Birth problems associated with low Zinc
Stillbirth associated with low Zinc - Feb 2018
A multilateral investigation of the effects of zinc level on pregnancy
J Clin Lab Anal. 2018 Feb 2. doi: 10.1002/jcla.22398. [Epub ahead of print]
Özgan Çelikel Ö1, Doğan Ö2, Aksoy N3.
1 Gynecology and Obstetrics Clinic, Yenimahalle Training and Research Hospital, Yildirim Beyazıt University, Ankara, Turkey.
2 Department of Biochemistry, Ankara University Faculty of Medicine, Ankara, Turkey.
3 Department of Biochemistry, Yenimahalle Training and Research Hospital, Yildirim Beyazıt University, Ankara, Turkey.
BACKROUND:
The relationship between maternal zinc level and birth weight, birth week, delivery type, garvida, maternal age, etc., contribute to diagnosis and clinical follow-up.
METHOD:
Multivariate investigated for data of 275 patients were obtained during their pregnancy periods until birth. 3 cc blood samples were centrifuged for 15 minutes at 2500 g within a period of 30 minutes and were stored at -80°C until the time of analysis. The zinc levels of the patients were found to be within the range of 49-129 μg/dL. Patients were divided into 8 groups according to their zinc levels (49-59, 60-69, …, 120-129) and the relationships of zinc level with the parameters related to the mode of delivery, week of delivery, birth weight, age, early membrane rupture, live-stillbirth, and gravid were statistically analyzed to determine differences between the groups.
RESULTS:
There was a significant difference between the live births and stillbirths with a 95% confidence level regarding the zinc level. The zinc level affected the live-stillbirth status; patients with a zinc level of 49-59 μg/dL had stillbirths, the live birth rate for 59-69 μg/dL was approximately 50%, whereas it was approximately 88% for in the patients with a zinc level of 109-119 μg/dL. All patients with a zinc level of 119 μg/dL and above had live births.
CONCLUSION:
Based on the results of this study, it is suggested that zinc supplementation may be an appropriate treatment for the pregnant women with low zinc levels to provide the realization of live births.
PMID: 29392763 DOI: 10.1002/jcla.22398
Preterm birth 4.9 X more likely if low Zinc in first trimester Chinese pregnancies - March 2016
Maternal Serum Zinc Concentration during Pregnancy Is Inversely Associated with Risk of Preterm Birth in a Chinese Population
J Nutr. 2016 Mar;146(3):509-15. doi: 10.3945/jn.115.220632. Epub 2016 Jan 27.
Wang H1, Hu YF2, Hao JH1, Chen YH1, Wang Y2, Zhu P1, Zhang C1, Xu YY1, Tao FB3, Xu DX3.
📄 Download the PDF from VitaminDWiki
BACKGROUND: Evidence exists that maternal zinc status during pregnancy is linked to adverse pregnancy outcomes including abortion, fetal growth restriction, and neural tube defects. However, it remains unclear whether maternal serum zinc concentration (SZC) during pregnancy is associated with risk of preterm birth.
OBJECTIVE: This study was designed to investigate the association between maternal SZC during pregnancy and risk of preterm birth.
METHODS:
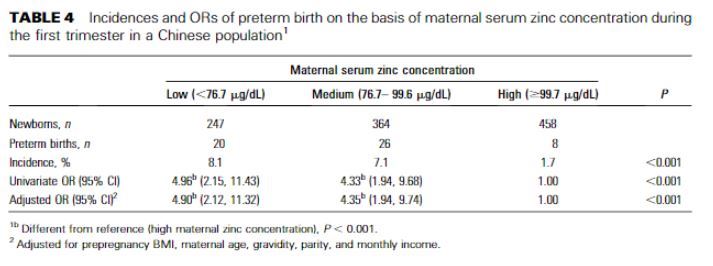
For this substudy of the China-Anhui Birth Cohort Study, 3081 maternal-singleton pairs with detailed birth records and available serum samples were identified. The maternal SZC was determined with flame atomic absorption spectroscopy. A total of 169 preterm births were identified. In this study, the women were divided into tertiles on the basis of their SZC: low (<76.7 μg/dL), medium (76.7-99.6 μg/dL), and high (≥99.7 μg/dL). The ORs for preterm birth were estimated by using multiple logistic regression models.
RESULTS:
The median SZC was 87.3 μg/dL (range: 11.1-211 μg/dL). Incidences of preterm birth were 7.3% and 6.0% among subjects with low and medium SZCs, respectively, which were significantly higher than 3.1% among subjects with a high SZC [ORs (95% CIs) for low and medium SZCs: 2.45 (1.60, 3.74), P < 0.001, and 2.00 (1.29, 3.09), P < 0.01, respectively]. After adjustment for prepregnancy body mass index, maternal age, time of serum collection, gravidity, parity, and monthly income, adjusted ORs were 2.41 (95% CI: 1.57, 3.70; P < 0.001) and 1.97 (95% CI: 1.27, 3.05; P < 0.01) among subjects with low and medium maternal SZCs.
CONCLUSIONS: Maternal serum zinc concentration during pregnancy is inversely associated with risk of preterm birth in the Chinese population, and the results are driven by maternal SZC in the first trimester.
PMID: 26817714 DOI: 10.3945/jn.115.220632
