Vitamin D levels around the world - DSM review
3.1 Vitamin D: a critical and essential micronutrient for human health
Frontiers in Physiology, 1664-042X, Provisional PDF published on: www.frontiersin.org:
Igor Bendik, Angelika Friedel, Franz F. Roos, Peter Weber & Manfred Eggersdorfer
DSM Nutritional Products Ltd, Kaiseraugst, Switzerland
Correspondence: Dr. Igor Bendik, DSM Nutritional Products Ltd,
Department of Human Nutrition and Health, Bldg 201/219A, P.O. Box 2676, CH-4002 Basel, Switzerland, E-mail: Igor.bendik@dsm.com
Conflict of Interest Statement: All authors are employees of DSM Nutritional Products Ltd. They declare no conflict of interest.
Note by VitaminDWiki: images were adapted by this study from another DSM publication in 2014 which is behind a paywall
64 Hilger J, Friedel A, Herr R, Rausch T, Roos F, Wahl DA, et al. A systematic review of vitamin D status in populations worldwide. Br J Nutr (2014) 111(1):23-45.
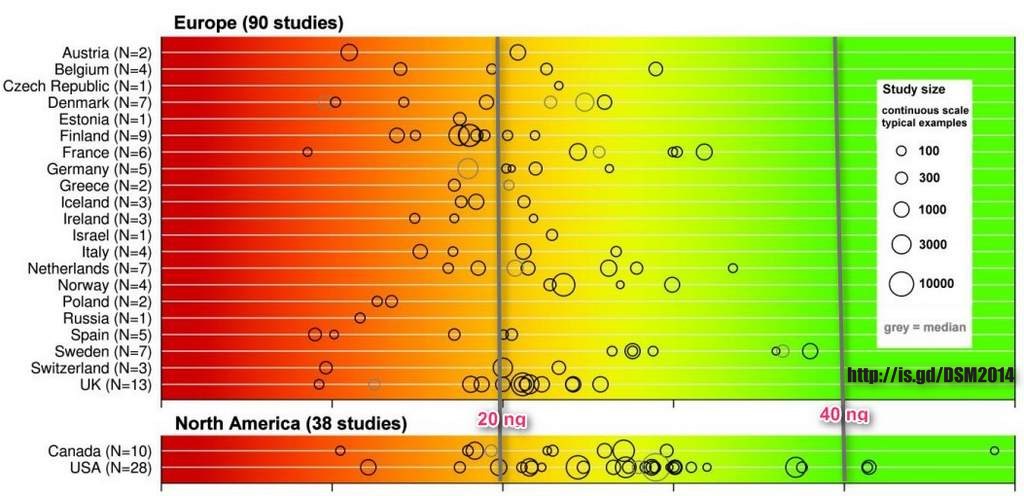
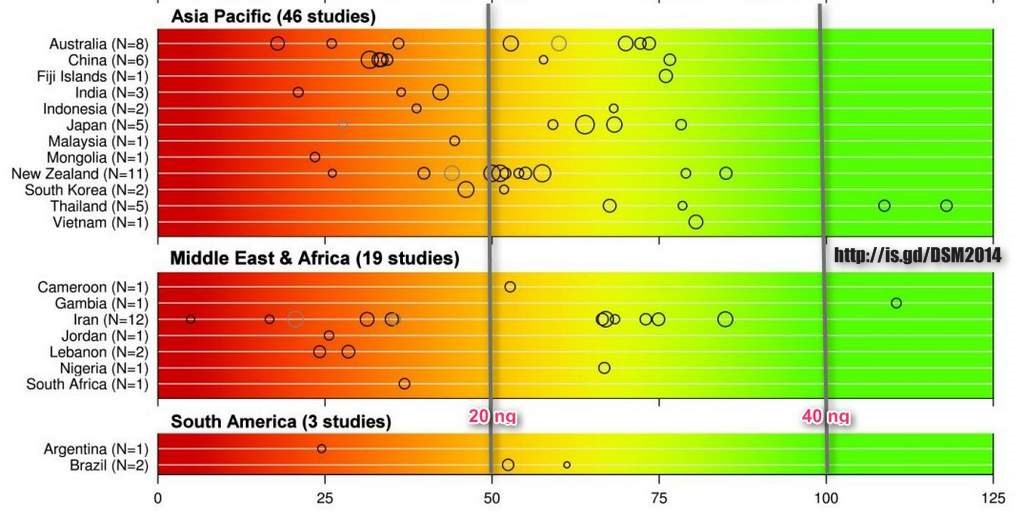
Fig. 1 Overview of published 25-hydroxyvitamin D mean / median values by countries .
The color trend from red, yellow to green shown above the graphical diagram represents the current uncertainty around the definition of 25-hydroxyvitamin D3 serum thresholds starting from severe deficiency (red), deficiency, insufficiency to total repletion (green). The reported medians are shown as black circles, studies that reported means are given in grey circle. The strength of the published valued (study size) is indicated by the circle size. Mean/median values falling within the intensely red zone are most consistent with severe vitamin D.
Vitamin D is a micronutrient that is needed for optimal health throughout the whole life. Vitamin D3 (cholecalciferol) can be either synthesized in the human skin upon exposure to the UV light of the sun, or it is obtained from the diet. If the photoconversion in the skin due to reduced sun exposure (e.g. in wintertime) is insufficient, intake of adequate vitamin D from the diet is essential to health. Severe vitamin D deficiency can lead to multitude of avoidable illnesses; among them are well known bone diseases like osteoporosis, a number of autoimmune diseases, many different cancers and some cardiovascular diseases like hypertension are being discussed. Vitamin D is found naturally in only very few foods. Foods containing vitamin D include some fatty fish, fish liver oils, and eggs from hens that have been fed vitamin D and some fortified foods in countries with respective regulations. Base on geographic location or food availability adequate vitamin D intake might not be sufficient on a global scale. The International Osteoporosis Foundation (IOF) has collected the 25-hydroxy-vitamin D plasma levels in populations of different countries using published data and developed a global vitamin D map. This map illustrates the parts of the world, where vitamin D did not reach adequate 25-hydroxy-vitamin D plasma levels: 6.7 % of the papers report 25-hydroxy-vitamin D plasma levels below 25 nmol/L, which indicates vitamin D deficiency, 37.3 % are below 50 nmol/l and only 11.9% found 25-hydroxy-vitamin D plasma levels above 75 nmol/L target as suggested by vitamin D experts. The vitamin D map is adding further evidence to the vitamin D insufficiency pandemic debate, which is also an issue in the developed world. Besides malnutrition, a condition where the diet does not match to provide the adequate levels of nutrients including micronutrients for growth and maintenance, we obviously have a situation where enough nutrients were consumed, but lacked to reach sufficient vitamin D micronutrient levels. The latter situation is known as hidden hunger. The inadequate vitamin D status impacts on health care costs, which in turn could result by significant savings, if corrected. Since little is known about the effects on the molecular level that accompany the pandemic like epigenetic imprinting, the insufficiency-triggered gene regulations or the genetic background influence on the body to maintain metabolic resilience, future research will be needed. The nutrition community is highly interested in the molecular mechanism that underlies the vitamin D insufficiency caused effect. In recent years, novel large scale technologies have become available that allow the simultaneous acquisition of transcriptome, epigenome, proteome or metabolome data in cells of organs. These important methods are now used for nutritional approaches summarized in emerging scientific fields of nutrigenomics, nutrigenetics or nutriepigenetics. It is believed that with the help of these novel concepts further understanding can be generated to develop future sustainable nutrition solutions to safeguard nutrition security.
3.1.1. Introduction
Vitamin D is needed to maintain calcium concentrations within a narrow physiological range. This function is vital as the calcium ion is essential for a large variety of cellular and metabolic processes in the body (1). To secure the calcium supplies besides intestinal absorption, calcium is stored in the skeleton and acts as a large calcium reservoir that is mainly controlled by PTH and vitamin D (2). Humans produce vitamin D by exposure to sunlight that includes ultraviolet B radiation (wavelength 290 to 315 nm); if ultraviolet B radiation is not available in sufficient amounts, vitamin D needs to be obtained from the diet or dietary supplements (3). The start of the vitamin D endocrine system is believed to have been initiated before the start of vertebrates and evolved over millions of years (4). Therefore, the vitamin D micronutrient either synthesized through the sun by the skin or through dietary uptake is well adapted to the human body. The endogenously conjugated vitamin D metabolites have taken over many important roles in the maintenance of human health, of which many still await to be discovered.
In this paper, we summarize the knowledge on vitamin D as an essential micronutrient important for human health and discuss the new nutritional research on its way to gain further knowledge on the function of vitamin D for nutrition.
3.1.2. Vitamin D part of nutrition and content in foods
The history of vitamin D is linked to first scientific description of the classic bone disease rickets by Whistler in 1645 (5). Two centuries later it was Schiitte who observed the usefulness of cod liver oil in the treatment of rickets and osteomalacia in 1824. The hunt for the anti-rachitic factor ended in early 20th century, when Mellanby could demonstrate in a series of hallmark studies (1919 to 1924) that a nutritional component in the diet was the anti-rachitic factor to prevent rickets (6-8). Shortly after, vitamin D was inaugurated without the characterization of the chemical structure. In 1919, Hudschinsky showed in parallel that UV light was able to ameliorate rickets by increasing calcification in rachitic children (9, 10). Both findings of the cod liver oil and the UV light preventing rickets remained independent observations until Hess and Weinstock elegantly could demonstrate that the anti-rachitic vitamin D was produce by UV irradiation in skin (11, 12). In 1936, Windaus and colleagues determined the chemical structure of the fat-soluble seco-steroid vitamin D (13).
The vitamin D definition comprises a group of molecules called the calciferols. The main forms present in foods are cholecalciferol (vitamin D3) and ergocalciferol (vitamin D2), whereas the metabolite 25-hydroxycholecalciferol (25-hydroxyvitamin D3) is a natural part of the food chain by its occurrence in animal products. Vitamin D3 is unique by the fact that the same nutrient can be synthesized in the skin through the action of sunlight or being taken up by diet. This dual source of intake secures the body to maintain sufficient vitamin D levels in the body. The production in skin is the major vitamin D3 source for the body. Exposure of the precursor 780 dehydrocholesterol in the basal and suprabasal layers of the epidermis to ultraviolet B (UVB) light with a wavelength of 290-315 nm is needed for the formation of the previtamin D3. The subsequent conversion is a non-enzymatic process that includes a thermal isomerization of the previtamin D3 to produce vitamin D3 (14, 15). This vitamin D3 is rapidly converted to 25-hydroxyvitamin D3 in the liver. The vitamin D status is evaluated by measuring the circulating levels of serum 25-hydroxyvitamin D, which is the sum of cutaneous synthesis (vitamin D3) or dietary contribution (vitamin D3 and vitamin D2). The 25-hydroxyvitamin D3 needs to be further hydroxylated in the kidney (or locally in other organs) to form 1,25-dihydroxyvitamin D3, the active endogenous hormone, which is responsible for most of the physiological actions of vitamin D through the binding to the vitamin D receptor (VDR). The plant-derived vitamin D2 is processed in the same way. For both vitamers, vitamin D2 and vitamin D3, the consecutive molecular action is believed to be identical, whereas only 1,25-dihydroxy vitamin D3 is the endogenous hormone, the activated vitamer 1,25-dihydroxyvitamin D2 is hormone mimetic. Therefore, it was not surprising that vitamin D3 has been reported to be superior to vitamin D2 in terms of bioavailability and maintaining the vitamin D status by the majority of studies (16, 21). Only one study reported that the two vitamers were essentially equipotent (22).
The level of cutaneous vitamin D3 synthesis is mainly affected by the amount of solar UVB radiation reaching the human skin, which is a function that needs to take into account the wavelength, thickness of the ozone layer in the atmosphere and solar zenith angle. Furthermore, the geographic latitude, season of the year and time of day influence and restrict the skin-borne synthesis of vitamin D3 (23, 24). It was described that vitamin D3 synthesis in the skin declines with age, which is due in part to a fall of 7-dehydrocholesterol and the morphological changes due to biological aging (25, 26). In 1991, Matsuoka et al (27) have shown that in Caucasians and Asian subjects having a lighter skin pigmentation UVB radiation produce significantly higher vitamin D3 serum levels than in African American and East Indian groups. It is not of a surprise that skin pigmentation reduces vitamin D3 formation. This skin tone dependent down regulation is easily overcome by increased sun exposures (28). Apart to darker pigmented skin, cutaneous vitamin D3 production can be reduced for many other reasons like severe air pollution in large cities, less outdoor activity as a consequence of an unhealthy lifestyle change, immobility of institutionalized elderly populations, topical application of sunscreens with a high sun protection factors or cultural dress codes (e.g. veiling). Therefore, dietary intake of vitamin D through foods or supplements plays a vital part to maintain healthy vitamin D levels.
Through nutrition, vitamin D intake is limited. There are few naturally-occurring food sources containing relevant levels of vitamin D. Table 1 summarizes the vitamin D content in selected foods. Vegetarian diets are limited to the plant vitamin D2 (ergocalciferol) that is only present in some mushrooms. Commercially dark cultivated white button mushrooms contain low amounts of vitamin D2, only wild mushrooms or sun-dried mushrooms contain elevated amounts of ergocalciferol (29-32). Some commercial producers include an UVB radiation step to increase the vitamin D2 content in their products (33, 34). Vitamin D2 is formed out from ergosterol in the mushrooms. Some plants that are used as foods however can contain ergosterol, but this provitamin form is not converted to vitamin D2. Vitamin D3 is not found in food-borne plants. In plants, the occurrence of vitamin D3-related compounds is scarce. Interestingly, the botanical Solanaceae family, Solanum malacoxylon (S. glaucophiyllum and S. glaucum) contains a glycoside of the active 1,25-dihydroxyvitamin D3 hormone (35-37). This deciduous shrub (1.53.0 m stem length) is widely distributed in the provinces of Buenos Aires in Argentina and in Brazil and is responsible for the calcinotic disease in cattle and other grazing animal.
Animal food products are the main dietary source for naturally occurring vitamin D3 (38). Since the discovery of vitamin D, vitamin D was associated with oily fish products. It was driven by the early observation that the amount of vitamin D in a teaspoon of cod liver oil was sufficient to prevent rickets in infants. It is still the fish liver oil that contains the highest amounts of vitamin D3. The highest reported concentration was found in skipjack liver oil 144'400 |ig / 100 g (39). The fish liver oils besides other nutritional ingredients might contain high levels of vitamin A.
The vitamin A to vitamin D ratio in the fish liver oils is species and fishing area dependent. The ratio range starts with a factor of 0.5 for skipjack liver oil and can even reach an extreme ratio of 119 (pollack liver oil) (39). This wide vitamin A to vitamin D ratio range is the reason why fish liver oils often need further processing. In fresh fish products we observe a huge variation in the vitamin D3 content per 100 g wet weight (39-47) (table 1). Large variations in vitamin D3 content were found within the same species, but also between the different fish species. Fish
obtain their vitamin D3 requirements through their diet (48). Therefore, the vitamin D3 levels in the zooplankton, the primary food source of fish, or seasonal changes in the zooplankton reservoirs in the different habitats, might be the reasons for the observed fluctuation in the fish product. Interestingly, the weight, the sex, or the age of the fish could not be correlated to the vitamin D3 content. Furthermore, no significant correlation between the tissue fat content and vitamin D levels was detected (43, 44). Significant differences in vitamin D3 content were found between muscle and skin tissues and even more pronounced between muscle and liver tissues (46). The 25-hydroxyvitamin D3 compound was also detected, though at low concentrations (44,46, 49, 50).
Wild and sun-dried mushrooms can be a good dietary source of vitamin D2 (29-32, 47, 51). However, the commercially produced mushrooms, e.g. the white button mushroom, do not contain or contain only very low amounts of vitamin D2 (29, 32, 51). The vitamin D2 content in commercially produced mushrooms can be increased by UVB exposure during the culturing or the postharvest process (33, 34). The concentration of vitamin D in eggs can vary from 0.4 |ig to 12.1 |ig (49, 52-55), it is in a similar range like offal (56-58). Other animal products like pork, beef and chicken muscle meat are low in vitamin D content (49, 56-59). By adding vitamin D3 into the feed, the vitamin D3 content can be increased in muscle and liver of cattle, to 4.6 |g per 100 g of tissue and 99.6 |ig per 100 g of tissue, respectively (60). Milk, unless fortified, has been shown to contain no or very little amounts of vitamin D, whereas in dairy products like butter and cheese the vitamin D content is higher, but in serving size amounts still very low (47, 56, 61, 62). In general, household cooking seems to have some effect on vitamin D stability depending on the actual foodstuffs and the heating process used (30, 63). To meet the vitamin D needs in the countries some states fortify foods. Dairy products are ideal for vitamin D fortification. In Canada vitamin D fortification is mandatory for milk (1 |g / 100 ml) and margarine (13.3 |ig / 100 g) (64). In other countries, like the United States, vitamin D fortification is optional for products like milk, breakfast cereals and fruit juices (65). In the National Nutrient Database for Standard Reference (release 26) of the U.S. Department of Agriculture (USDA)'s Nutrient Databank System (66), 5'036 foods have been determined for their vitamin D content, of which only 259 food items had detectable vitamin D levels. The data showed that per serving only seven fish products had >15 |ig vitamin D. All 29 foods that contained between 15 |ig - 2.5 |ig vitamin D per serving were either fortified foods (21) or fish produce (8). Two-thirds of all vitamin D containing foods were far below the 1.0 |ig level, whereas 20 percent had even negligible vitamin D content per serving (below 0.1 |ig).
Despite the fact that moderate sun exposure of arms and legs in summer for 5 to 30 minutes between the hours of 10 a.m. and 3 p.m. twice a week is enough to produce sufficient vitamin D3 in the body(3), it is astonishing that many populations fail to achieve this goal (67-70). During winter time, when vitamin D3 production by the sun ceased, adequate vitamin D levels can only be achieved by UVB exposure from indoor tanning units, or by a daily diet of fortified foods or a few selected food items. This limitation is one of the reasons, why the use of dietary vitamin D supplements has become so popular. It is currently the most applied and secure option to reach adequate vitamin D intake levels (3).
3.1.3. Vitamin D map, malnutrition, hidden hunger and nutrition security
An accepted biomarker for the vitamin D status in the general population is to measure the serum concentration of 25-hydroxyvitamin D levels, which is the major circulating form of vitamin D and reflects both dietary vitamin D intake and the endogenous vitamin D production (71, 72). The serum concentration of 25-hydroxyvitamin D is linked to the serum level of the active hormone 1,25-dihydroxyvitamin D and also to the clinical relevant parathyroid hormone level. Lips has classified the 25-hydroxyvitamin D levels into four stages (72, 73): severe deficiency (<12.5 nmol/L), deficiency (12.5 - 25 nmol/L), insufficiency (25 - 50 nmol/L), repletion (> 50 nmol/L). The thresholds for severe deficiency and deficiency are undisputed; however, a controversy has arisen for defining the border between insufficiency and repletion. In 2011, the Institute of Medicine (IOM) suggested a serum level of 50 nmol/L as the value at which 97.5% of the vitamin D needs of the population would be covered (74, 75), whereas, the Endocrine Society (ES) defined it to be higher: 75 nmol/L (76). All deficiency levels including insufficiency, as so-called mild deficiency, must be prevented through focused supplementation.
In 2010, the Institute of Medicine (IOM) introduced new dietary reference intake (DRI) values for vitamin D after comprehensive reviewing of more than 1'000 high quality research articles to renew thereby their first settings from 1997 (74). The DRIs address an adequate nutritional intake of all sources. The IOM has set the dietary allowance (RDA) to 600 IU per day for the general population and at 800 IU per day for persons 70 years and older, whereas 1 IU is the biological equivalent of 0.025 |ig vitamin D3. The tolerable upper intake level or UL (Upper Level of Intake), which represents the safe upper limit, was set to 4'000 IU per day for vitamin D intake (75). The new RDAs reflect the scientific outcome from large dietary studies that revealed vitamin D insufficiency (77, 78). In 2012, Troesch et al. analyzed the vitamin intake from different dietary surveys that included the German Nutritional Intake Study (Nationale Verzehrstudie II) 2008, the US National Health and Nutrition Examination Survey (NHANES) from 2003 to 2008, the UK (the British National Diet and Nutrition Survey 2003) and the Netherlands (Dutch National Food Consumption Survey 2007-10), and could confirm that vitamin D is one of the critical vitamins, which intake is below the recommendation (79).
A gap exists between the intake and the recommendation of vitamin D. The chronic insufficient intake of micronutrients like vitamin D without seeing immediate clinical signs is called Hidden Hunger. Hidden Hunger, in particular for vitamin D, is more prevalent in the populations of the developed countries as anticipated (80). Hidden Hunger is a threat for the nutrition security for a given country. Nutrition security mandates sufficient micronutrients in an adequate food supply and is required to safeguard an optimal nutritional status of a population.
Many groups have identified vitamin D deficiency or insufficiency to become a public health problem worldwide (3, 67, 68, 70, 81, 82). Mithal et al., 2009 described in their global report that most populations do not achieve a desirable vitamin D status and particular people at risk and elderly people suffer from vitamin D deficiency. In two reports, the International Osteoporosis Foundation (IOF) and its partners published the global vitamin D status map (67, 70). The vitamin D map was based on a systematic review of the worldwide vitamin D levels, using all available publications published between 1990 and February 2011 (67). Eligible studies include 168'389 participants from the general populations throughout the world where the mean or median serum 25-hydroxyvitamin D levels were measured. Studies included had a cross-sectional design or were based on a population based cohorts. The analysis identified nearly 200 studies from 44 countries, whereas only half of the studies were included in the global vitamin D status map as 50.2% of the studies were not representative for the target populations.
Figure 1 Vitamin D an important micronutrient
shows the global vitamin D status map listed by countries and by continents. The largest numbers of studies were performed in Europe, followed by North America and Asia-Pacific. Available data from Latin America and even more from Africa are limited. Results of this review showed that 6.7% of the population were vitamin D deficient (mean 25-hydroxyvitamin D values <25nmol/l), 37.3% were vitamin D insufficient according to IOM (mean values below 50nmol/l) and 88.1% of the population showed an insufficient vitamin D status according to the Endocrine Society (mean values below 75nmol/l). No significant differences were found for gender or age, when looking at the worldwide data, but some regional differences could be identified (67). The 25-hydroxyvitamin D serum levels were higher in Europe and the US, when compared to Middle East and Africa. This might be due to the vitamin D food fortification programs in North America (83). Furthermore, the systematic analysis revealed that institutionalized elderly were more at risk to have low 25-hydroxyvitamin D levels in Europe and Asia/Pacific. The compared non-institutionalized elderly group showed higher levels, possibly due to spending more of time outdoors. The group of institutionalized elderly is therefore at high risk to become vitamin D deficient. Further research is needed to inform public health policy makers to reduce the risk for potential health consequences of low vitamin D status.
In the past few years the national recommendations for dietary vitamin D were adjusted in several countries; they are not harmonized across the European Union yet and vary from 200 IU to 800 IU. The higher recommendations for dietary vitamin D intake are increasingly being suggested in government documents, position statements and clinical practice guidelines for bone health. In 2008, the U.S. Food and Drug Administration updated the health claim for the prevention of osteoporosis by including vitamin D to the consumption of calcium (84). In 2008, the American Academy of Pediatrics also reacted and issued an update of their guidelines for vitamin D intake and rickets prevention (85). They doubled the recommended dose of vitamin D for children to 400 IU per day, beginning in the first few days of life and continuing throughout adolescence. In 2010, the Institute of Medicine (IOM) released the revised Dietary Reference Intakes (DRI's) for calcium and vitamin D and tripled the recommendations for vitamin D intakes to 600 IU per day for children and all adults up to age 69 years (74). The IOM stated that there was insufficient evidence to make recommendations for non-skeletal benefits.
In 2012, the German, Austrian and Swiss Nutrition Societies raised the recommended vitamin D intake to 800 IU per day , in case of absent UVB exposure, for all age groups starting from 1 year of age (86). Furthermore, key opinion leaders are increasingly recommending higher daily intakes for vitamin D, between 800 IU and 1000 IU or even higher for people at risk or older adults. The recent statement by the International Osteoporosis Foundation (IOF) and the guidelines by the US Endocrine Society suggest that higher vitamin D doses would be needed to achieve the desirable 25-hydroxyvitamin D serum level of 75 nmol/L for people at risk or older individuals.
Increasing the vitamin D levels in the population would also ameliorate health economics. Grant et al., 2009 calculated the benefit of increasing vitamin D levels to reduce the economic burden of diseases (87). A rise in the vitamin D serum level of all European to 40 nmol/L would reduce the economic burden of different diseases and could save health care costs of up to 16.7%. Besides reducing the economic costs vitamin D intake could in addition also reduce mortality rates and maintain a longer healthy life style.
3.1.4. Nutritional research to address and understand vitamin D insufficiency
Vitamin D deficiency is undoubtedly linked to severe consequences in the growing child by causing incomplete mineralization of the bone and in the adult accounting to wasteful osteomalacia. In the vitamin D insufficiency stage, this severity gets gradually less, but the outcome remains unchanged. Besides the established and accepted functional skeletal health relationship, more and more evidence is accumulating for falls (88-94) and physical performance (95-100), which has been recognized by a health claim of the European Food and Safety Authority in 2011: 'Vitamin D may reduce the risk of falling. Falling is a risk factor for bone fractures.' This health claim is targeting men and women 60 years of age and older and the dose required is a daily consumption of 800 IU vitamin D which can come from all sources. Further emerging vitamin D health relationships include physiological parameters like improved immune response (101-104), improved respiratory health(105-108) possibly also relate to reduced tuberculosis incidence (109-114); and reduced risk to develop autoimmune diseases like multiple sclerosis (115-117) or type 1 diabetes (48, 101, 118-122). In chronic, non-communicable diseases, vitamin D deficiency is being discussed to possibly ameliorate the incidence of some neoplastic diseases like colorectal, lung, prostate and breast cancers (123-126); cardiovascular diseases (CVDs) including hypertension, myocardial infarction, stroke (127-134); life-style diseases like obesity and type 2 diabetes (2, 122, 135-140); diseases related to the decline in sight function including age-related macular degeneration(141-143); and neurological disorders including Alzheimer and Parkinson disease (144-147). One may wonder about the width of possible implications being looked at, but considering the more than 1'000 genes which vitamin D is regulating through the vitamin D receptor (148), this may actually not be a surprise. To determine the potential role of vitamin D supplementation in the prevention or treatment of chronic non-skeletal diseases notwithstanding, large-scale clinical trials are demanded. In this respect for the nutrition field, four new large-scale ongoing long-term supplementation studies are expected to deliver results in near future (Table 2). The two very large studies, VITAL trial (n=20'000) and FIND study (n=18'000), are meant to deliver clinical evidence what effect vitamin D3 has on cancer CVDs and diabetes outcomes. The two smaller trials, CAPS and DO-HEALTH, including more than 2'000 participants each are including cancer, infections, fractures, hypertension, cognitive function and physical performance outcomes. In all four studies the placebo group will produce vitamin D3 in the skin and will consume part of it in the food, and therefore this will narrow the gap between the placebo and treatment groups. It remains to be seen whether the applied supplementation doses (2'000IU and 1'600 IU, 3'200 IU) will be sufficient to see a clear difference between the treatment and the control groups. An open likelihood will remain for the placebo group potentially obtaining sufficient vitamin D3 (600 IU - 800 IU), levels that are considered to be sufficient for skeletal effects. In such a case only an incremental increase of an additional ~1'000 IU can be considered as the effective dose, for which no power calculation was available at the time before study begin. In light of such a situation, it will be of interest whether the micronutrient triage theory of Bruce Ames can be validated with vitamin D3 (149, 150). The triage theory postulates, as a result of recurrent shortages of micronutrients during evolution, that the body has selected and developed a metabolic rebalancing response to shortage. These rebalancing favored micronutrient-needs for short term survival, while those only required for long-term health were starved. In the case of the micronutrient vitamin D3, calcium and bone metabolism can be considered to be secured with highest priority, therefore, it might be speculated that the 600 IU- 800 IU intake would satisfy this vitamin D3 serum level threshold. For the chronic non-skeletal diseases however, which have only secondary priority in an evolutionary perspective, higher serum vitamin D3 levels would be required. The ongoing four vitamin D3 studies that have chronic diseases as their main outcomes and use nutritionally relevant ~2'000 IU are therefore well suited to address whether the triage theory holds also true for the micronutrient vitamin D3.
Vitamin D3 once in the blood immediately binds to the vitamin D-binding protein (DBP) and gets transported into the liver (3). The first hydroxylation at position 25 generates the major circulating metabolites 25-hydroxyvitamin D3. This metabolite circulates throughout all organs and undergoes hydroxylation at position 1, which occurs mainly in the kidney, but also in other organs, to form 1,25-dihydroxyvitamin D3, the active hormone. Besides the major circulating metabolite 25-hydroxyvitamin D3 and the hormonally active metabolite 1,25-dihydroxyvitamin D3, more than 35 additional vitamin D3 metabolites are formed by the body (151, 152). It is speculated that they might be intermediates in the catabolism of 1,25-dihydroxyvitamin D3. The human body has evolved many CYP enzymes and invests energy to form these additional 35 vitamin D3 metabolites, whether this is for the purpose to catabolize 1,25-dihydroxyvitamin D3, remains still to be answered. More appealing is the theory that these metabolites are formed to fulfill yet unknown functions of vitamin D3. This perspective could potentially also account to the pleiotropic non-skeletal health benefits reported from the many vitamin D intake studies. For some of the vitamin D3 metabolites like the 24R,25-dihydroxyvitamin D3 potential function was explored in vitro (153).
The 24R,25-dihydroxyvitamin D3 has been shown to be an essential hormone in the process of bone fracture healing. The 24R,25-dihydroxyvitamin D3 likely initiates its biological responses via binding to the ligand binding domain of a second cell membrane receptor, the VDR(mem24,25) (153). From the nutritional point of view it will be of interest to investigate the 355 function of the all vitamin D3 metabolites and relate the function to the level of vitamin D3 intake to secure the health benefit according the triage theory.
According to the current knowledge, the vitamin D endocrine system is funneled through the biologically most active metabolite 1,25-dihydroxyvitamin D3 that is mainly produced in the kidney, but also in other organs (154). Mechanistically 1,25-dihydroxyvitamin D3 binds the vitamin D receptor (VDR) directly on a DNA sequence, the 1,25-dihydroxyvitamin D3 response element (VDRE), in the regulatory region of primary 1,25-dihydroxyvitamin D3 target genes (148). The VDR forms together with the retinoid X receptor or putative other transcription factors a heterodimer on the VDRE, recruiting tissue-specific transcriptional co-activators and regulates through a conformational change upon 1,25-dihydroxyvitamin D3 binding the downstream gene. The VDR is widespread in more than 30 tissues (152) and may trigger expression of more than 1'000 genes through 1,25-dihydroxyvitamin (155, 156). The regulation of tissue-specific gene expression by 1,25-dihydroxyvitamin D3 is of high interest, as it guides us towards the better understanding of the mechanistic action of vitamin D3 in the different tissues. The gained knowledge from the mechanistic studies can help to design smaller and more focused nutritional intervention RCTs to answer whether vitamin D contributes to a specific health benefit of interest. In this respect the GeneChip-based transcriptomics methodology using high-density microarrays demonstrated the expression of genes in a variety of important functions of more than 100 different pathways that could be linked to vitamin D deficiency (156,158). The development of chromatin immunoprecipitation (ChiP) methodology linked to site-specific PCR amplification of the VDR bound genomic DNA fragment, and later the methods using tiled microarrays (ChiP-chip) applying the first unbiased genome-wide approach, which then was followed by the massive parallel NGS sequencing approach of the immunoprecipitated DNA segments, opened up new avenues to investigate 1,25-dihydroxyvitamin D3 target genes in selected tissues (155, 159-162). In an elegant study, Carlberg et al. identified in samples of 71 pre-diabetic individuals of the VitDmet study changes in serum 25-hydroxyvitamin D3 concentrations that were associated to primary vitamin D target genes (155). Based on their finding the authors proposed the genes CD14 and THBD as transcriptomics biomarkers, from which the effects of a successful vitamin D3 supplementation can be evaluated. These 385 biomarkers are potentially suitable for displaying the transcriptomics response of human tissues to vitamin D3 supplementation.
Epigenetic alterations of the genome refer to heritable and modifiable changes in gene expression that are not affecting the DNA sequence. They may be inherited as Mendelian, non- Mendelian or environmentally caused traits. One of the 1,25-dihydroxyvitamin D3 induced epigenetic modification was shown for the hypo-methylating effect on the osteocalcin promoter (163). 1,25-dihydroxyvitamin D3-was associated with the demethylation of the osteocalcin promoter and induced the osteocalcin gene expression. The activity of VDR can be modulated by epigenetic histone acetylation. The VDR alone or in concert with other transcription factors can recruit histone-modifying enzymes like histone acetyl transferases (HATs) or histone deacetylases (HDACs) and epigenically direct transcriptional expression of downstream genes (156, 164-166). The trans-generational epigenetic inheritance of vitamin D3 triggered epigenome modification is not fully explored, however maternal vitamin D deficiency has been discussed with adverse pregnancy outcomes or potential susceptibility for diseases (156, 165, 166). For future nutritional research it would be of great value to identify and validate epigenetic biomarkers that could serve as risk assessment tool for vitamin D insufficiency related susceptibility to develop a disease later in life.
Variations in vitamin D status have been shown to be related to inheritance. The disparity of vitamin D levels according to ethnicity given skin pigmentation is well established (167, 168). Dark skinned population individuals have compared to Caucasian descendants almost one-half the serum concentrations of 25-hydroxyvitamin D (169). From twin studies it has been estimated that the heritability of genetic regulation of vitamin D levels to be between 23% to 80% (170). In addition, large-scale genetic association studies using linkage disequilibrium analysis have identified genetic loci correlating with serum vitamin D level within five candidate genes (170). The identified SNPs are within the 1alpha-hydroxylase of 25-hydroxyvitamin D (CYP27B1) gene, the 25-hydroxylase of vitamin D (CYP2R1) gene, the vitamin D carrier protein (GC) gene, the vitamin D receptor (VDR) gene, and the cytochrome P-450 (CYP24A1) gene coding for an enzyme that inactivates 1,25-dihydroxyvitamin D. It is important to note that replication studies in separate populations have to follow to verify the validity of the identified SNPs. The SNP information will provide the additional guidance towards a personalized nutritional advice to reach a sufficient vitamin D status.
3.1.5. Conclusion and future perspectives
In the recent years the knowledge about vitamin D and its implications have extended far beyond its classical role in bone health in either fields of basic research as well as in human trials. In particular, the evidence for the role of vitamin D in reducing the risk of fractures as well as decreasing the risk for falling is convincing and authorities have responded to it. Besides a health claim issued by the EFSA on the risk reduction for falling the dietary intake recommendations have been significantly increased in several countries such as the US and in Europe (Austria, Germany, Switzerland). A number of other countries around the globe are in the process of establishing new dietary intake recommendations as well. It turns out that on average a daily intake of 600 - 800 IU vitamin D appears to be required to meet fundamental needs of the human body, for specific applications higher daily intakes may be necessary, which will become clearer as the results of a number of ongoing clinical studies will become available.
The obvious question to answer is: do people obtain the recommended amounts of vitamin D? The diet is typically only a minor vitamin D source as only few food items contain relevant amounts of vitamin D, such as fatty sea fish. The primary vitamin D source for humans is the vitamin D synthesis in the skin from vitamin D precursors by the sunlight - provided the skin is sufficiently exposed to strong enough sun radiation. Several groups have reviewed the published results on 25-hydroxyvitamin D serum levels the established marker of the vitamin D status showing that low 25-hydroxyvitamin D levels are found in many cohorts around the world. A recent systematic review of the global vitamin D status (67) showed that 6.7% of the overall populations reported deficient 25-hydroxyvitamin D levels below 25 nmol/L, 37% had 25-hydroxyvitamin D levels below 50 nmol/L and only 11% were above 75 nmol/L, which is considered an adequate status by the IOF and the Endocrine Society. So a very important task ahead of us is to find efficient ways to improve the vitamin D status on the population level, be it by dietary means, food fortification or dietary supplements.
In addition, it will be very important to gather sound and convincing evidence for the many additional implicated health benefits of vitamin D besides the ones that already reached a health claim status and to see which of them will actually hold up. This will require appropriate human studies on the one hand, and also involve the appropriate use of the novel experimental approaches like nutrigenomics , nutrigenetics and nutriepigenetics on the other hand. In conclusion, the evidence we have for vitamin D in human health is exciting, however we have to make sure that appropriate measures are taken to improve the vitamin D status to the levels required to be beneficial for human health. In future, we will also need to further apply, exploit and invest in novel, innovative and break-through technologies in the vitamin D research to understand the underlying mechanisms by which vitamin D is exerting so many effects in the human body, which is knowledge needed to the purpose to obtain and secure optimal public health through nutrition.
Table 2. List of ongoing large nutritional vitamin D3 supplementation trials (> 2'000 subjects)
using nutrition-related daily vitamin D3 doses (1'600 -3'200 IU)
|
ACRONYM |
NAME CLINICALTRIAL IDENTIFIER |
PRINCIPAL INVESTIGATOR |
PLACE |
PARTICIPANTS |
DOSE |
DURATION |
MAIN OUTCOMES |
RESULTS EXPECTED |
WEB LINK |
|
CAPS |
Clinical Trial of Vitamin D3 to Reduce Cancer Risk in Postmenopausal Women NCT01052051 |
Joan Lappe, Creighton University |
USA |
2'332, healthy postmenopausal women: 55+ |
2'000 IU D3(and 1,500 mg calcium) daily |
5 years |
All cancers |
2015 |
http://clinicaltrials.gov/ct2/show/ NCT01052051?term=NCT01052 051&rank=1 |
|
VITAL |
Vitamin D and Omega-3 Trial NCT01169259 |
JoAnn E. Manson, Brigham and Women's Hospital |
USA |
20'000, men: 50+ women: 55+ |
2'000 IU D3, daily omega-3 fatty acids |
5 years |
Cancer, Cardiovascular disease |
2017 |
http://clinicaltrials.gov/show/NCT 01169259 |
|
DO-HEALTH |
Vitamin D3 - Omega3 - Home Exercise -Healthy Ageing and Longevity Trial NCT01745263 |
Heike Bischoff- Ferrari, University Zurich |
8 European Cities |
2'152, 70+ |
2'000 IU D3 daily omega-3 fatty acids |
3 years |
Infections, Fractures, Blood pressure, Cognitive function, Lower extremity function |
2017 |
http://clinicaltrials.gov/ct2/show/ NCT01745263?term=bischoff-ferrari&rank=1: |
|
FIND |
Finnish Vitamin D Trial NCT01463813 |
Tomi-Pekka Tuomainen, University of Eastern Finland |
Finland |
18'000 men: 60+, women: 65+ |
1'600 IU D3 daily or 3'200 IU D3 daily |
5 years |
Cancer, Cardiovascular disease Diabetes |
2020 |
http://clinicaltrials.gov/show/NCT 01463813 |
References
1. Berridge MJ. Calcium signalling remodelling and disease. Biochem Soc Trans (2012) 40(2):297-309.
2. Bouillon R, Carmeliet G, Lieben L, Watanabe M, Perino A, Auwerx J, et al. Vitamin D and energy homeostasis - Of mice and men. Nature Reviews Endocrinology (2014) 10(2):79-87.
3. Holick MF. Vitamin D deficiency. N Engl JMed (2007) 357(3):266-81.
4. Bouillon R, Suda T. Vitamin D: calcium and bone homeostasis during evolution. BoneKEy Rep (2014) 3.
5. Norman AW. The history of the discovery of vitamin D and its daughter steroid hormone. Ann Nutr Metab (2012) 61(3):199-206.
6. Mellanby E. An Experimental Investigation ON RICKETS. The Lancet (1919) 193(4985):407-12.
7. Mellanby E. Nutrition Classics. The Lancet 1:407-12, 1919. An experimental investigation on rickets. Nutrition Reviews (1976) 34(11):338-40.
8. Platt BS. Sir Edward Mellanby, 8 April 1884-30 January 1955. The British journal of nutrition (1956) 10(3):177-81.
9. Huldschinsky K. Heilung von Rachitis durch kunstliche Hohensonne. Dtsch med Wochenschr (1919) 45(26):712-3.
10. Huldschinsky K. The antirachitic: zone of the ultra-violet. Klinische Wochenschrift (1926) 5:1972-3.
11. Hess AF, Weinstock M. The antirachitic value of irradiated cholesterol an phytosterol. III. Evidence of chemical change as shown by absorption spectra. Methods Enzymology (1925) 64:193-201.
12. Hess AF, Weinstock M. The antirachitic value of irradiated cholesterol an phytosterol. II. Further evidence of change in biological activity. Methods Enzymology (1925) 64:181-91.
13. Windaus A, Schenck F, von Werder F. Uber das antirachitisch wirksame Bestrahlungsprodukt aus 7-Dehydrocholesterin. Hoppe-Seyler's Zeitschrift fur Physiologische Chemie (1936) 241:100-3.
14. Collins ED, Norman AW. Vitamin D. In: Rucker RB, Suttie JW, McCormick DB, Machlin LJ, editors. Handbook of Vitamins. New York: Marcel Dekker Inc. (2001). p. 51-113.
15. Holick MF. Vitamin D: Photobiology, metabolism, and clinical applications. In: de Groot CP, Besser M, Burgeret HG, editors. Endocrinology. 3rd Edition ed. Philadelphia, PA: Saunders W. B. (1995).
16. Lehmann U, Hirche F, Stangl GI, Hinz K, Westphal S, Dierkes J. Bioavailability of Vitamin D2 and D3 in Healthy Volunteers, a randomised placebo-controlled trial. J Clin Endocrinol Metab (2013).
17. Trang HM, Cole DE, Rubin LA, Pierratos A, Siu S, Vieth R. Evidence that vitamin D3 increases serum 25-hydroxyvitamin D more efficiently than does vitamin D2. The American Journal of Clinical Nutrition (1998) 68(4):854-8.
18. Glendenning P, Chew GT, Seymour HM, Gillett MJ, Goldswain PR, Inderjeeth CA, et al. Serum 25-hydroxyvitamin D levels in vitamin D-insufficient hip fracture patients after supplementation with ergocalciferol and cholecalciferol. Bone (2009) 45(5):870-5.
19. Romagnoli E, Mascia ML, Cipriani C, Fassino V, Mazzei F, D'Erasmo E, et al. Short and long-term variations in serum calciotropic hormones after a single very large dose of ergocalciferol (vitamin D2) or cholecalciferol (vitamin D3) in the elderly. J Clin EndocrinolMetab (2008) 93(8):3015-20.
20. Armas LA, Hollis BW, Heaney RP. Vitamin D2 is much less effective than vitamin D3 in humans. J Clin Endocrinol Metab (2004) 89(11):5387-91.
21. Heaney RP, Recker RR, Grote J, Horst RL, Armas LA. Vitamin D3 Is More Potent Than Vitamin D2 in Humans. J Clin Endocrinol Metab (2011).
22. Holick MF, Biancuzzo RM, Chen TC, Klein EK, Young A, Bibuld D, et al. Vitamin D2 is as effective as vitamin D3 in maintaining circulating concentrations of 25-hydroxyvitamin D. J Clin Endocrinol Metab (2008) 93(3):677-81.
23. Webb AR, Kline L, Holick MF. Influence of Season and Latitude on the Cutaneous Synthesis of Vitamin D3: Exposure to Winter Sunlight in Boston and Edmonton Will Not Promote Vitamin D3 Synthesis in Human Skin. The Journal of Clinical Endocrinology & Metabolism (1988) 67(2):373-8.
24. Holick MF. Photobiology of Vitamin D. In: Feldman D, Pike JW, Adams JS, editors. Vitamin D. 1. 3rd Edition ed. London, GB: Elsevier (2011). p. 13-22.
25. MacLaughlin J, Holick MF. Aging decreases the capacity of human skin to produce vitamin D3. The Journal of Clinical Investigation (1985) 76(4):1536-8.
26. Holick MF, Matsuoka LY, Wortsman J. Age, vitamin D, and solar ultraviolet. Lancet (1989) 2(8671):1104-5.
27. Matsuoka LY, Wortsman J, Haddad JG, Kolm P, Hollis BW. Racial pigmentation and the cutaneous synthesis of vitamin D. Arch Dermatol (1991) 127(4):536-8.
28. Armas LA, Dowell S, Akhter M, Duthuluru S, Huerter C, Hollis BW, et al. Ultraviolet-B radiation increases serum 25-hydroxyvitamin D levels: the effect of UVB dose and skin color. J Am Acad Dermatol (2007) 57(4):588-93.
29. Mattila P, Konko K, Eurola M, Pihlava JM, Astola J, Vahteristo L, et al. Contents of vitamins, mineral elements, and some phenolic compounds in cultivated mushrooms. JAgricFood Chem (2001) 49(5):2343-8.
30. Mattila P, Ronkainen R, Lehikoinen K, Piironen V. Effect of Household Cooking on the Vitamin D content in Fish, Eggs, and Wild Mushrooms. JOURNAL OF FOOD COMPOSITION AND ANALYSIS (1999) 12:153-60.
31. Mattila PH, Piironen VI, Uusi-Rauva EJ, Koivistoinen PE. Vitamin D contents in edible mushrooms. Journal of Agricultural and Food Chemistry (1994) 42(11):2449-53.
32. Teichmann A, Dutta PC, Staffas A, Jagerstad M. Sterol and vitamin D2 concentrations in cultivated and wild grown mushrooms: Effects of UV irradiation. LWT - Food Science and Technology (2007) 40(5):815-22.
33. Mau JL, Chen PR, Yang JH. Ultraviolet Irradiation Increased Vitamin D2 Content in Edible Mushrooms. Journal of Agricultural and Food Chemistry (1998) 46(12):5269-72.
34. Roberts JS, Teichert A, McHugh TH. Vitamin D2 formation from post-harvest UV-B treatment of mushrooms (Agaricus bisporus) and retention during storage. Journal of Agricultural and Food Chemistry (2008) 56(12):4541-4.
35. Japelt RB, Silvestro D, Smedsgaard J, Jensen PE, Jakobsen J. Quantification of vitamin D3 and its hydroxylated metabolites in waxy leaf nightshade (Solanum glaucophyllum Desf.), tomato (Solanum lycopersicum L.) and bell pepper (Capsicum annuum L.). Food Chemistry (2013) 138(2-3): 1206-11.
36. Boland RL. Plants as a source of vitamin D3 metabolites. Nutr Rev (1986) 44(1):1-8.
37. Boland R, Skliar M, Curino A, Milanesi L. Vitamin D compounds in plants. Plant Science (2003) 164(3):357-69.
38. Schmid A, Walther B. Natural vitamin D content in animal products. Adv Nutr (2013) 4(4):453-62.
39. Takeuchi A, Okano T, Ayame M, Yoshikawa H, Teraoka S, Murakami Y, et al. High-performance liquid chromatographic determination of vitamin D3 in fish liver oils and eel body oils. J Nutr Sci Vitaminol (Tokyo) (1984) 30(5):421-30.
40. Byrdwell WC, Horst RL, Phillips KM, Holden JM, Patterson KY, Harnly JM, et al. Vitamin D levels in fish and shellfish determined by liquid chromatography with ultraviolet detection and mass spectrometry. Journal of Food Composition and Analysis (2013) 30(2):109-19.
41. Egaas E, Lambertsen G. Naturally occurring vitamin D3 in fish products analysed by HPLC, using vitamin D2 as an international standard. International Journal for Vitamin and Nutrition Research (1979) 49(1):35-42.
42. Lu Z, Chen TC, Zhang A, Persons KS, Kohn N, Berkowitz R, et al. An evaluation of the vitamin D3 content in fish: Is the vitamin D content adequate to satisfy the dietary requirement for vitamin D? Journal of Steroid Biochemistry and Molecular Biology (2007) 103(3-5):642-4.
43. Mattila P, Piironen V, Haapala R, Hirvi T, Uusi-Rauva E. Possible Factors Responsible for the High Variation in the Cholecalciferol Contents of Fish. Journal of Agricultural and Food Chemistry (1997) 45(10):3891-6.
44. Mattila P, Piironen V, Uusi-Rauva E, Koivistoinen P. Cholecalciferol and 25-Hydroxycholecalciferol Contents in Fish and Fish Products. Journal of Food Composition and Analysis (1995) 8(3):232-43.
45. Ostermeyer U, Schmidt T. Vitamin D and provitamin D in fish : Determination by HPLC with electrochemical detection. European Food Research and Technology (2006) 222(3-4):403-13.
46. Takeuchi A, Okano T, Sayamoto M, Sawamura S, Kobayashi T, Motosugi M, et al. Tissue distribution of 7-dehydrocholesterol, vitamin D3 and 25-hydroxyvitamin D3 in several species of fishes. J Nutr Sci Vitaminol (Tokyo) (1986) 32(1):13-22.
47. Kobayashi T, Takeuchi A, Okano T. Vitamin D Contents in Various Kinds of Japanese Foods. Challenges of Modern Medicine. 7. Ares-Serono Symposia , Rome (1995). p. 345-50.
48. Holick MF. Vitamin D: A millenium perspective. J Cell Biochem (2003) 88(2):296-307.
49. Bilodeau L, Dufresne G, Deeks J, Clement G, Bertrand J, Turcotte S, et al. Determination of vitamin D3 and 25-hydroxyvitamin D3 in foodstuffs by HPLC UV-DAD and LC-MS/MS. Journal of Food Composition and Analysis (2011) 24(3):441-8.
50. Ovesen L, Brot C, Jakobsen J. Food contents and biological activity of 25-hydroxyvitamin D: a vitamin D metabolite to be reckoned with? Ann Nutr Metab (2003) 47(3-4):107-13.
51. Phillips KM, Ruggio DM, Horst RL, Minor B, Simon RR, Feeney MJ, et al. Vitamin D and sterol composition of 10 types of mushrooms from retail suppliers in the United States. JAgricFood Chem (2011) 59(14):7841-53.
52. Exler J, Phillips KM, Patterson KY, Holden JM. Cholesterol and vitamin D content of eggs in the U.S. retail market. Journal of Food Composition and Analysis (2013) 29(2):110-6.
53. Mattila P, Lehikoinen K, Kiiskinen T, Piironen V. Cholecalciferol and 25-hydroxycholecalciferol content of chicken egg yolk as affected by the cholecalciferol content of feed. Journal of Agricultural and Food Chemistry (1999) 47(10):4089-92.
54. Mattila P, Piironen V, Backman C, Asunmaa A, Uusi-Rauva E, Koivistoinen P. Determination of vitamin D3 in egg yolk by high-performance liquid chromatography with diode array detection. Journal of Food Composition and Analysis (1992) 5(4):281-90.
55. Parrish DB. Determination of vitamin D in foods: a review. CRC critical reviews in food science and nutrition (1979) 12(1):29-57.
56. Mattila PH, Piironen VI, Uusi-Rauva EJ, Koivistoinen PE. Contents of cholecalciferol, ergocalciferol, and their 25-hydroxylated metabolites in milk products and raw meat and liver as determined by HPLC. Journal of Agricultural and Food Chemistry (1995) 43(9):2394-9.
57. Montgomery JL, Carr IMA, Kerth CR, Hilton GG, Price BP, Galyean ML, et al. Effect of vitamin D3 supplementation level on the postmortem tenderization of beef from steers. Journal of Animal Science (2002) 80(4):971-81.
58. Montgomery JL, Parrish FC, Beitz DC, Horst RL, Huff-Lonergan EJ, Trenkle AH. The use of vitamin D3 to improve beef tenderness. Journal of Animal Science (2000) 78(10):2615-21.
59. Strobel N, Buddhadasa S, Adorno P, Stockham K, Greenfield H. Vitamin D and 25-hydroxyvitamin D determination in meats by LC-IT-MS. Food Chem (2013) 138(2-3):1042-7.
60. Montgomery JL, King 1MB, Gentry JG, Barham AR, Barham BL, Hilton GG, et al. Supplemental vitamin D3 concentration and biological type of steers. II. Tenderness, quality, and residues of beef. Journal of Animal Science (2004) 82(7):2092-104.
61. Jakobsen J, Saxholt E. Vitamin D metabolites in bovine milk and butter. Journal of Food Composition and Analysis (2009) 22(5):472-8.
62. Trenerry VC, Plozza T, Caridi D, Murphy S. The determination of vitamin D3 in bovine milk by liquid chromatography mass spectrometry. Food Chemistry (2011) 125(4):1314-9.
63. Jakobsen J, Knuthsen P. Stability of vitamin D in foodstuffs during cooking. Food Chemistry (2014) 148:170-5.
64. Canada H. Consolidation Food and Drugs Regulation. Canada, editor: The Minister of Justice Canada (2014).
65. Calvo MS, Whiting SJ, Barton CN. Vitamin D fortification in the United States and Canada: current status and data needs. The American Journal of Clinical Nutrition (2004) 80(6):1710S-6S.
66. Haytowitz DB, Lemar LE, Pehrsson PR. USDA's Nutrient Databank System - A tool for handling data from diverse sources. Journal of Food Composition and Analysis (2009) 22(5):433-41.
67. Hilger J, Friedel A, Herr R, Rausch T, Roos F, Wahl DA, et al. A systematic review of vitamin D status in populations worldwide. Br J Nutr (2014) 111(1):23-45.
68. Holick MF, Chen TC. Vitamin D deficiency: a worldwide problem with health consequences. Am J Clin Nutr (2008) 87(4):1080S-6S.
69. Lips P. Worldwide status of vitamin D nutrition. J SteroidBiochem Mol Biol (2010) 121(1-2):297-300.
70. Wahl DA, Cooper C, Ebeling PR, Eggersdorfer M, Hilger J, Hoffmann K, et al. A global representation of vitamin D status in healthy populations. Archives of Osteoporosis (2012):1-18.
71. Lips P. Relative value of 25(OH)D and 1,25(OH)2D measurements. J Bone Miner Res (2007) 22(11):1668-71.
72. Lips P. Vitamin D Deficiency and Secondary Hyperparathyroidism in the Elderly: Consequences for Bone Loss and Fractures and Therapeutic Implications. Endocrine Reviews (2001) 22(4):477-501.
73. Lips P, van Schoor NM, Bravenboer N. Vitamin D-Related Disorders. Primer on the Metabolic Bone Diseases and Disorders of Mineral Metabolism. John Wiley & Sons, Inc. (2013). p. 613-23.
74. Institute of Medicine FaNB. Dietary Reference Intakes for Calcium and Vitamin D. Ross AC, Taylor CL, Yaktine AL, Valle HBD, editors. Washington, DC: The National Academies Press (2011).
75. Ross AC, Manson JE, Abrams SA, Aloia JF, Brannon PM, Clinton SK, et al. The 2011 Report on Dietary Reference Intakes for Calcium and Vitamin D from the Institute of Medicine: What Clinicians Need to Know. Journal of Clinical Endocrinology & Metabolism (2011) 96(1):53-8.
76. Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, treatment, and prevention of vitamin d deficiency: an endocrine society clinical practice guideline. J Clin Endocrinol Metab (2011) 96(7):1911-30.
77. Looker AC, Dawson-Hughes B, Calvo MS, Gunter EW, Sahyoun NR. Serum 25-hydroxyvitamin D status of adolescents and adults in two seasonal subpopulations from NHANES III. Bone (2002) 30(5):771-7.
78. Zadshir A, Tareen N, Pan D, Norris K, Martins D. The prevalence of hypovitaminosis D among US adults: Data from the NHANES III. Ethnicity and Disease (2005) 15(4 SUPPL. 5):S5-97-S5-101.
79. Troesch B, Hoeft B, McBurney M, Eggersdorfer M, Weber P. Dietary surveys indicate vitamin intakes below recommendations are common in representative Western countries. Br J Nutr (2012) 108(4):692-8.
80. Biesalski HK. Hidden Hunger in the Developed World. In: Eggersdorfer M, Kraemer K, Ruel M, van Ameringen M, Biesalski HK, Bloem M, et al., editors. The Road to Good Nutrition, A Global Perspective. first edition ed. Basel: Karger (2013). p. 39-50.
81. Mithal A, Wahl DA, Bonjour JP, Burckhardt P, Dawson-Hughes B, Eisman JA, et al. Global vitamin D status and determinants of hypovitaminosis D. Osteoporos Int (2009) 20(11):1807-20.
82. Lips P, Van Schoor N. Worldwide vitamin D status. In: Feldman D, Pike JW, Adams JS, editors. Vitamin D. 1. 3rd edition ed. London, GB: Elsevier Inc. (2011). p. 947-63.
83. Prentice A. Vitamin D deficiency: A global perspective. Nutrition Reviews (2008) 66(SUPPL.2):S153-S64.
84. Administration FaD. Food Labeling: Health Claims; Calcium and Osteoporosis, and Calcium, Vitamin D, and Osteoporosis. Federal Register(2008). p. 56477-87.
85. Perrine CG, Sharma AJ, Jefferds MED, Serdula MK, Scanlon KS. Adherence to Vitamin D Recommendations Among US Infants. Pediatrics (2010) 125(4):627-32.
86. New reference values for vitamin D. Ann Nutr Metab (2012) 60(4):241-6.
87. Grant WB, Cross HS, Garland CF, Gorham ED, Moan J, Peterlik M, et al. Estimated benefit of increased vitamin D status in reducing the economic burden of disease in western Europe. Progress in Biophysics and Molecular Biology (2009) 99(2-3):104-13.
88. Pfeifer M, Begerow B, Minne HW, Suppan K, Fahrleitner-Pammer A, Dobnig H. Effects of a long-term vitamin D and calcium supplementation on falls and parameters of muscle function in community-dwelling older individuals. Osteoporos Int (2009) 20(2):315-22.
89. Bischoff-Ferrari HA, Dawson-Hughes B, Staehelin HB, Orav JE, Stuck AE, Theiler R, et al. Fall prevention with supplemental and active forms of vitamin D: a meta-analysis of randomised controlled trials. BMJ (2009) 339:b3692.
90. Prince RL, Austin N, Devine A, Dick IM, Bruce D, Zhu K. Effects of ergocalciferol added to calcium on the risk of falls in elderly high-risk women. Arch Intern Med (2008) 168(1):103-8.
91. Broe KE, Chen TC, Weinberg J, Bischoff-Ferrari HA, Holick MF, Kiel DP. A higher dose of vitamin d reduces the risk of falls in nursing home residents: a randomized, multiple-dose study. J Am Geriatr Soc (2007) 55(2):234-9.
92. Flicker L, MacInnis RJ, Stein MS, Scherer SC, Mead KE, Nowson CA, et al. Should older people in residential care receive vitamin D to prevent falls? Results of a randomized trial. J Am Geriatr Soc (2005) 53(11):1881-8.
93. Bischoff HA, Stahelin HB, Dick W, Akos R, Knecht M, Salis C, et al. Effects of vitamin D and calcium supplementation on falls: a randomized controlled trial. J Bone Miner Res (2003) 18(2):343-51.
94. Pfeifer M, Begerow B, Minne HW, Abrams C, Nachtigall D, Hansen C. Effects of a short-term vitamin D and calcium supplementation on body sway and secondary hyperparathyroidism in elderly women. J Bone Miner Res (2000) 15(6):1113-8.
95. Bischoff-Ferrari HA, Dietrich T, Orav EJ, Hu FB, Zhang Y, Karlson EW, et al. Higher 25-hydroxyvitamin D concentrations are associated with better lower-extremity function in both active and inactive persons aged >60 y. American Journal of Clinical Nutrition (2004) 80(3):752-8.
96. Houston DK, Tooze JA, Hausman DB, Johnson MA, Nicklas BJ, Miller ME, et al. Change in 25-hydroxyvitamin D and physical performance in older adults. J Gerontol A Biol Sci Med Sci (2011) 66(4):430-6.
97. Ceglia L, Niramitmahapanya S, da Silva Morais M, Rivas DA, Harris SS, Bischoff-Ferrari H, et al. A randomized study on the effect of vitamin d3 supplementation on skeletal muscle morphology and vitamin d receptor concentration in older women. J Clin Endocrinol Metab (2013) 98(12):E1927-35.
98. Redzic M, Lewis RM, Thomas DT. Relationship between 25-hydoxyvitamin D, muscle strength, and incidence of injury in healthy adults: a systematic review. Nutrition Research (2013) 33(4):251-8.
99. Sohl E, van Schoor NM, de Jongh RT, Visser M, Deeg DJ, Lips P. Vitamin d status is associated with functional limitations and functional decline in older individuals. J Clin Endocrinol Metab (2013) 98(9):E1483-90.
100. Tieland M, Brouwer-Brolsma EM, Nienaber-Rousseau C, van Loon LJ, De Groot LC. Low vitamin D status is associated with reduced muscle mass and impaired physical performance in frail elderly people. Eur J Clin Nutr (2013) 67(10):1050-5.
101. Baeke F, Takiishi T, Korf H, Gysemans C, Mathieu C. Vitamin D: modulator of the immune system. Curr Opin Pharmacol (2010) 10(4):482-96.
102. Schwalfenberg GK. A review of the critical role of vitamin D in the functioning of the immune system and the clinical implications of vitamin D deficiency. Mol Nutr Food Res (2011) 55(1):96-108.
103. Hewison M. An update on vitamin D and human immunity. Clinical Endocrinology (2012) 76(3):315-25.
104. White JH. Vitamin D metabolism and signaling in the immune system. RevEndocr Metab Disord (2012) 13(1):21-9.
105. Berry DJ, Hesketh K, Power C, Hypponen E. Vitamin D status has a linear association with seasonal infections and lung function in British adults. British Journal of Nutrition (2011) 106(09):1433-40.
106. Charan J, Goyal JP, Saxena D, Yadav P. Vitamin D for prevention of respiratory tract infections: A systematic review and meta-analysis. J Pharmacol Pharmacother (2012) 3(4):300-3.
107. Choi C-J, Seo M, Choi W-S, Kim K-S, Youn S-A, Lindsey T, et al. Relationship Between Serum 25-Hydroxyvitamin D and Lung Function Among Korean Adults in Korea National Health and Nutrition Examination Survey (KNHANES), 2008-2010. Journal of Clinical Endocrinology & Metabolism (2013).
108. Hirani V. Associations Between Vitamin D and Self-Reported Respiratory Disease in Older People from a Nationally Representative Population Survey. J Am Geriatr Soc (2013).
109. Salahuddin N, Ali F, Hasan Z, Rao N, Aqeel M, Mahmood F. Vitamin D accelerates clinical recovery from tuberculosis: results of the SUCCINCT Study [Supplementary Cholecalciferol in recovery from tuberculosis]. A randomized, placebo-controlled, clinical trial of vitamin D supplementation in patients with pulmonary tuberculosis'. BMC Infect Dis (2013) 13:22.
110. Nnoaham KE, Clarke A. Low serum vitamin D levels and tuberculosis: A systematic review and meta-analysis. International Journal of Epidemiology (2008) 37(1):113-9.
111. Martineau AR, Timms PM, Bothamley GH, Hanifa Y, Islam K, Claxton AP, et al. High-dose vitamin D3 during intensive-phase antimicrobial treatment of pulmonary tuberculosis: a double-blind randomised controlled trial. The Lancet (2011) 377(9761):242-50.
112. Huaman MA, Sterling TR, Shepherd BE, Fiske CT. 25-Hydroxyvitamin D levels after recovery from tuberculosis: Insights into pathogenesis. Tuberculosis (2014) 94(1):51-4.
113. Coussens AK, Wilkinson RJ, Hanifa Y, Nikolayevskyy V, Elkington PT, Islam K, et al. Vitamin D accelerates resolution of inflammatory responses during tuberculosis treatment. Proc Natl Acad Sci US A (2012) 109(38):15449-54.
114. Mitchell K, Griffiths CJ, Martineau AR. Vitamin D and Tuberculosis. Current Respiratory Medicine Reviews (2011) 7(6):435-9.
115. Solomon AJ, Whitham RH. Multiple sclerosis and vitamin D: a review and recommendations. Curr Neurol Neurosci Rep (2010) 10(5):389-96.
116. Dobson R, Giovannoni G, Ramagopalan S. The month of birth effect in multiple sclerosis: systematic review, metaanalysis and effect of latitude. J Neurol Neurosurg Psychiatry (2013) 84(4):427-32.
117. Cantorna MT. Vitamin D, multiple sclerosis and inflammatory bowel disease. Arch Biochem Biophys (2012) 523(1):103-6.
118. Hypponen E, Laara E, Reunanen A, Jarvelin MR, Virtanen SM. Intake of vitamin D and risk of type 1 diabetes: a birth-cohort study. Lancet (2001) 358(9292):1500-3.
119. Ramos-Lopez E, Jansen T, Ivaskevicius V, Kahles H, Klepzig C, Oldenburg J, et al. Protection from type 1 diabetes by vitamin D receptor haplotypes. Ann N YAcad Sci (2006) 1079:327-34.
120. de Boer IH, Sachs MC, Cleary PA, Hoofnagle AN, Lachin JM, Molitch ME, et al. Circulating Vitamin D Metabolites and Kidney Disease in Type 1 Diabetes. Journal of Clinical Endocrinology & Metabolism (2012) 97(12):4780-8.
121. Dong JY, Zhang WG, Chen JJ, Zhang ZL, Han SF, Qin LQ. Vitamin d intake and risk of type 1 diabetes: a meta-analysis of observational studies. Nutrients (2013) 5(9):3551-62.
122. Van Belle TL, Gysemans C, Mathieu C. Vitamin D and diabetes: the odd couple. Trends Endocrinol Metab (2013) 24(11):561-8.
123. Welsh J. Cellular and molecular effects of vitamin D on carcinogenesis. Arch Biochem Biophys (2012) 523(1):107-14.
124. Rosen CJ, Adams JS, Bikle DD, Black DM, Demay MB, Manson JE, et al. The nonskeletal effects of vitamin D: an Endocrine Society scientific statement. Endocr Rev (2012) 33(3):456-92.
125. Ng K, Meyerhardt JA, Wu K, Feskanich D, Hollis BW, Giovannucci EL, et al. Circulating 25-hydroxyvitamin d levels and survival in patients with colorectal cancer. J Clin Oncol (2008) 26(18):2984-91.
126. Cheng TY, Lacroix AZ, Beresford SA, Goodman GE, Thornquist MD, Zheng Y, et al. Vitamin D intake and lung cancer risk in the Women's Health Initiative. Am J Clin Nutr (2013) 98(4):1002-11.
127. Bischoff-Ferrari HA, Dawson-Hughes B, Stocklin E, Sidelnikov E, Willett WC, Edel JO, et al. Oral supplementation with 25(OH)D3 versus vitamin D3: effects on 25(OH)D levels, lower extremity function, blood pressure, and markers of innate immunity. J Bone Miner Res (2012) 27(1):160-9.
128. Forman JP, Giovannucci E, Holmes MD, Bischoff-Ferrari HA, Tworoger SS, Willett WC, et al. Plasma 25-hydroxyvitamin D levels and risk of incident hypertension. Hypertension (2007) 49(5):1063-9.
129. Gardner DG, Chen S, Glenn DJ, Ni W. Vitamin D and the cardiovascular system. Elsevier Inc. (2011). p. 541-63.
130. Giovannucci E, Liu Y, Hollis BW, Rimm EB. 25-hydroxyvitamin d and risk of myocardial infarction in men: A prospective study. Archives of Internal Medicine (2008) 168(11):1174-80.
131. Karakas M, Thorand B, Zierer A, Huth C, Meisinger C, Roden M, et al. Low Levels of Serum 25-Hydroxyvitamin D Are Associated with Increased Risk of Myocardial Infarction, Especially in Women: Results from the MONICA/KORA Augsburg Case-Cohort Study. Journal of Clinical Endocrinology & Metabolism (2013) 98(1):272-80.
132. Pilz S, Gaksch M, O'Hartaigh B, Tomaschitz A, Marz W. The role of vitamin D deficiency in cardiovascular disease: Where do we stand in 2013? Archives of Toxicology (2013) 87(12):2083-103.
133. Schroten NF, Ruifrok WP, Kleijn L, Dokter MM, Sillje HH, Lambers Heerspink HJ, et al. Short-term vitamin D3 supplementation lowers plasma renin activity in patients with stable chronic heart failure: an open-label, blinded end point, randomized prospective trial (VitD-CHF trial). Am Heart J (2013) 166(2):357-64 e2.
134. Tamez H, Thadhani RI. Vitamin D and hypertension: An update and review. Current Opinion in Nephrology and Hypertension (2012) 21(5):492-9.
135. Tsur A, Feldman BS, Feldhammer I, Hoshen MB, Leibowitz G, Balicer RD. Decreased serum concentrations of 25-hydroxycholecalciferol are associated with increased risk of progression to impaired fasting glucose and diabetes. Diabetes Care (2013) 36(5):1361-7.
136. Schottker B, Herder C, Rothenbacher D, Perna L, Muller H, Brenner H. Serum 25-hydroxyvitamin D levels and incident diabetes mellitus type 2: a competing risk analysis in a large population-based cohort of older adults. Eur J Epidemiol (2013) 28(3):267-75.
137. Pilz S, Kienreich K, Rutters F, de Jongh R, van Ballegooijen AJ, Grubler M, et al. Role of vitamin D in the development of insulin resistance and type 2 diabetes. Curr Diab Rep (2013) 13(2):261-70.
138. Khan H, Kunutsor S, Franco OH, Chowdhury R. Vitamin D, type 2 diabetes and other metabolic outcomes: a systematic review and meta-analysis of prospective studies. Proc Nutr Soc (2013) 72(1):89-97.
139. Gonzalez-Molero I, Rojo-Martlnez G, Morcillo S, Gutierrez-Repiso C, Rubio-Martin E, Almaraz MC, et al. Vitamin D and incidence of diabetes: A prospective cohort study. Clinical Nutrition (2012) (0).
140. Pittas AG, Lau J, Hu FB, Dawson-Hughes B. The role of vitamin D and calcium in type 2 diabetes. A systematic review and meta-analysis. J Clin Endocrinol Metab (2007) 92(6):2017-29.
141. Parekh N, Chappell RJ, Millen AE, Albert DM, Mares JA. Association between Vitamin D and age-related macular degeneration in the third National Health and Nutrition Examination Survey, 1988 through 1994. Archives of Ophthalmology (2007) 125(5):661-9.
142. Millen AE, Voland R, Sondel SA, Parekh N, Horst RL, Wallace RB, et al. Vitamin D status and early age-related macular degeneration in postmenopausal women. Archives of Ophthalmology (2011) 129(4):481-9.
143. Lee V, Rekhi E, Hoh Kam J, Jeffery G. Vitamin D rejuvenates aging eyes by reducing inflammation, clearing amyloid beta and improving visual function. Neurobiol Aging (2012) 33(10):2382-9.
144. Zhao Y, Sun Y, Ji HF, Shen L. Vitamin D levels in Alzheimer's and Parkinson's diseases: A meta-analysis. Nutrition (2013) 29(6):828-32.
145. Eyles DW, Burne THJ, McGrath JJ. Vitamin D, effects on brain development, adult brain function and the links between low levels of vitamin D and neuropsychiatric disease. Frontiers in Neuroendocrinology (2013) 34(1):47-64.
146. Buell JS, Dawson-Hughes B. Vitamin D and neurocognitive dysfunction: preventing "D"ecline? Mol Aspects Med (2008) 29(6):415-22.
147. Annweiler C, Rolland Y, Schott AM, Blain H, Vellas B, Herrmann FR, et al. Higher Vitamin D Dietary Intake Is Associated With Lower Risk of Alzheimer's Disease: A 7-Year Follow-up. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences (2012) 67(11):1205-11.
148. Carlberg C, Campbell MJ. Vitamin D receptor signaling mechanisms: integrated actions of a well-defined transcription factor. Steroids (2013) 78(2):127-36.
149. Ames BN. Low micronutrient intake may accelerate the degenerative diseases of aging through allocation of scarce micronutrients by triage. Proc Natl Acad Sci US A (2006) 103(47):17589-94.
150. McCann JC, Ames BN. Vitamin K, an example of triage theory: is micronutrient inadequacy linked to diseases of aging? Am J Clin Nutr (2009) 90(4):889-907.
151. Norman AW, Ishizuka S, Okamura WH. Ligands for the vitamin D endocrine system: different shapes function as agonists and antagonists for genomic and rapid response receptors or as a ligand for the plasma vitamin D binding protein. J Steroid Biochem Mol Biol (2001) 76(1-5):49-59.
152. Bouillon R, Okamura WH, Norman AW. Structure-function relationships in the vitamin D endocrine system. Endocr Rev (1995) 16(2):200-57.
153. Norman AW, Okamura WH, Bishop JE, Henry HL. Update on biological actions of 1alpha,25(OH)2-vitamin D3 (rapid effects) and 24R,25(OH)2-vitamin D3. Mol Cell Endocrinol (2002) 197(1-2):1-13.
154. Bouillon R, Lieben L, Mathieu C, Verstuyf A, Carmeliet G. Vitamin D action: lessons from VDR and Cyp27b1 null mice. Pediatric endocrinology reviews : PER (2013) 10 Suppl 2:354-66.
155. Carlberg C, Seuter S, de Mello VD, Schwab U, Voutilainen S, Pulkki K, et al. Primary vitamin d target genes allow a categorization of possible benefits of vitamin D3 supplementation. PLoS One (2013) 8(7):e71042.
156. Hossein-Nezhad A, Spira A, Holick MF. Influence of vitamin d status and vitamin d3 supplementation on genome wide expression of white blood cells: a randomized double-blind clinical trial. PLoS One (2013) 8(3):e58725.
157. Bosse Y, Maghni K, Hudson TJ. 1 a,25-dihydroxy-vitamin D3 stimulation of bronchial smooth muscle cells induces autocrine, contractility, and remodeling processes. Physiological Genomics (2007) 29(2):161-8.
158. Tarroni P, Villa I, Mrak E, Zolezzi F, Mattioli M, Gattuso C, et al. Microarray analysis of 1,25(OH) 2D 3 regulated gene expression in human primary osteoblasts. Journal of Cellular Biochemistry (2012) 113(2):640-9.
159. Carlberg C, Seuter S, Heikkinen S. The first genome-wide view of vitamin D receptor locations and their mechanistic implications. Anticancer Res (2012) 32(1):271-82.
- '' In VitaminDWiki Vitamin D Receptor locations – Dec 2012''
160. Heikkinen S, Vaisanen S, Pehkonen P, Seuter S, Benes V, Carlberg C. Nuclear hormone 1alpha,25-dihydroxyvitamin D3 elicits a genome-wide shift in the locations of VDR chromatin occupancy. Nucleic Acids Res (2011) 39(21):9181-93.
161. Pike JW, Lee SM, Meyer MB. Regulation of gene expression by 1,25-dihydroxyvitamin D3 in bone cells: exploiting new approaches and defining new mechanisms. BoneKEy Rep (2014) 3.
162. Ramagopalan SV, Heger A, Berlanga AJ, Maugeri NJ, Lincoln MR, Burrell A, et al. A ChIP-seq defined genome-wide map of vitamin D receptor binding: Associations with disease and evolution. Genome Research (2010) 20(10):1352-60.
163. Haslberger A, Varga F, Karlic H. Recursive causality in evolution: A model for epigenetic mechanisms in cancer development. Medical Hypotheses (2006) 67(6):1448-54.
164. Karlic H, Varga F. Impact of vitamin D metabolism on clinical epigenetics. ClinicalEpigenetics (2011) 2(1):55-61.
165. Sundar IK, Rahman I. Vitamin D and susceptibility of chronic lung diseases: Role of epigenetics. Frontiers in Pharmacology (2011) AUG.
166. Burrell AM, Handel AE, Ramagopalan SV, Ebers GC, Morahan JM. Epigenetic mechanisms in multiple sclerosis and the major histocompatibility complex (MHC). Discovery medicine (2011) 11(58):187-96.
167. Cashman KD. The vitamin D RDA for African American adults: higher than that for white persons? The American Journal of Clinical Nutrition (2014) 99(3):427-8.
168. Ng K, Scott JB, Drake BF, Chan AT, Hollis BW, Chandler PD, et al. Dose response to vitamin D supplementation in African Americans: results of a 4-arm, randomized, placebo-controlled trial. The American Journal of Clinical Nutrition (2014) 99(3):587-98.
169. Nesby-O'Dell S, Scanlon KS, Cogswell ME, Gillespie C, Hollis BW, Looker AC, et al. Hypovitaminosis D prevalence and determinants among African American and white women of reproductive age: third National Health and Nutrition Examination Survey, 1988-1994. The American Journal of Clinical Nutrition (2002) 76(1):187-92.
170. Dastani Z, Li R, Richards B. Genetic regulation of vitamin D levels. Calcif Tissue Int (2013) 92(2):106-17.
171. Aminullah Bhuiyan AKM, Ratnayake WMN, Ackman RG. Nutritional Composition of Raw and Smoked Atlantic Mackerel (Scomber scombrus): Oil- and Water-Soluble Vitamins. Journal of Food Composition and Analysis (1993) 6(2):172-84.
172. Wagner D, Sidhom G, Whiting SJ, Rousseau D, Vieth R. The bioavailability of vitamin D from fortified cheeses and supplements is equivalent in adults. J Nutr (2008) 138(7):1365-71.
173. Wacker M, Holick M. Vitamin D — Effects on Skeletal and Extraskeletal Health and the Need for Supplementation. Nutrients (2013) 5(1):111-48.
174. Tippetts M, Martini S, Brothersen C, McMahon DJ. Fortification of cheese with vitamin D3 using dairy protein emulsions as delivery systems. Journal of dairy science (2012) 95(9):4768-74.
PDF is attached at the bottom of this page
See also VitaminDWiki
Search VitaminDWiki for DSM 587 hits March 2020
DSM - holder of many vitamin D patents - to make deficiency map - Dec 2010
Is HyD (25(OH)D) a better form of vitamin D for some animals and maybe humans with liver problems a DSM product
Patent for combination of vitamin D3 and calcifediol– Sept 2009
143 papers referenced this study by March 2020
Short url = http://is.gd/DSM2014
