Vitamin D deficiency in Middle East and North Africa
Hypovitaminosis D in the Middle East and North Africa: Prevalence, risk factors and impact on outcomes
📄 Download the PDF from VitaminDWiki
XML File
 Full Text XML
Full Text XML
- 387.24 KB XML Document
![]() This is an open access article.
This is an open access article.
[![]() Print this page ][
Print this page ][![]() Email this page ]
Email this page ]
---Article Citation
{ANAME()}showfullcitation![]() FULL CITATION{ANAME}
FULL CITATION{ANAME}
![]() Volume 5, Issue 2 April/May/June 2013 Dermato-Endocrinology
Volume 5, Issue 2 April/May/June 2013 Dermato-Endocrinology
http://dx.doi.org/10.4161/derm.25111
Keywords : genetics polymorphisms, infections, musculoskeletal outcomes, osteomalacia, pleotropic, policy, prevalence, region specific guidelines, rickets, risk factors
Authors : Darina Bassil, Maya Rahme, Maha Hoteit and Ghada El-Hajj Fuleihan
Abstract:
Background: The Middle East and North Africa (MENA) region registers some of the highest rates of hypovitaminosis D worldwide.
Aim: We systematically reviewed the prevalence of hypovitaminosis D, rickets and osteomalacia, their predictors and impact on major outcomes, in the region.
Methods: Medline, Pubmed and Embase search engines, entering keywords and concepts, combined with individual countries of interest, were used. Search was limited years 2000–2012; and review articles were used for the period preceding year 2000.
Results: Rickets and osteomalacia still occur in this sunny region. Hypovitaminosis D prevails, with rates varying 30–90%, considering a desirable serum 25 hydroxy-vitamin D [25(OH)D] of 20 ng/ml. Advancing age, female gender, multi-parity, clothing style, season, socio-economic status and urban living are recognized predictors of hypovitaminosis D in adults. Prolonged breastfeeding without vitamin D supplementation and low dietary calcium intake are the recognized risk factors for rickets and hypovitaminosis D in children.. Associations with pain score and disease activity in rheumatologic disorders, viral load and interleukins in hepatitis C, BMI, lipids and insulin sensitivity, blood pressure, heart failure and mortality are described. Sun exposure in adults decreased prevalence of metabolic syndrome in one study. Few randomized vitamin D trials revealed that the majority of mothers or children failed to achieve a desirable 25(OH)D level, even with doses by far exceeding current recommendations. A trial in adolescent girls reveals substantial bone and lean mass increments.
Conclusion: Hypovitaminosis D is prevalent in MENA. The lack of populations based studies, gaps in studies in infants, pre-pubertal children and pregnant women, hinder the development of region specific guidelines and constitute a major obstacle to impact this chronic and most often subclinical disease.
Received: January 15, 2013; Accepted: May 21, 2013; Published Online: April 1, 2013
Provisional Full-Text corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions containing any author galley corrections will be made available soon. When Provisional Full Text is displayed, it will always be open access.
Full Text
![]()
Introduction
Vitamin D is a steroid hormone that modulates a wide range of molecular and cellular functions, most readily recognized are its beneficial effects on musculoskeletal parameters. Rickets and osteomalacia represent short-term latency manifestation of vitamin D deficiency and osteoporosis the long-term latency manifestation of more subtle chronic deficiencies.1,2 An increasing body of evidence also supports non-traditional, extra-skeletal, benefits of vitamin D on the immune system, fuel metabolism, cardiovascular system diseases and cancer.2-5 In addition, associations with decreased mortality have been described.6
While rickets is almost eradicated in western populations, its prevalence remains unacceptably high in Asia, Africa and the Middle East and resurgence is also registered in ethnic minority groups in some Northern European countries.7,8 Conversely, hypovitaminosis D is prevalent worldwide, but is again most notable in Asia and surprisingly the Middle East, despite its plentiful sunshine.1,3 Although such observations stem mostly from non-population based studies, they have for the most part been consistent across reviews over the last decade.9-14 Such findings are explained by the prevalence of specific risk factors for hypovitaminosis D in this region. These include the classic predictors, in addition to conservative concealed clothing style in women in general and in men from gulf countries in particular. The, lack of governmental regulation for food fortification with vitamin D in the region has also been noted
The aim of this paper is to systematically review the prevalence of rickets, osteomalacia and hypovitaminosis D, in the Middle East and North Africa (MENA) region, evaluate relevant predictors and describe the impact of low vitamin D status on relevant outcomes in studies from the region. Implications of the vitamin D guidelines issued by the Institute of Medicine and the Endocrine Society in 2011 will be put in perspective taking into consideration the status of vitamin D in the MENA.15,16
Methods
Definition of Middle East North Africa region
According to the UNICEF, the MENA is composed of 20 countries: Algeria, Bahrain, Lebanon, Egypt, Djibouti, Syria, Occupied Palestinian Territory, Iran, Iraq, Yemen, Tunisia, Sudan, UAE, Saudi Arabia, Jordan, Oman, Libya, Kuwait, Morocco and Qatar.17 According to the World Bank, countries in the Middle East include United Arab Emirates (UAE), Syria, Qatar, Lebanon, Kuwait, Saudi Arabia, Jordan, Iraq, Iran, Yemen, Oman and Bahrain; and in North Africa Algeria, Egypt, Libya, Morocco, Tunisia and Sudan.18
Literature search methodology
A systematic review of the literature was implemented targeting the following keywords: vitamin D, vitamin D deficiency or rickets, osteomalacia, conducted separately for each of the individual countries listed above for the Middle East North Africa region (MENA). Each of these keywords were searched on OVID Medline as MeSH terms and also as synonyms or related terms to achieve a comprehensive literature review. The OVID Medline interface was utilized as it allows searching for related MeSH-terms, explode functions, keyword searching in title, abstract and subject headings, adjacency and publication types, in addition to Boolean operators (and, or ) and truncation, to identify as many relevant articles as possible. OVID Medline search was conducted from year 1946 until the third week of September, 2012, then tailored to years 2000-Dec 2012 (see Appendix S1). The exact procedure used for every country of the MENA region is detailed in Appendix S1. A PubMed search was also done using the key terms for each of the countries of interest to capture the most recent publications entered into PubMed, not yet indexed in OVID Medline. The following search was entered for each of the countries of the MENA region, the example for Lebanon was: (vitamin D OR rickets OR osteomalacia) AND (Lebanon OR Lebanese). The Embase database was also used to capture a more comprehensive view on studies done in the Middle Eastern region. We also used data compiled in the 2011 International Osteoporosis Foundation (IOF) Middle East Africa Osteoporosis Audit,19 and additional studies and reviews detailed in the papers retrieved and available in authors' libraries.
Search yield and manuscripts reviewed
A total of 2323 hits were identified from Embase, PubMed and OVID Medline for all the countries, with the exception of Djibouti and Libya, that had no hits. Three screening phases were implemented for identifying relevant articles. The first phase involved screening the titles and abstracts and resulted in 362 manuscripts between 1946 and 2012. The second phase involved deleting studies published before year 2000, thus resulting in 295 papers. The third phase involved retrieving and reviewing the full-text for all 295 papers, of which only 176 where retrievable and these were scored for quality measures based on specific criteria: type of the study (population based yes or no), sample size (n > 100 yes or no), whether the vitamin D assay was specified (yes or no), whether predictors were specified (yes or no) and exclusion criteria were specified (yes/no). Each criterion received a score of 1 if answered positively and articles were sorted into four quality categories: very good for score ≥ 4/5, good for score 3/5, fair for score 2/5 or poor if score 1/5. The large majority of the 295 retrieved papers were from Iran (n = 86), Saudi Arabia (n = 47), UAE (n = 21), Egypt (n = 20), followed by Lebanon, Kuwait, Jordan, Qatar and Morocco Jordan (n = 11−16 each) and Yemen, Tunisia, Iraq, Bahrain, Oman (n = 1−5 each). Out of the total of 176 studies, 109 studies characterized as of very good or good quality are detailed in this review.
For association and intervention studies, as well as reports on rickets or osteomalacia, rating score was not applied and all relevant studies were examined. Titles and abstracts for reviews on osteomalacia retrieved prior to 2000 (n = 338) were screened and all relevant reviews in the MENA, in addition to those on hypovitaminosis D9-11 were used to summarize information for the period preceding year 2000.
Interpretation of results from papers on vitamin D and cut-offs used to determine desirable levels
Serum 25 hydroxy-vitamin D [25(OH)D] 25(OH)D level is the best indicator of vitamin D nutritional status. The importance of variations in serum 25(OH)D assays and the lack of their standardization has been recently recognized.20,21 Furthermore, there is no universal agreement on what constitutes a desirable level to optimize musculoskeletal health in elderly Caucasians,15,16 let alone optimal levels across the lifecycle, for other ethnic groups or targeting other major chronic diseases outcomes. Findings from any paper on vitamin D, have to therefore be interpreted in this context. Results for serum 25(OH)D are reported in ng/ml, to convert to from ng/ml to nmol/L multiply the value by 2.5.
Magnitude of the Problem and Predictors of Low Vitamin D Status
Rickets and osteomalacia
Rickets and osteomalacia are conditions that can result from severe vitamin D deficiency, hypophosphatemia or mineralization defects. This paper focuses on those resulting from vitamin D deficiency, best captured by measurement of serum 25 hydroxy-vitamin D [25(OH)D] level. Rickets is a childhood condition caused by serious vitamin D deficiency and is characterized by soft and weak bones, slowed growth and skeletal development and convulsions. Rickets, by definition, is a disorder which begins in childhood. If this problem occurs later in life it is known as osteomalacia. In a review on rickets worldwide, covering 30 y from 1968–1998, Prentice et al. noted that Asia, the Middle East and Africa, a region spanning latitudes from 5° to 40° North, registered the highest rates. The reported rates for clinical or radiological rickets were 70% in Mongolia (1998), 66% in Tibet (1994), 44% in Ethiopia (1987), 27% in Yemen (1987), 15% in Iran (1975), 10% in Turkey (1994) and 9% in Nigeria (1998), compared with 1.6% in Manchester minorities mostly Pakistanis.7,8 Similarly, a review by our group underscored the lack of adequate population based studies and reported rates to be 10–100 folds higher than those in western populations.11 These include a prevalence of 27% in children < 5 y in North Yemen, 10% in a field sample from rural Egypt, 1% Kuwait if < 2yrs (1981−86), 0.5% of Saudis < 2 y (1997–1999) and 6% in Turkey in 1998 down to < 1% in 2008, the latter following a National Vitamin D supplementation program.11 Rickets accounted for a substantial number of pediatric hospital admissions, 50% of children hospitalized with pneumonia in Yemen, 11% of infant’s admissions with acute illness in Jordan, 6.5% of newborn admissions in Kuwait and 1.8% of pediatric admissions in 1986–88 in Saudi Arabia.9,11 Non-skeletal manifestations of rickets included convulsions in 4−79% of patients, acute chest infections and asthmatic bronchitis in 66% of 500 cases in Saudi Arabia, broncho-pneumonia in 43% of 200 Iranian children and 44% of 250 children from Kuwait. An acute infection or respiratory diseases were the presenting manifestation in 20–60% of cases presenting with rickets in smaller studies from Turkey, Egypt, Jordan and Saudi Arabia, while gastroenteritis accounted for 8–56% of reasons for admission in hospitals in Middle East. Dilated cardiomyopathy was reported in three infants from Asia, one from Turkey and two from UAE.11 Predictors of rickets included, low maternal vitamin D status, prolonged breast feeding, low socioeconomic status (SES), educational level and crowding. It has been recognized that primary vitamin D deficiency does not adequately describe nutritional rickets explained in some African, Middle Eastern and Asian countries and that concomitant low calcium intake and possibly disturbances of phosphate metabolism, renal compromise and iron deficiency may also play an important role in the pathophysiology of the disease.9
In our current search, we retrieved 13 publications on rickets, but only 8 were on nutritional rickets. Case series were published in Iran, Saudi Arabia, Kuwait, United Arab Emirates, Qatar and Egypt, with sample sizes ranging 21 to 283 subjects and age ranging from infants all the way to adolescents, with the majority being infants and toddlers.22-30 In a study of 98 rachitic children from Egypt and Turkey, mean age 11.7 y, mean 25(OH)D was 14.3 (± 11.2) ng/ml in patients from Egypt and 10.1 (± 7.9) ng/ml in Turkey, compared with mean levels above 20 ng/ml in controls, underscoring a combined etiology that includes insufficient calcium intake, in the pathophysiology of rickets and possibly other factors, especially in Egypt.29 Similarly, in a small study of 16 Emirati children from Abu Dhabi (24°), nutritional rickets from vitamin D deficiency was reported in eight subjects, with a mean 25(OH)D of 7(± 2) ng/ml and a mixed etiology with combined calcium deficiency in the rest with a mean 25(OH)D of 17 (± 8) ng/ml.31 Common risk factors included multiparity, prolonged breast feeding, delayed intake of semi-solids, maternal education and complete wrapping of the child.28
Osteomalacia, the adult manifestation of rickets, may be asymptomatic and go undetected, thus making true prevalence studies very difficult. The diagnosis is usually made on basis of the classic clinical profile of bone pain, fractures and proximal myopathy, combined with confirmatory laboratory tests including a low 25(OH)D, usually below 5–10 ng/ml (25–50 nmol/L), low serum calcium and phosphate levels and a high alkaline level . However, the patient may not have hypocalcemia due to correction of serum calcium level from secondary hyperparathyroidism. Moreover, hypovitaminosis D can be misdiagnosed as fibromyalgia, chronic fatigue syndrome or simply depression.32,33 The above 25(OH)D cut-offs are not diagnostic of osteomalacia, as demonstrated in a study in Caucasian subjects.34 We are unaware of such studies in MENA. Convulsions and hypocalcemic cardiomyopathy are also very rare manifestation of severe hypocalcemia from rickets or any other causes.35 To-date, most publications on osteomalacia are limited to case reports or case series, made on basis of a clinical diagnosis.36,37 The condition can mimic osteoporosis, with severe bone demineralization due to severe vitamin D deficiency, hyperparathyroidism, vertebral compression fractures, T-scores ranging from -5 to -4, with normalization after aggressive vitamin D therapy.
Hypovitaminosis D
Despite limitations caused by the lack of methodological standardization, in general, a serum 25(OH)D at concentration less than25 nmol/L (10 ng/mL) is a useful marker of the risk of clinical deficiency, but the terminology and cut-offs used to define less than desirable vitamin D status is controversial. It includes terms such as insufficiency, inadequate level, sub-optimal level and hypovitaminosis D and may result in subclinical conditions with chronic latent manifestations, the most recognized of which is osteoporosis. The 25(OH)D cut-offs to define this condition vary and have most recently been framed by the 2011 desirable levels of the Institute of Medicine Report set at 20 ng/ml (50 nmol/L),16 and the Endocrine Society Guidelines set at 30 ng/ml (75 nmol/L).15 Most studies have however predated these recommendations and used variable cut-offs.
In a review conducted by the nutrition working group of the IOF, hypovitaminosis defined as 25 (OH)D level below 30 ng/ml (75 nmol/L) was prevalent in all regions of the world, whereas levels below 10 ng/ml (25 nmol/L) were most common in South Asia and the Middle East. Predictors of low 25(OH)D levels included older age, female sex, higher latitude, winter season, darker skin pigmentation, less sun exposure, dietary habits and absence of vitamin D fortification.12 The high prevalence of hypovitaminosis D worldwide, and not only in risk groups, was again underscored in a recent review, Asia and the Middle East being at particular risk, albeit with high variability between studies within the ME.13,14 The latest attempt at a global representation of vitamin D status in healthy populations, commented on the lack of representative studies, large gaps in information in children, adolescents worldwide and in adults in Central and South America, as well as Africa.14
One of the original studies on hypovitaminosis D in the Middle East was conducted in apparently healthy 104 male Saudi university students, who had a mean 25(OH)D of 12.8 (± 6.3)ng/ml with 35% < 10 ng/ml38. The high prevalence of hypovitaminosis D in Saudi subjects has been validated in numerous studies. Table 1 summarizes key findings from studies of good or very good quality retrieved from our search, for adults from the MENA region.39-81 The overwhelming majority of studies revealed 25(OH)D levels in the low teens [25(OH)D 10−15 ng/ml], even considering population-based studies. Consistent predictors across these studies for lower values were age, albeit with differing findings, some studies showing older age to be a risk factor,57,67,69 while others point to younger age,41,42,77 female gender in adults41,61,63,72,75,82 and children,83-89winter season, sunlight exposure and veiling,40,41,44,56,60,63,66,75,78,81,90,92except in some studies from gulf countries where summer registers lowest values in studies from the United Arab Emirates,75,77 pollution,43 low calcium or vitamin D dietary intake,67,77,80,81,90,92 and exclusive breast feeding in infants88. Other predictors included high BMI and /or increased adiposity,39,60,66-68,72,93 and lower SES status or educational level44,60,64,68,80,83.The impact of menopause was not consistent across studies, whereas premenopausal women had higher levels in the study from Saudi Arabia,67 the opposite was found in UAE.77Table 1 details studies conducted in adults, Table 2 in children, Table 3 in mothers-neonates, by country, and highlights are underscored here-in.
* Table 1. *Overview of Studies on 25(OH) D Values in Adults in Middle East and North Africa
| Country | Author/Yr | Sampling Method | ||||
| City (Latitude) | N Gender/ Age | Exclusion criteria specified | Assay type/ Manufacturer | Season Yr | Predictors for low 25(OH)D | 25(OH)D Level Mean ng/ml % below cut-off |
| Middle East | ||||||
| Iran | Baradaran et al. 201239 | Hospital based | ||||
| Iran (32°N) | 259 ♀♂ | |||||
| 20–64 y | Yes | EIA/IDS | NA 2010 | High adiposity, | ||
| high BMI | 12 ± 6 | |||||
| Median: 10 |
| Kashi et al. 201140 | Telephone population based Sari (37°N) | 232 ♀,118♂ | | 11–69 y | Yes | ELISA/DRG | End of summer | | and winter NA | High humidity climate, winter | Summer: 13.4 ± 13 | | Winter: 11.7 ± 11
| Hovsepian et al. 201141 | Outpatient clinic | | Isfahan (32°N) | 243 ♂, 868 ♀ | | 20–80 y | Yes | RIA/ Biosource | Autumn/ Winter-Spring/ Summer NA | Young age, women | Median Spring: 21 (2–300) | | Median Summer: 18 (3–208) | | Median Autumn: 19 (1.5–425) | | Median Winter: 17 (2–281) | | 27% < 10, 24% 10–20, 20% 20–30
| Kaykhaei et al. 201042 | Population based | | Zahedan (30°N) | 431 ♂, 562♀ | | 20–88 y | No | CIA/ DiaSorin | June -Aug 2008 | Younger age | 13.8 | | 95% < 30 85% < 20 | | 10% 20–30 5% 30–150
| Hosseinpanah et al. 201043 | Clustered sampling Tehran (35° N), | | Ghazvin (36°N) | 200♀ | | 20- 55 y | Yes | EIA/DRG | Sept 2007 | Air pollution | Ghazvinian: ♀ 18 ± 11 | | Tehranian: ♀ 13 ± 7 | | Tehranian: 36% < 10 54% 10–20 | | Ghazvinian: 31% < 10 32% 10–20
| Maddah et al. 200944 | Clustered sampling | | Guilan (37°N) | 427 ♀ Urban | | 219 ♀ Rural | | 51–92 y | No | Commercial kit/ BioSource | Oct 2004-Feb 2005 | Low education, urban living | ♀ Urban: 18.5 ± 13.5 | | ♀ Rural: 22.9 ± 13.8
| Masoompour et al. 200845 | Clustered sampling | | Shiraz (30°N) | 520 ♂ | | 20–74 y | Yes | IRMA/IDS | Jan-Mar 2001 | NA | 14 ± 6.8 | | 34% ≤ 10
| Hosseinpanah et al. 200846 | Population based study Tehran (35°N) | 245 p.m.♀ | | 40–80 y | Yes | RIA/IDS | NA | NA | 5% < 10 38% 10–20 | | 43% < 20 25% > 32
| Hashemipour et al. 200647 | Clustered sampling | | Tehran (35°N) | 1210 ♂♀ | | 20–69 y | Yes | RIA/IDS | NA | NA | 12.9 ± 16.5 | | 9% ≤ 5 56% 5–10
| Rassouli et al. 200148 | Densitometry center Tehran (35°N) | 73 p.m.♀ | | 49–63 y | Yes | HPLC | Feb-June 2000 | NA | Winter: 13.3 ± 5.0 | | Spring: 18.3 ± 12 | | 36% < 12 | | Occupied Palestine/Israel | Saliba et al. 201249 | Population Based CHF covers > 50% of Israeli population (31°N) | 198,834♀♂ | | Median 60 y | Yes | CIA/ Diasorin | Jan-Dec 2009 | Female gender, winter, adults, Arabs > Jews | Summer-Autumn: 22.52 ± 9.8 | | Winter-Spring: 18.72 ± 9.4 | | 14% < 10 31% < 15 | | 50% < 20 16% > 30
| Saliba et al. 201250 | Population Based | 2571♂, 6310♀ | | 56.1 ± 17.6 y (1st test) | | 57.6 ± 17.7 y (Last test) | Yes | CIA / Diasorin | Jan 2008-Sep 2011 | Female gender | First test: 20.68 ± 9.6 50% < 20 | | Last test: 22.68 ± 9.88 41% < 20 | | * First and last test done in the same month | | Middle East
| Saliba et al. 201251 | Population Based | 182, 152 ♀♂ | | VitD ≤ 13: 59.4 ± 17.4yrs | | VitD13–20: 61 ± 16.1 y | | VitD20–26: 61.1 ± 16 y | | VitD > 26: 59.9 ± 17.1yrs | No | CIA/ Diasorin | Jan 2008 - Dec 2009 | History of diabetes | | History of Cardiovascular disease | 25% ≤ 13ng/ml, mean 9.3 ± 2.7 | | 25% 13–20 ng/ml, mean 16.8 ± 1.8 | | 25% 20–26ng/ml, mean 22.8 ± 1.8 | | 25% > 26ng/ml, mean 32.6 ± 6.4 |
| Tsur et al. | |||||
| 201152 | Institution based Jerusalem (31.7°N) | 74♂ students | |||
| (A) Ultra-orthodox Indoors 20.1 ± 0.6yrs | |||||
| (B) Ultra-Orthodox Outdoors 33.0 ± 4.2yrs | |||||
| (C) Religious 19 ± 2.0yrs | Yes | RIA /DLS | Mar-Apr NA | Low sun exposure, traditional clothing | (A) 8.9 ± 3.6 100% < 20 65% < 10 |
| (B) 10.2 ± 5.7 91% < 20 65% < 10 | |||||
| (C) 21.7 ± 10.4 51% < 20 12% < 10 |
| Saliba et al. 2011 53 | Population Based | | (31°N) | 19,172 ♂♀ | | 63.7 ± 15.5 y | | Normal:19,172 | | Renal failure:5449 | No | CIA/ Diasorin | Jan-Dec 2009 | Renal Failure | Renal Failure: 22.8 ± 11 | | Normal Function: 25.32 ± 10.64
| Steinvil et al. 201154 | Retrospective | | Population based (31°N) | 26,699♀ 55 ± 15 y | | 8175♂ 55 ± 17 y | No | RIA /Diasorin | Jan-Dec 2001–2008 | Low sun exposure | ♂ 23.22 ± 10.1 79% < 30 | | ♀ 22.7 ± 9.9 78% < 30
| Oren et al. | | 201055 | NA | | (31°N) | 100♀, 95♂ | | 50yrs | No | CIA/ Diasorin | Feb-Jan NA | Older Age, Ashkenazi > Sephardic > Arab | 22.9 ± 10.1 | | 78% < 30 | | Jordan | Nichols et al. 201256 | National micronutrient survey | | Jordan (31°N) | 2032 ♂ 15–49 y | No | LC-MS/MS | Mar-Apr 2010 | Urban living, veiling | Median: 11 96% < 20 60% < 12 | | No cover n = 98 40% < 12 | | Scarf/hijab n = 1842 62% < 12 | | Niqab (full) n = 73 68% < 12
| Batieha et al. 201157 | National population based | | Jordan (31°N) | 1128 ♂, 3462 ♀ | | > 18 y | No | RIA/ Biosource | July–Oct-Nov 2009 | Older age, middle and south region, winter season, low altitude, sunscreen use, indoor work, urban, veiling | ♂ 73.3 ± 29.3 | | 94% ≥ 30 4% 20–29.9 2% < 20 | | ♀ 39.8 ± 20.7 | | 63% ≥ 30 23% 20–29.9 14% < 20
| Mallah et al. 201158 | NA | | Jordan (31°N) | 201 ♀, 99 ♂ | | 29–32 y | No | ELISA/IDS | November 2010 | Veiling | ♂18 ± 4 ♀ 12 ± 5 | | Western Style: 16 ± 3 | | Hijab: 12.5 ± 2.5 | | Niqab: 11.4 ± 1.52
| Mishal 200159 | Hospital based | | Jordan (31°N) | 131 ♀, 23 ♂ | | 18- 45 y | Yes | RIA/Diasorin | Summer: July–Sep Winter: Jan–Mar NA | Winter, veiling | 3% < 5 60% 5–12 | | Both seasons: 62% < 12 | | Summer: 50% < 12 | | Winter: 73% < 12 | | Middle East | | Lebanon | Gannaje-Yared et al. 200960 | Hospital based | | Lebanon (33°N) | 151 Christians, | | 100 Muslims ♀ | | 50–87 y | Yes | CIA/Nichols | July –Aug 2004 | | Feb-Mar 2005 | Dress code covering the arms, high BMI, | | low education | 19·5 ± 9·8
| Arabi et al. 200661-201062 | Population based | | Beirut (34°N) | 286♀,157 ♂ | | 65–85 y | | Mean 73 y | Yes | RIA/ IDS | Nov 2002-Mar2003 | Female gender | 11.4 ± 4.9 | | ♀ 55% < 10 | | ♂ 37% < 10
| Gannaje-Yared et al. 200063 | Community centers | | Bekaa, Beirut (34°N) | 99 ♂, 217 Prem♀ | | 30–50 y | Yes | RIA/ Incstar | | Veiling, | | ♀ rural living, ♂urban living, | | low vit D intake | 9.7 ± 7.1 | | 31% (42% ♀, 7% ♂) < 5 | | 73% (84%♀, 49% ♂) < 12 | | 80% (89% ♀, 51% ♂) < 15 | | Saudi Arabia | Ardawi et al. 201264 | Population based | | Health Care Centers | | Jeddah (22°N) | 834 ♂ 20–74yrs | | 42.1 ± 13.9 y | Yes | CIA/ Liaison | Jun 2008-Jun 2009 | Heavy weight, summer, smoking, no education, sedentary lifestyle, low Vit D supplementation, low sun exposure | Total: 11.6 ± 6.45 | | < 50 y: 12.5 ± 7.01 | | ≥ 50yrs: 10.7 ± 5.992 | | 88% < 20 10% ≥ 20–30
| El Shafie et al. 201265 | Healthcare Center | | Riyadh (25°N) | 50 married couples | | ♂40.1 ± 7.4 y | | ♀30.6 ± 6.8yrs | Yes | ECLIA/Roche | Dec 2010 - Jan 2011 | Male gender, high physical activity, milk intake | ♀ 8.5 ± 3.9 70% < 10 98% < 20 | | ♂ 12.2 ± 5.5 40% < 10 92% < 20
| Kanan et al. 201266 | Retrospective | | out-patient clinics | | Riyadh (25°N) | 1556 ♀ | | Summer | | 44.4 ± 16.1 y | | Winter | | 46.1 ± 15.9 y | Yes | HPLC | Jan- Dec 2009 | Low latitude, veiling, | | sun avoidance | 13.3 ± 0.7 Prem Summer 80% < 20 | | 11.4 ± 0.5 Prem Winter 85% < 20 | | 17.7 ± 0.9 p.m. Summer 68% < 20 | | 14.5 ± 0.6 p.m. Winter 76% < 20
| Ardawi et al. | | 201167 | Population based | | Health Care centers | | Jeddah (22°N) | 1,172 healthy ♀ | | 50.9 ± 12.6 y | Yes | CIA/ Liaison | Jun 2008-Jun 2009 | Older age, high BMI, low sun exposure, poor dietary, | | low vit D supplementation, high WHR | 17.18 ± 12.19 (Prem) | | 13.32 ± 9.94 (PM) | | 11% (6% Prem 14% PM) < 5 | | 46% (38% Prem 51% PM) < 10 | | 34% (34% Prem 34% PM) 10–20 | | 9% (11% Prem 7% PM) 20–30 | | 12% (16% Prem 8% PM) ≥ 30
| Alissa et al. | | 201168 | Hospital based | | Jeddah (22°N) | 122 p.m.♀ | | 46–70 y | Yes | RIA/ Diasorin | NA | High SES, | | heavy weight, low activity | 9.6 ± 0.47 (Controls) 100% < 20 | | 12.7 ± 1.06 (Osteopenic) 97% < 20 | | Middle East
| Sadat-Ali et al. | | 201169 | Hospital based | | Al-Khobar (26°N) | 400 Peak Bone Mass age group and ≥ 50yrs | Yes | RIA / Wallac | Feb -May 2008 | Older age | PBM age group | | 11% ♀ 10% ♂ < 20 | | 19% ♀ 19% ♂ 20–30 | | 70% ♀ 71% ♂ > 30 | | ≥ 50 y | | 19% ♀ 12% ♂ < 20 | | 36% ♀ 25% ♂ 20–30 | | 45% ♀ 63% ♂ > 30
| El Sammak et al. 201170 | Hospital based | | Al-Khobar (26°N) | 87 ♂, 52 ♀ blood donors | Yes | CIA/ Liaison | Dec 2008- Mar2009 | Veiling | ♂ 10.1 ± 4.5 | | ♀ 9.9 ± 4.5
| El Sammak et al. 201071 | Hospital based | | Al-Khobar (26°N) | 87 ♂ 30.0 ± 8.5yrs | | 52 ♀ 31.0 ± 7.2yrs | Yes | CIA/Liaison | Dec 2008-Mar 2009 | NA | ♂ 10.1 ± 4.7 | | ♀ 9.9 ± 4.5
| Al-Elq et al. | | 200972 | Hospital based | | Al-Khobar (26°N) | 200 ♂ 46.5 ± 14.6yrs 200 ♀ 42.6 ± 15.9yrs | Yes | RIA/Wallac | Feb-May 2008 | Older age, life Style, higher BMI ♂, lower BMI♀ | ♂ 31.1 ± 10.7 | | ♀ 28.9 ± 10.7
| Sadat-Ali et al. | | 200973 | Hospital based | | Al-Khobar (26°N) | 100 ♂ 28.2 ± 4.5yrs | | 100 ♂ 59.4 ± 15.6yrs | Yes | RIA/ Wallac | Feb-May 2008 | Low sun exposure | Younger: | | Mean 16.6 ± 3.4 in those ≤ 20 | | Mean 25.4 ± 2.7 in those > 20- < 30 | | Older: | | Mean 16.7 ± 3.4 in those ≤ 20 | | Mean 25.3 ± 3.3 in those > 20–30
| Al-Turki et al. | | 200874 | Hospital based | | Al-Khobar (26°N) | 200 ♀ | | 25–35 y (Group 1) | | ≥ 50 y (Group 2) | Yes | RIA/ Wallac | Feb -May 2008 | Low sun exposure, low vit D diet | Group 1: | | 11% < 20 19% 21–29 70% > 30 | | Group 2: | | 19% < 20 36% 21–29 45% > 30 | | UAE | Al Anouti et al. | | 201175 | University based | | Al-Ain (24° N) | 208 ♀ 20.8 ± 4.0 y | | 70 ♂ 21.0 ± 4.6 y | No | HPLC | Oct 2009 138♀70 ♂ | | Apr 2010 70 ♀ | Low sun exposure, female gender | Summer ♀ 8.3 ± 5.9 | | ♂10.9 ± 6.2 | | Winter ♀ 12.5 ± 4.9
| Dawodu et al. | | 201176 | Pilot Study | | Al-Ain (24° N) | 8 Healthy Arab ♀ | | 20–30 y. | Yes | HPLC | Sep –Nov 2001 | Decreased surface area of the skin exposed, | | sun exposure | | low vit D intake | Expose face, arms and hands 15 min/ d twice a week for 4 weeks | | pre-intervention 7.04 | | post intervention 9.2
| Saadi et al. | | 200677 | Local clubs, | | primary care clinics, local hospitals | | Al-Ain (24° N) | 175Prem 84PM♀ | | Prem: 37.5 ± 9.5 y | | PM: 58.3 ± 8.9 y | Yes | RIA/Diasorin | Jan 2003-Jun 2005 | Younger age, | | low vit D intake, summer | 10.1 ± 4.3 Prem: 9.7 ± 4.2 | | PM: 10.9 ± 4.5 | | All ♀ vit D < 32 | | Apr 11.6 ± 5.2 | | Aug 7.2 ± 2.3 | | North Africa | | Morocco | | | | | | | |
| El Maghraoui et al. 201278 | Hospital based | | Rabat (34°N) | 178 p.m. ♀ | | ≥ 50 y | Yes | ECLIA/Roche | Summer 2010 | NA | 15.8 ± 11.6 | | 85% < 30 | | 66% < 20 | | 52% < 10
| Allali et al. 200979 | Hospital based Rabat (34°N) | 415 ♀ | | 24–77 y | Yes | CIA/Diasorin | Summer NA | Older age, lack of sun exposure, veiling, Ca intake < 700 mg | 91% < 30 | | 43% < 15 | | 4% < 5 | | Tunisia | Bahlous et al. 200980 | NA | | Manouba (37°N) | 134 p.m. ♀ with osteoporosis | Yes | HPLC | March–April 2004 | Osteoporosis | Fracture pts: 27.5 ± 15.1 51% < 20 | | Non fracture pts: 21.3 ± 13 25% < 20
| Meddeb et al. | | 200581 | NA | | Ariana (37°N) | 261♀ 128♂ | | 20–60 y | Yes | RIA/Incstar | Jan-March 2002 | Older age, veiling, high parity, postmenopausal | 47% < 15, 16% 5–10 | | 36% 20–28 y | | 60% 50–59 y |
Abbreviations in table listed here in alphabetical order: BMI: Body Mass Index; Ca: Calcium; CIA: Chemiluminescent Assay; EIA: Enzyme immunoassay; ELISA: Enzyme-linked immunosorbent Assay; ECLIA: Electrochemiluminescent Immunoassay; HPLC: High-performance liquid chromatography; IDS: Immunodiagnostic Systems; IRMA: Immunoradiometric Assay; LC-MS: Liquid Chromatography–Mass Spectrometry; NA: Not Available; PM: Post-Menopausal; Prem: Pre-Menopausal; PBM: Peak Bone Mass; RIA: Radioimmunoassay; SES: Socio-Economic Status; Vit: Vitamin ; WHR: Waist Hip Ratio ; Yrs: Years
* Table 2. *Overview of studies on 25(OH) D values in Children in Middle East
| Country | Author/Yr | Sampling Method City (Latitude) | N Gender/ Age | Exclusion criteria specified | Assay type/ Manufacturer | Season Yr | Predictors for low 25(OH)D | 25(OH)D Level Mean ng/ml % below cut-off |
| Iran | Ghergherechi et al. 201293 | Children hospital Tabriz (38°N) | 52 Obese children | |||||
| 4–16 y | ||||||||
| 57 Control | Yes | CIA/ Nichols | NA 2009–2011 | Obesity, high BMI | Case: 32.7 ± 29.6 | |||
| Control: 44.2 ± 11.2 |
| Neysestani et al. 201286 | Random systematic | | districts schools | | Tehran (35°N) | 573 Boys, 538 Girls | | 9–12 y | Yes | Competitive protein-binding assay/ IDS | Fall-winter | | 2007–2008 | Female gender | Boys: 11 | | Girls: 8
| Olang et al. 201187 | Vaccination heath centers | | Tehran (35°N) | 7112 infants | | 15– 23 mo | Yes | HPLC | May– June2001 | Female gender | 24.5 | | 3% < 10 33% < 20 | | 44% 20–30 20% > 30
| Ardestani et al. 201091 | School random sampling | | Isfahan (32°N) | 271 Boys, 242 Girls 6–7 y | Yes | RIA/ Incstar | Summer 2006 | Low intake of vitamin D, low sun exposure, dress style | 46 ± 17 | | 3% < 20
| Razzaghy Azar 201089 | Clinic university hospital | | Tehran (35°N) | 192 Girls, 121 Boys 8–18 y | Yes | EIA/ IDS | Apr 2006-Apr 2007 | High BMI, puberty stage, female gender | 25% (Boys 8% Girls 92%) < 5 | | 27% (Boys 34% Girls 66%) 5–10 | | 26% (Boys 58% Girls 42%) 10–20
| Dahifar et al. 200730 | One middle school | | Tehran (35°N) | 414 Girls | | 11–15 y | Yes | Gamma counter/ Genesys | Dec 2002- Mar 2003 | NA | 30 ± 15.8
| Moussavi et al. 200584 | High school Sampling | | Isfahan (32°N) | 153 Boys, 165 Girls 14–18 y | Yes | RIA/ Biosource | NA 2004 | Female gender | Total: 46.2% < 20 | | Boys: 37.3 ± 18.8 | | 18% < 20 1% < 8 | | Girls: 16.8 ± 8.4 | | 72% < 20 14% < 8 | | Jordan | Abdul Razzak et al. 201188 | Hospital based | | Amman (32°N) | 136 Infants, | | 139 Toddlers | | 6–36 mo | Yes | EIA/ IDS | Oct 2008- Jan 2009 | Sun exposure < 30 min, female gender, exclusive breast feeding | 17% < 15 | | 11% < 20 | | 28% < 30 | | 44% > 30
| Jazar et al. | | 201197 | Pediatrics Clinic Jordan (31°N) | 100 Boys 1–3 y | | 100 Girls 3–6 y | Yes | ECLIA/ Roche | May – June 2009 | Older age, high BMI, low outdoor activity indoor physical activity, nutrition | Toddler: 26.2 ± 1.2 | | Preschool children: 21.5 ± 1.2 | | 17% ≤ 15 | | 16% 15- 20
| Gharaibeh et al. 200998 | Local community center | | Jordan (31°N) | 93 Mothers 30yrs Children 60.7 mo | Yes | ELISA/IDS | June -July 2007 | Low milk intake, | | high income > 212$/month | Mother: 10.2 | | 2% < 5 49% < 10 98% < 20 | | Children: 22.3 82% < 20 15% > 30 | | Lebanon | El Hajj-Fuleihan et al. 200799 | School based | | Beirut (33.5°N) | 180 Boys13.1 ± 2 y | Yes | RIA/ Diasorin | Winter- Spring 2001–2002 | NA | 17 ± 7
| El Hajj-Fuleihan et al. 2006100 | School based | | Beirut (33.5°N) | 179 Girls 13.1 ± 2 y | Yes | RIA/ Diasorin | Winter- Spring 2001–2002 | NA | 14 ± 8
| El Hajj-Fuleihan et al. 200183 | School based | | Beirut (33.5°N) | Spring: | | 81 Boys, 88 Girls 13.3 ± 1.6yrs | | Fall: | | 83 Boys, 94 Girls | | 13.3 ± 1.7yrs | Yes | RIA/ Diasorin | Spring- Fall 1999 | Spring season, female gender, age, Tanner staging, low sun exposure, | | calcium intake, vitamin D intake, BMI | Spring: | | Total:17 ± 8 21% < 10 44% 10–20 | | Boys:19 ± 7 9% < 10 46% 10–20 | | Girls:15 ± 8 32% < 10 42% 10–20 | | Fall: | | Total: 22 ± 7 4% < 10 36% 10–20 | | Boys: 24 ± 6.2 25% 10–20 | | Girls: 19 ± 7 7% < 10 46% 10–20 | | Qatar | Bener et al. | | 2009103 | Primary Health Care Centers | | Doha (25.3°N) | 458 | | Mean 10.9 ± 3.54 y in those < 20 ng/ml | | Mean 9.54 ± 3.98 y in those 20–80 ng/ml | No | RIA/ Diasorin | Aug 2007-Mar 2008. | Older Age, non White low sunlight expos, low physical activity, low dietary vit D, family history of vit D deficiency | 69% < 20 ng/ml, mean 13.4 ± 8.9 | | 31% < 20 ng/ml, mean 27.5 ± 8.3 | | Saudi Arabia | Al-Ghamdi et al. 201285 | School-based | | Jeddah (22°N) | 150 ♂ 7–16 y | | 150 ♀ 6–18 y | Yes | ECLIA/ Roche | May NA | Female gender | 16.5 ± 3.7 (6–9 y ♀) | | 24.5 ± 5.2 (6–9 y ♂) | | 22 ± 4.5 (10–12 y ♂) | | 12.6 ± 3.7 (10–12 y ♀) | | 19.6 ± 5.2 (13–14 y ♂) | | 11.6 ± 3.6 (13–14 y ♀) | | 8.8 ± 3.8 (15–18 y ♀) | | 15.7 ± 5.6 (15–18 y ♂)
| Al Othman et al. 201282 | Primary Health Care Centers | | Riyadh (25°N) | 331 (153♂178 ♀) | | Physically inactive: | | 13.4 ± 3.2 y | | Moderate Activity: | | 12.6 ± 3.3 y | | Active: 12.1 ± 3.6 y | Yes | ELISA /IDS | Mar- Dec 2010 | Low physical activity, low sun exposure | 7.1 ± 0.6 (Physically In Active) | | 8.5 ± 0.6 (Moderate Activity) | | 9.1 ± 0.6 (Active) | | 11% < 5 72% 5–10 17% 10–20
| Kensarah et al. 2012102 | School-based | | Makkah (21°N) | 87 ♂ 61♀ | | ♂10.4yrs,♀9.6yrs | Yes | ECLIA /Roche | NA | Female gender | 97% ♀ < 20 | | 78% ♂ < 20 | | UAE | Rajah et al. | | 2012101 | Pediatric outpatient clinics | | Abu Dhabi(24°N) | 183 (52% ♂) | | 5.32 ± 3.76 y | Yes | RIA /Diasorin | All year 2005–2008 | Sedentary lifestyle, veiling, Ca deficient diet. | Total:21.4 18% > 10 | | 27.5 (0–0.9yrs) 31 (1–2yrs) | | 21.2 (2–8yrs) 14.1(8–12yrs)
| Dawodu et al. 200390 | Maternal and child health clinics | | Al-Ain (24° N) | 90 unsupp breast feeding Infants and Mothers | Yes | HPLC | Apr- Oct 1999 | Low dietary vit D intake, low sun exposure | Mothers 8.6 (61% < 10) | | Infants 4.6 (82% < 10)
| Dawodu et al. 2001104 | Hospital based | | Al-Ain (24° N) | 51 | | 15.4 mo | | UAE nationals (26) non-Gulf Arabs(25) | Yes | HPLC | Feb- Sep NA | Low Vit D supplementation | Infants 22% < 10 | | 25 ± 11.9 (dietary Vit D supp) | | 15.4 ± 10.9 (unsupp) | | Mothers 50% < 10 | | 11.36 ± 5.6 |
Abbreviations in table listed here in alphabetical order. BMI: Body Mass Index; CIA: Chemiluminescent Assay; EIA: Enzyme immunoassay; ELISA: Enzyme-linked immunosorbent Assay; ECLIA: Electrochemiluminescent Immunoassay; HPLC: High-performance liquid chromatography; IDS: Immunodiagnostic Systems; NA: Not Available; RIA: Radioimmunoassay; Supp: Supplemented; Unsupp: Unsupplemented; Vit: Vitamin; Yrs: Years
* Table 3. *Overview of Studies on 25(OH) D Values in Pregnant Women/Neonates in Middle East
| Country | Authors/Yr | Sampling Method City (Latitude) | N/ Age | Exclusion criteria specified | Assay type/ Manufacturer | Season /Yr | Predictors for low 25(OH)D | 25(OH)D Level Mean ng/ml % below cut-off |
| Iran | Asemi et al. 2010109 | Maternity clinic Kashan (34°N) | 147 pregnant ♀ | |||||
| 18–35 y | Yes | HPLC | NA/ 2008–2009 | NA | 15 ± 8 |
| Kazemi et al. 2009108 | Maternity clinics general hospital Zanjan (37°N) | 67 full-term pregnant mothers 28.5 ± 5 y and 61 neonates | Yes | ELISA | Mar- Sep 2005 | Winter for maternal and cord blood | Mother 8 ± 1.5 Summer 13 Winter 3 | | Cord 7 ± 1 Summer 8.7 Winter 5
| Bassir et al. 2001110 | Maternity Hospital Shohalda | | Tehran (25–35°N) | 50 mothers 16–40 y and their neonates | Yes | Radioligand assay | Jan- Sep 1997 | NA | Mother 5 ± 2 80% < 10 | | Cord 2 | | Israel | Mukamel et al. 2001111 | | 156 Orthodox and 185 non- Orthodox Jewish mothers | | at delivery | Yes | Competitive Protein Binding Assay | All year 1998–1999 | Sect | Orthodox 13.5 ± 7.5 | | 5% < 5 32% < 10 | | Non-Orthodox 18.6 ± 9.6 | | 3% < 5 13% < 10 | | Kuwait | Molla et al. 2005112 | Hospital based n = 2 | | Kuwait city (29 °N) | 214 pregnant mothers 27.7yrs | | and their neonates | Yes | RIA/ Incstar | All year 1999–2000 | NA | Mothers 13–17 | | Neonates 8 | | 40% mothers, 60% neonates < 15 | | UAE | Narchi et al. 201092 | Maternal and Child Health | | Al Ain (24°N) | 75 pregnant from early pregnancy to 6 mo postpartum | | 18–40 y | Yes | RIA/IDS | Sep-Nov 2007 | Dietary habits, | | voluntary avoidance of sun exposure, veiling | First antenatal visit 17.3 ± 10.5 | | After delivery 14.4 ± 9.8 | | At 6 mo 11.9 ± 11.2 |
Abbreviations listed in alphabetical order: ELISA: Enzyme-linked immunosorbent Assay; HPLC: High-performance liquid chromatography; IDS: Immunodiagnostic Systems; NA: Not Available; RIA: Radioimmunoassay; Yrs: Years
Adults in Middle East Iran
The mean 25(OH)D level in several cross-sectional studies of good to very good quality was in the low teens [25(OH)D 10−15 ng/ml],39,40,42-45 and the majority of these studies used randomized cluster sampling that was population based, be it at city level or nation level.
Jordan
Quite opposing results were found in two large, recent, population based studies graded as very good. The first included 4590 subjects and revealed a surprising high mean 25(OH)D level of 73 ng/ml in males and 40 ng/ml in females,57 levels that remain unmatched in any other study or population. Conversely, a study of 2032 women, age 15−49 y revealed a median vitamin D of 11 ng/ml, 96% of subjects had levels below 20 ng/ml, and 60% were below a cut-off of 12 ng/ml.56 While the former study used a Biosource assay, the latter used the gold standard LCMS assay to measure vitamin D. Aside from assay differences, reasons for such wide discrepancies remain unexplained.
Lebanon
Several studies including a population-based study conducted in elderly subjects revealed mean 25(OH)D levels varying between the low-high teens [25(OH)D 12–18 ng/ml].60,61,94In an interesting sub-set analysis of a large international study in post-menopausal women, Lebanese Muslim women had lower levels than Christian women, findings that could in part be explained by dress style and higher BMI in Muslims.60
Occupied Palestine/Israel
In general 25(OH)D mean levels were higher than those recorded in other countries in Middle East, including those reported in several large scale studies that took advantage of Health Maintenance Organization (HMO) or Non-Governmental Organization (NGO) databases, averaging around 20 ng/ml.51,53,54 One ecological study revealed vitamin D levels to be highest in Ashkenazi Jews and lowest in Arabs.55
Saudi Arabia
While several large sample population based studies as well as smaller studies revealed a high prevalence of hypovitaminosis D in Saudi Arabia (> 80% below 20 ng/ml),64,66,70 few smaller studies revealed replete levels.72,74 In a sample of 1,172 women from of population-based survey of 40 primary health care centers around the city of Jeddah, 80% of subjects had a 25(OH)D level below 20 ng/ml. Mean levels in pre-menopausal women were 17 and in post menopausal women were 13 ng/ml.67 Similarly a mean level of 12 ng/ml was found in a sample of 834 adults men, age 42 y.64
United Arab Emirates
The mean levels from the three studies listed in Table 1 are close to 10 ng/ml, with inverse seasonal pattern.75-77
Adults in North Africa
Studies from this region are scarce, limited to Morocco and Tunisia. Two hospital-based studies conducted in women in Rabat revealed a 25(OH)D level in the mid-high teens.78,79 Studies in Moroccan immigrants revealed similarly low levels.95,96 A study of 100 immigrants with mean age of 49 y, showed a mean 25(OH)D of 11 ng/ml and 90% of subjects had mean levels below 20 ng/ml.96Findings were not different in Tunisian women, with mean levels again noted in mid-teens.80,81
Children and adolescents in the Middle East
As detailed in Table 230,82-91,93,97-104 most studies reported mean 25(OH)D levels in teens or close to 20 ng/ml, thus again revealing a large proportion of apparently healthy children, that is 30–75%, to have 25(OH)D levels below this deemed desirable cut-off.
Iran
Registered the largest number of studies with wide variations in 25(OH)D levels, in general being lower in winter, in girls and in older children. The proportion of subjects with 25(OH)D level below 20 ng/ml was 33% in 7,112 infants and toddlers in Tehran (36° North) in early summer,87 3% in a sample of 513 young school children, age 6−7 y in Isfahan (33° North) in the summer,91 up to 78% in school adolescents from Tehran in the spring,89 and 46% in high school students.84 Mean levels were quite low in the winter in 1,111 older school children from Tehran, measured at 11ng/ml in boys and 8 ng/ml in girls,86 and surprisingly high in middle school girls in Isfahan in winter.30
Jordan
Two studies conducted in hospital based clinics in Amman, in toddlers and pre-school children, one in summer and the other in the winter, revealed that one-third of subjects had mean 25(OH)D levels below 20 ng/ml,88,97 while a community based sample in 93 children mean age 60 mo, in the summer of 2007, revealed the proportion to be even higher at 82%.98
Lebanon
Two separate studies reported mean 25(OH)D levels in mid-teens conducted in school adolescents from greater Beirut.83,99,100 Between 30–40% had a mean 25(OH)D levels below 20 ng/ml, proportions being higher in the winter and in girls.
Saudi Arabia
A school-based study reveals 25(OH)D levels in mid-high teens in children, being lower in girls than boys, whereas mean levels were below 10 ng/ml in a study of adolescents recruited from primary health care centers in Ryadh.82,85
United Arab Emirates
In study of 183 children, age 1−12 y, selected from an urban ambulatory clinic in Abu Dhabi, there was a decrease in 25(OH)D levels with age from infancy to early adolescence; 21% of girls and 16% of boys had a 25(OH)D below 10 ng/ml, and the proportions were 46% and 32% respectively for a cut-off below 20 ng/ml.101 Levels were lower in mother and infants from 2 hospital based studies, where 61% of the mothers and 82% of the 78 infants tested had hypovitaminosis D (serum 25(OH)D < 10 ng/ml).90,104
Qatar
In a small study of 65 school girls, age 9−15 y, 25(OH)D levels were below 20 ng/ml in 98%.105 The weighted average for 25(OH)D was 17.5 ng/ml level in 458 subjects, age < 16 y, attending a primary health clinic and was less than 20 ng/ml in 69%.103
We could not identify any studies conducted in children and adolescents for countries in North Africa.
Pregnant women and neonates
A systematic review of first trimester normative 25(OH)D levels, of 18 studies across the world, revealed mean 25(OH)D levels ranging between 29 and 73 nmol/L in white Caucasian women and between 15–26 nmol/L in Turkish and Moroccan and other non-western women in Netherlands.106 Similarly, a high prevalence of low 25(OH)D levels was reported in ethnic minority groups in western countries, the prevalence ranged between 59–84% in the Netherlands, exceeded 50% in the UK, averaged 61% in New Zealand, was above 80% in Australia, using a cut-off of 10 ng/ml; and it was 5–30% in the US at a cut-off of 15 ng/ml.7 Investigations in Saudi Arabia, Kuwait, United Arab Emirates and Iran reveal that 10–60% of mothers and 40–80% of their neonates had undetectable low 25(OH)D levels (0–25 nmol/L) at delivery.106 Such low levels may be associated with poor maternal and neonatal outcomes, as has been documented in women from western countries. Indeed, Caucasian women with low 25(OH)D levels had a higher risk of pre-eclampsia and Cesarean sections, but we are unaware of any such studies in the ME or Asia.106 More recently, children of women with low 25(OH)D levels in third term had smaller anthropometric parameters.107 In Iran, neonates born to mothers with low 25(OH)D levels have lower cord 25(OH)D levels, and in one study were more likely to have lower birth weight, height, Apgar score and may be at risk for the development of rickets.106 Unfortunately, the few studies conducted in the MENA were not population-based and thus not necessarily representative of vitamin D nutritional status of pregnant women and their neonates in the region. But the few studies available, revealed a 25(OH)D level below 20 ng/ml in mothers in all 6 studies and below 10 ng/ml in two of them and even lower levels in neonates and cord blood.108-112 Predictors for low maternal 25(OH)D levels included dress code, winter season, dietary habits and avoidance of sun exposure.92,108
![]()
Is There a Genetic Basis for Low Vitamin D Levels and Rickets in the MENA?
Lifestyle factors, namely sunlight exposure, diet and use of supplements, are well recognized major determinants of circulating 25(OH)D levels, in general,1 including subjects from the MENA, as detailed above. Interestingly, it has been recently underscored that genetic factors may contribute up to 50% of inter-individual variability in serum 25(OH)D levels (Fig. 1).113 Several genetics determinants of vitamin D status were recently described in a large genome wide association study of over 30,000 individuals of European descent from 15 cohorts.114 In addition, single nucleotide polymorphisms (SNPs) at or near 6 pre-specified vitamin D pathways candidate genes were considered. These include the vitamin D receptor (VDR), 1-α-hydroxylase (CYP27B1), 25-hydroxylase (CYP2R1), 24-hydroxylase (CYP24A1), vitamin D binding protein (GC, DBP) and 27- and 25-hydroxylse (CYP27A1) genes. The discovered genetic polymorphisms included variants near genes involved in cholesterol synthesis (DHCR7), hydroxylation (CYP2R1 and CYP24A1) and vitamin D transport (GC), and these may identify individuals at high risk of vitamin D deficiency.114 African Americans are a subgroup at higher risk for low vitamin D levels. A recent study investigating associations between 94 three single nucleotide polymorphisms (SNPs) in 5 vitamin D pathway genes (GC, VDR, CYP2R1, CYP24A1, CYP27B1) and serum 25(OH)D in 379 African American and 379 Caucasian controls, revealed statistical associations for 3 SNPS, 2 in the vitamin D transport pathway and one in the hydroxylation pathway, only in African Americans.115 Loss of CYP2R1 was also shown to be associated with 25(OH)D deficiency in several families in Nigeria116-118 and associations between VDR polymorphisms and rickets in subjects from the Middle East has also been previously raised.31,119 In a retrospective study of 34 Saudi children above age 10 y, who presented with rickets to a major hospital in Riyadh between 1994–2000, 59% had vitamin D deficiency, 11% calcium deficiency, 3% renal failure and 27% genetic causes. Of the total, 12% were reported by authors to have hypophosphatemic rickets, 9% to have 25-hydroxylase deficiency and 6% to suffer from vitamin D dependent rickets type I.119 In addition, a recent report of 2 adolescent siblings from a Saudi family presenting with short stature and rickets, revealed 2 new mutations in CYP2R1.120 The classical biochemical profile of very low 25(OH)D levels (below 4 ng/ml), within normal range calcitriol levels, the very high doses needed to normalize serum 25(OH)D levels, and an autosomal recessive inheritance pattern, had raised the author's suspicion for 25 hydroxylase deficiency. Residual hydroxylase function in the mutant allele or the presence of other hydroxylase enzymes that became more functional, in the presence of high levels of substrate, were proposed as possible mechanisms for the correction with supra-physiologic doses of vitamin D.120
Figure 1. Serum 25(OH)D Levels in Adults (A) and Children (B) Based on Color Codes. The color codes are: green > 30 ng/ml, yellow 20–29 ng/ml, orange 10–19 ng/ml, and red < 10 ng/ml. To convert from ng/ml to nmol multiply by 2.5. The color codes were selected based on mean or median results from population based studies available or as obtained from most representative studies for each country. For countries with varying results, the color code was chosen as valid for ≥ 50% of reported values; or more than one color code was used (for, e.g., children in Iran).
In conclusion, there is a growing body of substantial evidence supporting a genetic basis for low 25(OH)D levels in several populations and some data for it in cases of rickets in the MENA, the latter is however based on small series and case reports. Thus the need for large scale population based genome wide association studies to adequately address this question in a definitive manner.
![]()
Impact of Vitamin D on Surrogate Markers or Major Health Outcomes in MENA
The evidence for a beneficial effect of vitamin D on musculoskeletal health and a potential effect on non-classical outcomes, such as cardiovascular diseases, diabetes, inflammatory, infectious, immune disorders and cancers, as well as mortality has been extensively reviewed,1,3,5,121,122 and is beyond the scope of this paper. Cardiovascular diseases, maternal-neonatal health and infections are on the top of the health agenda of the World Health Organization and health authorities in countries worldwide, including the MENA region. Association and intervention studies evaluating the relationship between vitamin D and health outcomes, available to-date in the MENA region, will be examined here-in Table 4,61,94,123-140 and Table 5.100,141-149
* Table 4. *Overview on Association Studies Between 25(OH) D Levels and Health Outcomes in the Middle East and North Africa
| Country | Author/Yr | Sampling Method City | ||
| Cases/ Controls N Gender/ Age | Assay type /Manufacturer | Exclusion criteria specified | Disease condition | |
| /Health Outcomes | 25(OH)D Level | |||
| Mean ng/ml | Association between 25(OH)D and outcome (Correlation) | |||
| Egypt | Olama et al. | |||
| 2012123 | Clinic based | |||
| Cases: 50 ♀ 32.3 ± 9.4 y | ||||
| Controls: 50 healthy ♀ 33.1 ± 9.7 y | ELISA/IDS | Yes | Fibromyalgia | Cases: 15.1 ± 6.1 |
| Controls: 18.8 ± 5.4 | Lumbar spine: r = -0.352 | |||
| VAS of pain: r = -0.338 | ||||
| Beck score for depression: r = -0.328 |
| El Husseiny et al. 2012124 | Clinic based Cairo | | Cases: 36♂, 14 ♀ 30–65 y | | Controls:: 25 age- and gender-matched healthy subjects | RIA/Incstar | Yes | HCV infection | Cases: 15 ± 5.2 | | Controls: 39.7 ± 10.8 | Cases: | | Viral load: r = -0.84 IL-23: r = -0.776 | | IL-17: r = -0.665 MCP-1: r = -0.94
| Schaalan et al. 2012125 | Clinic based Cairo | | Cases: 36♂, 14 ♀ | | Controls:: 25 age- and gender matched healthy subjects | RIA/Incstar | Yes | HCV infection | Cases: ♂10.30 ± 2.12 | | ♀10.00 ± 2.60 | | Controls: 39.70 ± 10.80 | Cases: | | 25(OH)D and IL-17: r = -0.679 | | 1.25(OH)D and IL-17: r = -0.679 | | 1.25(OH)D and IL-23: r = -0.801
| Hamza et al. | | 2011126 | Clinic, Hospital and university based Cairo | | Cases: 52 ♀ and 8 ♂/ 6–19 y | | Controls: 50 ♀, 10 ♂/ 7.2–18.5 y | ELISA/ VDBP | Yes | SLE | Cases: 26.33 ± 12.05 | | 13% < 10 60% < 30 27% > 30 | | Controls: 42.66 ± 9.20 | SLEDAI: r = -0.91
| Al Sayed | | 2007127 | Clinic based Cairo | | Cases:93♂♀ 45.2 ± 2.6 y | | Controls:70 healthy 47.1 ± 3.1 y | RIA/IDS | Yes | Metabolic syndrome | Cases: 16.2 ± 4.52 | | Control: 25 ± 4.48 | Cases: | | BMI: r = -0.684 HOMA: r = -0.395 | | HDL: r = 0.277 PTH: r = -0.235 | | S. Insulin:r = -0.396 | | Iran | Khalili et al. | | 2012128 | Hospital based Tehran | | 139 ♀ > 55 y, ♂ > 45 y | RIA/ Abcam pic | Yes | Acute Myocardial infarction | 10.92 ± 7.2 | Hypertension: OR = 2.92 | | Use of cardiovascular drugs: OR = 2.36 | | Survival: OR = 0.216
| Hosseinpanah et al. 2011129 | Population based Tehran | | Cases: 251♂♀ 56.0 ± 10.6 y | | Controls: 251 healthy subjects 56.7 ± 11.7 y | EIA/ DRG | Yes | Cardiovascular | Median | | Cases: 12.5 (8.4–24.4) | | Controls: 18.1 (11–31) | Vit D < 10 had an almost 3-fold higher risk of developing cardiovascular outcomes ra = 2.90 than those between 10–15ng/ml r = 1.46
| Bonakdar et al. 2011130 | Clinic based Isfahan | | 40 ♀ 25.46 ± 4.16 y | RIA/ DIAsource | Yes | SLE | 9.68 ± 0.84 | BILAG: r = -0.486 | | BILAG after Adjustment: rb = - 0.292 | | Low vit D higher titers of anti-dsDNA
| Heidari et al. 2010131 | Clinic based Babol | | Cases: 276 ♂♀ 44.3 ± 15 y | | Controls: 202♂♀ 46.4 ± 14.2 y | ELISA/DRG | Yes | Musculoskeletal pain | Cases: 33.1 ± 28.4 | | Controls: 23.8 ± 29.1 | Vit D < 20 vs. ≥ 20 with: | | Musculoskeletal pain: ORc = 2.95 | | Leg pain: ORc = 7.4 | | Widespread pain: ORc = 2.8 | | Arthralgia: ORc = 3.9
| Garakyaraghi et al. 2010132 | Hospital based Isfahan | | 28 ♀, 67 ♂ 62 ± 11 y | CIA/Diasorin | Yes | Heart failure | 56.78 ± 51.33 | Diastolic volume: r = −0.24 | | Adjusted for age, Creatinine: r = −0.261
| Bonakkdaran et al. 2009133 | Hospital based Mashhad | | 119 ♂♀ 55.3 ± 11.2 y | RIA/Biosource | Yes | T2DM | 32.4 ± 21.6 | Age: r = -0.21, BMI: r = -0.25, CRP: r = -0.06
| Omrani et al. 2006134 | Cluster sampling Shiraz | | 676 healthy women aged 20–74 y | IRMA/ IDS | Yes | Mineral Metabolism | 28.9 ± 23.0 | PTH r = –0.10 | | Independent of age | | Occupied Palestine/ Israel | Saliba et al. | | 2012135 | Population Based Clalit Health Services | | Cases: 1180 ♂♀ 65.30 ± 13.52 y | | Controls:184,479 ♂♀ 57.67 ± 18.25 y | CIA/DiaSorin | Yes | Primary Hyperparathyroidism | Cases: 19 ± 9 | | Controls: 20.8 ± 9.8 | Cases: | | PTH: r = −0.238 ALKPhos: r = −0.180 Calcium: r = −0.054
| Amital et al. 2010136 | 278 with systemic lupus erythematosus activity (SLEDAI) | | 100 with European Lupus activity measurement (ECLAM) 40.2 ± 14.2 y | CIA/Diasorin | No | SLE | SLEDAI: 23.9 ± 14.0 | | ECLAM: 27.6 ± 13.9 | Standardized values z-scores r = -0.12 The more active the disease, the lower the vitamin D concentration | | Lebanon | Arabi et al. | | 201294 | Population based Beirut | | 65 ♂and 130 ♀ 72.5 ± 5.1 y | RIA/ IDS | Yes | BMD | | Mineral Metabolism | ♂ 14.7 ± 4.0 | | ♀ 14.6 ± 7.4 | Overall: | | % Change Trochanter BMD: rd = 0.19 | | ♂:% Change Total hip BMD: rd = 0.31 | | % Change F. Neck BMD: rd = 0.36 | | % Change Trochanter BMD rd = 0.26
| Arabi et al. | | 200661 | Population based Beirut | | 286♀ 73.4 ± 5.2 y | | 157♂ 74.1 ± 5.08 y | RIA/ IDS | Yes | BMD | | Mineral Metabolism | | ♀BMD Total hip, FN, Troch: re = 0.10–0.18 | | ♂ BMD Total hip,spine, FN, Troch:re = 0.16 -0.27 | | Qatar | Bener et al. | | 2009137 | Clinics /Face to face Interviews Doha | | Cases: 170 ♂♀ 10.5 ± 3.8 y | | Controls: 170 ♂♀ 9.9 ± 4.2. yrs | RIA/DiaSorin | No | T1DM | Cases: 15.8 ± 9.2 | | Controls:18.5 ± 9.6 | NA | | Saudi Arabia | Bin –Abbas et al. 2011138 | Pediatric and Endo Clinics Riyadh | | Cases:59 ♀ 41 ♂ | | Controls: 52♀ 48 ♂ | HPLC | Yes | T1DM | Cases: 14.7 ± 5.7 | | Controls:17.9 ± 5.6 | No Correlation between glycemic control and 25 OHD level.
| Al Daghri et al. 2010139 | Primary Health Care Centers Riyadh | | Cases: 76 ♀, 88 ♂ 50.6 ± 10.1 y | | Controls: 106 ♀, 71 ♂non-diabetic | | 37.5 ± 15.3 y | ELISA/ IDS | Yes | T2DM | Cases: 10.8 ± 4.7 | | Controls: 7.2 ± 2.9 | Cases: TC: r = -0.20 LDL-C: r = -0.17 | | TG: r = -0.17 BMI: r = -0.22 | | Controls: SBP: r = 0.22 WHR: r = 0.16 | | Non-Adjusted values | | Yemen | Salem et al. | | 2009140 | Hospital based Sana’a | | 152 children with VSP 2–59 mo | ELISA/ IDS | yes | Very severe pneumonia, | | some with rickets | Deficient n = 50:37.2 ± 17.3 | | Sufficient n = 9: 47.3 ± 17.6 | Failure to respond to antibiotic therapy in rachitic compared with non rachitic OR = 1.38 | | * | | Only significantly different 25(OH)D levels between cases and controls, and correlations .Details on studies that presented adjusted correlations are as follows: Hosseinpahanh et al. 2011, ra adjusted for BMI, FPG, SBP, DBP,CT,TG,HDL-C, Smoking Status, degree of physical activity, premature CVD familial history . Bonakdar et al. 2011, rb adjusted for age, BMI, sun exposure, use of sunscreen, physical activity. Heidari et al. 2011, ORc adjusted for sex. Arabi et al. 2012, rc adjusted for age, calcium intake, serum Creatinine and PTH in multivariate models, mean 25OHD was no more a predictor of bone loss. Arabi et al. 2006, rd adjusted for age, height, lean mass and PTH levels, 25OHD level did not have residual significant contribution to BMD at any skeletal site except the trochanter in men. Abbreviations in table listed here in alphabetical order: ALKPhos:Alkaline Phosphatase; BILAG: British Isles Lupus Assessment Group; BMD: Bone Mineral Density; BMI: Body Mass Index; CIA: Chemiluminescent Assay; CRP: C- Reactive Protein; DsDNA: Double Stranded DNA; EIA: Enzyme immunoassay; ELISA: Enzyme-linked immunosorbent Assay; ECLAM: European Consensus Lupus Activity Measurement; FN: Femoral Neck; HCV: Hepatitis C virus; HDL: High Density Lipoprotein; HOMA: Homeostasis Model Assessment ; HPLC: High-performance liquid chromatography; IDS: Immunodiagnostic Systems; IL-17: Interleukin-17; IL-23: Interleukin-23; IRMA: Immunoradiometric Assay; LDL-C: Low Density Lipoprotein- Cholesterol; MCP-1: Macrophage chemoattractant protein-1; NA: Not Available; OR: Odds Ratio; r: Correlation; RIA: Radioimmunoassay; SBP: Systolic Blood Pressure; SLE: Systemic Lupus Erythematosus; SLEDAI: Systemic Lupus Erythematosus Disease Activity Index; TC: Total Cholesterol; TG: Triglycerides ; Troch: Trochanter; T1DM: Type 1 Diabetes Mellitus; T2DM: Type 2 Diabetes Mellitus; Vit: Vitamin; VAS: Visual Analogue Scale; VSP: Very Severe Pneumonia; VDBP: Vitamin Tracer, for the Binding Pocket of Vitamin D Protein; WHR: Waist Hip Ratio; Yrs: Years | | * Table 5. *Overview on Interventional Studies between 25(OH)D Levels and Health Outcomes in the Middle East
| | Country | Author | | Yr | Sampling Method | | City (Latitude) | | N Gender/ Age | Protocol Design | Intervention | | Type/Dose/Duration | Assay type/ Manufacturer | Exclusion criteria specified | 25(OH)D Level Mean ng/ml | Effect on Health Outcome | | Iran | Shakinba et al. | | 2011141 | School Based | | Yazd (32°N) | | 120 girls 12–15 y | | Group 1: 28 with Vit D Deficiency | | Group 2: 23 with Vit D Deficiency | | Group 3: 30 | | Group 4: 30 | RCT | Group 1: 300,000 IU D3 once, | | randomized to 50,000IU D3/month | | Group 2: 300,000 IU D3 once, | | randomized to 100,000 IU D3/ | | 3 mo | | Group 3: 50,000 IU D3/3 mo | | Group 4: 100,000 IU D3/3 mo | CIA/DiaSorin | No | Baseline One year | | Group 1 29.7 ± 4.6 47% 20–30 | | 53% 30–100 | | Group 2 30 ± 5.6 57% 20–30 | | 43% 30–100 | | Group 3 15.2 ± 6 13% < 10 | | 73% 10–20 | | 11% 20–30 | | 3% 30–100 | | Group 4 23 ± 6.8 45% 10–20 | | 35% 20–30 | | 19% 30–100 | NA
| Ghazi et al. | | 2010142 | School Based | | Tehran (35.7°N) | | 105 ♂, 105 ♀14–20 y 16 ± 1.5 y | | Group A:35♂,35♀ | | Group B:34♂,35♀ | | Group C:34♂,35♀ | Double-blinded RCT | Group A:50,000 IU D3/monthly | | Group B: 50,000 IU D3/2 mo+ placebo every alternative month | | Group C:Placebo | ELISA/IDS | | Baseline 6 mo | | Group A: 12.8 ± 8.8 ♀19.2 ± 9.4 | | ♂29 ± 10.5 | | Group B: 11.3 ± 5.8 ♀13.5 ± 9.2 | | ♂23.1 ± 7.6 | | Group C: 11.6 ± 7.2 ♀8 ± 5.6 | | ♂15.6 ± 6.4 | NA | | Israel | Gotsman et al. | | 2012143 | Population based Clalit Health Services | | A- 3009 ♂♀ with Heart Failure 75.9 ± 10.7 y | | 46,825♀♂ controls 64.7 ± 11.3 y | | B- 791 ♂♀with Heart Failure | | 458 ♂♀ with supplementation | | 333 ♀♂without supplementation | A-Case-Control | | B-Interventional | B. 800 IU/d and 1000 IU/d for median follow up of 518 d. | RIA/DiaSorin | No | A- Cases Median:14.8 | | Controls Median:16.3 | | B- Survival Rate | | HF patients < 10 ng/ml with supplementation:85.6 ± 1.7% | | HF patients < 10 ng/ml without supplementation:81.6 ± 1.7% | Reduced Mortality in Heart Failure patients HR = 1.52 and controls HR = 1.91 | | Lebanon | El-Hajj Fuleihan | | et al 2006100 | School Based | | Beirut (33°N) | | 179 ♀ | | Group A: 13 ± 2.1 y | | Group B: 13.1 ± 2.2 y | | Group C: 13.6 ± 2.1 y | Double-blinded RCT | Group A:Placebo | | Group B: Low dose 200 IU D3/d | | Group C: High dose 2000 IU D3/d | RIA/DiaSorin | Yes | Baseline One year | | Group A: 14 ± 7 16 ± 8 | | Group B: 14 ± 9 17 ± 6 | | Group C: 14 ± 8 38 ± 31 | Low dose and High dose: increase in BMD, Lean Mass | | High dose:increase in Total BMD, Bone Area | | Premenarcheal girls had the highest increment | | Country | Author | | Yr | Sampling Method | | City (Latitude) | | N Gender/ Age | Protocol Design | Intervention | | Type/Dose/Duration | Assay type/ Manufacturer | Exclusion criteria specified | 25(OH)D Level Mean ng/ml | Effect on Health Outcome | | Qatar | Soliman et al. 2011144 | General Practitioner Clinic | | Doha(25.3°N) | | 40 Adolescents with Vit D Deficiency | Prospective | | Open-Label | | Non-Randomized | 600,000 IU D3 every 2–3 mo | RIA | No | Pre-Interv Post Interv | | 9.3 ± 4.6 27.7 ± 9.2 | Healing of Rickets in all patients at one year. | | Saudi Arabia | Al-Daghri et al. | | 2012145 | Primary Health Care Centers | | Riyadh (24.6°N) | | 31♂28♀ 18–65 y 38 ± 14.1 y | Interventional | Advice for 5–30 min sun exposure twice/ week and vitamin-D rich foods | ELISA/IDS | Yes | Baseline 6 mo 12 mo | | 7.6 ± 0.6 10.7 ± 0.6 11.4 ± 0.6 | Decrease of Metabolic Syndrome from 25% to 13% | | UAE | Rajah et al. | | 2010146 | Hospital Based | | Abu Dhabi (24°N) | | 10 Children with Rickets: | | Group 1: 7 children | | Group 2: 3 children | | 21.2 ± 8.4 mo | Retrospective | | Audit | Group 1:2000 IU D2/d for 3 mo +400 IU D2/d subsequently+ Ca 40 mg/Kg/d for 3 mo | | Group 2: stosstherapy 600,000IU D2 single dose + Ca 40 mg/Kg/d for 3 mo | HPLC | Yes | Baseline 3 mo | | 15.1 ± 10.3 NA | | Median: 11.6 Median: 57.4 | NA
| Saadi et al. | | 2009147 | Maternal-Child Health Clinic | | Al-Ain(24°N) | | Group 1: 22 mothers 28.1 ± 4.7 y | | Group 2: 22 mothers 27.6 ± 6.5 y | | Group 1: 22 infants 19.1 ± 25.4 d | | Group 2: 24 infants 20.6 ± 22.9 d | RCT | Mothers: | | Group 1:2000 IU D2/d for 3 mo | | Group 2:60,000 IU D2/m for 3months | | Infants:400 IU D2/d for 3 mo | RIA /DiaSorin | No | Mothers Pre-Interv Post Interv | | Group 1: 11 ± 4 16.9 ± 5.6 | | Group 2: 8.9 ± 4 15 ± 4 | | Infants 30% < 20 ng/ml at 3 mo | | Group 1: 5.6 ± 3.4 19.8 ± 7.4 | | Group 2: 5.5 ± 4.8 17.8 ± 6 | NA
| Rajah et al. | | 2008148 | Hospital Based | | Abu Dhabi (24°N) | | 31 Children with Rickets: | | 8 Vit D deficient 14.8 ± 3.2 mo | | 8 Ca deficient 19.8 ± 2.3 mo | Quasi-Experimental Non-Randomized | 2000–5000 IU D2/d for 3 mo + 400 IU D2/d for a variable period | CIA/Nichols | No | Baseline: | | 8 Vit D deficient: 6.9 ± 1.3 | | 8 Ca deficient: 17.7 ± 7.1 | Height z-score | | Entry: -1.74 Termination:-0.88
| Saadi et al. | | 2007149 | Maternal-Child Health Clinic | | Al-Ain(24°N) | | Group 1:45 lactating♀29.2 ± 5.5yrs | | Group 2:45 lactating♀29.9 ± 6.7yrs | | Group1:43nulliparous♀23 ± 5.2yrs | | Group2:45nulliparous♀24.6 ± 5.1yrs | Open-Label | | RCT | Group 1:2000 IU D2/d for 3 mo | | Group 2:60,000 IU D2/m for 3months | RIA /DiaSorin | Yes | Lactating Pre-Interv Post-Interv | | Group 1: 10.9 ± 4.2 17 ± 5.6 | | Group 2: 9.3 ± 4.3 15 ± 4.2 | | Nulliparous | | Group 1: 7.8 ± 5 16.7 ± 10.6 | | Group 2: 7.6 ± 4.9 15.7 ± 8.6 | 1/3 ♀achieved 25(0H)D ≥ 20ng/ml |
Abbreviations in table listed here in alphabetical order: BMD: Bone Mineral Density; Ca: Calcium; CIA: Chemiluminescent Assay; ELISA: Enzyme-linked immunosorbent Assay; HPLC: High-performance liquid chromatography; HR: Hazard Ratio; IDS: Immunodiagnostic Systems; NA: Not Available; RIA: Radioimmunoassay.
Associations studies Musculoskeletal health
Significant negative associations between 25(OH)D and PTH levels were reported in young and old Lebanese subjects,62 adults and elderly subjects from Iran,134,150 and patients with hyperparathyroidism from Israel.135 Positive associations between 25(OH)D levels and bone mass were also reported at several skeletal sites, in adolescent Lebanese girls100 and elderly subjects.61 In the elderly Lebanese, 25(OH)D levels also correlated with lean mass in men but not women and the correlations with BMD disappeared for all skeletal sites except for trochanter after adjusting for lean mass and PTH.61 In the same study, subjects were followed prospectively and25(OH)D levels significantly correlated with bone loss over a mean follow-up of 4.4 y. This relation disappeared after adjusting for PTH levels.94 In the adolescent study, there were no significant relationships between VDR genotype and baseline bone mass BMD, but in the elderly study, elderly women with the heterozygous VDR genotype had the highest bone mass at the lumbar spine and forearm.151
Non-classical outcomes
Lower mean 25(OH)D levels were reported in patients with type I DM in Saudi Arabia and Qatar137,138 and it has been suggested that low levels may also contribute to metabolic syndrome and type II DM.152 This is particularly pertinent, considering that the Middle East registers some of the highest rates for obesity, exceeding the rising tide in western countries, reaching 40–50%,153 and has the greatest relative increase in diabetes prevalence, with rates reaching 20% in Bahrain, Saudi Arabia and the United Arab Emirates.153,154 In patients with type II diabetes, negative correlations with BMI and several lipid parameters, were reported in studies from Iran and Saudi Arabia.133,139 Mean 25(OH)D levels were also low in subjects with metabolic syndrome and also negatively correlated with BMI, lipid parameters, blood pressure and indices of insulin sensitivity.127,145 The relationship between vitamin D and cardiovascular diseases and mortality has been intensely scrutinized in western populations,122 and examined in three studies from MENA (Table 4). In the Tehran Lipid Glucose study, subjects with 25(OH)D levels below 10 ng/ml, had an almost 3-fold higher risk of developing cardiovascular outcomes than those above 15 ng/ml.129 In a small longitudinal study of 139 Iranian women admitted with acute myocardial infarction, 25(OH)D levels correlated with overall survival.128 These findings were validated in large HMO population-based database from Israel, that demonstrated that patients with heart failure and 25(OH)D levels below 10 ng/ml, had an increased risk of mortality, HR 1.52 (95% CI 1.21−1.92) and that patients who took vitamin D, at doses of 800–1000 IU/day reduced mortality, HR = 0.68 (95% CI 0.54−0.85), at a median follow-up of 518 d.143
Lower 25(OH)D levels have also been described in subjects with Systemic Lupus Erythematosis (SLE) and negative correlations reported with several indices of SLE disease activity in patients from Iran, Egypt and Israel.126,130,136 Associations with other rheumatologic conditions, musculoskeletal pain and fibromyalgia have also been described in patients from Egypt and Iran.123,131 Mean 25(OH)D level was significantly lower in Egyptian patients with Hepatitis C Virus (HCV) infection than controls, measured at 10 ng/ml and negatively correlated with viral load and circulating levels of several interleukins.124 Calcitriol also negatively correlated with interleukin levels in the same study subjects.125 Lower 25(OH)D levels have also been noted in adults Iranian patients with multiple sclerosis,155 and children suffering from Celiac Disease in Israel.156 Only few are the studies that performed the necessary adjustments to identify the independent impact of vitamin D on health outcomes. Furthermore, association studies cannot control for all potential confounders and thus the lack of good evidence for a cause- effect relationship. For example obese subjects have low vitamin D and are also more likely to display the profile of metabolic syndrome, but that does not prove that low vitamin D is the cause for metabolic syndrome. Similarly, illnesses in general and cirrhosis in particular are conditions more likely to be associated with low vitamin D, but there is no good evidence for a causative effect for vitamin D in the illness. Thus there exists the need to rely on intervention studies, which are however scarce.
![]()
Intervention Studies
Rickets
A Cochrane review of four interventions trials enrolling around 1700 term infants, lasting between 9 mo and 2 y, showed that vitamin D at doses of 300−400 IU/day was sufficient to prevent rickets.157
Various regimens to treat rickets in the region have been described and were mostly conducted in non-randomized, non-blinded interventional studies. Treatment with a single intramuscular injection of vitamin D at doses of 150,000–600,000 IU, single oral doses between 50,000 IU and 600, 000 IU, daily injections or oral doses of 5,000 to 20, 000 IU for 1–3 mo followed by 400 IU daily maintenance, all revealed substantial improvement in biochemical, clinical and radiological features of rickets.11
In a dose ranging study of 52 Turkish infants with nutritional rickets and a mean age of 10 mo, subjects were randomized to receive one oral dose of vitamin D of 50,000 IU, 300,000 IU or 600,000 IU, and all received oral calcium for one week. On the 30th day there was no difference in the improvement between the three groups, and all patients had improved by the 60th day post-therapy, however, eight infants developed hypercalcemia, six of which were allocated to the high dose group.158 The two most recent intervention studies conducted in ME are detailed in Table 5 and confirm findings from previous studies as summarized above. Children with rickets from some countries in ME such as Egypt, Saudi Arabia and the United Arab Emirates have low calcium intake. Therefore, careful assessment of calcium nutrition and concomitant therapy with calcium, in cases from the region is indicated and would expedite clinical recovery.
Skeletal health in adults
The relationship between 25(OH)D levels and indices of bone and mineral metabolism, based on randomized controlled trials, are well established and extensively studied in western populations and to a lesser extent in other ethnic groups.106 There are no such studies on subjects in the MENA region.
Skeletal health in children and adolescents
The IOM report states that the Recommended Dietary Allowance (RDA) is the dose of vitamin D that would result in desirable 25(OH)D levels, above 20 ng/ml, in 97.5% of the population. . In children, the RDA is 600 IU/d.16Table 5 summarizes mean pre- and post-intervention 25(OH) D levels from recent studies in the region. The administration of doses of vitamin D, several folds above 600IU, fail to bring most subjects above the 20 ng/ml cut-off, presuming the same desirable level is needed across ethnic groups.
A recent meta-analysis of 6 randomized placebo controlled trials studies, concluded that it is unlikely that vitamin D supplements are beneficial to bone mass in subjects with normal 25 (OH)D levels.159 However, planned subgroup analyses by baseline 25(OH)D level suggest that vitamin D supplementation of deficient children and adolescents could result in clinically useful improvements.159 The latter was in large part driven by results from a randomized placebo controlled trial in 179 Lebanese girls, mean age 13 y, that showed a positive impact of vitamin D, administered weekly, at the equivalent daily doses of 200 IU and 2000 IU/day on musculoskeletal parameters in girls, including bone mineral content, density, area and lean mass, especially during the pre-menarcheal period.100 A significant relationship between VDR genotypes and changes in bone mass at one year emerged and remained significant after adjustment for puberty, changes in lean mass, height and bone area.160
Maternal and neonatal health
There are very few studies evaluating effect of vitamin D on musculoskeletal outcomes in mothers or neonates. In a randomized controlled vitamin D trial, conducted in 2000 neonates in India, vitamin D administration at 35 µg/day (1400IU/day), significantly increased standard deviation (Z) scores for weight, length and arm circumference and decreased the proportion of children with stunted growth at 6 mo, but had no effect on death, hospitalization, in or out-patient visits.161 Two on-going large multicenter trials, one conducted in US and the other in England, are evaluating the safety and efficacy of vitamin D administration, in pregnant mothers after the first term. The first uses doses of 400, 2000 to 4000 IU D /d until delivery,162 and the second 1000 IU cholecalciferol/d or Placebo from 14 weeks gestation until delivery.163 Considering the severe vitamin D deficiency in pregnant and lactating women in MENA, the gap in this field is substantial.
Metabolic syndrome
A close examination of individual randomized controlled trials investigating the effect of vitamin D supplementation (± calcium) on components of the MetS reveals negative findings for most trials, with the exception of the few that used high doses of vitamin D in high-risk individuals with obesity and insulin resistance at entry, but none was conducted in MENA.152 In a study of 59 adult non diabetic, overweight and obese Saudis, advised to regularly expose themselves to sunlight and increase intake of vitamin D–rich foods, mean 25(OH)D levels increased from 7.6 to 11.2 ng/ml and the overall prevalence of MetS decreased from 25% to 13%, after one year.145
Infections
Chronic infections are still prevalent in the MENA region. Strong associations between hypovitaminosis D and tuberculosis (TB) infection and acute lower respiratory tract infections have been reported in Indian, Turkish and Sub-Saharan African populations.10 Although 25(OH)D levels below 20 ng/ml were associated with increased susceptibility to active TB in HIV-uninfected (n = 196) and HIV-infected (n = 174) black Africans in Cape Town, South Africa,164 vitamin D supplementation failed to improve clinical outcome or mortality in a randomized placebo controlled trial of 126 subjects recruited from National Health Service in United Kingdom with active TB.165 Vitamin D did not significantly affect time to sputum culture conversion in the whole study population, but it did significantly hasten sputum culture conversion in participants with the tt genotype of the TaqI vitamin D receptor polymorphism.165 However, vitamin D supplementation contributed to accelerating resolution of inflammatory responses and sputum smear conversion during tuberculosis treatment.166
![]()
Conclusion
Reports of nutritional rickets and osteomalacia occur in the MENA region, despite its plentiful sunshine and at much higher rates than in western countries. Hypovitaminosis, defined as a serum 25(OH)D below 20 ng/ml, is also prevalent across populations throughout the lifecycle, with proportions varying for the most part between 30–90%, depending on gender, season and lifestyle pattern. Population based studies are scarce, but results available from such studies validate the above observations. Genetic polymorphisms along the vitamin D pathway have been described mostly in western populations. The extent to which they account for low 25 (OH)D levels in the region awaits population-based genome wide association studies. There are large information gaps on what may constitute a desirable level for various health outcomes for subjects from this region. Furthermore, the recommended vitamin D doses by the IOM and even ES are sub-optimal to bring 25(OH)D to the putative “desirable” level in various age groups. Thus the pressing need to address such knowledge gaps, in order to facilitate the development of evidence-based region specific guidelines and to impact this subclinical condition that may be at the root of several chronic diseases.
![]()
Disclosure of Potential Conflicts of Interest
No potential conflict of interest was disclosed.
![]()
Acknowledgments
The authors would like to thank Ms Aida Farha, Medical Information Specialist, Saab Medical Library, American University of Beirut, for her advice and assistance in designing comprehensive and complex searches of the various medical literature resources and for the provision of select articles and Mr. Samir Hanoun for the art work.
![]()
References
Holick MF. Vitamin D deficiency. N Engl J Med 2007; 357:266-81; PMID: 17634462; DOI: 10.1056/NEJMra070553.
Rosen CJ. Clinical practice. Vitamin D insufficiency. N Engl J Med 2011; 364:248-54; PMID: 21247315; DOI: 10.1056/NEJMcp1009570.
Lips P, van Schoor NM. The effect of vitamin D on bone and osteoporosis. Best Pract Res Clin Endocrinol Metab 2011; 25:585-91; PMID: 21872800; DOI: 10.1016/j.beem.2011.05.002.
Norman AW, Bouillon R. Vitamin D nutritional policy needs a vision for the future. Exp Biol Med (Maywood) 2010; 235:1034-45; PMID: 20667908; DOI: 10.1258/ebm.2010.010014.
Bouillon R, Bischoff-Ferrari H, Willett W. Vitamin D and health: perspectives from mice and man. J Bone Miner Res 2008; 23:974-9; PMID: 18442312; DOI: 10.1359/jbmr.080420.
Zittermann A, Iodice S, Pilz S, Grant WB, Bagnardi V, Gandini S. Vitamin D deficiency and mortality risk in the general population: a meta-analysis of prospective cohort studies. Am J Clin Nutr 2012; 95:91-100; PMID: 22170374; DOI: 10.3945/ajcn.111.014779.
Prentice A. Vitamin D deficiency: a global perspective. Nutr Rev 2008; 66:S153-64; PMID: 18844843; DOI: 10.1111/j.1753-4887.2008.00100.x.
Prentice A. Nutritional rickets around the world. J Steroid Biochem Mol Biol 2012; ; PMID: 23220549; DOI: 10.1016/j.jsbmb.2012.11.018.
El-Kaissi S, Sherbeeni S. “Vitamin D Deficiency in the Middle East and Its Health Consequences for Adults. Nutr Health” in Vitamin D: Physiology, Molecular Biology, and Clinical Applications, ed. Michael Holick. New York (NY): Humana Press; 2010.
Arabi A, El Rassi R, El-Hajj Fuleihan G. Hypovitaminosis D in developing countries-prevalence, risk factors and outcomes. Nat Rev Endocrinol 2010; 6:550-61; PMID: 20852586; DOI: 10.1038/nrendo.2010.146.
El-Hajj Fuleihan G. Vitamin D Deficiency in the Middle East and its Health Consequences. Clin Rev Bone and Min Met 2009; 7:77-93; DOI: 10.1007/s12018-009-9027-9.
Mithal A, Wahl DA, Bonjour JP, Burckhardt P, Dawson-Hughes B, Eisman JA, et al. Global vitamin D status and determinants of hypovitaminosis D. Osteoporos Int 2009; 20:1807-20; PMID: 19543765; DOI: 10.1007/s00198-009-0954-6.
van Schoor NM, Lips P. Worldwide vitamin D status. Best Pract Res Clin Endocrinol Metab 2011; 25:671-80; PMID: 21872807; DOI: 10.1016/j.beem.2011.06.007.
Wahl DA, Cooper C, Ebeling PR, Eggersdorfer M, Hilger J, Hoffmann K, et al. A global representation of vitamin D status in healthy populations. Arch Osteoporos 2012; 7:155-72; PMID: 23225293; DOI: 10.1007/s11657-012-0093-0.
Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 2011; 96:1911-30; PMID: 21646368; DOI: 10.1210/jc.2011-0385.
Ross AC, Manson JE, Abrams SA, Aloia JF, Brannon PM, Clinton SK, et al. The 2011 report on dietary reference intakes for calcium and vitamin D from the Institute of Medicine: what clinicians need to know. J Clin Endocrinol Metab 2011; 96:53-8; PMID: 21118827; DOI: 10.1210/jc.2010-2704.
Barake M, Daher RT, Salti I, Cortas NK, Al-Shaar L, Habib RH, et al. 25-hydroxyvitamin D assay variations and impact on clinical decision making. J Clin Endocrinol Metab 2012; 97:835-43; PMID: 22238386; DOI: 10.1210/jc.2011-2584.
Sempos CT, Vesper HW, Phinney KW, Thienpont LM, Coates PM. Vitamin D status as an international issue: national surveys and the problem of standardization. Scand J Clin Lab Invest Suppl 2012; 243:32-40; PMID: 22536760.
Dawodu A, Agarwal M, Sankarankutty M, Hardy D, Kochiyil J, Badrinath P. Higher prevalence of vitamin D deficiency in mothers of rachitic than nonrachitic children. J Pediatr 2005; 147:109-11; PMID: 16027707; DOI: 10.1016/j.jpeds.2005.03.001.
Al-Atawi MS, Al-Alwan IA, Al-Mutair AN, Tamim HM, Al-Jurayyan NA. Epidemiology of nutritional rickets in children. Saudi J Kidney Dis Transpl 2009; 20:260-5; PMID: 19237815.
Al-Mustafa ZH, Al-Madan M, Al-Majid HJ, Al-Muslem S, Al-Ateeq S, Al-Ali AK. Vitamin D deficiency and rickets in the Eastern Province of Saudi Arabia. Ann Trop Paediatr 2007; 27:63-7; PMID: 17469734; DOI: 10.1179/146532807X170529.
Narchi H, El Jamil M, Kulaylat N. Symptomatic rickets in adolescence. Arch Dis Child 2001; 84:501-3; PMID: 11369569; DOI: 10.1136/adc.84.6.501.
Soliman AT, El-Dabbagh M, Adel A, Al Ali M, Aziz Bedair EM, Elalaily RK. Clinical responses to a mega-dose of vitamin D3 in infants and toddlers with vitamin D deficiency rickets. J Trop Pediatr 2010; 56:19-26; PMID: 19506025; DOI: 10.1093/tropej/fmp040.
Najada AS, Habashneh MS, Khader M. The frequency of nutritional rickets among hospitalized infants and its relation to respiratory diseases. J Trop Pediatr 2004; 50:364-8; PMID: 15537725; DOI: 10.1093/tropej/50.6.364.
Majid Molla A, Badawi MH, al-Yaish S, Sharma P, el-Salam RS, Molla AM. Risk factors for nutritional rickets among children in Kuwait. Pediatr Int 2000; 42:280-4; PMID: 10881586; DOI: 10.1046/j.1442-200x.2000.01230.x.
Baroncelli GI, Bereket A, El Kholy M, Audì L, Cesur Y, Ozkan B, et al. Rickets in the Middle East: role of environment and genetic predisposition. J Clin Endocrinol Metab 2008; 93:1743-50; PMID: 18285415; DOI: 10.1210/jc.2007-1413.
Dahifar H, Faraji A, Yassobi S, Ghorbani A. Asymptomatic rickets in adolescent girls. Indian J Pediatr 2007; 74:571-5; PMID: 17595501; DOI: 10.1007/s12098-007-0095-x.
Rajah J, Jubeh JA, Haq A, Shalash A, Parsons H. Nutritional rickets and z scores for height in the United Arab Emirates: to D or not to D?. Pediatr Int 2008; 50:424-8; PMID: 18937749; DOI: 10.1111/j.1442-200X.2008.02700.x.
Plotnikoff GA, Quigley JM. Prevalence of severe hypovitaminosis D in patients with persistent, nonspecific musculoskeletal pain. Mayo Clin Proc 2003; 78:1463-70; PMID: 14661675; DOI: 10.4065/78.12.1463.
Holick MF. Vitamin D deficiency: what a pain it is. Mayo Clin Proc 2003; 78:1457-9; PMID: 14661673; DOI: 10.4065/78.12.1457.
Priemel M, von Domarus C, Klatte TO, Kessler S, Schlie J, Meier S, et al. Bone mineralization defects and vitamin D deficiency: histomorphometric analysis of iliac crest bone biopsies and circulating 25-hydroxyvitamin D in 675 patients. J Bone Miner Res 2010; 25:305-12; PMID: 19594303; DOI: 10.1359/jbmr.090728.
Ballane GT, Sfeir JG, Dakik HA, Brown EM, El-Hajj Fuleihan G. Use of recombinant human parathyroid hormone in hypocalcemic cardiomyopathy. Eur J Endocrinol 2012; 166:1113-20; PMID: 22430263; DOI: 10.1530/EJE-11-1094.
Ukinc K. Severe osteomalacia presenting with multiple vertebral fractures: a case report and review of the literature. Endocrine 2009; 36:30-6; PMID: 19543841; DOI: 10.1007/s12020-009-9209-8.
Al-Ali H, Fuleihan GE. Nutritional osteomalacia: substantial clinical improvement and gain in bone density posttherapy. J Clin Densitom 2000; 3:97-101; PMID: 10745306; DOI: 10.1385/JCD:3:1:097.
Sedrani SH. Low 25-hydroxyvitamin D and normal serum calcium concentrations in Saudi Arabia: Riyadh region. Ann Nutr Metab 1984; 28:181-5; PMID: 6610383; DOI: 10.1159/000176801.
Baradaran A, Behradmanesh S, Nasri H. Association of body mass index and serum vitamin D level in healthy Iranian adolescents. Endokrynol Pol 2012; 63:29-33; PMID: 22378095.
Kashi Z, Saeedian Fs, Akha O, Gorgi Ma, Emadi Sf, Zakeri H. Vitamin D deficiency prevalence in summer compared to winter in a city with high humidity and a sultry climate. Endokrynol Pol 2011; 62:249-51; PMID: 21717408.
Hovsepian S, Amini M, Aminorroaya A, Amini P, Iraj B. Prevalence of vitamin D deficiency among adult population of Isfahan City, Iran. J Health Popul Nutr 2011; 29:149-55; PMID: 21608424; DOI: 10.3329/jhpn.v29i2.7857.
Kaykhaei MA, Hashemi M, Narouie B, Shikhzadeh A, Rashidi H, Moulaei N, et al. High prevalence of vitamin D deficiency in Zahedan, southeast Iran. Ann Nutr Metab 2011; 58:37-41; PMID: 21304235; DOI: 10.1159/000323749.
Hosseinpanah F, Pour SH, Heibatollahi M, Moghbel N, Asefzade S, Azizi F. The effects of air pollution on vitamin D status in healthy women: a cross sectional study. BMC Public Health 2010; 10:519; PMID: 20799984; DOI: 10.1186/1471-2458-10-519.
Maddah M, Sharami SH, Neyestani TR. Vitamin D insufficiency among postmenopausal women in urban and rural areas in Guilan, Northern Iran. J Nutr Elder 2009; 28:386-93; PMID: 21184380; DOI: 10.1080/01639360903393523.
Masoompour SM, Sadegholvaad A, Larijani B, Ranjbar-Omrani G. Effects of age and renal function on vitamin D status in men. Arch Iran Med 2008; 11:377-81; PMID: 18588368.
Hosseinpanah F, Rambod M, Hossein-nejad A, Larijani B, Azizi F. Association between vitamin D and bone mineral density in Iranian postmenopausal women. J Bone Miner Metab 2008; 26:86-92; PMID: 18095069; DOI: 10.1007/s00774-007-0791-7.
Hashemipour S, Larijani B, Adibi H, Sedaghat M, Pajouhi M, Bastan-Hagh MH, et al. The status of biochemical parameters in varying degrees of vitamin D deficiency. J Bone Miner Metab 2006; 24:213-8; PMID: 16622734; DOI: 10.1007/s00774-005-0674-8.
Rassouli A, Milanian I, Moslemi-Zadeh M. Determination of serum 25-hydroxyvitamin D(3) levels in early postmenopausal Iranian women: relationship with bone mineral density. Bone 2001; 29:428-30; PMID: 11704493; DOI: 10.1016/S8756-3282(01)00591-9.
Saliba W, Barnett-Griness O, Rennert G. The relationship between obesity and the increase in serum 25(OH)D levels in response to vitamin D supplementation. Osteoporos Int 2013; 24:1447-54; PMID: 22955311; DOI: 10.1007/s00198-012-2129-0.
Saliba W, Barnett O, Stein N, Kershenbaum A, Rennert G. The longitudinal variability of serum 25(OH)D levels. Eur J Intern Med 2012; 23:e106-11; PMID: 22560393; DOI: 10.1016/j.ejim.2012.02.002.
Saliba W, Barnett O, Rennert HS, Rennert G. The risk of all-cause mortality is inversely related to serum 25(OH)D levels. J Clin Endocrinol Metab 2012; 97:2792-8; PMID: 22648653; DOI: 10.1210/jc.2012-1747.
Tsur A, Metzger M, Dresner-Pollak R. Effect of different dress style on vitamin D level in healthy young Orthodox and ultra-Orthodox students in Israel. Osteoporos Int 2011; 22:2895-8; PMID: 21110005; DOI: 10.1007/s00198-010-1492-y.
Saliba W, Barnett O, Rennert HS, Lavi I, Rennert G. The relationship between serum 25(OH)D and parathyroid hormone levels. Am J Med 2011; 124:1165-70; PMID: 22114830; DOI: 10.1016/j.amjmed.2011.07.009.
Steinvil A, Leshem-Rubinow E, Berliner S, Justo D, Finn T, Ish-shalom M, et al. Vitamin D deficiency prevalence and cardiovascular risk in Israel. Eur J Clin Invest 2011; 41:263-8; PMID: 20955219; DOI: 10.1111/j.1365-2362.2010.02403.x.
Oren Y, Shapira Y, Agmon-Levin N, Kivity S, Zafrir Y, Altman A, et al. Vitamin D insufficiency in a sunny environment: a demographic and seasonal analysis. Isr Med Assoc J 2010; 12:751-6; PMID: 21348404.
Nichols EK, Khatib IM, Aburto NJ, Sullivan KM, Scanlon KS, Wirth JP, et al. Vitamin D status and determinants of deficiency among non-pregnant Jordanian women of reproductive age. Eur J Clin Nutr 2012; 66:751-6; PMID: 22415337; DOI: 10.1038/ejcn.2012.25.
Batieha A, Khader Y, Jaddou H, Hyassat D, Batieha Z, Khateeb M, et al. Vitamin D status in Jordan: dress style and gender discrepancies. Ann Nutr Metab 2011; 58:10-8; PMID: 21252499; DOI: 10.1159/000323097.
Mallah E, Hamad M, Elmanaseer M, Qinna N, Idkaidek N, Arafat T, et al. Plasma concentration of 25-hydroxyvitamin D among Jordanians: Effect of biological and habitual factors on vitamin D status. Bio Med Central Clin Path 2011; 11:8.
Mishal AA. Effects of different dress styles on vitamin D levels in healthy young Jordanian women. Osteoporos Int 2001; 12:931-5; PMID: 11804019; DOI: 10.1007/s001980170021.
Gannagé-Yared MH, Maalouf G, Khalife S, Challita S, Yaghi Y, Ziade N, et al. Prevalence and predictors of vitamin D inadequacy amongst Lebanese osteoporotic women. Br J Nutr 2009; 101:487-91; PMID: 18631414; DOI: 10.1017/S0007114508023404.
Arabi A, Baddoura R, Awada H, Salamoun M, Ayoub G, El-Hajj Fuleihan G. Hypovitaminosis D osteopathy: is it mediated through PTH, lean mass, or is it a direct effect?. Bone 2006; 39:268-75; PMID: 16495164; DOI: 10.1016/j.bone.2006.01.140.
Arabi A, Baddoura R, El-Rassi R, El-Hajj Fuleihan G. Age but not gender modulates the relationship between PTH and vitamin D. Bone 2010; 47:408-12; PMID: 20452474; DOI: 10.1016/j.bone.2010.05.002.
Gannagé-Yared MH, Chemali R, Yaacoub N, Halaby G. Hypovitaminosis D in a sunny country: relation to lifestyle and bone markers. J Bone Miner Res 2000; 15:1856-62; PMID: 10977006; DOI: 10.1359/jbmr.2000.15.9.1856.
Ardawi MS, Sibiany AM, Bakhsh TM, Qari MH, Maimani AA. High prevalence of vitamin D deficiency among healthy Saudi Arabian men: relationship to bone mineral density, parathyroid hormone, bone turnover markers, and lifestyle factors. Osteoporos Int 2012; 23:675-86; PMID: 21625888; DOI: 10.1007/s00198-011-1606-1.
Elshafie DE, Al-Khashan HI, Mishriky AM. Comparison of vitamin D deficiency in Saudi married couples. Eur J Clin Nutr 2012; 66:742-5; PMID: 22415335; DOI: 10.1038/ejcn.2012.29.
Kanan RM, Al Saleh YM, Fakhoury HM, Adham M, Aljaser S, Tamimi W. Year-round vitamin D deficiency among Saudi female out-patients. Public Health Nutr 2013; 16:544-8; PMID: 22691699; DOI: 10.1017/S1368980012002947.
Ardawi MS, Qari MH, Rouzi AA, Maimani AA, Raddadi RM. Vitamin D status in relation to obesity, bone mineral density, bone turnover markers and vitamin D receptor genotypes in healthy Saudi pre- and postmenopausal women. Osteoporos Int 2011; 22:463-75; PMID: 20431993; DOI: 10.1007/s00198-010-1249-7.
Alissa EM, Qadi SG, Alhujaili NA, Alshehri AM, Ferns GA. Effect of diet and lifestyle factors on bone health in postmenopausal women. J Bone Miner Metab 2011; 29:725-35; PMID: 21594583; DOI: 10.1007/s00774-011-0274-8.
Sadat-Ali M, Al Elq AH, Al-Turki HA, Al-Mulhim FA, Al-Ali AK. Influence of vitamin D levels on bone mineral density and osteoporosis. Ann Saudi Med 2011; 31:602-8; PMID: 22048506; DOI: 10.4103/0256-4947.87097.
Elsammak MY, Al-Wossaibi AA, Al-Howeish A, Alsaeed J. High prevalence of vitamin D deficiency in the sunny Eastern region of Saudi Arabia: a hospital-based study. East Mediterr Health J 2011; 17:317-22; PMID: 22259890.
Elsammak MY, Al-Wosaibi AA, Al-Howeish A, Alsaeed J. Vitamin d deficiency in Saudi Arabs. Horm Metab Res 2010; 42:364-8; PMID: 20213587; DOI: 10.1055/s-0030-1248296.
Al-Elq AH, Sadat-Ali M, Al-Turki HA, Al-Mulhim FA, Al-Ali AK. Is there a relationship between body mass index and serum vitamin D levels?. Saudi Med J 2009; 30:1542-6; PMID: 19936417.
Sadat-Ali M, AlElq A, Al-Turki H, Al-Mulhim F, Al-Ali A. Vitamin D levels in healthy men in eastern Saudi Arabia. Ann Saudi Med 2009; 29:378-82; PMID: 19700896; DOI: 10.4103/0256-4947.55168.
Al-Turki HA, Sadat-Ali M, Al-Elq AH, Al-Mulhim FA, Al-Ali AK. 25-Hydoxyvitamin D levels among healthy Saudi Arabian women. Saudi Med J 2008; 29:1765-8; PMID: 19082230.
Al Anouti F, Thomas J, Abdel-Wareth L, Rajah J, Grant WB, Haq A. Vitamin D deficiency and sun avoidance among university students at Abu Dhabi, United Arab Emirates. Dermatoendocrinol 2011; 3:235-9; PMID: 22259650; DOI: 10.4161/derm.3.4.16881.
Dawodu A, Kochiyil J, Altaye N. Pilot study of sunlight exposure and vitamin D status in Arab women of childbearing age. East Mediterr Health J 2011; 17:570-4; PMID: 21972479.
Saadi HF, Nagelkerke N, Benedict S, Qazaq HS, Zilahi E, Mohamadiyeh MK, et al. Predictors and relationships of serum 25 hydroxyvitamin D concentration with bone turnover markers, bone mineral density, and vitamin D receptor genotype in Emirati women. Bone 2006; 39:1136-43; PMID: 16814623; DOI: 10.1016/j.bone.2006.05.010.
El Maghraoui A, Ouzzif Z, Mounach A, Rezqi A, Achemlal L, Bezza A, et al. Hypovitaminosis D and prevalent asymptomatic vertebral fractures in Moroccan postmenopausal women. BMC Womens Health 2012; 12:11; PMID: 22531050; DOI: 10.1186/1472-6874-12-11.
Allali F, El Aichaoui S, Khazani H, Benyahia B, Saoud B, El Kabbaj S, et al. High prevalence of hypovitaminosis D in Morocco: relationship to lifestyle, physical performance, bone markers, and bone mineral density. Semin Arthritis Rheum 2009; 38:444-51; PMID: 18336870; DOI: 10.1016/j.semarthrit.2008.01.009.
Bahlous A, Farjallah N, Bouzid K, Klouz A, Mohsni A, Sahli H, et al. Hypovitaminosis D in Tunisian osteoporotic postmenopausal women and the relationship with bone fractures. Tunis Med 2009; 87:188-90; PMID: 19537011.
Meddeb N, Sahli H, Chahed M, Abdelmoula J, Feki M, Salah H, et al. Vitamin D deficiency in Tunisia. Osteoporos Int 2005; 16:180-3; PMID: 15197539; DOI: 10.1007/s00198-004-1658-6.
Al-Othman A, Al-Musharaf S, Al-Daghri NM, Krishnaswamy S, Yusuf DS, Alkharfy KM, et al. Effect of physical activity and sun exposure on vitamin D status of Saudi children and adolescents. BMC Pediatr 2012; 12:92; PMID: 22759399; DOI: 10.1186/1471-2431-12-92.
El-Hajj Fuleihan G, Nabulsi M, Choucair M, Salamoun M, Hajj Shahine C, Kizirian A, et al. Hypovitaminosis D in healthy schoolchildren. Pediatrics 2001; 107:E53; PMID: 11335774; DOI: 10.1542/peds.107.4.e53.
Moussavi M, Heidarpour R, Aminorroaya A, Pournaghshband Z, Amini M. Prevalence of vitamin D deficiency in Isfahani high school students in 2004. Horm Res 2005; 64:144-8; PMID: 16192739; DOI: 10.1159/000088588.
Al-Ghamdi MA, Lanham-New SA, Kahn JA. Differences in vitamin D status and calcium metabolism in Saudi Arabian boys and girls aged 6 to 18 years: effects of age, gender, extent of veiling and physical activity with concomitant implications for bone health. Public Health Nutr 2012; 15:1845-53; PMID: 22348990; DOI: 10.1017/S1368980011003612.
Neyestani TR, Hajifaraji M, Omidvar N, Eshraghian MR, Shariatzadeh N, Kalayi A, et al. High prevalence of vitamin D deficiency in school-age children in Tehran, 2008: a red alert. Public Health Nutr 2012; 15:324-30; PMID: 21356149; DOI: 10.1017/S1368980011000188.
Olang B, Naghavi M, Bastani D, Strandvik B, Yngve A. Optimal vitamin A and suboptimal vitamin D status are common in Iranian infants. Acta Paediatr 2011; 100:439-44; PMID: 20950411; DOI: 10.1111/j.1651-2227.2010.02058.x.
Abdul-Razzak KK, Ajlony MJ, Khoursheed AM, Obeidat BA. Vitamin D deficiency among healthy infants and toddlers: a prospective study from Irbid, Jordan. Pediatr Int 2011; 53:839-45; PMID: 21507148; DOI: 10.1111/j.1442-200X.2011.03388.x.
Razzaghy-Azar M, Shakiba M. Assessment of vitamin D status in healthy children and adolescents living in Tehran and its relation to iPTH, gender, weight and height. Ann Hum Biol 2010; 37:692-701; PMID: 20166840; DOI: 10.3109/03014460903527348.
Dawodu A, Agarwal M, Hossain M, Kochiyil J, Zayed R. Hypovitaminosis D and vitamin D deficiency in exclusively breast-feeding infants and their mothers in summer: a justification for vitamin D supplementation of breast-feeding infants. J Pediatr 2003; 142:169-73; PMID: 12584539; DOI: 10.1067/mpd.2003.63.
Ardestani PM, Salek M, Keshteli AH, Nejadnik H, Amini M, Hosseini SM, et al. Vitamin D status of 6- to 7-year-old children living in Isfahan, Iran. Endokrynol Pol 2010; 61:377-82; PMID: 20806182.
Narchi H, Kochiyil J, Zayed R, Abdulrazzak W, Agarwal M. Maternal vitamin D status throughout and after pregnancy. J Obstet Gynaecol 2010; 30:137-42; PMID: 20143971; DOI: 10.3109/01443610903315652.
Ghergherechi R, Hazhir N, Tabrizi A. Comparison of vitamin D deficiency and secondary hyperparathyroidism in obese and non-obese children and adolescents. Pak J Biol Sci 2012; 15:147-51; PMID: 22866545; DOI: 10.3923/pjbs.2012.147.151.
Arabi A, Baddoura R, El-Rassi R, El-Hajj Fuleihan G. PTH level but not 25 (OH) vitamin D level predicts bone loss rates in the elderly. Osteoporos Int 2012; 23:971-80; PMID: 21656018; DOI: 10.1007/s00198-011-1659-1.
van der Meer IM, Middelkoop BJ, Boeke AJ, Lips P. Prevalence of vitamin D deficiency among Turkish, Moroccan, Indian and sub-Sahara African populations in Europe and their countries of origin: an overview. Osteoporos Int 2011; 22:1009-21; PMID: 20461360; DOI: 10.1007/s00198-010-1279-1.
Moreno-Reyes R, Carpentier YA, Boelaert M, El Moumni K, Dufourny G, Bazelmans C, et al. Vitamin D deficiency and hyperparathyroidism in relation to ethnicity: a cross-sectional survey in healthy adults. Eur J Nutr 2009; 48:31-7; PMID: 19030910; DOI: 10.1007/s00394-008-0756-1.
Jazar A, Takruri H, Khuri-Bulos N. Vitamin D status in a sample of preschool children aged from 1 to 6 years visiting the pediatrics clinic at Jordan University hospital. J Med J 2011; 45:308-16.
Gharaibeh MA, Stoecker BJ. Assessment of serum 25(OH)D concentration in women of childbearing age and their preschool children in Northern Jordan during summer. Eur J Clin Nutr 2009; 63:1320-6; PMID: 19707220; DOI: 10.1038/ejcn.2009.99.
El-Hajj Fuleihan G, Vieth R. Vitamin D insufficiency and musculoskeletal health in children and adolescents. International Congress Series 2007; 1297:91-108.
El-Hajj Fuleihan G, Nabulsi M, Tamim H, Maalouf J, Salamoun M, Khalife H, et al. Effect of vitamin D replacement on musculoskeletal parameters in school children: a randomized controlled trial. J Clin Endocrinol Metab 2006; 91:405-12; PMID: 16278262; DOI: 10.1210/jc.2005-1436.
Rajah J, Haq A, Pettifor JM. Vitamin D and calcium status in urban children attending an ambulatory clinic service in the United Arab Emirates. Dermatoendocrinol 2012; 4:39-43; PMID: 22870351; DOI: 10.4161/derm.18250.
Kensarah O, Azzeh F, Vitamin D. Status of Healthy School Children from Western Saudi Arabia. Pakistan Journal of Nutrition 2012; 11:288-92; DOI: 10.3923/pjn.2012.288.292.
Bener A, Al-Ali M, Hoffmann GF. Vitamin D deficiency in healthy children in a sunny country: associated factors. Int J Food Sci Nutr 2009; 60:60-70; PMID: 18946796; DOI: 10.1080/09637480802400487.
Dawodu A, Dawson KP, Amirlak I, Kochiyil J, Agarwal M, Badrinath P. Diet, clothing, sunshine exposure and micronutrient status of Arab infants and young children. Ann Trop Paediatr 2001; 21:39-44; PMID: 11284245; DOI: 10.1080/02724930020028902.
Racinais S, Hamilton B, Li CK, Grantham J. Vitamin D and physical fitness in Qatari girls. Arch Dis Child 2010; 95:854-5; PMID: 20554768; DOI: 10.1136/adc.2009.163238.
El-Hajj Fuleihan G, Rahme M, Bassil D. Do Desirable Vitamin D Levels Vary Globally? In: Burckhardt P, Dawson-Hughes B, and Weaver C, eds. Nutritional Influences on Bone Health – 8th International Symposium. Springer Science publisher, 2012 (In Press).
Gernand AD, Simhan HN, Klebanoff MA, Bodnar LM. Maternal serum 25-hydroxyvitamin D and measures of newborn and placental weight in a U.S. multicenter cohort study. J Clin Endocrinol Metab 2013; 98:398-404; PMID: 23162094; DOI: 10.1210/jc.2012-3275.
Kazemi A, Sharifi F, Jafari N, Mousavinasab N. High prevalence of vitamin D deficiency among pregnant women and their newborns in an Iranian population. J Womens Health (Larchmt) 2009; 18:835-9; PMID: 19514825; DOI: 10.1089/jwh.2008.0954.
Asemi Z, Taghizadeh M, Sarahroodi S, Jazayeri S, Tabasi Z, Seyyedi F. Assessment of the relationship of vitamin D with serum antioxidant vitamins E and A and their deficiencies in Iranian pregnant women. Saudi Med J 2010; 31:1119-23; PMID: 20953527.
Bassir M, Laborie S, Lapillonne A, Claris O, Chappuis MC, Salle BL. Vitamin D deficiency in Iranian mothers and their neonates: a pilot study. Acta Paediatr 2001; 90:577-9; PMID: 11430721; DOI: 10.1111/j.1651-2227.2001.tb00802.x.
Mukamel MN, Weisman Y, Somech R, Eisenberg Z, Landman J, Shapira I, et al. Vitamin D deficiency and insufficiency in Orthodox and non-Orthodox Jewish mothers in Israel. Isr Med Assoc J 2001; 3:419-21; PMID: 11433634.
Molla AM, Al Badawi M, Hammoud MS, Molla AM, Shukkur M, Thalib L, et al. Vitamin D status of mothers and their neonates in Kuwait. Pediatr Int 2005; 47:649-52; PMID: 16354218; DOI: 10.1111/j.1442-200x.2005.02141.x.
Shea MK, Benjamin EJ, Dupuis J, Massaro JM, Jacques PF, D’Agostino RB, et al. Genetic and non-genetic correlates of vitamins K and D. Eur J Clin Nutr 2009; 63:458-64; PMID: 18030310; DOI: 10.1038/sj.ejcn.1602959.
Wang TJ, Zhang F, Richards JB, Kestenbaum B, van Meurs JB, Berry D, et al. Common genetic determinants of vitamin D insufficiency: a genome-wide association study. Lancet 2010; 376:180-8; PMID: 20541252; DOI: 10.1016/S0140-6736(10)60588-0.
Signorello LB, Shi J, Cai Q, Zheng W, Williams SM, Long J, et al. Common variation in vitamin D pathway genes predicts circulating 25-hydroxyvitamin D Levels among African Americans. PLoS One 2011; 6:e28623; PMID: 22205958; DOI: 10.1371/journal.pone.0028623.
Cheng JB, Levine MA, Bell NH, Mangelsdorf DJ, Russell DW. Genetic evidence that the human CYP2R1 enzyme is a key vitamin D 25-hydroxylase. Proc Natl Acad Sci U S A 2004; 101:7711-5; PMID: 15128933; DOI: 10.1073/pnas.0402490101.
Levine M, Dang A, Ding C, Fischer P, Singh R, Thacher T. Tropical rickets in Nigeria: Mutation of the CYP2R1 gene encoding vitamin D 25-hydroxylase as a cause of vitamin D dependent rickets. Bone 2007; 40:S60-1; DOI: 10.1016/j.bone.2007.04.079.
Dong Q, Miller WL. Vitamin D 25-hydroxylase deficiency. Mol Genet Metab 2004; 83:197-8; PMID: 15464435; DOI: 10.1016/j.ymgme.2004.07.006.
Abdullah MA, Salhi HS, Bakry LA, Okamoto E, Abomelha AM, Stevens B, et al. Adolescent rickets in Saudi Arabia: a rich and sunny country. J Pediatr Endocrinol Metab 2002; 15:1017-25; PMID: 12199329; DOI: 10.1515/JPEM.2002.15.7.1017.
Al Mutair AN, Nasrat GH, Russell DW. Mutation of the CYP2R1 vitamin D 25-hydroxylase in a Saudi Arabian family with severe vitamin D deficiency. J Clin Endocrinol Metab 2012; 97:E2022-5; PMID: 22855339; DOI: 10.1210/jc.2012-1340.
Holick MF. The vitamin D deficiency pandemic and consequences for nonskeletal health: mechanisms of action. Mol Aspects Med 2008; 29:361-8; PMID: 18801384; DOI: 10.1016/j.mam.2008.08.008.
Sempos C, Vesper H, Phinny K, Thienpont L, Coates P. VDSP. Is there a U- or J-shaped Association between 25-Hydroxyvitamin D and All-Cause Mortality?. Results from the US Nationally Representative NHANES, JCEM 2012; .
Olama SM, Senna MK, Elarman MM, Elhawary G. Serum vitamin D level and bone mineral density in premenopausal Egyptian women with fibromyalgia. Rheumatol Int 2013; 33:185-92; PMID: 22311432; DOI: 10.1007/s00296-012-2361-0.
El Husseiny NM, Fahmy HM, Mohamed WA, Amin HH. Relationship between vitamin D and IL-23, IL-17 and macrophage chemoattractant protein-1 as markers of fibrosis in hepatitis C virus Egyptians. World J Hepatol 2012; 4:242-7; PMID: 22993666; DOI: 10.4254/wjh.v4.i8.242.
Schaalan MF, Mohamed WA, Amin HH. Vitamin D deficiency: correlation to interleukin-17, interleukin-23 and PIIINP in hepatitis C virus genotype 4. World J Gastroenterol 2012; 18:3738-44; PMID: 22851868; DOI: 10.3748/wjg.v18.i28.3738.
Hamza RT, Awwad KS, Ali MK, Hamed AI. Reduced serum concentrations of 25-hydroxy vitamin D in Egyptian patients with systemic lupus erythematosus: relation to disease activity. Med Sci Monit 2011; 17:CR711-8; PMID: 22129903; DOI: 10.12659/MSM.882131.
Alsayed A, Gad A, Azab A. Serum 25-hydroxyvitamin D concentrations and metabolic syndrome in Egyptian men. J Med Sci 2007; 7:850-4; DOI: 10.3923/jms.2007.850.854.
Khalili H, Talasaz AH, Salarifar M. Serum vitamin D concentration status and its correlation with early biomarkers of remodeling following acute myocardial infarction. Clin Res Cardiol 2012; 101:321-7; PMID: 22159952; DOI: 10.1007/s00392-011-0394-0.
Hosseinpanah F, Yarjanli M, Sheikholeslami F, Heibatollahi M, Eskandary PS, Azizi F. Associations between vitamin D and cardiovascular outcomes; Tehran Lipid and Glucose Study. Atherosclerosis 2011; 218:238-42; PMID: 21676397; DOI: 10.1016/j.atherosclerosis.2011.05.016.
Bonakdar ZS, Jahanshahifar L, Jahanshahifar F, Gholamrezaei A. Vitamin D deficiency and its association with disease activity in new cases of systemic lupus erythematosus. Lupus 2011; 20:1155-60; PMID: 21680639; DOI: 10.1177/0961203311405703.
Heidari B, Shirvani JS, Firouzjahi A, Heidari P, Hajian-Tilaki KO. Association between nonspecific skeletal pain and vitamin D deficiency. Int J Rheum Dis 2010; 13:340-6; PMID: 21199469; DOI: 10.1111/j.1756-185X.2010.01561.x.
Garakyaraghi M, Kerdegari M, Siavash M. Calcium and vitamin D status in heart failure patients in Isfahan, Iran. Biol Trace Elem Res 2010; 135:67-73; PMID: 19690819; DOI: 10.1007/s12011-009-8492-9.
Bonakdaran S, Varasteh AR. Correlation between serum 25 hydroxy vitamin D3 and laboratory risk markers of cardiovascular diseases in type 2 diabetic patients. Saudi Med J 2009; 30:509-14; PMID: 19370277.
Omrani GR, Masoompour SM, Sadegholvaad A, Larijani B. Effect of menopause and renal function on vitamin D status in Iranian women. East Mediterr Health J 2006; 12:188-95; PMID: 17037237.
Saliba W, Lavi I, Rennert HS, Rennert G. Vitamin D status in primary hyperparathyroidism. Eur J Intern Med 2012; 23:88-92; PMID: 22153538; DOI: 10.1016/j.ejim.2011.07.008.
Amital H, Szekanecz Z, Szücs G, Dankó K, Nagy E, Csépány T, et al. Serum concentrations of 25-OH vitamin D in patients with systemic lupus erythematosus (SLE) are inversely related to disease activity: is it time to routinely supplement patients with SLE with vitamin D?. Ann Rheum Dis 2010; 69:1155-7; PMID: 20439290; DOI: 10.1136/ard.2009.120329.
Bener A, Alsaied A, Al-Ali M, Al-Kubaisi A, Basha B, Abraham A, et al. High prevalence of vitamin D deficiency in type 1 diabetes mellitus and healthy children. Acta Diabetol 2009; 46:183-9; PMID: 18846317; DOI: 10.1007/s00592-008-0071-6.
Bin-Abbas BS, Jabari MA, Issa SD, Al-Fares AH, Al-Muhsen S. Vitamin D levels in Saudi children with type 1 diabetes. Saudi Med J 2011; 32:589-92; PMID: 21666940.
Al-Daghri NM, Al-Attas OS, Al-Okail MS, Alkharfy KM, Al-Yousef MA, Nadhrah HM, et al. Severe hypovitaminosis D is widespread and more common in non-diabetics than diabetics in Saudi adults. Saudi Med J 2010; 31:775-80; PMID: 20635011.
Banajeh SM. Nutritional rickets and vitamin D deficiency--association with the outcomes of childhood very severe pneumonia: a prospective cohort study. Pediatr Pulmonol 2009; 44:1207-15; PMID: 19911367; DOI: 10.1002/ppul.21121.
Shakinba M, Tefagh S, Nafei Z. The optimal dose of vitamin D in growing girls during academic years: a randomized trial. Turk J Med Sci 2011; 41:33-7.
Ghazi AA, Hosseinpanah F, M Ardakani E, Ghazi S, Hedayati M, Azizi F. Effects of different doses of oral cholecalciferol on serum 25(OH)D, PTH, calcium and bone markers during fall and winter in schoolchildren. Eur J Clin Nutr 2010; 64:1415-22; PMID: 20823895; DOI: 10.1038/ejcn.2010.169.
Gotsman I, Shauer A, Zwas DR, Hellman Y, Keren A, Lotan C, et al. Vitamin D deficiency is a predictor of reduced survival in patients with heart failure; vitamin D supplementation improves outcome. Eur J Heart Fail 2012; 14:357-66; PMID: 22308011; DOI: 10.1093/eurjhf/hfr175.
Soliman AT, Adel A, Wagdy M, Alali M, Aziz Bedair EM. Manifestations of severe vitamin D deficiency in adolescents: effects of intramuscular injection of a megadose of cholecalciferol. J Trop Pediatr 2011; 57:303-6; PMID: 20427425; DOI: 10.1093/tropej/fmq028.
Al-Daghri NM, Alkharfy KM, Al-Saleh Y, Al-Attas OS, Alokail MS, Al-Othman A, et al. Modest reversal of metabolic syndrome manifestations with vitamin D status correction: a 12-month prospective study. Metabolism 2012; 61:661-6; PMID: 22075268; DOI: 10.1016/j.metabol.2011.09.017.
Rajah J, Abdel-Wareth L, Haq A. Failure of alphacalcidol (1alpha-hydroxyvitamin D3) in treating nutritional rickets and the biochemical response to ergocalciferol. J Steroid Biochem Mol Biol 2010; 121:273-6; PMID: 20398760; DOI: 10.1016/j.jsbmb.2010.03.075.
Saadi HF, Dawodu A, Afandi BO, Zayed R, Benedict S, Nagelkerke N. Efficacy of daily and monthly high-dose calciferol in vitamin D-deficient nulliparous and lactating women. Am J Clin Nutr 2007; 85:1565-71; PMID: 17556694.
Rajah J, Jubeh JA, Haq A, Shalash A, Parsons H. Nutritional rickets and z scores for height in the United Arab Emirates: to D or not to D?. Pediatr Int 2008; 50:424-8; PMID: 18937749; DOI: 10.1111/j.1442-200X.2008.02700.x.
Saadi HF, Dawodu A, Afandi B, Zayed R, Benedict S, Nagelkerke N, et al. Effect of combined maternal and infant vitamin D supplementation on vitamin D status of exclusively breastfed infants. Matern Child Nutr 2009; 5:25-32; PMID: 19161542; DOI: 10.1111/j.1740-8709.2008.00145.x.
Porhashem Z, Biani M, Noreddini H, Bijani A, Hosseini S. Prevalence of osteoporosis and its association with serum vitamin D level in older people in Amirkola, North of Iran. Caspian J Intern Med 2012; 3:347-53.
Arabi A, Mahfoud Z, Zahed L, El-Onsi L, El-Hajj Fuleihan G. Effect of age, gender and calciotropic hormones on the relationship between vitamin D receptor gene polymorphisms and bone mineral density. Eur J Clin Nutr 2010; 64:383-91; PMID: 20145667; DOI: 10.1038/ejcn.2010.5.
El-Hajj Fuleihan G. Can the sunshine vitamin melt the fat?. Metabolism 2012; 61:603-10; PMID: 22304833; DOI: 10.1016/j.metabol.2011.12.006.
Fahed AC, El-Hage-Sleiman AK, Farhat TI, Nemer GM. Diet, genetics, and disease: a focus on the middle East and north Africa region. J Nutr Metab 2012; 2012:109037; PMID: 22536488; DOI: 10.1155/2012/109037.
Mehio Sibai A, Nasreddine L, Mokdad AH, Adra N, Tabet M, Hwalla N. Nutrition transition and cardiovascular disease risk factors in Middle East and North Africa countries: reviewing the evidence. Ann Nutr Metab 2010; 57:193-203; PMID: 21088386; DOI: 10.1159/000321527.
Shaygannejad V, Golabchi K, Haghighi S, Dehghan H, Moshayedi A. A Comparative Study of 25 (OH) Vitamin D Serum Levels in Patients with Multiple Sclerosis and Control Group in Isfahan, Iran. Int J Prev Med 2010; 1:195-201; PMID: 21566791.
Lerner A, Shapira Y, Agmon-Levin N, Pacht A, Ben-Ami Shor D, López HM, et al. The clinical significance of 25OH-Vitamin D status in celiac disease. Clin Rev Allergy Immunol 2012; 42:322-30; PMID: 21210250; DOI: 10.1007/s12016-010-8237-8.
Lerch C, Meissner T. Interventions for the prevention of nutritional rickets in term born children. Cochrane Database Syst Rev 2007; :CD006164; PMID: 17943890.
Cesur Y, Caksen H, Gündem A, Kirimi E, Odabaş D. Comparison of low and high dose of vitamin D treatment in nutritional vitamin D deficiency rickets. J Pediatr Endocrinol Metab 2003; 16:1105-9; PMID: 14594170; DOI: 10.1515/JPEM.2003.16.8.1105.
Winzenberg T, Powell S, Shaw KA, Jones G. Effects of vitamin D supplementation on bone density in healthy children: systematic review and meta-analysis. BMJ 2011; 342:c7254; PMID: 21266418; DOI: 10.1136/bmj.c7254.
Arabi A, Zahed L, Mahfoud Z, El-Onsi L, Nabulsi M, Maalouf J, et al. Vitamin D receptor gene polymorphisms modulate the skeletal response to vitamin D supplementation in healthy girls. Bone 2009; 45:1091-7; PMID: 19647104; DOI: 10.1016/j.bone.2009.07.074.
Kumar GT, Sachdev HS, Chellani H, Rehman AM, Singh V, Arora H, et al. Effect of weekly vitamin D supplements on mortality, morbidity, and growth of low birthweight term infants in India up to age 6 months: randomised controlled trial. BMJ 2011; 342:d2975; PMID: 21628364; DOI: 10.1136/bmj.d2975.
Hollis BW, Johnson D, Hulsey TC, Ebeling M, Wagner CL. Vitamin D supplementation during pregnancy: double-blind, randomized clinical trial of safety and effectiveness. J Bone Miner Res 2011; 26:2341-57; PMID: 21706518; DOI: 10.1002/jbmr.463.
Harvey NC, Javaid K, Bishop N, Kennedy S, Papageorghiou AT, Fraser R, et al. MAVIDOS Maternal Vitamin D Osteoporosis Study: study protocol for a randomized controlled trial. Trials 2012; 13:13; PMID: 22314083; DOI: 10.1186/1745-6215-13-13.
Martineau AR, Nhamoyebonde S, Oni T, Rangaka MX, Marais S, Bangani N, et al. Reciprocal seasonal variation in vitamin D status and tuberculosis notifications in Cape Town, South Africa. Proc Natl Acad Sci U S A 2011; 108:19013-7; PMID: 22025704; DOI: 10.1073/pnas.1111825108.
Martineau AR, Timms PM, Bothamley GH, Hanifa Y, Islam K, Claxton AP, et al. High-dose vitamin D(3) during intensive-phase antimicrobial treatment of pulmonary tuberculosis: a double-blind randomised controlled trial. Lancet 2011; 377:242-50; PMID: 21215445; DOI: 10.1016/S0140-6736(10)61889-2.
Coussens AK, Wilkinson RJ, Hanifa Y, Nikolayevskyy V, Elkington PT, Islam K, et al. Vitamin D accelerates resolution of inflammatory responses during tuberculosis treatment. Proc Natl Acad Sci U S A 2012; 109:15449-54; PMID: 22949664; DOI: 10.1073/pnas.1200072109.
See also VitaminDWiki
Opportunity to give 400 IU of vitamin D to children at risk of rickets
Rare Nutritional Rickets increased 10X in 20 years – Feb 2013
Africa category listing has items along with related searches
Wikipedia Nov 2013
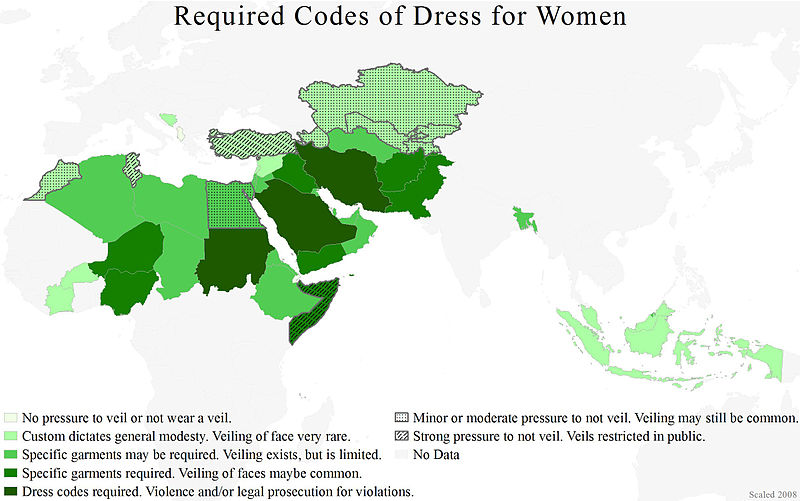
short URL - http://is.gd/qh0gtT
