Vitamin D3 becomes Calcidiol which becomes Calcitriol
Cholecalciferol (ko-ler-cal-'si ferol) = vitamin D3, from diet or your skin (from cholesterol and UV)
{img fileId="2696" width ="700"}
click on chart to see it larger, along with description
Liver uses enzymes to add water ==> Calcidiol (kal-sĭ-dī′ol)
25-hydroxy-vitamin-D
25(OH)D
what a blood test measures
stored all around the body, including in the blood
appears to last for weeks (> about 50 ng) to months (< about 30 ng)
Kidneys and paracrine system use other enzymes to add more water ==> Calcitriol (KAL-si-TRYE-ole)
1,25-di-hydroxy-cholecalciferol
1,25(OH)2D
lasts only a few days in the body
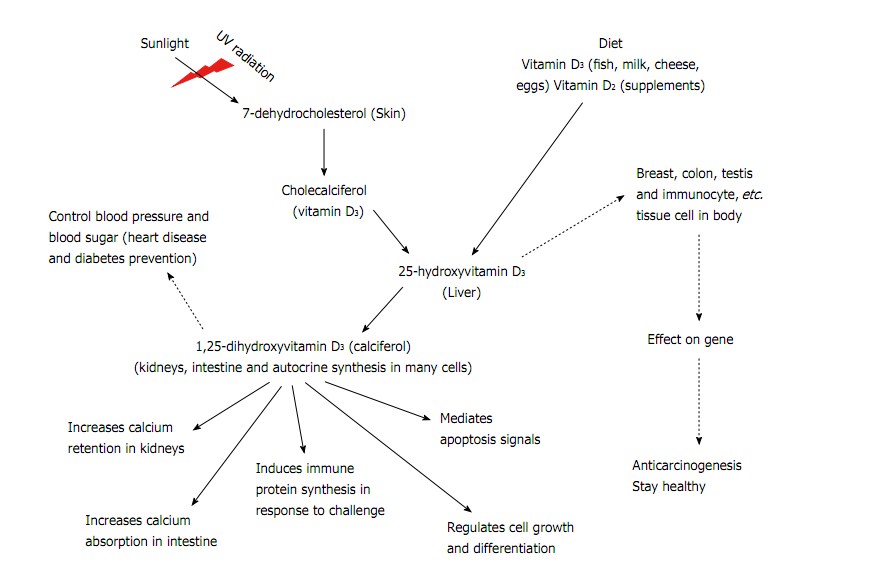
The above image is from This page

The above image is from This page
Oct 2011 800 IU double blind of Vitamin D3 and Calcidiol (note: oral not injection)
URICH—Blood levels of vitamin D increased and were more sustained by oral supplementation with 25(OH)D(3) than they were with vitamin D3 supplementation, as were improvements to lower extremity function, according to new research from University Hospital Zurich; both forms improved several markers of innate immune function. The results were published online ahead of print Oct. 25 in the Journal of Bone and Mineral Research.
Twenty healthy postmenopausal women with an average 25(OH)D level of 13.2?ng/ml (SD?=?±?3.9) and a mean age of 61.5 years (SD?=?±?7.2) were randomized to receive either 20?µg of 25(OH)D(3), also known as calcidiol, or 20?µg (800 IU) of vitamin D(3) per day in a double-blind design. During 14 visits over the course of four months, researchers measured 25(OH)D serum levels, blood pressure, and 7 markers of innate immunity (eotaxin, IL-8, IL-12, IP-10, MCP-1, MIP-1?, RANTES). They also tested for lower extremity function (knee extensor and flexor strength, timed up and go, repeated sit-to-stand) at baseline and at four months, adjusting for baseline measurement, age and body mass index (BMI) in all analyses.
In the calcidiol group, mean 25(OH)D levels increased to 69.5?ng/ml, and the rise was more immediate and sustained compared to the D3 group, which showed a slow increase to 31.0 ng/ml. The calcidiol group also had a 2.8-fold increased odds of maintained or improved lower extremity function (OR= 2.79; 95%CI: 1.18-6.58), compared to the D3 group, and a 5.7 mmHg decrease in systolic blood pressure. Both types of vitamin D were linked to a decrease in 5 out of 7 markers of innate immunity, although decreases for eotaxin, IL-12, MCP-1 and MIP-1 ? were significantly more pronounced with calcidiol. The researchers noted there were no cases of hypercalcemia at any time point in the study.
[Full paper is on VitaminDWiki at Vitamin D3 vs serum D3 (Calcitriol, HyD) – Jan 2012]
Calcidiol form of vitamin D is better – Feb 2014
Pharmacokinetics of oral vitamin D(3) and calcifediol
Bone. 2014 Feb;59:14-9.
Jetter A, Egli A, Dawson-Hughes B, Staehelin HB, Stoecklin E, Goessl R, Henschkowski J, Bischoff-Ferrari HA.
AIM:
Long-term pharmacokinetics after supplementation with vitamin D3 or calcifediol (the 25-hydroxyvitamin D3 metabolite) is not well studied. Additionally, it is unclear whether bolus doses of vitamin D3 or calcifediol lead to 25(OH)D3 plasma concentrations considered desirable for fracture prevention (30 ng/mL). We therefore investigated plasma pharmacokinetics of 25(OH)D3 during different vitamin D3 and calcifediol supplementation regimens.
METHODS:
In this seven-arm, randomized, double-blind, controlled parallel-group study, 35 healthy females aged 50–70 years (5 per group) received 20 μg calcifediol or vitamin D(3) daily, 140 μg calcifediol or vitamin D(3) weekly, for 15 weeks, or a single bolus of either 140 μg calcifediol, or vitamin D(3), or both. 25(OH)D3 plasma concentrations were quantified using LC–MS/MS in 14 clinical visits among all participants.
RESULTS:
For daily (weekly) dosing, the area under the concentration–time curve (AUC0–24h), which is the measure for exposure, was 28% (67%) higher after the first dose of calcifediol than after the first dose of vitamin D3. After 15 weeks, this difference was 123% (178%). All women in the daily and weekly calcifediol groups achieved 25(OH)D3 concentrations > 30 ng/mL (mean, 16.8 days), but only 70% in the vitamin D3 daily or weekly groups reached this concentration (mean, 68.4 days). A single dose of 140 μg calcifediol led to 117% higher 25(OH)D3 AUC0–96h values than 140 μg vitamin D3, while the simultaneous intake of both did not further increase exposure.
CONCLUSIONS:
Calcifediol given daily, weekly, or as a single bolus is about 2–3 times more potent in increasing plasma 25(OH)D3 concentrations than vitamin D3.
Plasma 25(OH)D3 concentrations of 30 ng/mL were reached more rapidly and reliably with calcifediol.
PMID: 24516879
Calcifediol = calcidiol = 25-hydroxycholecalciferol = 25-hydroxyvitamin D = 25(OH)D)
See also VitaminDWiki
Overview Liver and vitamin D probably should consider Calcidiol if have liver problems or perhaps have had gallbladder removed
Nano-encapsulated of Vitamin D3, Calcidiol, calcitriol look promising, esp time release – Dec 2012 7 day!!
Time-release form of active vitamin D granted a patent for chronic kidney disease – July 2014
Calcidiol may be 5X more effective than Vitamin D3 – June 2012
Application to FDA for use of active Vitamin D for hemodialysis patients – July 2011
Active form of vitamin D appears to help prevent and treat some cancers – Feb 2011
Some form of vitamin D may be the lowest cost treatment for CKD – Spanish Sept 2011
Calcitrol was as effective as Vitamin D analogues, and 17X less costly – May 2012
PhD Dissertation - Local production of active vitamin D inhibits Prostate Cancer – Oct 2012
Pre-cursor of active vitamin D made from plants is better than calcitriol – Sept 2012
- Time to get peak response: 6-12 hours instead of 1 hour
Search VitaminDWiki for Calcitriol 948 hits Jan 2014
25-Hydroxyvitamin D3 suppresses hepatitis C virus production – Oct 2012
Kidney not essential for Vitamin D3 activation – fungi can do it – Jan 2014
Getting Vitamin D into your blood and cells detials on the above chart
See also Web Calcitriol Injection
- Description at Drugs.com
- Calcitriol when administered by bolus injection is rapidly available in the blood stream.
- The pharmacologic activity of an administered dose of calcitriol is about 3 to 5 days .
- Description at Medicine.net
- This medication is given by injection into a vein, usually by a health care professional 3 times a week (every other day), or during dialysis
- Rockwell announced launching Calcitriol injection for secondary hyperparathyroidism May 2012
PubMed search for calcitriol and kidney in the title/abstract 774 items as of Nov 2020
Plain vitamin D or active vitamin D in the treatment of osteoporosis: where do we stand today? - Nov 2020 doi: 10.1007/s11657-020-00842-0.
Vitamin d in the patients with chronic kidney disease: when, to whom and in which form. April 2015
http://www.drugs.com/mtm/calcitriol.html Precautions
http://www.drugs.com/ppa/calcitriol.html
http://www.wisegeek.com/what-is-calcitriol.htm Wise Geek 1 page overview
http://www.healthline.com/goldcontent/calcitriol interactions and side-effects
http://www.vitamindcouncil.org/vitaminDPhysiology.shtml has the following
Calcitriol (1,25(OH)2D3 or 1,25D3) - Calcitriol (1,25-dihydroxyvitamin D) is made from calcidiol in both the kidneys and in other tissues and is the most potent steroid hormone derived from cholecalciferol. Calcitriol has powerful anti-cancer properties. It is sometimes referred to as the active form of vitamin D. Calcitriol levels should never be used to determine if you are deficient in vitamin D.
Cochrane review found vitamin D and Calcitriol helped with Kidney
Why Dialysis Patients Need Combination Therapy with Both Cholecalciferol and A Calcitriol Analogs.
Semin Dial. 2010 May 10. Jones G.
Departments of Biochemistry and Medicine, Queen's University, Kingston, Ontario, Canada.
The roles of vitamin D, mediated through its conversion to 1,25-dihydroxyvitamin D(3) (calcitriol), have been expanded recently through new knowledge about the range of tissues capable of activating it and the breadth of the genes under its regulatory control. This basic science together with the fact that numerous studies across North America are revealing that vitamin D insufficiency/deficiency (as defined by 25-OH-D levels <30 ng/ml) is extremely common (>80%) in dialysis patients are indicative that these patients have two vitamin D-related problems that require different treatment regimens. Combinations of vitamin D(3) (cholecalciferol) or vitamin D(2) (ergocalciferol) and an active calcitriol analog should be used to treat their vitamin D deficiency and their calcitriol hormone insufficiency, respectively. This mini-review provides the case for combination therapy. PMID: 20492584
[tiki-download_file.php?fileId=1172]
The journal article has images showing the pathways of vitamin D thru the kidney
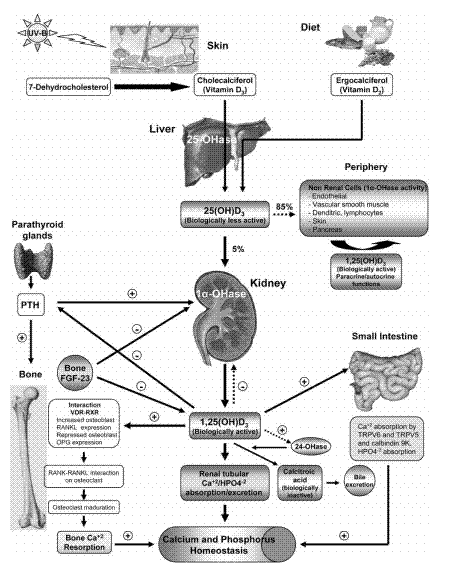
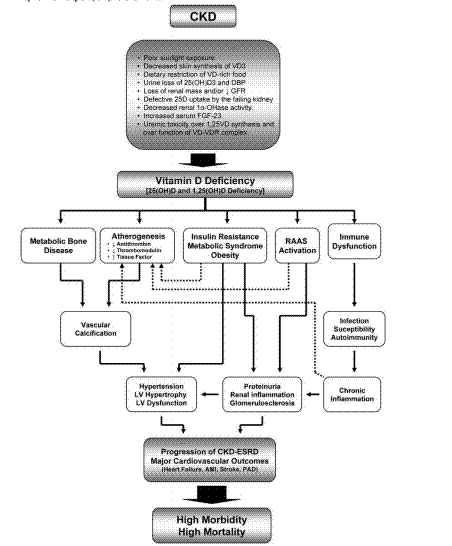
The way we used to think about vitamin D has it being converted in the kidney
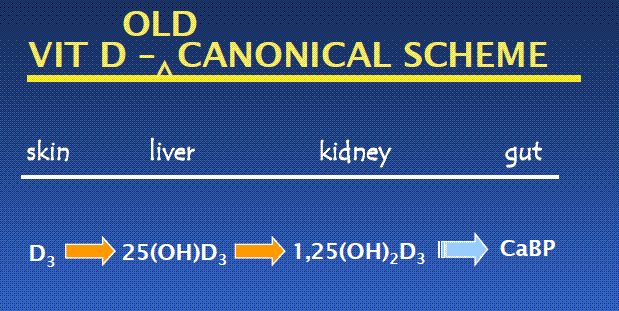
But now we realize that it has a minor role for other than the gut
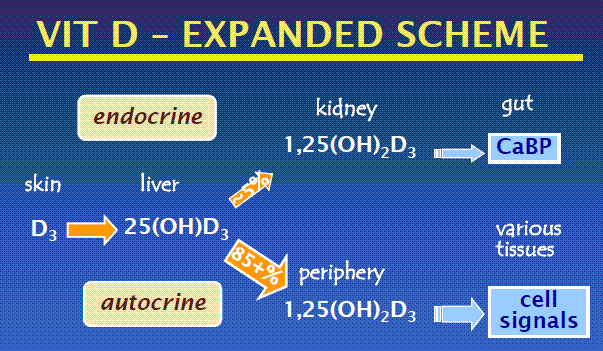
Both from April PDF or Video at 2010 http://www.ucsd.tv/search-details.aspx?showID=18718
Calcitriol is far more expensive than Vitamin D3, but far less than the co-pay for an injection
There are a few sources for it on the internet for $40+ which require a prescription, but most are $100 to $200
At about $2 per 1/2 microgram pill, they are far less expensive than just the co-pay for getting injections at the doctor's office.
And, would be far easier than having to get an injection every 4 days for the rest of your life.
Note: Caclitriol is the unlabeled line which is the output of the kidney/Paracrine system
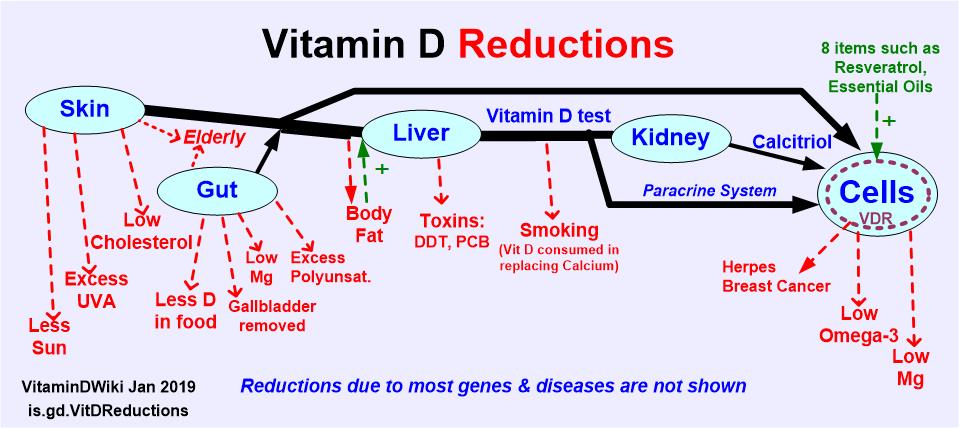
Treat with Calcidiol if liver is malfunctioning - Review Nov 2013
Calcidiol [25(OH)D3]: from diagnostic marker to therapeutical agent.
Curr Med Res Opin. 2013 Nov;29(11):1565-72. doi: 10.1185/03007995.2013.838549. Epub 2013 Sep 13.
Brandi ML1, Minisola S. 1Department of Surgery and Translational Medicine, University of Florence , Italy.
OBJECTIVE:
Osteoporosis is a skeletal disorder characterized by diminished bone strength, which results in an increased risk of fracture. Currently, osteoporosis is a public health priority due to the large number of individuals affected and the detrimental effect on quality of life. Primary osteoporosis, the most common form, usually results from age-related reduction in bone mineral strength. Over time, the individual's capacity to build bone is impaired, as the synthesis of vitamin D, the hormone responsible for calcium absorption, tends to decline. As serum calcium levels decrease, metabolic control serves to increase the removal of calcium from the skeleton to make up for the deficit. The synthesis of the 'hormone' vitamin D and its control therefore become central to intervention in involutional osteoporosis syndromes. In humans, plain vitamin D (cholecalciferol), also called parental or native vitamin D, is photosynthesized in the skin and then hydroxylated in the liver into the vitamin D analog calcidiol [25(OH)D3], which is hydroxylated again in the kidney into the vitamin D analog calcitriol [1,25(OH)2D3].
The advantage of administering vitamin D analogs is that the pro-drug calcidiol avoids the effect of declines in hepatic function , while calcitriol avoids the effect of declines in hepatic and kidney function. A strategy to enhance [25(OH)D3] levels to the optimal threshold of vitamin D is supplementation with the calcidiol metabolite itself. The goal of this paper is to review published studies on the efficacy of the calcidiol metabolite in increasing 25(OH)D3 serum levels and improving skeletal health parameters in humans.
METHODS:
A library search of published papers in the area of use of calcidiol in humans from 1967 to 2013 was performed (key words: calcidiol, 25-hydroxy-vitamin D3, vitamin D supplementation, vitamin D metabolism, osteomalacia).
RESULTS AND CONCLUSION:
The results of the survey made it possible to conclude that calcidiol is characterized by a number of features that make the compound ideal in conditions that require supplementation with a 25-hydroxylated metabolite.
PMID: 24020910
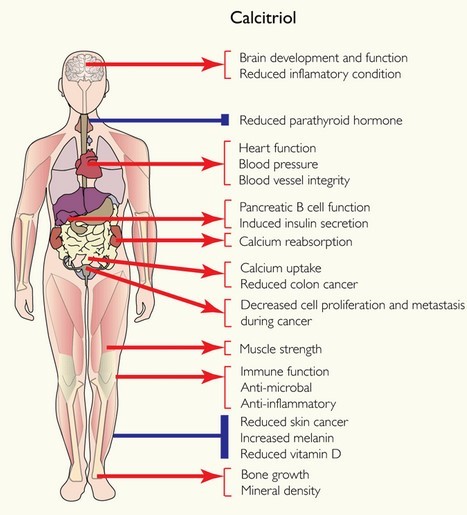
Calcitriol benefits to the body
VITAMIN D: A NATURAL WONDER DRUG WE’RE ALL AVOIDING? National Institue for Medical Research 2012