeutic agent. If one were to judge solely on the basis of subjective and objective improvement experienced during the period of therapy only, one might be more enthusiastic concerning the value of vitamin D as a therapeutic agent for rheumatoid arthritis. When, however, a group of rheumatoid arthritic patients observed on the same constant general therapeutic regimen before, during and after the administration of large doses of vitamin D fail to show both clinical and laboratory evidence of improvement and no material alteration in the course of the disease, one is forced to conclude that the results are disappointing. Such an experience serves to stress the fact that each patient should serve as his own control and that adequate follow-up periods are necessary to judge the therapeutic results when one is dealing with a chronic disease such as rheumatoid arthritis. One might contend that beneficial effects are observed only while vitamin D is being administered. The data herein presented nullify such a contention. It might be argued that large doses of vitamin D are a useful addition to the therapeutic armamentarium employed in treating this disease. From our results we would conclude that the same general beneficial effects are experienced as often when vitamin D is administered in the usual therapeutic doses and that such dosages do not entail the risks attendant on hypercalcemia.
One might argue that failure to administer the same large doses of vitamin D employed by others is adequate reason for our not having obtained the same beneficial results previously reported. Evidence in favor of such an argument is readily obtained from tables 1 and 2, which show that only three patients in our series ever received a dose exceeding 200,000 U. S. P. units daily, whereas other workers have administered as much as 500,000 U. S. P. units or more daily . Because severe toxic symptoms or hypercalcemia were encountered in all but three patients whenever the daily dose exceeded 200,000 U. S. P. units, we did not feel justified in employing larger doses. As can be seen from table 2, hypercalcemia was encountered more frequently than were toxic symptoms. Of these two complications of vitamin D therapy the hypercalcemia is the more serious, because if it is allowed to persist extensive calcium deposits and other pathologic changes may ensue.
Other workers have reported that hypercalcemia and toxic symptoms are rarely encountered when large doses of vitamin D are administered, yet in our small series of patients receiving smaller doses hypercalcemia was observed in sixteen of the eighteen patients, and in seven cases it persisted *for weeks unless the dose of vitamin D was reduced or the drug was discontinued. There appears to be only one possible explanation for such discrepancies, namely that the vitamin D preparation administered to the patients in this series was always given in milk. The medium of milk, according to the work of Lewis,17 allows for better utilization of a solution of crystalline vitamin D in propylene glycol than does the medium of corn oil (the medium employed by Reed and others). Lewis’s results indicate that the antirachitic potency of such crystalline vitamin D preparations is increased tenfold when administered in milk. Whether a similar increased vitamin D potency resulted in our studies in consequence of the administration of the vitamin in milk we are unable to say with certainty. The high percentage of patients in whom hypercalcemia and toxic symptoms developed would suggest that such an increase in potency had occurred. If it did, then we were administering larger doses than the dosage in table 2 indicates. If this is true, the argument that failure to obtain better clinical results in this series was due to the employment of smaller doses no longer holds.
In order to be certain that the medium of propylene glycol might not be responsible for the high percentage of patients exhibiting toxic symptoms, this possibility was investigated. Propylene glycol was administered in milk to five patients in doses the same as or larger than they had received when taking the propylene glycol containing vitamin D. In no instance were any symptoms experienced; therefore this possibility is untenable.
Some workers have contended that the simultaneous administration of yeast will aid greatly in controlling or preventing the toxic symptoms associated with large doses of vitamin D. Such was not our experience. As previously stated, all our patients received yeast throughout the period of observation, yet in a large percentage toxic symptoms developed.
No increased calcification or intra-articular changes were demonstrable roentgenographically in this series or others following the administration of vitamin D. This is not surprising. We know that we are not dealing with a calcium and phosphorus deficiency disease and that the ability of articular cartilage to repair itself is at best very limited. Therefore we are skeptical of statements20 to the effect that filling in of rarefied areas and reconstruction of articular cartilage in cases of rheumatoid arthritis have been observed in consequence of large doses of vitamin D.
Most therapeutic discoveries are soon acclaimed by others and the original reports of the discoverers substantiated by further and more detailed reports. As in the case of many other previously discovered antirheumatic remedies, such acclaim and substantiations have not appeared. Until they do, one is hardly justified in prescribing an expensive therapeutic agent capable of producing toxic symptoms and serious pathologic changes. For these reasons the Council on Pharmacy and Chemistry of the American Medical Association has been unwilling to include in New and Nonofficial Remedies Ertron and other high potency viosterol preparations as being specific in the treatment of arthritis.27 If the beneficial results from vitamin D are to be ascribed to some impurity contained in the preparations employed, it had best be isolated and tested separately.
SUMMARY AND CONCLUSIONS
The effect of massive doses of vitamin D has been observed on eighteen patients with rheumatoid arthritis.
Observations prior to treatment showed that all the patients were in a stationary or slowly progressive state.
Subjective improvement lasting throughout the period of therapy was observed in eight cases. In only three instances was this accompanied by objective improvement and in only one was it marked. Such improvement was short lived when therapy was discontinued.
Only five patients showed a significant alteration in the curves of their sedimentation rate, and only two of these were improved subjectively and objectively.
Five patients gained weight during treatment.
Our results indicate that the administration of massive doses of vitamin D in rheumatoid arthritis is of little or no value in altering the course of the disease. The general effects of the larger doses do not appear significantly different from those observed with the usual therapeutic doses and do not justify the expense and dangers involved.
