Crohn's disease in black children is worse in 6 ways
Racial disparities in readmission, complications, and procedures in children with Crohn's disease.
Inflamm Bowel Dis. 2015 Apr;21(4):801-8. doi: 10.1097/MIB.0000000000000325.
Dotson JL1, Kappelman MD, Chisolm DJ, Crandall WV.
📄 Download the PDF from VitaminDWiki
BACKGROUND:
Racial disparities in care and outcomes contribute to mortality and morbidity in children; however, the role in pediatric Crohn's disease is unclear. In this study, we compared cohorts of black and white children with Crohn's disease to determine the extent race is associated with differences in readmissions, complications, and procedures among hospitalizations in the United States.
METHODS:
Data were extracted from the Pediatric Health Information System (January 1, 2004-June 30, 2012) for patients with 21 years or younger hospitalized with a diagnosis of Crohn's disease. White and black cohorts were randomly selected in a 2:1 ratio by hospital. The primary outcome was time from index hospital discharge to readmission. The most frequent complications and procedures were evaluated by race.
RESULTS:
There were 4377 patients. Black children had a
shorter time to first readmission and
higher probability of readmission (P = 0.009) and a
16% increase in risk of readmission
- compared with white children (P = 0.01). Black children had
longer length of stay and
higher frequency of overall and
late (30-d to 12-mo postdischarge) readmissions (P < 0.001).
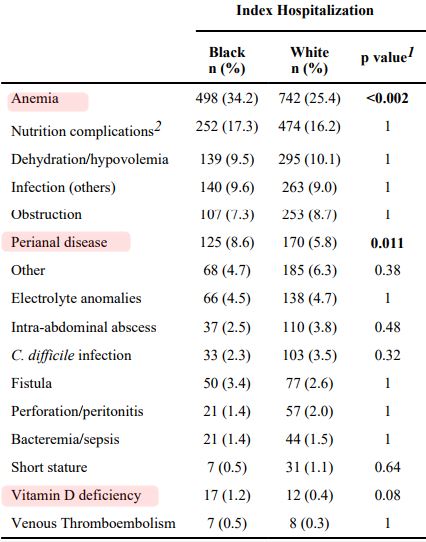
During index hospitalization, more black children had perianal disease and anemia (P < 0.001).
- During any hospitalization, black children had
higher incidence of perianal disease,
anemia, and
vitamin D deficiency, [2.3% vs .9%] and
greater number of perianal procedures,
endoscopies, and
blood product transfusion (P < 0.001).
CONCLUSIONS:
There are differences in hospital readmissions, complications, and procedures among hospitalized children related to race. It is unclear whether these differences are due to genetic differences, worse intrinsic disease, adherence, access to treatment, or treatment disparities.
Comment in
African Americans May Access the Emergency Department for Inflammatory Bowel Disease Care More Often than Whites.

