50,000 IU of vitamin D weekly following cardiac failure helps – RCT 2014
The Effect of Vitamin D on Aldosterone and Health Status in Patients With Heart Failure
Journal of Cardiac Failure DOI: https://doi.org/10.1016/j.cardfail.2014.01.019
Rebecca S. Boxer, MD, MS MD, MS Rebecca S. MD, MS Rebecca S. Boxer, Brian D. Hoit, MD, Brian J. Schmotzer, MS, Gregory T. Stefano, MD, Amanda Gomes, MSc, MD, Lavinia Negrea, MD
📄 Download the PDF from VitaminDWiki
Background: Vitamin D deficiency is associated with heart failure (HF) events, and in animal models vitamin D down-regulates renin-angiotensin-aldosterone system hormones.
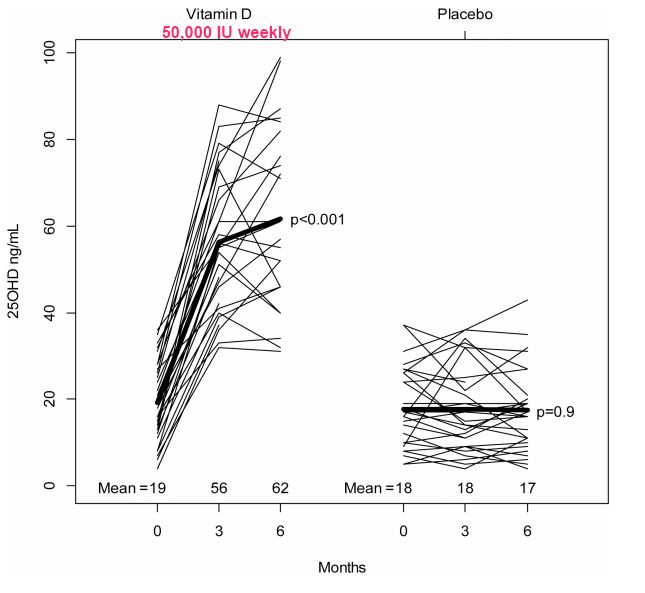
Methods: Patients with New York Heart Association (NYHA) functional class II–IV HF and a 25OH-D level ≤37.5 ng/mL received 50,000 IU vitamin D3 weekly (n = 31) or placebo (n = 33) for 6 months. Serum aldosterone, renin, echocardiography, and health status were determined at baseline and 6 months.
Results
Mean age of participants was 65.9 ± 10.4 years, 48% were women, 64% were African American, mean ejection fraction was 37.6 ± 13.9%, 36% were in NYHA functional class III, and 64% were in class II. The vitamin D group increased serum 25OH-D (19.1 ± 9.3 to 61.7 ± 20.3 ng/mL) and the placebo group did not (17.8 ± 9.0 to 17.4 ± 9.8 ng/mL).
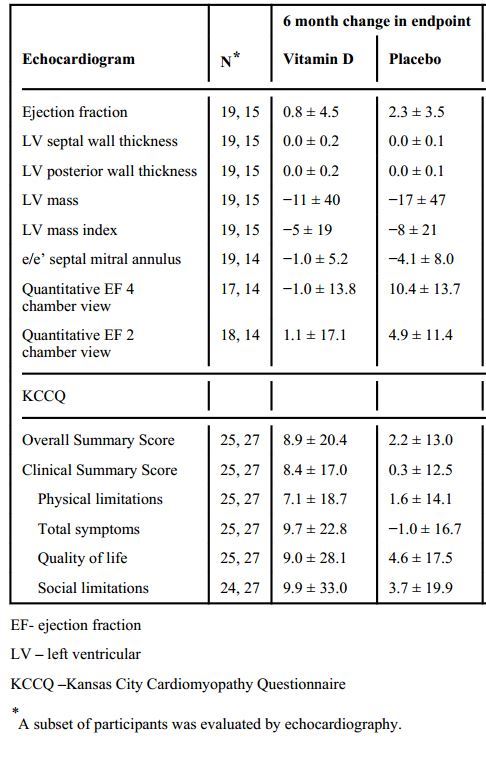
Aldosterone decreased in the vitamin D group (10.0 ± 11.9 to 6.2 ± 11.6 ng/dL) and not in the placebo group (8.9 ± 8.6 to 9.0 ± 12.4 ng/dL; P = .02). There was no difference between groups in renin, echocardiographic measures, or health status from baseline to 6 months. Modeling indicated that variables which predicted change in aldosterone included receiving vitamin D, increasing age, African American race, and lower glomerular filtration rate.
Conclusions
Vitamin D3 repletion decreases aldosterone in patients with HF and low serum vitamin D. Vitamin D may be an important adjunct to standard HF therapy. Further study will assess if vitamin D provides long-term benefit for patients with HF.
