Hospital or ICU death about twice as likely if low vitamin D
Vitamin D status and its association with season, hospital and sepsis mortality in critical illness.
Crit Care. 2014 Mar 24;18(2):R47
Amrein K, Zajic P, Schnedl C, Waltensdorfer A, Fruhwald S, Holl A, Urbanic Purkart T, Wünsch G, Valentin T, Grisold A, Stojakovic T, Amrein S, Pieber TR, Dobnig H.
INTRODUCTION:
Vitamin D plays a key role in immune function. Deficiency may aggravate the incidence and outcome of infectious complications in critically ill patients. We aimed to evaluate the prevalence of vitamin D deficiency and the correlation between serum 25-hydroxyvitamin D (25(OH) D) and hospital mortality, sepsis mortality and blood culture positivity.
METHODS:
In a single-center retrospective observational study at a tertiary care center in Graz, Austria, 655 surgical and non-surgical critically ill patients with available 25(OH) D levels hospitalized between September 2008 and May 2010 were included. Cox regression analysis adjusted for age, gender, severity of illness, renal function and inflammatory status was performed. Vitamin D levels were categorized by month-specific tertiles (high, intermediate, low) to reflect seasonal variation of serum 25(OH) D levels.
RESULTS:
Overall, the majority of patients were vitamin D deficient (< 20 ng/ml; 60.2%) or insufficient (>=20 and < 30 ng/dl; 26.3%), with normal 25(OH) D levels (>30 ng/ml) present in only 13.6%. The prevalence of vitamin D deficiency and mean 25(OH) D levels was significantly different in winter compared to summer months (P < 0.001). Hospital mortality was 20.6% (135 of 655 patients).
Adjusted hospital mortality was significantly higher in patients in the
low (hazard ratio (HR) 2.05, 95% confidence interval (CI) 1.31-3.22) and
intermediate (HR 1.92, 95% CI 1.21-3.06) compared to the high tertile.
Sepsis was identified as cause of death in 20 of 135 deceased patients (14.8%). There was no significant association between 25(OH) D and C-reactive protein (CRP), leukocyte count or procalcitonin levels. In a subgroup analysis (n = 244), blood culture positivity rates did not differ between tertiles (23.1% versus 28.2% versus 17.1%, P = 0.361).
CONCLUSIONS:
Low 25(OH) D status is significantly associated with mortality in the critically ill. Intervention studies are needed to investigate the effect of vitamin D substitution on mortality and sepsis rates in this population.
Seasonal variation in Vitamin D levels

VitaminDWiki comment: Looks like 30% of Austrians who went to hospital Nov-March previously took suncations or Vitamin D supplements
Hospital survival
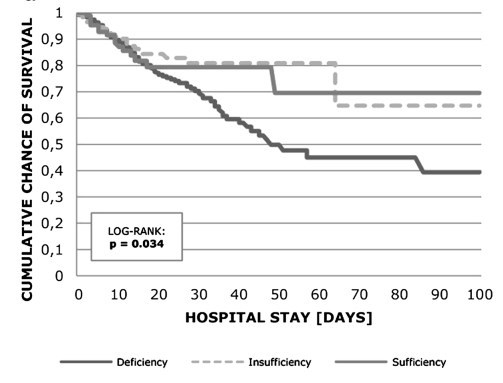
ICU survival

PDF is attached at the bottom of this page
See also VitaminDWiki
More sepsis deaths in those entering hospital with low vitamin D – Jan 2014
6 percent less likely to die by taking just a little vitamin D for 3 plus years – RCT Dec 2013
Chance of dying within 1 month of entering hospital is 45 percent higher if low vitamin D – July 2013 death after leaving ICUl is ofte ignored
1 month after plasma exchange vitamin D levels reduced by 40 percent – Oct 2013
With just 200 IU vitamin D in intravenous feeds, deficiency results
ICU survival increased with vitamin D single 540K IU loading dose - JAMA Sept 2014
- Same hospital? - but with intervention - has the following chart

