Vaginal Vitamin D reduced vaginal infections
Chronical cervical infections and dysplasia (CIN I, CIN II): Vaginal vitamin D (high dose) treatment - A new effective method?
Dermato-Endocrinology, el; January 2014; © 2014 Landes Bioscience
C Schulte-Uebbing , S Schlett, ID Craiut, L Antal and H olah
International Vitamin D Congress; University Charite; Berlin, Germany
In a small praxis/ambulance study we evaluated data of 200 women with chronical recurrent cervical infections and with a cervix dysplasia (CIN 1, CIN 2). who got after the primary therapy a treatment with vitamin D vaginal suppositories (12.500 IU, 3 nights a week, for 6 weeks). We found that - when compared with the lactobacillus vaginal suppositories - the high dose vitamin D vaginal treatment might be more effective. Vitamin D showed very good antiinflammatory effects. In the survey after six weeks therapy 79% of the women had "less vaginal problems," "less discharge" and "less problems with the sexual intercourse." Objectively after six weeks therapy only 7% of the patients still had bacterial and/ or fungal vaginal infections that required a treatment. We found that vitamin D is reabsorbed by the vaginal mucosa, but the reabsorption may be individually very different. In the CIN 1 group we found six weeks after treatment good antidysplastic effects, in the CIN 2 group we often found no or only temporary antidysplastic effects. So this vaginal vitamin D treatment method might be an option for the therapy and prevention of chronical cervical infections and maybe of a cervic dysplasia CIN 1 (good antiinflammatory effects, antidysplastic effects). This small study is not representative. We need much bigger studies with much more dates and with a longer follow up. Caution: At the moment we do not know, if the vaginal vitamin D treatment with 12500 IE is possible in pregnancy. We have no experience. Therefore we recommend an effective contraception during the application.
Introduction
In the last almost 20 y in our praxis/ambulance we treated some thousands of patients suffering from vaginal and cervical infections, many of them with a dysplasia of the cervix uteri. Some hundreds of them were so called "problem patients": they had persisting chronical vaginal and cervical infections, some of them four times a year—despite an adequate therapy (primary therapy with antibiotics/antimycotics acording to the antibiogram and secondary vaginal lactobacillus treatment).
For this study, we evaluated data of 200 "problem patients" with chronical recurrent cervical infections:
100 of them with chronical bacterial and/or fungal infections had no dysplasia.
100 of them with chronical bacterial and/or fungal infections had dysplasia. 50 with a CIN 1 and 50 with a CIN 2. Of the 50 CIN 1 patients 86% and of the 50 CIN 2 patients 92% had high risk of HPV.
Bacterial infections
Of the two hundred patients 51 had an infection with G. vaginalis, E. coli and/or coccus (Streptococcus, Staphylococcus), 44 patients mainly with coccus (Streptococcus, Staphylococcus), 16 patients mainly with G. vaginalis. 45 patients had a C. trachomatis infection, partially combined with bacterial mixed and/or fungal infection. Five patients had an infection with T. vaginalis, all plus coccus and/or C. trachomatis. (Fig. 1).
Fungal infections
Of the two hundred patients 39 patients had a fungal infection (above all with C. albicans), partially combined with a mixed bacterial infection. (Fig. 1).
Viral infections
Of the 50 CIN 1 patients 43 and of the 50 CIN 2 patients 46 had high risk of HPV (mostly type 16 and 18).
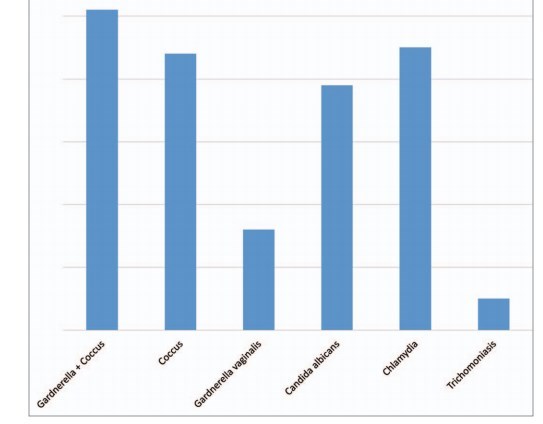
Figure 1. Data of 200 "problem patients" evaluated.
Percentage of bacterial and/or fungal infections before the treatment.
Patients, suffering from G. vaginalis + E. coli + Coccus (E. coli, Streptococcus, Staphylococcus) 25.5% n = 51.
Pat. suffering from Streptococcus, Staphylococcus 22% n = 44.
Pat. suffering from G. vaginalis 8% n = 16.
Pat. suffering from C. albicans 19.5% n = 39.
C. trachomatis (sometimes in combination coccus/candida) 22.5% n = 45.
T. vaginalis 2.5% n = 5.
Results
Vaginal vitamin D Reabsorption
The standard values for 25-hydroxy vitamin D in the serum:
< 30 ng/ml insufficient,
30—50 ng/ml sufficient,
50—70 ng/ml satisfying,
70 ng/ml good. 1
In our small praxis/ambulance study before the vaginal vitamin D treatment 100 of the 200 patients (=50%) had insufficient 25-hydroxy vitamin D serum values (< 30 ng/ml).
• Only 10 (=5%) had good 25-hydroxy vitamin D serum values (> 70 ng/ml)
• 20 (=10%) had satisfying 25-hydroxy vitamin D serum values (50-70 ng/ml)
• 70 (=35%) had sufficient 25-hydroxy vitamin D serum values (30-50 ng/ml)
• and 100 (=50%) had insufficient 25 hydroxy vitamin D serum values (< 30 ng/ml).
We could observe that most of our elder patients with estrogen deficiency colpitis had an extreme vitamin D deficiency. Obviously, in menopause with the increasing age, the vitamin D serum values are continously decreasing. We suppose that this might be caused by the metabolic, endocrin and intestinal deficits increasing with the age-also, the decreasing outdoor activities might contribute to this1-6 We were astonished, that some of our patients had insufficient 25-hydroxy vitamin D serum values (< 30 ng/ml), although they just had been in summer holidays and had got more than enough sun. Therefore, we come to the conclusion that the vitamin D food supply might be much more important than reported for many decades.
We could find that obviously vitamin D is reabsorbed by the vaginal mucosa. We found that the reabsorption was individually very different. But after treatment, 58 of these 100 patients (=58%) had vitamin D serum values (> 30 ng/ml).
Cervicitis without dysplasia group
Most of the patients subjectively and objectively had a benefit of the therapy. In the survey after six weeks therapy 79 of 100 women subjectively declared to have "less vaginal problems," "less discharge" and "less problems with the sexual intercourse." This we also could find objectively: After six weeks therapy only 7% of the patients still had bacterial and/or fungal vaginal infections that required a treatment.
Cervicitis and CIN 1 group
Immediately after six weeks of treatment only 10% still had a bacterial and/or fungal cervicitis. Of the 50 patients immediately after six weeks of treatment 24 patients were free of dysplastic cells (PAP III, PAP II or PAP I). Twenty-six patients still had a CIN 1. Of the 50 patients 21 still had a high risk of HPV, before the treatment 43 had a high risk of HPV
Cervicitis and CIN 1 group: Follow-up two years after
Unfortunately not all of the patients are still in our praxis/ ambulance. At the moment we also do not have the time and the manpower to make a perfect follow up evaluation. But of the 50 patients in the "Cervicitis and CIN 1" group we now can present the data of 20 patients among them:
Of these 20 patients in the Cervicitis and CIN 1 group two years after the therapy 15 patients had a better PAP (PAP I, II, II W, III)
Of these 20 patients in the Cervicitis and CIN 1 group three patients had a CIN 1 again, one patient had a CIN 2—3, one patient a CIN 3.
- These three patients needed and got a conization and a curettage (=15%).
- All three patients had a therapy resistant HPV high risk infection and chronical therapy resistant bacterial cervicitis (chlamydia trachomatis, coccus).
So of these 20 patients in three cases (= 15%) the vaginal vitamin D treatment was ineffective:
- Neither a cervicitis nore a higher grade dysplasia and operation could be prevented.
Cervicitis and CIN 2 group
Immediately after six weeks of treatment of the 50 patients in the Cervicitis and CIN 2 group eight patients (16%) still had a bacterial and/or fungal cervicitis that required a treatment. Of the 50 patients in the Cervicitis and CIN 2 group nine patients were free of dysplastic cells (PAP 2 or PAP 1). Seven of these nine patients were free of high risk HPV. Of the 50 patients in the Cervicitis and CIN 2 group 22 patients still had dysplastic cells, but with a better trend (CIN 1). Five of these 22 patients had no more high risk HPV infection. Of the 50 patients in the Cervicitis and CIN 2 group 19 patients immediately after the six weeks of treatment still had an unchanged CIN 2. All still had a high risk HPV infection. HPV: Of the 50 patients in the Cervicitis and CIN 2 group 38 patients still had a high risk HPV infection (before the therapy of the 50 patients 46 patients had a high risk HPV infection).
Cervicitis and CIN 2 group: Follow-up two years after
Unfortunately not all of the patients are still in our praxis/ ambulance. At the moment we also do not have the time and the manpower to make a perfect follow up evaluation. But of the 50 patients in the Cervicitis and CIN 2 group we now can present the data of 18 patients among them. Of these 18 patients in the "Cervicitis and CIN 1" group two years after the therapy in ten cases so far a conization and abrasio could be prevented. Two years after the therapy these ten patients have a better PAP (three patients have a PAP II, one patient has a PAP II W, six patients have a CIN 1). The other eight patients needed and got a conization and a curettage. So we found that in CIN 2 this method obviously had no or only short time antidysplastic effects.
Discussion
Vitamin D and chronical infections
The vaginal vitamin D treatment method (e.g., with OVID®) showed very good antiinflammatory effects. In the survey after six weeks therapy 79% of the women had "less vaginal problems," "less discharge" and "less problems with the sexual intercourse." Objectively after six weeks therapy only 7% of the patients still had bacterial and/or fungal vaginal infections that required a treatment.
So we found that when compared with the lactobacillus vaginal suppositories (e.g., with Vagiflor® etc.) the vaginal vitamin D treatment method (e.g., with OVID®) might be more effective. The OVID® vaginal vitamin D treatment seems to have good antiinflammatory effects and in case of a CIN 1 also antidysplastic effects.
Vitamin D: Hormonal effects
We know that Vitamin D is not only a vitamin but also a hormone. And it has important metabolic, endocrinological, immunolocical and anticancer effects. It is regulating the growth of the endocrine cells and protecting them from malignant growth. If there is a predisposition, a chronic vitamin D deficiency can promote the growth of hormone-dependant tumors. New studies show that vitamin D might be an important cancer prevention and therapy factor. With a sufficient vitamin D supply (daily at least 1,000 IU) the colon cancer risk can be reduced to 50%. It even can be reduced to one-third by a daily vitamin D supply with 2,000 IU.7-9 If there is a cancer predisposition, a chronical vitamin D deficiency can promote the formation and the growth of malignant tumors: vitamin D deficiency can raise the risk of breast,10 ovarian and prostate cancer.
Vitamin D deficiency and cancer
New studies show a correlation between vitamin D deficiency and lung, bladder, esophagean, gastric, rectal, larynx and pancreas cancer.11-13 In vitro studies with prostate cell cultures showed that vitamin D could stop their growth. We do not know yet if there is also a correlation between a vitamin D deficiency and a cervix dysplasia and a higher cervix carcinoma risk. But we found in our small praxis/ambulance study that before the vaginal vitamin D treatment 100 of the 200 patients (=50%) had insufficient 25-hydroxy vitamin D serum values (< 30 ng/ml).
Vitamin D against HPV
In the Cervicitis and CIN 1 group the vaginal vitamin D treatment method (e.g., with OVID®) seemed to have also some antiviral effects, in the Cervicitis and CIN 2 group we did not find this effect. At the moment we also do not know if the vaginal vitamin D treatment method (e.g., with OVID®) has any longer time effect on high risk HPV infections. We do not believe that the vaginal vitamin D treatment method (e.g., with OVID®) could be an alternative to the HPV vaccination.
Vitamin D against cervix dysplasia
In the CIN 1 group we found six weeks after treatment good antidysplastic effects, in the CIN 2 group we often found no or only temporary antidysplastic effects. So this vaginal vitamin D treatment method might be an option for the therapy and prevention of chronical cervical infections and maybe of a cervic dysplasia CIN 1 (good antiinflammatory effects, antidysplastic effects).
Unfortunately the vitamin D treatment method (e.g., with OVID®) was not as effective in the treatment of a CIN 2 as we had hoped starting the study. Regarding also the follow up we unfortunately found either no or only few and/or short time antidysplastic effects.
Conclusion
Immediately after six weeks treatment most of the two hundred patients—subjectively and objectively—had a benefit. So this vaginal vitamin D treatment method (e.g., with OVID®) might be an option for the treatment (and maybe also for the prevention ?) of lighter vaginal infections (colpitis and cervicitis) and maybe also of a CIN 1.
Contraindication Pregnancy
So far we do not know if the vaginal vitamin D treatment method with 12500 IE (e.g., with OVID®) can be problematic in pregnancy: In 2011, just when we were about to publish the method first time international in Arch Gyn Obs, one of our patients with chronical vaginal infections got pregnant during the vaginal vitamin D treatment. Unfortunately she had an early abortion (in the fifth/sixth week of pregnancy). We got some problems and very short time decided to withdraw the publication. We do not think that our vaginal vitamin D treatment method with 12500 IE (e.g., with OVID®) was the reason for this unfortunate course. On the contrary. Meanwhile there appeared some new publications (Holis et al., 2012, 2013) on the importance of vitamin D for the pregnancy and for the development of the embryo and fetus. But so far we are forced to make the following warning: WARNING: So far do not know, if the high dose vitamin D treatment with 12500 IE is possible in pregnancy. We have no experience. Therefore we recommend an effective contraception during the application.
This small praxis study is not representative. We need much bigger studies with much more dates and with a follow up.
Materials and Methods
Primary treatment
We treated the bacterial and fungal infections according to the antibiogram. In case of infections with G. vaginalis, C. trachomatis, Ureaplasma, Mycoplasma and Trichomonas vaginalis infections also the partner(s) was/were treated simultaneously. Infections with C. trachomatis, Mycoplasma and Ureaplasma were treated with tetracyclines. Fungal infections were treated with combined antimycotic prescriptions (vaginal suppositories and cream for the vulva and the intimate area),including the partner(s) treatment.
Secondary treatment
After this primary treatment, all patients got a secundary treatment with high dose vitamin D.
The first years we started with a treatment with vaginal tampons with 5000 IU vitamin D and olive oil (vitamin D on the long side of the tampon, every night, for six weeks).
Since 2008 we treated with OVID® (=standardized 2 g vaginal suppositories containing 12.500 IU vitamin D, neutral oil and adeps solidus), three nights a week, also for six weeks.
Prescription
Vitamin D vaginal ovules (for compounding pharmacies) e.g. OVID® Klosterl Apotheke Munchen, e.g., Rondell Apotheke Munchen; 12.500 IE Vit D (e.g., Vigantol®), neutral oil, adeps solidus q.s. XII/XXIV ovules, ad 2 g.
Why Vitamin D?
Meanwhile, a lot of studies prove not only the central function of vitamin D for the calcium and bone metabolism, but also its excellent antiinflammatory immunomodulating and antioxidative effects. Vitamin D is more than only a vitamin. Simultaneously in Central Europe there seems to be an endemic vitamin D deficiancy.3 Vitamin D is not only produced in the dermis and epidermis (induced by UV B ) but also orally ingested. Today we know, that the oral ingestion seems to be much more important than it was supposed for many decades. The endemic vitamin D deficiency seems to have three main causes obviously increasing with the age: Sunlight exposure deficits, vitamin D food supply deficits and intestinal resorption deficits (e.g., by dysbiosis, metabolic dysbalance, leaky gut syndrome etc.).14 Vitamin D has important metabolic, endocrinological, immunolocical and anticancer effects: it is regulating the growth of the endocrine cells and protecting them from malignant growth. If there is a predisposition, a chronic vitamin D deficiency can promote the growth of hormone- dependant tumors. Vitamin D also can prevent from chronical degenerative and cardiovascular diseases, from multiple sclerosis, rheumatoid arthritis, diabetes mellitus, Crohn's disease,14 hepatitis C15 etc. New studies show that vitamin D might be an important cancer prevention and therapy factor. With a sufficient vitamin D supply (daily at least 1,000 IU) the colon cancer risk can be reduced to 50%. It even can be reduced to one-third by a daily vitamin D supply with 2,000 IU.7-9 If there is a cancer predisposition, a chronical vitamin D deficiency can promote the formation and the growth of malignant tumors: vitamin D deficiency can raise the risk of breast,10 ovarian and prostate cancer. New studies show a correlation between vitamin D deficiency and lung, bladder, esophagean, gastric, rectal, larynx and pancreas cancer.11-13 In vitro studies with prostate cell cultures showed that vitamin D could stop their growth. After the vitamin D supply, the prostate cancer cells stopped their uncontrolled growth. The same reaction could be observed with colon and breast cancer cells. Mice getting injections with colon cancer cells showed a much slower tumor growth after vitamin D supplementation.1,4 Some gynecological publications are showing good vitamin D effects.5,6,16 Therefore, we had some reasons to do this small study.
References
1. Holick MF. Vitamin D deficiency. N Engl J Med 2007; 357:266-81; PMID:17634462; http://dx.doi.org/10.1056/NEJMra070553
2. Autier P, Gandini S. Vitamin D supplementation and total mortality: a meta-analysis of randomized controlled trials. Arch Intern Med 2007; 167:17307; PMID: 17846391; http://dx.doi.org/10.1001/ archinte.167.16.1730
3. Bayer W, Schmidt K. Besteht in Mitteleuropa ein endemischer Vitamn D Mangel? Erfahrungsheilkunde 2004; 53:609-13; http://dx.doi.org/10.1055/s-2004-834412
4. Lappe JM, Travers-Gustafson D, Davies KM, Recker RR, Heaney RP. Vitamin D and calcium supplementation reduces cancer risk: results of a randomized trial. Am J Clin Nutr 2007; 85:1586-91; PMID:17556697
5. Schulte-Uebbing C, Schlett S. Vitamin D bei PAP III D und Zervizitis. Dtsch Z Onkol 2010; 42:118 -22; http://dx.doi.org/10.1055/s-0030-1257719
6. Schulte-Uebbing C, Schlett S. Kolpitis und Co. Vaginale Vitamin-D Applikation hilft. Gynakologie und Geburtshilfe 2010.
7. Garland CF, Comstock GW, Garland FC, Helsing KJ, 12. Shaw EK, Gorham ED. Serum 25-hydroxyvitamin D and colon cancer: eight-year prospective study. Lancet 1989; 2:1176-8; PMID:2572900; http://dx.doi.13.org/10.1016/S0140-6736(89)91789-3
8. Jenab M, Bueno de Mesquita H B, Ferrari P, et al. Association between prediagnostic circulating vitamin D concentration and risk of colorectal cancer in 14. European populations: a nested case control study. BMJ 2010; 340:b5500.
9. Jenab M, et al. High vitamin D levels, lower colon cancer risk? EPIC Norfolk Publications 2010.
10. Garland CF, Gorham ED, Mohr SB, Grant WB, Giovannucci EL, Lipkin M, Newmark H, Holick MF, Garland FC. Vitamin D and prevention of breast cancer: pooled analysis. J Steroid Biochem Mol Biol 15. 2007; 103:708-11; PMID:17368188; http://dx.doi.org/10.1016/j.jsbmb.2006.12.007 16.
11. Grant WB. Relation between prediagnostic serum 25-hydroxyvitamin D level and incidence of breast, colorectal, and other cancers. J Photochem Photobiol B 2010; 101:130-6; PMID:20570169; http://dx.doi.org/10.1016/j.jphotobiol.2010.04.008
(end of references at VitaminDWiki - all references are in the PDF)
See also VitaminDWiki
Vaginal suppository of 6300 IU vitamin D stopped vaginal infection – Feb 2011 previous report by same authors
Vaginal microbiome varies with race, vitamin D level, preterm birth, etc. - March 2019
Candida infections in PICU reduced by Vitamin D in yogurt – RCT Feb 2019
Post menopausal vaginal dryness treated with vitamin D vaginal suppositories – RCT March 2015
Vitamin D and the Magic Mountain: The Anti-Infectious Role of the Vitamin
Sublingual vitamin D – technical 2008 suspect that sublingual is similar to vaginal absorption
Vitamin D reduced bacterial infection in cows – RCT Sept 2013
Recurrent urinary tract infection 4X more likely if low vitamin D – Aug 2013
Vaginosis not reduced by average of 2800 IU vitamin D daily – RCT Nov 2014
See also web HPV, but not Vitamin D
- Natural Herbal HPV "Cure" Discovered GreenMedInfo 2014
- Vaginal cream = extracts of curcumin, reetha, amla and aloe vera, known by the trade name Basant; for 1 month
- HPV clearance rate in Basant arm (88%) was significantly higher than the combined placebo arms (73%)."
- Vaginal cream = extracts of curcumin, reetha, amla and aloe vera, known by the trade name Basant; for 1 month
