Migraine Headache association with poor gut
Gut-brain Axis and Migraine Headache: A Comprehensive Review
Advanced Studies of the European Headache Federation (EHF-SAS)
Review J Headache Pain, 21 (1), 15 2020 Feb 13, DOI: 10.1186/s10194-020-1078-9
Mahsa Arzani 1, Soodeh Razeghi Jahromi 2, Zeinab Ghorbani 3, Fahimeh Vahabizad 1 4, Paolo Martelletti 5, Amir Ghaemi 6, Simona Sacco 7, Mansoureh Togha 8 9,
📄 Download the PDF from VSci-Hub via itaminDWiki
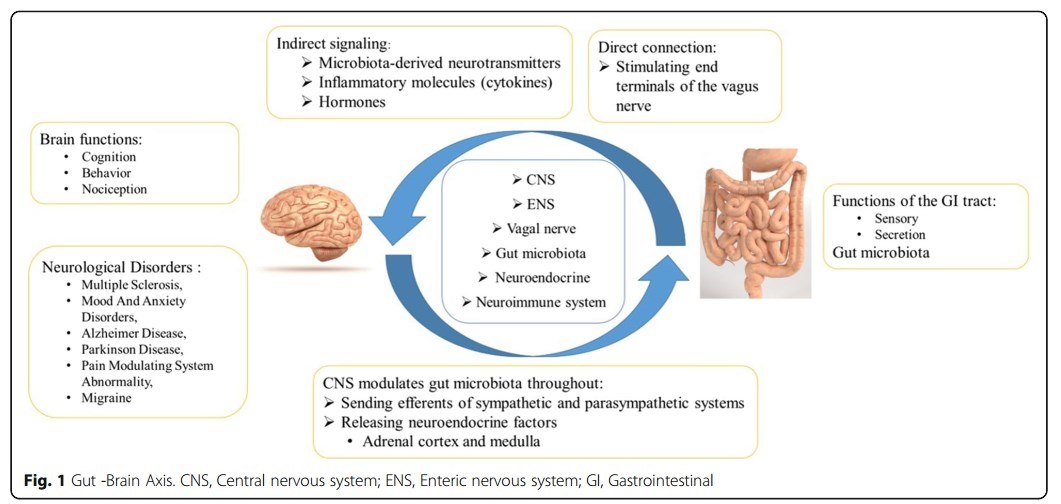
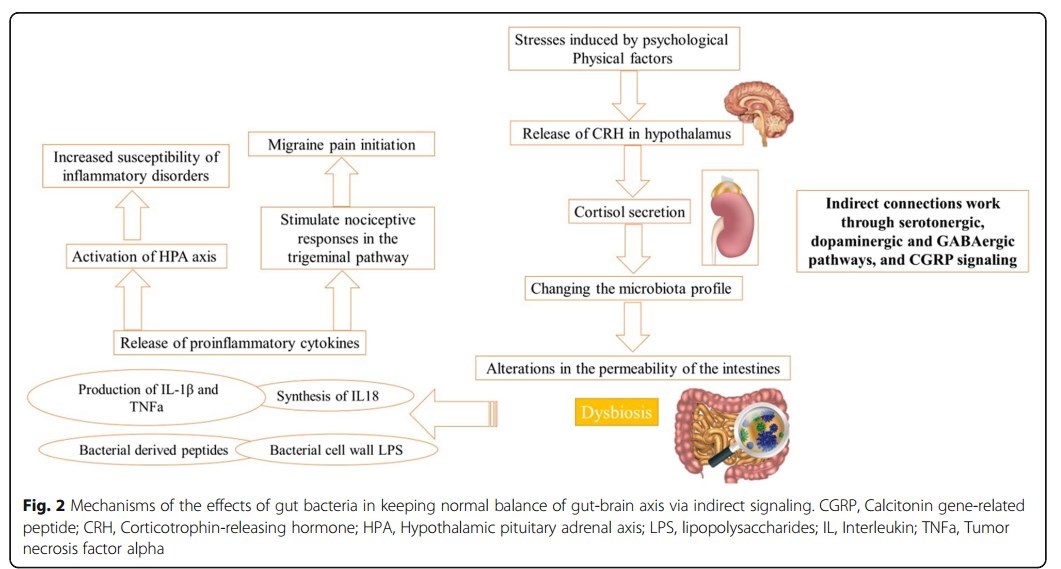
The terminology "gut-brain axis "points out a bidirectional relationship between the GI system and the central nervous system (CNS). To date, several researches have shown that migraine is associated with some gastrointestinal (GI) disorders such as
Helicobacter pylori (HP) infection,
irritable bowel syndrome (IBS), and
celiac disease (CD).
The present review article aims to discuss the direct and indirect evidence suggesting relationships between migraine and the gut-brain axis. However, the mechanisms explaining how the gut and the brain may interact in patients with migraine are not entirely clear. Studies suggest that this interaction seems to be influenced by multiple factors such as
inflammatory mediators (IL-1β, IL-6, IL-8, and TNF-α),
gut microbiota profile,
neuropeptides and serotonin pathway,
stress hormones and
nutritional substances.
Neuropeptides including CGRP, SP, VIP, NPY are thought to have antimicrobial impact on a variety of the gut bacterial strains and thus speculated to be involved in the bidirectional relationship between the gut and the brain. According to the current knowledge, migraine headache in patients harboring HP might be improved following the bacteria eradication.
Migraineurs with long headache history and high headache frequency have a higher chance of being diagnosed with IBS. IBS and migraine share some similarities and can alter gut microflora composition and thereby may affect the gut-brain axis and inflammatory status.
Migraine has been also associated with CD and the condition should be searched particularly in patients with migraine with occipital and parieto-occipital calcification at brain neuroimaging. In those patients, gluten-free diet can also be effective in reducing migraine frequency.
It has also been proposed that migraine may be improved by dietary approaches with beneficial effects on gut microbiota and gut-brain axis including appropriate consumption of fiber per day, adhering to a low glycemic index diet, supplementation with vitamin D, omega-3 and probiotics as well as weight loss dietary plans for overweight and obese patients.
