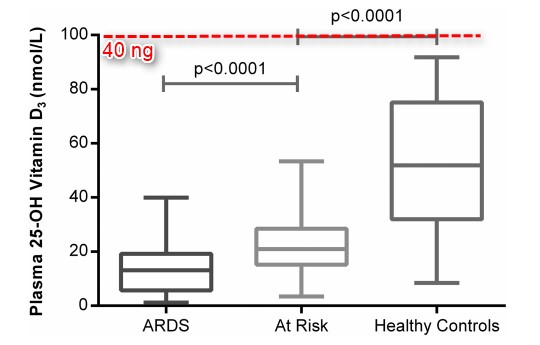
Acute respiratory distress – 100 percent of patients were vitamin D deficient
Vitamin D deficiency contributes directly to the acute respiratory distress syndrome (ARDS)
Thorax doi:10.1136/thoraxjnl-2014-206680
Rachel C A Dancer 1, Dhruv Parekh 1, Sian Lax1, Vijay D'Souza1, Shengxing Zheng1, Chris R Bassford1, Daniel Park1, D G Bartis1, Rahul Mahida1, Alice M Turner1, Elizabeth Sapey1, Wenbin Wei2, Babu Naidu1, Paul M Stewart3, William M Fraser4, Kenneth B Christopher5, Mark S Cooper6, Fang Gao1, David M Sansom7, Adrian R Martineau 8, Gavin D Perkins9, David R Thickett1
1Centre for Translational Inflammation and Fibrosis Research, School of Clinical and Experimental Medicine, University of Birmingham, Birmingham, UK
2School of Cancer Sciences, University of Birmingham, Birmingham, UK
3Centre for Endocrinology, Diabetes and Metabolism, School of Clinical and Experimental Medicine, University of Birmingham, Birmingham, UK
4Norwich Medical School, University of East Anglia, Norwich, UK
5Renal Division, Brigham and Women's Hospital, Harvard Medical School, Boston, Massachusetts, USA
6Department of Medicine, Concord Medical School, University of Sydney, Sydney, New South Wales, Australia
7Institute of Immunity and Transplantation, University College London, London, UK
8Blizard Institute, Queen Mary University of London, London, UK
9Warwick Clinical Trials Unit, Warwick Medical School, University of Warwick, Coventry, UK
Correspondence to: Professor David Thickett, Centre for Translational Inflammation and Fibrosis Research, Queen Elizabeth Hospital, University of Birmingham, Birmingham B15 2TH, UK; d.thickett@bham.ac.uk
Received 10 December 2014, Revised 10 March 2015, Accepted 2 April 2015, Published Online First 22 April 2015
Rationale Vitamin D deficiency has been implicated as a pathogenic factor in sepsis and intensive therapy unit mortality but has not been assessed as a risk factor for acute respiratory distress syndrome (ARDS). Causality of these associations has never been demonstrated.
Objectives To determine if ARDS is associated with vitamin D deficiency in a clinical setting and to determine if vitamin D deficiency in experimental models of ARDS influences its severity.
Methods Human, murine and in vitro primary alveolar epithelial cell work were included in this study.
Findings Vitamin D deficiency (plasma 25(OH)D levels <50 nmol/L) was ubiquitous in patients with ARDS and present in the vast majority of patients at risk of developing ARDS following oesophagectomy. In a murine model of intratracheal lipopolysaccharide challenge, dietary-induced vitamin D deficiency resulted in exaggerated alveolar inflammation, epithelial damage and hypoxia. In vitro, vitamin D has trophic effects on primary human alveolar epithelial cells affecting >600 genes. In a clinical setting, pharmacological repletion of vitamin D prior to oesophagectomy reduced the observed changes of in vivo measurements of alveolar capillary damage seen in deficient patients.
Conclusions Vitamin D deficiency is common in people who develop ARDS. This deficiency of vitamin D appears to contribute to the development of the condition, and approaches to correct vitamin D deficiency in patients at risk of ARDS should be developed.
Trial registration UKCRN ID 11994.
📄 Download the PDF from VitaminDWiki
MedPageToday article of the study
- All of the 55 patients in the study with ARDS were vitamin D deficient (defined as <50 nmol/L)
ARDS Wikipedia
“Acute respiratory distress syndrome (ARDS), previously known as respiratory distress syndrome (RDS), acute lung injury, adult respiratory distress syndrome, or shock lung, is a severe, life-threatening medical condition characterized by widespread inflammation in the lungs.”
“The syndrome has a high mortality between 20 and 50%.”
“The signs and symptoms of ARDS usually begins within 72 hours of the initial insult or injury to the lung”
‘The annual incidence of ARDS is 13-23 people per 100,000 in the general population.”
Vitamin D was NOT mentioned
Acute Respiratory Distress Syndrome (ARDS) American Lung Association
- “ARDS usually develops in people who are already very ill with another disease or who have major injuries. They are usually already in the hospital when they develop the ARDS.”
See also VitaminDWiki
Breathing category listing has items along with related searches
Trauma and surgery category listing has items along with related searches
Vitamin D as a modifiable risk factor in critical illness - English and Portuguese March 2014
Critically ill need vitamin D – how much and which test to use is TBD – Nov 2014
Hospital or ICU death about twice as likely if low vitamin D – March 2014
See also web
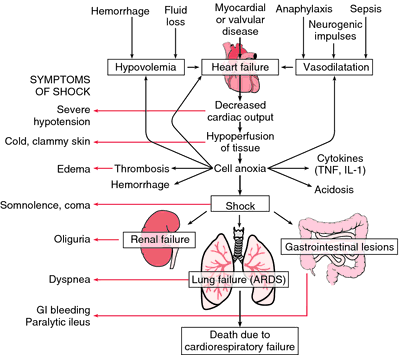
- Septic Shock - Medical dictionary has the following chart
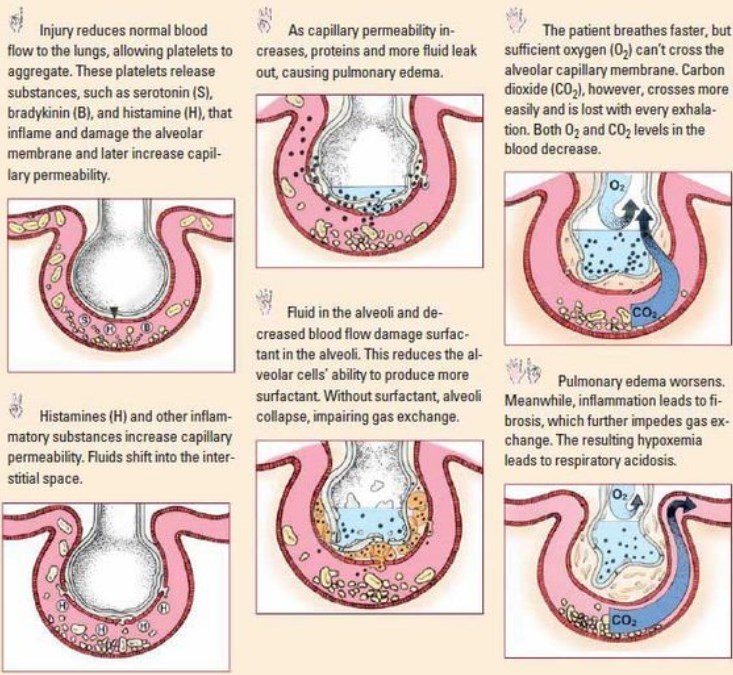
- ARDS Infographic 2018