Williams-Beuren Syndrome (rare) and too much Vitamin D

PDF is attached at the bottom of this page
Importance of dietary calcium and vitamin D in treatment of hypercalcaemia in Williams-Beuren syndrome
Anke L. Lameris1, Christel L.M. Geesing2, Joost G.J. Hoenderop1, Michiel F. Schreuder3
Radboud University Nijmegen Medical Centre, Departments of 1 Physiology and 3 Pediatric Nephrology, Nijmegen, The Netherlands Bernhoven Hospital, 2 Department of Pediatrics, Oss, The Netherlands
JPediatrEndocrinol Metab. (provisionally accepted), 2013
Chapter 7
Abstract
Williams-Beuren syndrome is a rare genetic disorder, caused by the deletion of 26-28 genes on chromosome 7. Fifteen percent of Williams-Beuren syndrome patients present with hypercalcaemia during infancy, which is generally mild and resolves spontaneously before the age of 4 years. The mechanisms underlying the transient hypercalcaemia in Williams-Beuren syndrome are poorly understood.
We report a case of severe symptomatic hypercalcaemia in a patient with Williams-Beuren syndrome, in which treatment with mild calcium restriction, hyperhydration and repeated bisphosphonate administration only resulted in short-lasting effects. Long-term lowering of serum calcium was only achieved after reducing calcium and vitamin D intake to the bare minimum.
This case illustrates the potential severity of hypercalcaemia in WBS, and demonstrates that both the cause as well as the solution of this problem may be found in the intestinal absorption of calcium. We hypothesize that the phenotypical resemblance between Williams-Beuren syndrome and transient idiopathic infantile hypercalcaemia can be explained by similarities in the underlying genetic defect. Patients suffering from transient infantile hypercalcaemia were recently described to have mutations in CYP24A1, the key enzyme in 1,25-dihydroxyvitamin D3 degradation. In the light of this new development we discuss the role of one of the deleted genes in WBS, Williams Syndrome Transcription Factor, in the etiology of hypercalcaemia in Williams-Beuren syndrome.
Hypercalcaemia in WBS
Introduction
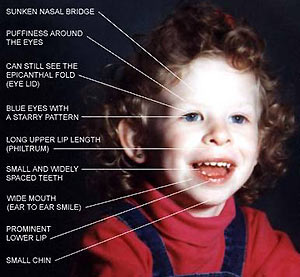
Williams-Beuren syndrome (WBS, OMIM 194050) is a rare genetic disorder, caused by a hemizygous deletion at 7qn.23 comprising approximately 26 to 28 genes [1]. WBS patients are generally characterized by distinctive facial dysmorphisms, mental retardation and cardiovascular abnormalities. In addition, approximately 15% of WBS patients present with hypercalcaemia during infancy, generally mild in nature. It resolves spontaneously before the age of 4 years, but sometimes reoccurs briefly during puberty [1]. The mechanisms explaining the transient hypercalcaemia are poorly understood. We report a case of severe symptomatic hypercalcaemia in a patient with WBS only resolving with a profound reduction of calcium and vitamin D intake, and present a potential mechanism for this metabolic abnormality.
Case report
An 18-months-old female patient was admitted to a local hospital to start tube feeding for treatment of failure to thrive due to feeding difficulties and persistent vomiting despite proton-pump inhibition. Three months earlier she was diagnosed with WBS with normal serum calcium levels (2.40 mmol/L), and was known with low birth weight, a cardiac murmur without a structural anomaly, and a developmental delay.
During her admission, her condition deteriorated, and she developed a hypercalcaemia (Table 1) and hypertension (up to 150/130 mmHg) for which she was transferred to the pediatric intensive care unit at the Radboud University Nijmegen Medical Centre. Her blood pressure was controlled with an intravenous calcium-antagonist, which was successfully switched to oral anti-hypertensive agents (amlodipine and labetalol). Extensive evaluation, excluding renal angiography, did not show an explanation for the hypertension, other than the hypercalcaemia and the underlying WBS.
The hypercalcaemia was treated with hyperhydration, furosemide and a reduced calcium intake. Laboratory tests ruled out other causes than the WBS for the hypercalcaemia (Table 1). To prevent nephrocalcinosis due to the subsequent hypercalciuria (urine calcium-creatinine ratio up to 3.0 mmol/mmol), potassium citrate was administered.
As this treatment just led to a small reduction in serum calcium (Figure 1), a bisphosphonate was administered, in a low dose to prevent hypocalcaemia. This resulted in only a short and mild reduction of the serum calcium, so repeated and increased doses of pamidronate were administered, all with only short-lasting effects (Figure 1). With every return of hypercalcaemia, the patient also showed
