Heart Failure 15X more likely if poor VDR, even if good level of vitamin D (China)
Vitamin D levels and vitamin D receptor variants are associated with chronic heart failure in Chinese patients.
Clin Lab Anal. 2019 Feb 4:e22847. doi: 10.1002/jcla.22847.
Hao Y1, Chen Y1.
📄 Download the PDF from VitaminDWiki
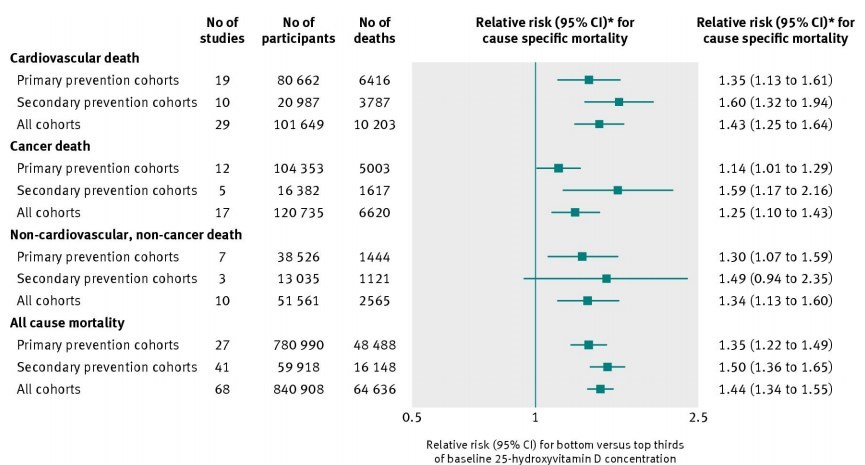
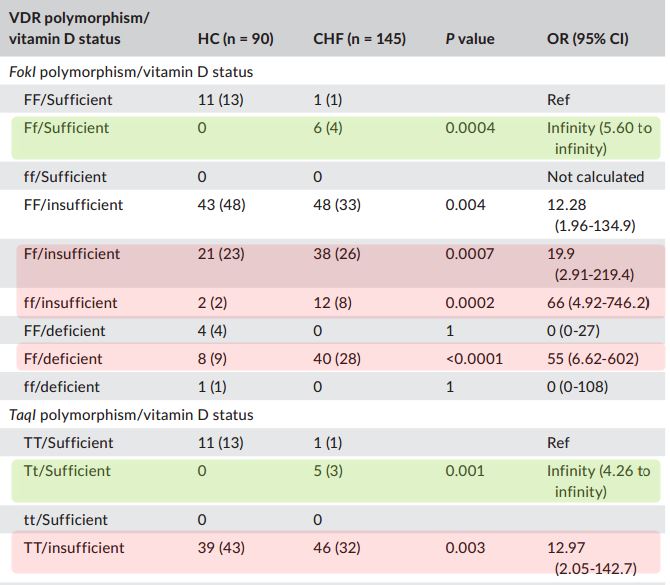
Good level of Vitamin D but Ft or Tt gene mutation: every person had Chronic Heart Failure
BACKGROUND:
Vitamin D is an indispensable molecule for human health. Wide ranges of diseases are linked with vitamin D deficiencies. Role of vitamin D in chronic heart failure has been demonstrated in different populations; however, reports are limited in Chinese population. Vitamin D exerts its effect through vitamin D receptor and variants in vitamin D receptor (VDR) gene are shown to affect vitamin D signaling. In the present study, we hypothesized that both vitamin D levels and VDR variants could be associated with the development of chronic heart failure.
MATERIALS AND METHODS:
We enrolled 145, chronic heart failure patients those admitted to Department of Cardiothoracic Surgery, Beijing Luhe Hospital of Capital Medical University and fulfilled NYHA inclusions criteria. In addition, ninety healthy subjects from similar geographical location were enrolled as healthy controls. Plasma levels of vitamin D were quantified by ELISA. VDR variants (BsmI, ApaI, TaqI, and FokI) were genotyped by PCR-RFLP.
RESULTS:
Plasma levels of vitamin D were significantly lower in chronic heart patients compared to healthy controls. Heterozygous and minor allele for FokI and TaqI polymorphisms were significantly higher in heart failure patients when compared to healthy controls. In addition, combined analysis of vitamin D levels and VDR mutants revealed association of vitamin D deficiencies and VDR mutants with chronic heart failure.
CONCLUSIONS: The results of the present investigation showed an important role of vitamin D and VDR variants with chronic heart failure.
