Very short sleep associated with low Vitamin D
Serum nutritional biomarkers and their associations with sleep among US adults in recent national surveys.
PLoS One. 2014 Aug 19;9(8):e103490. doi: 10.1371/journal.pone.0103490. eCollection 2014.
Beydoun MA1, Gamaldo AA1, Canas JA2, Beydoun HA3, Shah MT4, McNeely JM4, Zonderman AB1.
1 National Institute on Aging, NIA/NIH/IRP, Baltimore, Maryland, United States of America.
2 Pediatric Endocrinology, Diabetes and Metabolism Nemours Children's Clinic, Jacksonville, Florida,
3 Graduate program in Public Health, Eastern Virginia Medical School, Norfolk, Virginia,
4 National Institute on Aging, NIA/NIH/IRP, Baltimore, Maryland; Department of Psychology, University of Maryland, Baltimore, Maryland,
📄 Download the PDF from VitaminDWiki
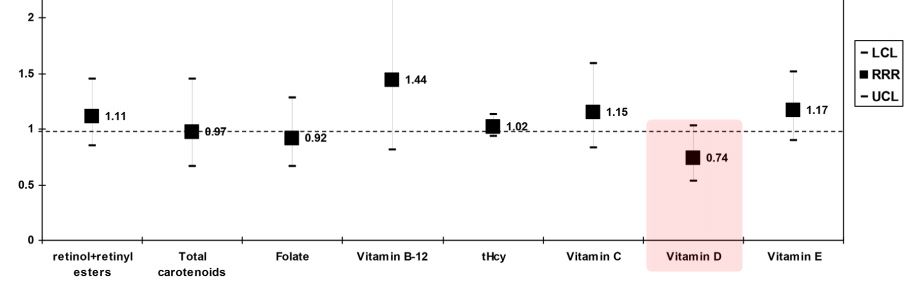
Risk of very short sleep
Risk of Insomia
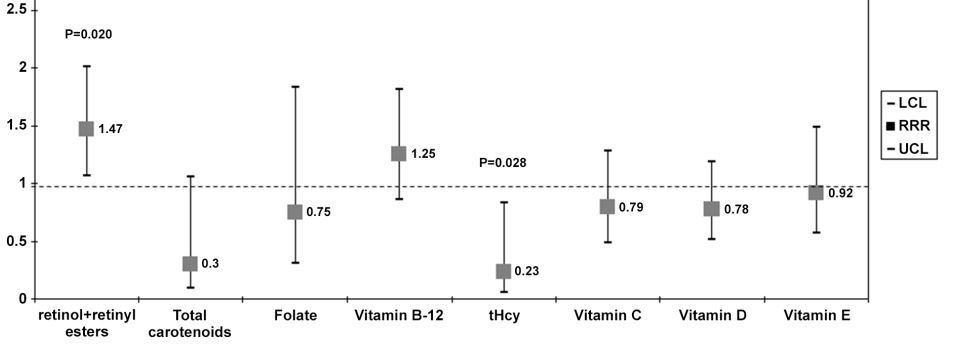
BACKGROUND: The associations between nutritional biomarkers and measures of sleep quantity and quality remain unclear.
METHODS:
Cross-sectional data from the National Health and Nutrition Examination Surveys (NHANES) 2005-2006 were used. We selected 2,459 adults aged 20-85, with complete data on key variables. Five sleep measures were constructed as primary outcomes:
(A) Sleep duration;
(B) Sleep disorder;
(C) Three factors obtained from factor analysis of 15 items and labeled as
"Poor sleep-related daytime dysfunction" (Factor 1),
"Sleepiness" (Factor 2) and
"Sleep disturbance" (Factor 3).
Main exposures were serum concentrations of key nutrients, namely
retinol,
retinyl esters,
carotenoids (α-carotene, β-carotene, β-cryptoxanthin, lutein+zeaxanthin, lycopene),
folate,
vitamin B-12,
total homocysteine (tHcy),
vitamin C,
25-hydroxyvitamin D (25(OH)D) and
vitamin E.
Main analyses consisted of multiple linear, logistic and multinomial logit models.
RESULTS: Among key findings, independent inverse associations were found between
serum vitamin B-12 and sleep duration,
25(OH)D and sleepiness (as well as insomnia), and between
folate and sleep disturbance.
Serum total carotenoids concentration was linked to higher odds of short sleep duration (i.e. 5-6 h per night) compared to normal sleep duration (7-8 h per night).
CONCLUSIONS: A few of the selected serum nutritional biomarkers were associated with sleep quantity and quality. Longitudinal studies are needed to ascertain temporality and assess putative causal relationships.
Clipped from PDF
There may be a narrow range of 25(OH) vitamin D3 blood levels that are necessary to produce normal sleep and clinical trials are needed to determine the effects of Vitamin D3 replacement in the prevention of sleep disorders such as insomnia, obstructive sleep apnea and rapid eye movement related apnea [89 – Gominak SC, Stumpf WE (2012) The world epidemic of sleep disorders is linked to vitamin D deficiency. Med Hypotheses 79: 132–135.]
The link between vitamin D metabolism and sleep medicine - 2014
Sleep Med Rev. 2014 Aug;18(4):311-9. doi: 10.1016/j.smrv.2013.07.001. Epub 2013 Sep 26.
McCarty DE1, Chesson AL Jr2, Jain SK3, Marino AA2.
Vitamin D is a hormone that interacts with intranuclear receptors to effect transcriptional changes in many cell types including those in gut, bone, breast, prostate, brain, skeletal muscle, and the immune system. Inadequacy of vitamin D is widely prevalent, and leads to the classic diseases of bone demineralization as well as to more recently recognized problems such as nonspecific pain and noninflammatory skeletal myopathy, which may disrupt sleep and directly cause daytime impairment.
Emerging lines of evidence suggest that low vitamin D levels increase the risk for autoimmune disease, chronic rhinitis, tonsillar hypertrophy, cardiovascular disease, and diabetes. These conditions are mediated by altered immunomodulation, increased propensity to infection, and increased levels of inflammatory substances, including those that regulate sleep, such as tumor necrosis factor alpha (TNF-α), interleukin (IL)-1, and prostaglandin D2 (PD2). Together, the recent reports suggest a role for inadequate vitamin D in the development of symptoms of wake impairment commonly associated with sleep disorders. Persistent inadequacy of vitamin D may also increase the risk for obstructive sleep apnea via promotion of adenotonsillar hypertrophy, airway muscle myopathy, and/or chronic rhinitis. Much remains to be learned concerning the complex relationship between chronically low levels of vitamin D, normal sleep, sleep disruption, and daytime neurocognitive impairment.
