Rheumatoid Arthritis associated with lower vitamin D and higher latitude – meta-analysis
Serum Vitamin D Level and Rheumatoid Arthritis Disease Activity: Review and Meta-Analysis.
PLoS One. 2016 Jan 11;11(1):e0146351. doi: 10.1371/journal.pone.0146351. eCollection 2016.
Lin J1, Liu J1, Davies ML2, Chen W1.
1 Department of Rheumatology, the First Affiliated Hospital, College of Medicine, Zhejiang University, Hangzhou, Zhejiang Province, China.
2 Clinical Immunology Laboratory, Department of Microbiology and Immunology, Rosalind Franklin University of Medicine and Science, North Chicago, Illinois, United States of America.
BACKGROUND:
The evidence from epidemiological studies concerning the relationship between serum vitamin D concentrations and rheumatoid arthritis (RA) is inconsistent. This meta-analysis is aimed at determining the magnitude of the correlation between this common autoimmune disease and vitamin D, an important nutrient known to dampen adaptive immune responses.
METHODS:
Through multiple search strategies, relevant literature was identified and evaluated for quality before May 16 2015. Data extracted from eligible studies was synthesized to calculate pooled correlation coefficient (r), mean difference (MD) and odds ratio (OR). The Venice criteria were applied to assess the credibility of the evidence for each statistically significant association.
RESULTS:
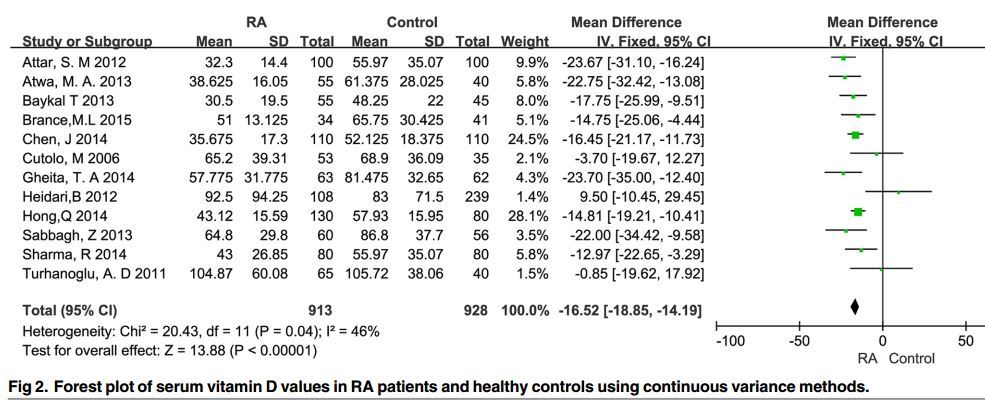
A total of 24 reports involving 3489 patients were selected for analysis. RA patients had lower vitamin D levels than healthy controls (MD:-16.52 nmol/L, 95% confidence intervals [CI]:-18.85 to -14.19 nmol/L). There existed a negative relationship between serum 25-hydroxyvitamin D (25OHD) level and disease activity index , e.g. 25OHD vs. Disease Activity Score in 28 joints (DAS28): r = -0.13, 95% CI -0.16 to -0.09; 25OHD vs. C-reactive protein: r = -0.12, 95% CI -0.23 to -0.00. Additionally, latitude-stratified subgroup analysis yielded a relatively stronger negative correlation between 25OHD and DAS28 in low-latitude areas. This inverse relationship also appeared more significant in developing countries than in developed countries. No publication bias was detected.
CONCLUSION:
RA patients had lower vitamin D values than healthy controls. There was a negative association between serum vitamin D and RA disease activity. However, more strictly controlled studies are needed to validate these findings.
One of many Forest Plots in the PDF
PMID: 26751969
