Interactions of Asthma Vitamin D, Pollution and Obesity
Pollution, Obesity, Vitamin D, or Why Is Asthma So Complicated—and Interesting
J Allergy Clin Immunol Pract DOI: https://doi.org/10.1016/j.jaip.2019.04.015 |
Erick Forno, MD, MPHa, Augusto A. Litonjua, MD, MPHb, MD, MPH Augusto A. Litonjua
Figure 1
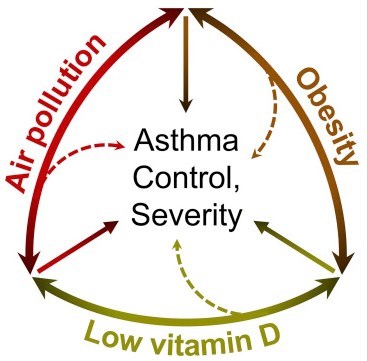
The vicious triad of vitamin D deficiency, air pollution exposure, and obesity.
Each of these exposures has independent adverse effects on asthma control and severity.
Each of these exposures interacts with each other, and the presence of all three has the greatest effect on loss of asthma control and increased severity.
Over 26 million people in the United States have asthma, including 6.1 million children.1 Similarly, overweight/obesity affects 93.3 million adults and 13.7 million children nationwide.2 Both diseases are complex and disproportionately affect racial/ethnic minorities and those of low socioeconomic status for various inter-related reasons. Air pollution contributes to asthma morbidity, and there are data indicating that it may also contribute to obesity. 3 In the United States, non-Hispanic whites experience 17% lower air pollution exposure than their consumption produces, whereas blacks and Hispanics experience approximately 60% excess pollution relative to what is caused by their consumption.4 Vitamin D insufficiency may exacerbate the effects of pollution exposure on severe asthma exacerbations,5 and both African American and obese children are more likely to have low vitamin D levels. The increase in asthma risk among obese children may be more pronounced among those exposed to higher levels of outdoor air pollution such as polycyclic aromatic hydrocarbons,6 and, conversely, low vitamin D in obese children is associated with lower lung function.7 Thus, air pollution, obesity, and low vitamin D may comprise a “vicious triad” that contributes to asthma morbidity, particularly in certain minorities (see Figure 1).
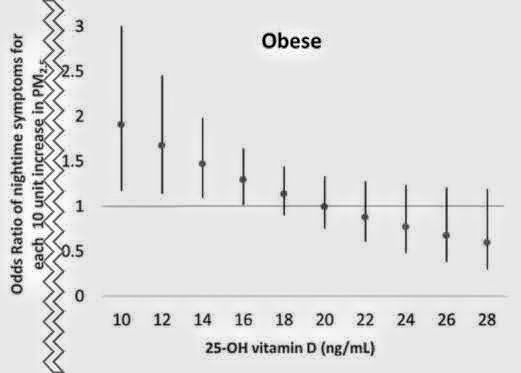
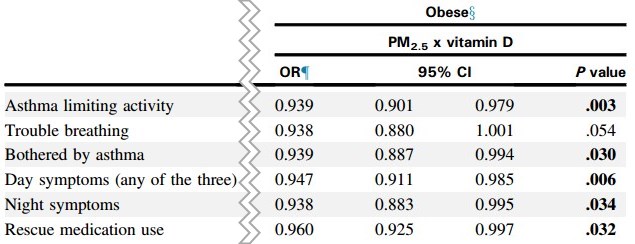
In this issue of JACI In Practice, Bose et al 8 look precisely at those 3 factors (air pollution, obesity, and low vitamin D). In a cohort of 120 predominantly black children with asthma from East Baltimore, they report a 3-way interaction between air pollution, obesity, and vitamin D levels: asthma symptoms were worse among children who were obese, had higher PM2.5 exposure, and had lower vitamin D levels. Those children also had a higher proportion of blood neutrophils, suggesting that the effects may be related to non-Th2 inflammation. Models also showed that in obese children with high PM2.5 exposure, higher vitamin D levels were associated with fewer symptoms, with no such associations seen in children of normal weight. These findings are in line with a prior report from the same group in obese adults with chronic obstructive pulmonary disease,9 suggesting that the associations may not be unique to childhood asthma. Vitamin D has been implicated in several potential mechanisms that might explain these findings. It plays a role in immune modulation and may also play a role against respiratory viral infections. It may have antioxidant effects and potentiate corticosteroid response,10 and its antioxidant effects may be particularly important on exposure to particulate matter.11 Notably, studies on the anti-inflammatory and antioxidant effects of vitamin D levels have suggested that the necessary levels may not be the same as those classically described for bone growth and health.
The current study has substantial strengths, including the prospective collection of longitudinal data, the objective and standardized measurement of indoor particulate air pollution, the repeated measurements of vitamin D serum levels,12 and the consideration of potential confounders. Interestingly, the repeated vitamin D determinations did not seem to alter the overall results. Unlike non-Hispanic whites, it may be that African Americans—and particularly those who live in urban areas and may tend to stay indoors—have a “steadily low” level; this could also partially explain the lack of association between obesity and low vitamin D, which has been described in multiple studies. It is especially important to emphasize that the interactions evaluated by Bose et al8 were based on prior knowledge and biological plausibility. In that context, their analysis constitutes a great example of why it is essential to carefully analyze the data. By grouping participants together without a careful study design and consideration of relevant subgroups, investigators could miss important findings that apply to specific populations. This is key in complex diseases such as asthma, which comprise several dissimilar phenotypes/endotypes. On the other hand, it is imperative to specify those subgroups and consider potential confounders a priori, lest one unintentionally succumb to the temptation of “p-hacking.”13
Some of the limitations of the study include the relatively small sample size and the lack of correction for multiple testing. Moreover, it is imperative to keep in mind that this is an observational study when interpreting the results. What is presented as “protective” is really an inverse association, whereby children with lower vitamin D levels have increased odds of reporting asthma symptoms. Rather than a therapeutic target, low vitamin D could be a biomarker (or a consequence) of PM2.5 exposure, obesity, and/or poor asthma control. This observational study was not designed to evaluate whether normalization of vitamin D levels (eg, via supplementation) could improve or reverse the findings. Studies of vitamin D supplementation for childhood asthma have shown some contradictory results. Antenatal supplementation reduces the risk of wheezing in young children,14, 15 although it is unclear whether the effect may extend onto asthma and to the school years. Data on supplementation for asthma symptoms and exacerbations are somewhat limited and based on small sample sizes.16, 17, 18 A recent individual-level meta-analysis of 7 randomized clinical trials showed overall improvements in exacerbations requiring steroids (incidence rate ratio [IRR] = 0.74, 95% confidence interval = 0.56-0.97).19 Interestingly, subgroup analyses in that meta-analysis showed a significant effect among overweight/obese participants and a trend among participants of African ancestry, although no significant effects were seen among participants ≤16 years of age.
In this setting, studies like the one by Bose et al8 become particularly important, allowing us to identify subgroups that are more likely to benefit from an intervention. Thus, it will be critical to replicate these findings, especially given the complex 3-way interactions described, which altogether apply to a small number of study participants (n ∼ 15, based on 36% being obese, 63% having vitamin D deficiency, and ∼50% above the median PM2.5 exposure). If validated in similar but larger cohorts, the next step might be to tailor interventional studies for this specific group of children. Air pollution, obesity, and low vitamin D may all play important roles in asthma risk and morbidity, but of these 3 factors vitamin D deficiency would certainly be the easiest to remediate.
First 9 References
Centers for Disease Control and Prevention. Asthma Data, Statistics, and Surveillance 2018. Most Recent Asthma Data. (Available from:) http://www.cdc.gov/asthma/mostrecentdata.htm
Centers for Disease Control and Prevention. Childhood Overweight and Obesity. (Available from:) https://www.cdc.gov/obesity/childhood/index.html Date: 2018
An, R., Ji, M., Yan, H., and Guan, C. Impact of ambient air pollution on obesity: a systematic review. Int J Obes (Lond). 2018; 42: 1112–1126
Tessum, C.W., Apte, J.S., Goodkind, A.L., Muller, N.Z., Mullins, K.A., Paolella, D.A. et al. Inequity in consumption of goods and services adds to racial-ethnic disparities in air pollution exposure. Proc Natl Acad Sci U S A. 2019; 116: 6001–6006
Rosser, F., Brehm, J.M., Forno, E., Acosta-Perez, E., Kurland, K., Canino, G. et al. Proximity to a major road, vitamin D insufficiency, and severe asthma exacerbations in Puerto Rican children. Am J Respir Crit Care Med. 2014; 190: 1190–1193
Jung, K.H., Perzanowski, M., Rundle, A., Moors, K., Yan, B., Chillrud, S.N. et al. Polycyclic aromatic hydrocarbon exposure, obesity and childhood asthma in an urban cohort. Environ Res. 2014; 128: 35–41
Lautenbacher, L.A., Jariwala, S.P., Markowitz, M.E., and Rastogi, D. Vitamin D and pulmonary function in obese asthmatic children. Pediatr Pulmonol. 2016; 51: 1276–1283
Bose, S., Diette, G.B., Woo, H., Koehler, K., Romero, K., Rule, A.M. et al. Vitamin D status modifies the response to indoor particulate matter in obese urban children with asthma. J Allergy Clin Immunol Pract . 2019; 7: 1815–1822
📄 Download the Bose PDF from Sci-Hub via VitaminDWiki