Getting vitamin D during pregnancy is even more important than avoiding alcohol
|| |Alcohol| Low Vitamin D (< 40 ng)
Stillbirth|0.9%
(>4drinks/week) |yes
Miscarriage|4 X increase |yes
Preterm birth|yes |2 X increase
Low birth weight|yes |yes
C- sections|no|4 X increase
Preeclampsia|1.1X increase
see PDF at bottom|4 X increase
Vaginosis|no|5 X increase
Small for Gestational Age|?|6.5 X increase
Childhood Asthma|no?|[tiki-download_file.php?fileId=1541]
Childhood Behaviour|Yes|ADHD
Autism
Childhood Health|?|Allergies
Infections
Childhood Cognition| Lower IQ|2X more language problems
Problem worse in|1st trimester|3rd trimester||


See also VitaminDWiki
Pregnancy category listing has items along with related searches
Alcohol while pregnant lowers the vitamin D levels in Winter and Spring – Jan 2017
Prenatal VITAMIN D is more important than other prenatal vitamins
Alcoholic liver disease 8X more likely among alcoholics if very low vitamin D – May 2015
Healthy pregnancies need lots of vitamin D has the following summary
{include}
See web
- Far More U.S. Children Than Previously Thought May Have Fetal Alcohol Disorders NYT Feb 2018
- ". . estimated conservatively that fetal alcohol spectrum disorders affect 1.1 to 5 percent of children in the country, up to five times previous estimates"
- Evaluated 2,962 children, 222 had FASD, but only 2 had been previously diagnosed, .
- 2015 - American Academy of Pediatrics - ZERO alcohol during pregnancy
- 2016 - CDC ZERO alcohol without birth control (since 1/2 of pregnancies are unplanned)
- : original JAMA article reported on by NYT doi:10.1001/jama.2017.21896
Drinking alcohol during pregnancy BabyCenter
Alcohol and Pregnancy: Is 'A Little Bit' Safe? Web MD
- A recent CDC study found that about one in eight pregnant women in the U.S. report drinking at least one alcoholic beverage in the past month.
- Although heavy drinking can obviously be harmful, the risks of light and moderate drinking aren’t as clear.
- 2010 U.K. reported that the 5-year-old children of women who drank up to one to two alcoholic drinks per week or per occasion while pregnant were not at an increased risk of behavioral or cognitive problem
- Alcohol-and-Pregnancy|Alcohol and Pregnancy Midwife.org
- about 1,3% of pregnant women in the United States reports binge drinking in the past 30 days (having four or more drinks at one time)
- The effects of low to moderate alcohol consumption and binge drinking in early pregnancy on behaviour in 5-year-old children Aug 2013
- no statistically significant associations were observed between maternal low to moderate average weekly alcohol consumption and SDQ behavioural scores OR 1.1,
- or between binge drinking and SDQ behavioural scores OR 1.2, Full free PDF is online
- Fetal Alcohol Spectrum Disorders (FASDs) CDC
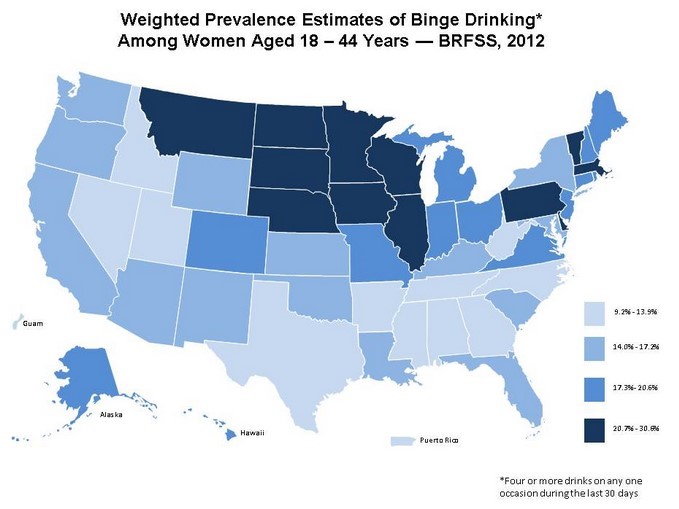
- CDC map of women with binge drinking (all women, not just pregnant)
No Alcohol for Sexually Active Women Without Birth Control, C.D.C. Recommends NYT Feb 2016
Wikipeida on Fetal Alcohol Syndrome
As of 1987, fetal alcohol exposure was the leading known cause of intellectual disability in the Western world. In the United States and Europe, the FAS prevalence rate is estimated to be between 0.2–2 in every 1000 live births. FAS should not be confused with Fetal Alcohol Spectrum Disorders (FASD), a condition which describes a continuum of permanent birth defects caused by maternal consumption of alcohol during pregnancy, which includes FAS, as well as other disorders, and which affects about 1% of live births in the US (i.e., about 10 cases per 1000 live births).

FAS term coined in 1974 Lancet article
Stillbirth rate = 0.9% if > 4 drinks per week
The authors evaluated the association between alcohol intake during pregnancy and risk of stillbirth and infant death in a cohort of pregnant women receiving routine antenatal care at Aarhus University Hospital (Aarhus, Denmark) between 1989 and 1996. Prospective information on alcohol intake, other lifestyle factors, maternal characteristics, and obstetric risk factors was obtained from self-administered questionnaires and hospital files, and 24,768 singleton pregnancies were included in the analyses (116 stillbirths, 119 infant deaths). The risk ratio for stillbirth among women who consumed ≥5 drinks/week during pregnancy was 2.96 (95% confidence interval: 1.37, 6.41) as compared with women who consumed <1 drink/week. Adjustment for smoking habits, caffeine intake, age, prepregnancy body mass index, marital status, occupational status, education, parity, and sex of the child did not change the conclusions, nor did restriction of the highest intake group to women who consumed 5–14 drinks/week ( risk ratio = 3.13, 95% confidence interval: 1.45, 6.77). The rate of stillbirth due to fetoplacental dysfunction increased across alcohol categories, from 1.37 per 1,000 births for women consuming <1 drink/week to 8.83 per 1,000 births for women consuming ≥5 drinks/week . The increased risk could not be attributed to the effect of alcohol on the risk of low birth weight, preterm delivery, or malformations. There was little if any association between alcohol intake and infant death.
