Vitamin D reduces inflammation in critically ill patients
The effect of vitamin D supplementation on inflammation in critically ill patients: A systematic review
PharmaNutrition. Volume 13, https://doi.org/10.1016/j.phanu.2020.100196
Seyed MostafaArabiaLeila SadatBahramiaGolnazRanjbarbHamedTabeshcAbdolrezaNorouzyb
📄 Download the PDF from sci-hub via VitaminDWiki
Purpose
Vitamin D intervention may affect the immune system function and modulate the innate and adaptive responses in relation to the status of patients with critical illness.
Methods
The search terms were conducted on PubMed, Cochrane Library, EMBASE, Scopus, clinical trials and gray literature databases and clinical trial studies published from 2000 to July 2019 were included in the present study. Two independent researchers selected 53 studies that examined vitamin D supplementation in critically ill patients. Three researchers assessed study designs, subjects, interventions, outcomes, and data quality according to the Cochrane scoring system.
Results
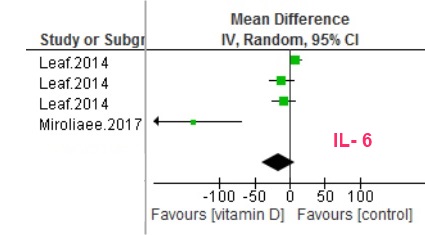
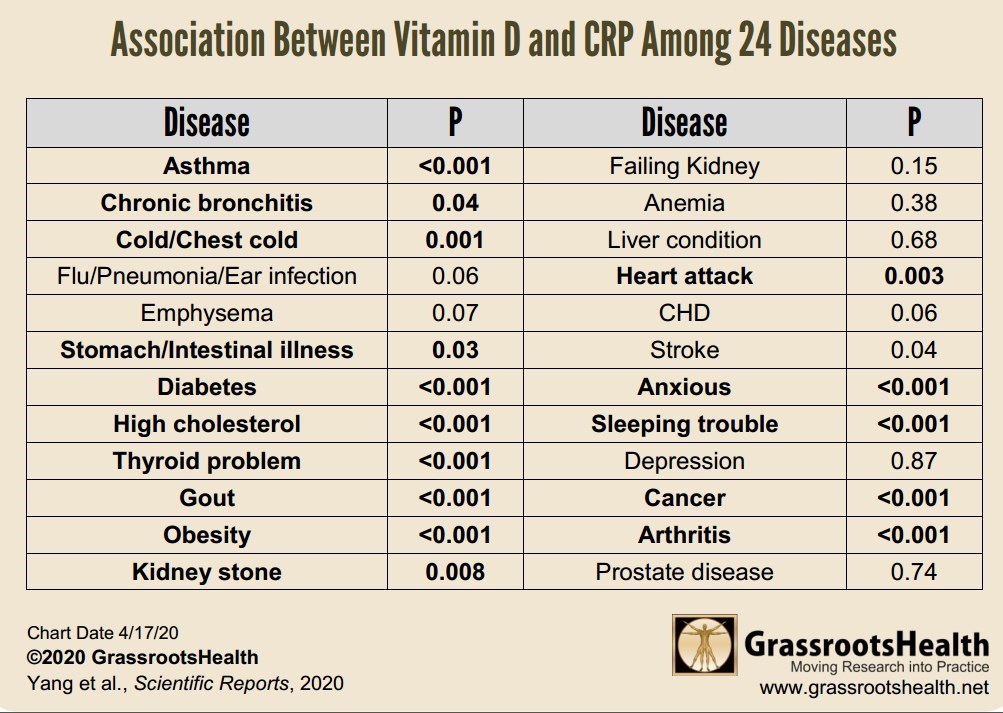
Three randomized clinical trials of critically ill patients treated with high dose of vitamin D supplements indicated consistent reductions in pro-inflammatory cytokines (interleukins 1 and 6). Five clinical trials illustrated no significant differences in C-reactive protein levels between vitamin D and placebo groups. Outcomes of secondary analyses in two trials showed no significant reduction in interleukin 6 levels (pooled effect size, IL-6, −16.32 [−40.78, 8.15]) while treated with high dose of vitamin D supplements. Moreover, vitamin D supplementation indicated no considerable effects on CRP levels in recipient group versus non-recipient group (pooled effect size −2.65 [−18.02, 12.72]).
Conclusions
Evidence from few clinical studies suggests that high doses of vitamin D interventions may reduce pro-inflammatory cytokines, whereas it appears to have no significant effects on anti-inflammatory cytokines and C-reactive protein levels. Further well-designed research studies are required to elucidate the effect of vitamin D supplementation on immune responses in critically ill patients.
