Problems with low UV and vitamin D in Scotland
Figure 2 from The Scots' Paradox - below
See also VitaminDWiki
Vitamin D - Experts' Forum – presentations April 2011 including one by Oliver Gillie : PDF and Video
Sunlight Robbery - Gillie Nov 2010 full text
Three free vitamin D books - focus on Scotland 2004-2008 All by Oliver Gillie
UK Health Policy regarding Vitamin D - Dr Oliver Gillie Video July 2011
Vitamin D insufficiency in UK youths – 37X more likely if dark skin – July 2011
- Dark Skin is a BIG PROBLEM = 37X more likely to be vitamin D insufficient in the UK
UK summers are not long enough to re-stock vitamin D – Aug 2010
Vitamin D in the UK = Vitamin D Association
Vitamin D UK 45 year olds by Hyppönen
Scotland and Vitamin D Multiple Sclerosis
Many reasons why vitamin D deficiency has become epidemic in past 30-40 years
Low vitamin D associated with low socio-economics in UK – Aug 2011 Dr. Grimes
Mother and father on trial for infant death – set free – death was due to rickets – Dec 2011 UK
Scotts having extremely low vitamin D got no or only minimal treatment – Feb 2012
Scottish doctors ignoring vitamin D? VitaminDWiki Blog - Feb 2012
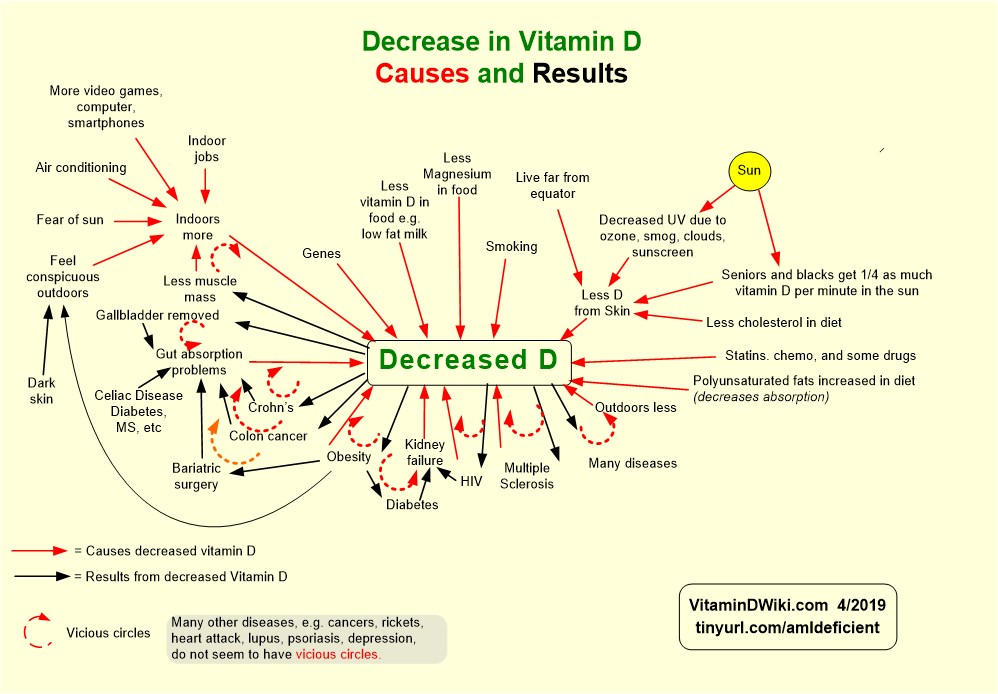
Vitamin D Deficiency has the following chart
Chronic lymphocytic leukaemia and Vitamin D and Dr. Gillie - Aug 2014
When there is little sun, you might consider wearing a shirt which allows sun to get to the skin
- TanThrough Shirt (be sure to not wear a tee shirt)

See also Web
BBC video on lack of vitamin D- Jan 2012 includes a short comment by Gillie __
BBC video on MS and lack of vitamin D in Scotland Dec 2011
- Prof George Ebers request adding Vitamin D, Govt waiting till 2014 Scientific Advisory Commission on Nutrition report
- Increasing requests for vitamin D measurement: costly, confusing, and without credibility
- Jan 2012 Lancet, authors are in Scotland, no abstract
The Scots' Paradox: Can Sun Exposure, or Lack of it, Explain Major Paradoxes in Epidemiology?
Anticancer Research 32-. 237-248 (2012), Oliver Gillie , Health Research Forum, London, U.K.
Anticancer Research Journal has>248 articles on vitamin D
Abstract. Five epidemiological paradoxes that have puzzled epidemiologists for a decade or more can be explained by the UVB-vitamin D hypothesis. The Scots' Paradox is examined in detail as an example. Many subsidiary factors varying over time and place influence the amount of UVB which reaches the skin of individuals and so the amount of vitamin D synthesised, while other factors influence the amount ingested. These factors are plotted leading to a common pathway that ends in vitamin D insufficiency and consequent disease. Examples suggest that the factors interact to increase mortality in Scotland in a way consistent with causation according to the criteria of Bradford Hill. It is suggested that different degrees of vitamin D insufficiency in populations can explain important differences in the health of nations and resolve health paradoxes. The analysis also shows that vitamin D insufficiency is a consequence of industrialisation and, like other consequences of industrial growth, such as water and air pollution, needs to be corrected by public health measures. Direct intervention with use of supplements and fortification of foods with vitamin D can be expected to provide considerable health gains, but progress will be slow until there is greater recognition of the vitamin D health crisis by the public, professionals and politicians. Health professionals need to be trained and motivated to encourage use of supplements, particularly by pregnant and nursing mothers, and infants. The importance of open sunny spaces and clean air that allows full penetration of UVB needs to be recognised by city planners and politicians. New advice and new fashions are needed to encourage maximum exposure of skin to summer sun without burning. Use of sunlamps to boost vitamin D synthesis could be useful.
Correspondence to: Oliver Gillie, B.Sc., Ph.D., FRSA, Health Research Forum, 68 Whitehall Park, London N19 3TN, U.K. Tel. +44 2075619677. Mobile. +44 7774995805,
olivergillie@blueyonder.co.uk /www.healthresearchforum.org.uk
A number of paradoxes have been identified which vividly illustrate the difficulty we have in accounting for differences in incidence of disease and mortality between nations. for example the French paradox (1, 2), the Albanian paradox (3 4), the Swiss paradox (5) and the Greek or Italian paradox (6, 7). Until these national paradoxes have been explained, we cannot be satisfied that the major causes of the most common diseases, together with regional variations, are well understood by science (5).
Sun exposure and the vitamin D levels of populations are risk factors that contribute to mortality and most likely to national differences in incidence of disease but, hitherto, they have not been widely considered in attempting to explain these national paradoxes. In this article, it is suggested that variation in sun exposure and hence in vitamin D sufficiency play an important part in explaining five such paradoxes. The suggestion is illustrated by detailed consideration of the Scots' paradox (7). Simply stated, this paradox, also known as the 'Scottish Effect' (8), tells us that the mortality of Scots is higher than that of the English across all social classes even though many aspects of culture, environment and health provision are the same.
In a bold attempt to account for the Scots' paradox, 17 different hypotheses have been considered by the Glasgow Centre for Population Health (GCPH) (9).
Hypotheses considered include social alienation, deindustrialization, sectarianism and limited social mobility.
The 17th and last hypothesis, a variation of the UVB-vitamin D hypothesis, is the suggestion by the present author that Scotland's northern location and cloudy maritime climate provide little sunlight and hence Scots are at risk of having low serum levels of vitamin D (10). It is suggested that this in turn causes an increased risk of serious disease, so accounting for Scotland's relatively high mortality (7, 10).
In this article I endeavor to show that the UVB-vitamin D hypothesis satisfies criteria required for an explanation of the Scots' paradox. If this supposition is correct, then important improvements in Scots' health relative to the English, and other nationalities, may be obtained by relatively straightforward public health measures such as fortification of food with vitamin D, use of vitamin D supplements, reduction in air pollution and careful sunlamp treatments.
Geography and Climate Provide Little Sun in Scotland
Sunlight, or more specifically UVB radiation, is our major source of vitamin D. A normal Western diet cannot provide more than about 10% of the optimum vitamin D supply (11, 12). Scotland has an extreme climate so far as sunlight is concerned, probably more extreme than that of any other industrialised country (12, 13). This is because Scotland (latitude 55° to 61° north) is not only located relatively far north but also has a very cloudy maritime climate. This is the result of the prevailing westerly wind which brings in moist air from the Atlantic. Much of England (latitude 50° - 55° north) is given some protection from this moist westerly air stream by the Irish landmass and the mountains of Wales and Cumbria which draw down precipitation. On the other hand the highly populated Glasgow/Edinburgh corridor (latitude 56° north) is open to the Atlantic winds on the west which bring in a great deal of cloud and rain that obscure the sun.
These geographic and climatic considerations have a profound effect on the amount of sunshine and, more particularly, on UVB reaching ground level in Scotland (Figure 1) (12-14). UVB is the part of the spectrum that catalyses vitamin D synthesis and so the special geographic/climatic situation of Scotland leads to there being low levels of serum vitamin D in the Scottish population as shown in surveys (12, 14, 15). In summer, 75% of Scots aged 45 years fail to obtain an optimum level of vitamin D (75 nmol/l) compared with 57% in southern England (16). While in winter 92% of Scots aged 45 fail to have the optimal level compared with 86% of people in southern England. Another study of 2235 healthy Scots aged 21-82 years showed that 34.5% were severely deficient in vitamin D (<25 nmol/l) while only a third of participants had a level of 25 (OH)D greater than 40 nmol/l (15). Furthermore 160 children in the west of Scotland were found to be suffering from obvious vitamin D deficiency in the period between 2002 and 2008; 40% of them had bowed legs (17).
Most public water supplies in Scotland are 'soft' (i.e. low in calcium) compared with southern England where much of the public water supply is 'hard' (18). Scottish water has low levels of calcium because the water comes from mountain and moorland sources that percolate through peat which absorbs calcium salts. This is of interest because vitamin D is needed for absorption of calcium in the bowel (19). If the diet is relatively rich in calcium, it has a sparing action which frees vitamin D for other uses, reducing the overall optimal vitamin D requirement (20-23). Thus soft water puts Scots at a further disadvantage when it comes to effective body levels of vitamin D.
Diseases Associated with Insufficient Vitamin D and Sunshine
The immediate causes of high Scottish mortality are known. high rates of alcohol and drug-related deaths, suicide, violence, cardiovascular disease, stroke and cancer (9). The last three of these are associated in numerous studies with low levels of vitamin D and sunshine as outlined below. colorectal cancer is one of the commonest malignancies and low serum vitamin D is now widely believed to be an important factor in its pathogenesis (24), although other factors, such as the amount of dietary fibre, may also be involved. The evidence that low serum levels of vitamin D are a risk factor for other types of cancer, heart disease and stroke is considered by many experts in the field to be compelling (25-32). Diabetes (33) and a number of other diseases (10) linked to low vitamin D levels might be usefully investigated as possible causes of excess deaths in Scotland.
Whether or not low vitamin D is a direct cause of these diseases is still open to some debate. Direct support for the hypothesis comes from evidence showing that low levels of vitamin D are associated with greater all-cause mortality (3436). In addition, according to a meta-analysis (37), supplementation with vitamin D reduces mortality in clinical trials testing benefits for patients with bone disease or prevention of fractures. A Cochrane Review of 50 randomised trials with 94,148 participants has extended this approach confirming a significant reduction in mortality of individuals taking vitamin D3 (38).
The "high rates of alcohol and drug-related deaths, suicide, and violence..." in Scotland, referred to in the GCPH report (9), may be accounted for, at least in part, by the UVB-vitamin D hypothesis. Insufficient vitamin D appears to be a risk factor for a number of psychiatric diseases which in turn are associated with vulnerability to premature mortality caused by drugs, alcohol and violence. Insufficient vitamin D at various crucial periods of development from pregnancy to puberty or later has been linked to schizophrenia (39), autism (40), depression (41, 42), cognitive deficit (43), Parkinson's disease (44), dementia Alzheimer's disease (45), and has been reviewed as a major contributor to neurodegenerative disease (46). Vitamin D is known to play a crucial role in early brain development (47). Furthermore deficiency of vitamin D in pregnancy is known to be common in Scotland because it is a risk factor for multiple sclerosis (MS) (48, 49) which is more common in Scotland than any other country surveyed (49).
Factors Affecting Temporal and Geographic Variation of Vitamin D Levels in Scotland
Scots' mortality began to diverge from the rest of Europe in 1950, failing to improve as rapidly as in other countries. The GCPH report states that it is "unclear how vitamin D can be an important cause [of the Scottish effect] unless there has been a temporal change in exposure" (9). The report also argues that the UVB-vitamin D hypothesis fails to explain why "more northern areas [of Scotland] are less affected [by ill health] than Glasgow". A number of factors that influence vitamin D synthesis and uptake are outlined below. consideration of the way these factors interact shows how vitamin D levels of the population may have varied over time, particularly since 1950, and how they may vary in different parts of Scotland.
Changes after 1950. The relatively high mortality of the Scottish population after 1950 compared to that of other industrial countries was in large part the result of an epidemic of coronary heart disease which affected all modern industrial countries (50). The peak in Europe and North America was observed about 1970, with 550 deaths per 100,000 in the UK (51). In Scotland the peak in men reached 960 deaths per 100,000, higher than anywhere else, possibly because of the particularly low level of vitamin D in the population (27, 29, 30). After 1970, mortality dropped rapidly to fewer than 25 per 100,000, which is the UK average today (52). However this epidemic and its extreme impact in Scotland cannot account for the Scottish paradox because the difference in mortality between Scotland and England today is larger than it was in 1950 (9).
Disease due to deficiency of vitamin D appears to occur when blood levels of the vitamin drop below certain physiological thresholds (53). Indeed it seems likely that there is a series of threshold levels of serum vitamin D below which different diseases may emerge, according to age and duration of deficiency. Secular changes, such as advice to avoid the sun, are likely to take a greater proportion of Scots to blood levels of vitamin D below thresholds for disease compared with such changes in other countries where the base level of vitamin D is higher. Since 1950 a number of these factors that lower vitamin D levels in individuals and populations have come into play and may have had a disproportionate effect in Scotland as a result of threshold effects. These are discussed below.
Latitude gradients. A clear North/South gradient has been found in hospital admissions for MS in Scotland. A similar North/South gradient for MS has been found in a large number of studies in both the northern and southern hemispheres (54). The effect of latitude has been explained as acting through intensity of environmental UVB radiation and synthesis of vitamin D. This is supported by independent evidence which points to the role of vitamin D insufficiency in pregnancy and early life as a major factor in the development of MS (48, 55-57).
The rate of hospital admissions for MS in the Orkney Islands, north of the Scottish mainland, are three times the one in the Scottish Borders region adjacent to England and overall there is a highly significant correlation of MS admissions with latitude (58). Other Scottish regions with high MS admission rates are Shetland, the Western Isles and the most northerly part of the Scottish mainland. Highland and Grampian. However, most of the Scottish population is clustered further south, between latitude 55 and latitude 56.5 degrees where the rates of admission for MS all fall in a narrow band. This is hardly surprising since such a small difference in latitude gives rise to very little difference in intensity of UVB light.
International comparisons of annual UVB show that Glasgow has a particularly low level compared with other locations at the same latitude (13). The prevailing westerly wind blows clouds coming from the Atlantic across Scotland from west to east. However the mountains of central Scotland draw down much of this cloud as precipitation which means that cities to the east, Edinburgh and Dundee, get more sunshine hours than Glasgow. According to the map of sunshine hours (Figure 1) compiled by the UK Meteorological Office, the east coast towns of Scotland may expect to get 75150 more hours of sunshine per year than those on the West coast based on 1971-2000 figures. Aberdeen is on the east and so gets more sun than Glasgow but the annual UVB intensity may be no better because it is substantially further north.
Distribution of heart disease in the UK has been found to correlate geographically with the amount of rain (18, 59), which is a surrogate measure for cloud and hence an inverse measure of sunshine or UVB. In Scotland, 73% of the geographic variation in mortality from heart disease, in particular some of the east-west gradient in mortality, can be explained by cloud and rainfall together with unemployment and social class (60). These observations show the importance of considering both social and climatic factors together in the same model.
Air pollution blocks UVB . Air pollution is another critical factor which may have a profound effect on solar UVB radiation reaching ground level (61). Long term air pollution measured as NO2 and particulate matter of 10 micrometers or less in size (PMW) is substantially worse in Glasgow and Edinburgh compared with Aberdeen and Dundee (62). Air pollution, especially particulate, has been found to correlate with hospital respiratory admissions which were greater in Glasgow and Edinburgh than in Aberdeen and Dundee (62). Greater air pollution in Glasgow may be the result, in part, of its proximity to the west coast so that, as in the San Francisco bay area (63), a persistent marine layer of low cloud and fog moves inland with the prevailing wind as the region warms up during the day. Air pollution then accumulates beneath this cloud and does not readily disperse.
A significant association has been found between air pollution and cancer of the bowel and breast in 20 canadian cities (64). These two types of cancer are particularly common in Scotland and contribute to the higher Scots mortality (8). Breast and bowel cancer have been associated with low vitamin D levels in a number of studies (65-68). Reanalysis of the Women's Health Initiative Trial shows that breast, bowel and total cancer is reduced by a vitamin D plus calcium supplement (69). Evidence that insufficient vitamin D is a major factor in bowel cancer was accepted by the International Agency for Research in Cancer, Lyons, to imply causation (24). As well as causing adverse effects on respiratory health, including asthma, air pollution may have adverse effects on pregnancy, and on the immune system, particularly in the case of children (61). These effects are likely to be mediated by vitamin D.
Detailed study of air pollution and geography shows that the distribution of disease within greater Glasgow correlates with air pollution and urban residence among other factors (70). Different levels of air pollution between Liverpool, Manchester and Glasgow may be a factor explaining differences between the health of inhabitants of these cities which has been remarked upon in studies of the Scottish effect (9).
clean air acts, passed in the UK in the 1950s prevent domestic use of coal in cities. In the following years gross air pollution from this source ended, but so-called smokeless fuel continues to be burnt. At the same time a massive increase in use of cars and other road transport has created another major source of air pollution in cities. These changes have occurred in a similar way in all European countries. However interpretation and implementation of such laws and regulations are controlled by individual cities and regions. This may have led to differences between Glasgow and other Scottish cities and between Scotland and England but it is beyond the scope of this article to investigate the issue further.
Fish - changes in a way of life . Oily fish is the best natural food source of vitamin D and so differences in fish consumption may contribute to differences in health between those living in different parts of Scotland. Fish is likely to have been more readily available as a cheap food in Aberdeen, which historically has been the largest fishing port and market in Scotland, than in Glasgow. Fish will also have been more readily available in the Scottish islands, particularly Orkney and Shetland and in the many small fishing towns and villages. The present investigation has endeavoured, but been unable to obtain, historical statistics on fish consumption in Scotland as a whole. Indeed, expert advice is that such data probably does not exist. However the historical decline in fishing in the North Sea and reduced catches resulting from legal restrictions limiting fishing by British vessels in Icelandic and Norwegian waters is well documented.
To understand the secular changes in diet on the second half of the 20th century it is helpful to look back to the first half of the century when traditional diets were still followed in more remote parts of Scotland. An inquiry undertaken by the Medical Research Council into the diet of families in the Highlands and Islands of Scotland in the late 1930s found that people on the island of Lewis still ate fish regularly (71). The average Lewis family ate 13.5 lbs (6.1 kg) of fish per week, more than half of it fatty fish. This is about half a pound (227 gm) of fish a day for each family member providing about 1500 IUs of vitamin D, an amount of vitamin D sufficient for basic good health. In the more remote south-eastern coastal districts of the island families ate even more fish, particularly herring (72). Traditional fish dishes eaten on Lewis included boiled cod's head and stomach of cod stuffed with chopped cod's liver, onions and oatmeal. crude cod liver oil was used traditionally in the more remote areas as a food (72).
In 1936 the Department of Health for Scotland noted (73) that witnesses "deplored the passing of the old staple foods of porridge, salt herring and potatoes and the substitution of shop bread, tinned foods, tea and sweets and other goods purchased from shops." However some doctors considered the diet was improving because it contained more meat (although much of it was tinned corned beef) and fruits such as apples, oranges and bananas (73). These changes to the Scottish diet, observed at the beginning of the 20th century, had been going on for more than 100 years as Scots moved from rural and maritime locations to work in industry. The changes have continued into the 21st century as fish has, more than ever before, become a cash crop, exported from Scotland all over the UK and abroad.
The price and availability of fish varied a great deal since 1950, when Scots health ceased to improve so rapidly. North Sea fish stocks recovered briefly following World War II when submarine hostilities prevented normal fishing. However the trend before the war to larger fishing vessels using purse seine nets continued after the war (74). These faster modern boats enabled larger catches further offshore, catching the fish before they had a chance to come inshore to breed. This led to the collapse in 1955 of one of the great European herring fisheries (off East Anglia). In the following years herring stocks which had been highly productive for the last 1000 years disappeared one after another, or were drastically reduced (74, 75).
Herring is one of the best food sources of vitamin D. Fresh, pickled or smoked herring (kippers) has historically been an important part of the Scottish national diet. In 1977 a moratorium was called on herring fishing in the North Sea and an important item of the traditional Scots diet became unobtainable. The herring fisheries re-opened in 1981 but the eating habits of a generation had begun to change. The increased cost of seafood, together with changes towards a 'modern' industrial diet, have led to reduced consumption of fish even in Orkney and Shetland (76). These secular changes in diet, well recognised in Scotland although poorly documented in statistical terms, increased greatly during
World War II when fishing was severely restricted by submarine activity around the British Isles. This change in diet may be responsible, at least in part, for epidemics of leukaemia and multiple sclerosis in Orkney, Shetland and Faroes which were first observed following the war (77). The persistent cloud that hangs over Orkney (latitude 59° north) and Shetland (latitude 60.5° north) obscures what little sun there is. This, together with the change from a diet rich in fish (76), is a factor which must be considered as a cause of the high incidence of MS admissions in Orkney and Shetland today (58). The relationship between fish consumption and disease in Scotland merits further investigation.
Fortification - very limited. Fortification of foods with vitamin D was introduced in the 1930s but became limited to margarine and cereals in the UK in the 1950s after alarm over possible excess vitamin D being taken by babies (78) (and see below). Fortified foods contribute insignificant amounts of vitamin D to total intake in the UK (16). In 2011 milk fortified with vitamin D came on sale again in the UK by one supplier (Marks and Spencer).
Vitamins in infants - a frightening 'epidemic'. An 'epidemic' of hypercalcaemia in babies in Glasgow and elsewhere in the UK in the 1950s was associated with some deaths. An excess intake of vitamin D was blamed, although this was never proven with blood tests of vitamin D in the babies because reliable testing was not available at that time (78). The result of this 'epidemic' was the ending of fortification of milk with vitamin D in the UK, whereas other countries continued fortification. The blame attached to vitamin D following this scare led to mothers being advised not to give their babies cod liver oil or NHS infant vitamins (containing A, D and C) until they were six months old whereas other countries provide babies with a vitamin D supplement from the first week or so of life.
Failure to provide babies with a vitamin D supplement in the first six months of life may have profound effects on the nervous system. Babies in Scotland are particularly vulnerable because population levels of vitamin D are so low (16, 17) and so Scots' babies obtain minimal supplies of vitamin D in the womb. Insufficient vitamin D in early life is now known to be a crucial risk factor for MS (48, 49) and diabetes type 1 (79).
Official advice in the UK to doctors and mothers about receiving vitamin D in pregnancy has been inconsistent (80). In 1991 and 1998 one learned UK committee (COMA -Committee on Medical Aspects of Food and Nutrition Policy) recommended a supplement of vitamin D for all women in pregnancy. This was countermanded by another committee (NICE - National Institute of Clinical Excellence) in 2003 on grounds of lack of evidence. Then in 2008, the NICE advice was countermanded again by NICE itself which then recommended a vitamin D supplement for mothers and children in low income households. It is hardly surprising that obstetricians and midwives have been confused and a recommendation to take vitamin D in pregnancy and while breast feeding is not passed on to mothers.
Mistaken advice to cover up and avoid the sun . In the 1970s the UK Health Education Council (HEC) started to advise that sunlight is dangerous and should be avoided. The HEC spent some £3 million telling people to put on suncream before going out, cover up with clothing and a hat and avoid the sun in the middle of the day. When HEC was dissolved Cancer Research UK, the national charity, obtained a government grant to continue the campaign under their SunSmart banner. This advice, which continued until 2010, can only have lowered vitamin D uptake generally in the UK (80). Each year in April or May, Cancer Research UK promoted their 'SunSmart' advice to avoid the sun in the middle of the day, cover up with long sleeves and a hat and wear suncream. Anecdotally, many people tried to follow this advice and reduced sun exposure to a minimum, while many also ignored it. Now Cancer Research UK have changed their advice and say people should go out in the sun in the middle of the day (81, 82) but they have not issued any corrective advertising and the old message persists.
Between the 1930s and the 1960s, infants in the UK were commonly exposed to UV sunlamp treatments in clinics as a measure to prevent rickets and tuberculosis. These treatments went out of fashion in the 1960s or earlier, Since then sunlamps have been condemned as dangerous devices by Cancer Research UK and others without providing adequate scientific evidence (83-85).
Clothing, suncream, home entertainment. Until the 1960s, it was customary for boys in the UK to wear short trousers all year round until about 12-13 years of age. A person wearing short trousers with a short sleeved shirt has sun exposure of 30-50% of the skin which may allow optimal synthesis of vitamin D in summer if sufficient time is spent outdoors. Now most boys of all ages wear long trousers all year round. Young girls may still wear skirts that expose the knees and lower legs. However, in the UK today tights or leggings are generally worn with such skirts all year round and so casual exposure to the sun is minimal. As a result of these fashions young children are getting much less exposure to the sun than they obtained previously.
The first sunscreen creams became available in the late 1940s and were continuously improved. In the 1970s new sunscreen creams were developed containing chemicals that were more effective at blocking UVB and these became increasingly popular. When a sun screen with a modest sun protection factor (SPF) of 15 is used only 'miniscule' amounts of vitamin D will be made (86). By the mid-1990s many, perhaps most, women's cosmetics, face creams, foundation, and hand creams contained sun block.
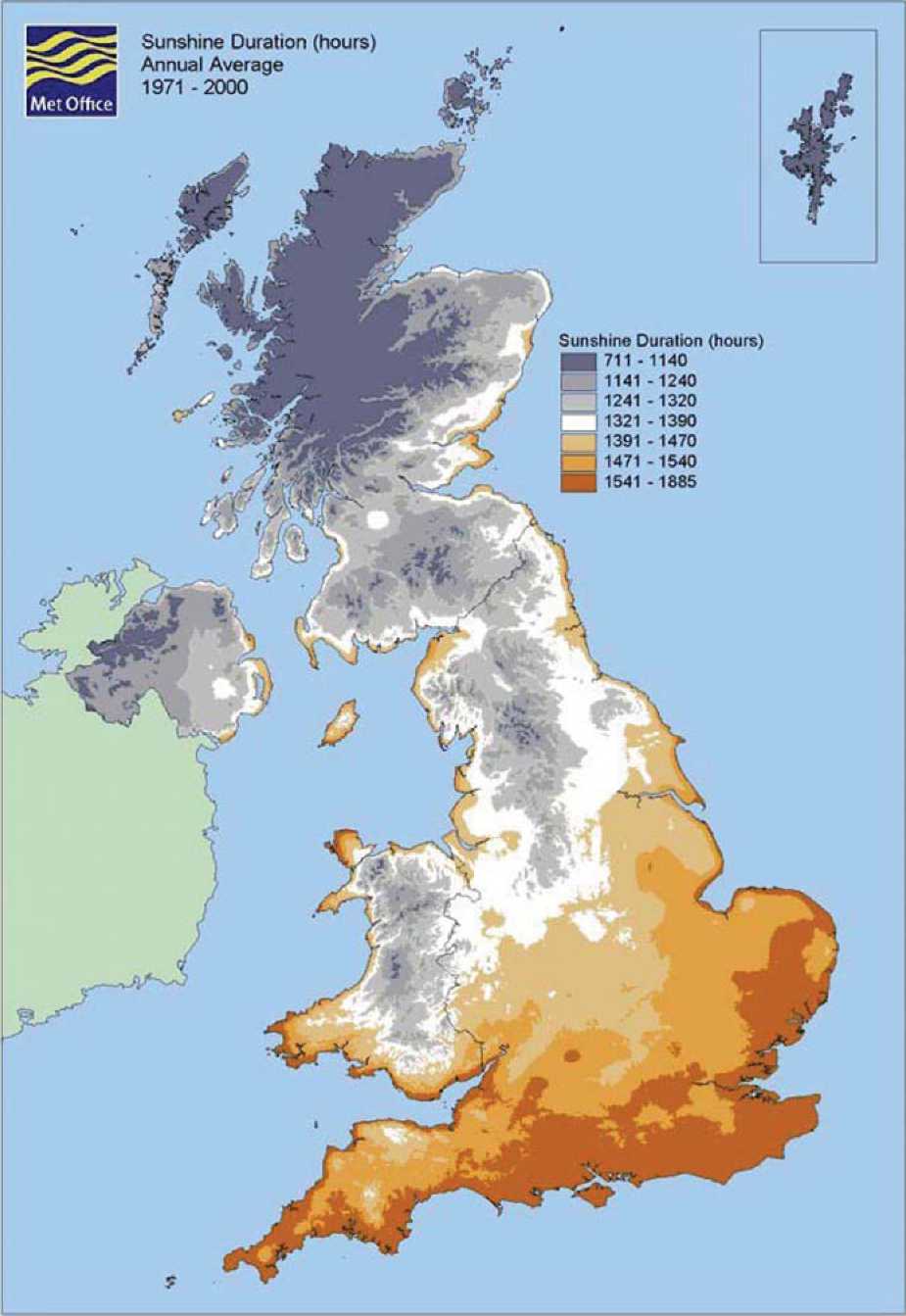
Figure 1. Sunshine duration map of the UK compiled by the Meteorological Office. Reproduced with permission.
Home entertainment is another factor keeping people out of the sun. TV was available throughout the UK by the end of the 1950s. But the increase in number of channels and diversity of programmes means that every year, the average time spent watching TV has increased, keeping more and more people indoors at weekends. From the 1990s on computers and digital screen games became increasingly popular doing even more to trap people indoors in summer as well as winter. While these changes have occurred throughout the modern world the effect may have been greater in Scotland, where a small lowering of population levels of vitamin D might be expected to take more people below threshold levels for disease.
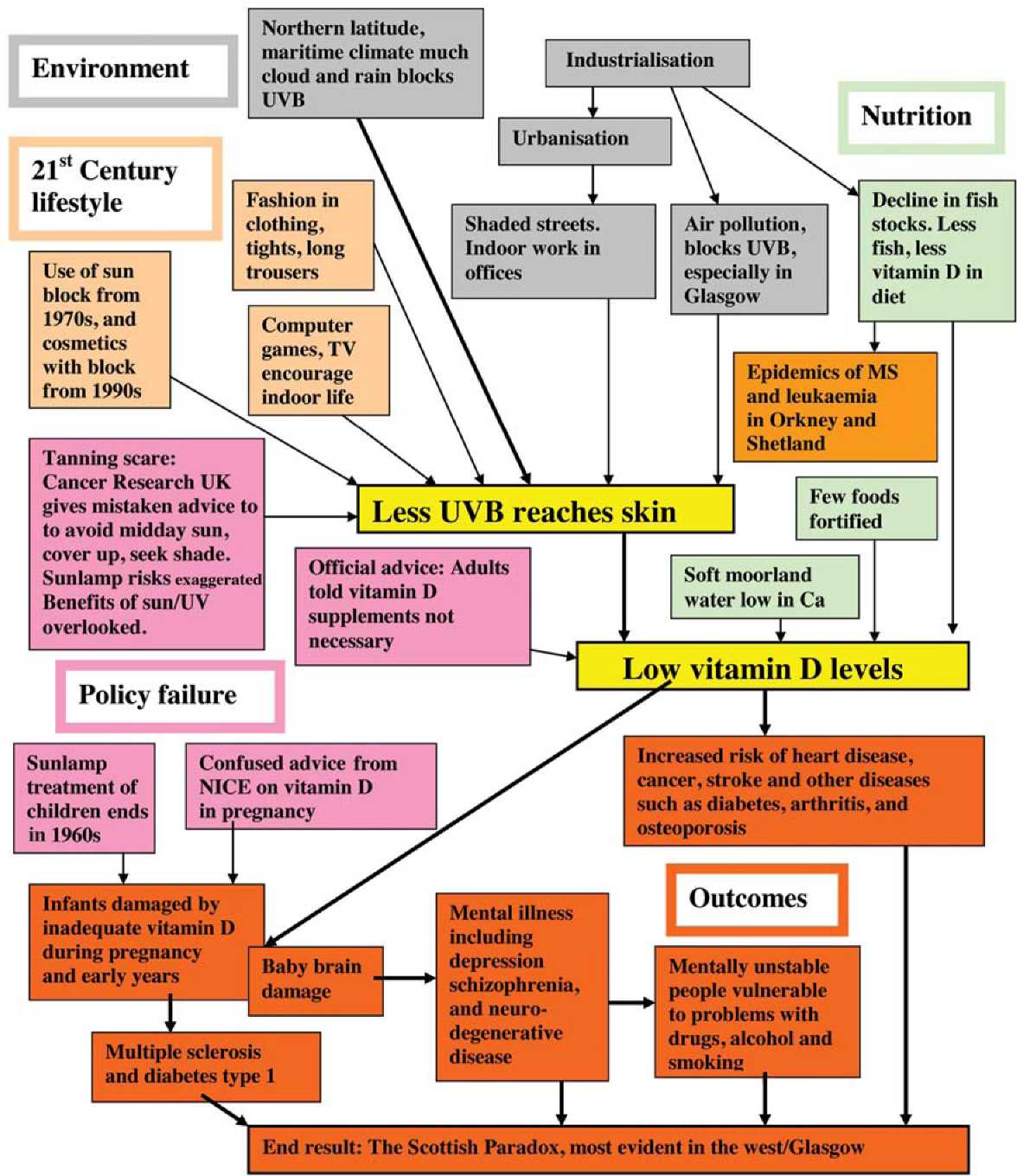
Figure 2. The pathway of vitamin D deficiency in Scotland. (at beginning of this page)
The Pathway to Scotland's Health Deficit
A clear pathway (Figure 2) of cause and effect can be shown from environmental factors and the modern effects of industrialization, which reduce sun exposure and vitamin D uptake, to the major physical illnesses that excessively afflict Scots today. The same pathway can also be traced to an increased vulnerability of Scots to mental illness, drug and alcohol problems, although social factors must clearly be involved with these endpoints. The pathway also shows the complex interaction of these factors with diet, 21st century lifestyle and national failures in policy and advice. The various factors in the pathway are discussed and referenced above.
Five Paradoxes and a Hypothesis
The UVB-vitamin D-cancer hypothesis was first proposed by the Garland brothers in 1980 (87) but was largely overlooked by mainstream epidemiologists. Since 1980, the hypothesis has been extended to take in many other diseases (88, 89) but it still remains to be fully accepted and integrated into mainstream accounts of major health risks. This delay has hindered epidemiologists striving to explain striking national differences in health which have been highlighted as paradoxes.
Many factors, geographical, climatic, social and biological influence the amount of sunlight reaching the skin. The complexity of all these factors and the influence of vitamin D on so many diseases have delayed acceptance of the UVB-vitamin D hypothesis as an explanation of international paradoxes in epidemiology. Difficulties in understanding all these variables and their interactions have been considerable as this article aims to show by a consideration of the Scots paradox.
Latitude is a major factor which is present by definition in the five epidemiological paradoxes considered here. However the implications of latitude have generally been overlooked, perhaps because epidemiologists have been reluctant to accept ecological evidence (90). The French paradox highlights the low mortality from coronary heart disease in France (latitude 42° to 51° north) compared with northern European countries despite a high intake of animal fat by the French. The concept of the French paradox is in conflict with conventional theories on the causes of coronary heart disease. (2) Most emphasis in attempting to explain the French paradox, and its close relative 'the Mediterranean diet' (2), have been given to differences in nutrition and wine drinking. Vitamin D does not seem to have been given serious consideration, which is particularly striking when, as everyone knows, the Mediterranean is the sunniest part of Europe (91).
Albania (latitude 41° north) is the poorest country in Europe and has one of the highest infant mortality rates. Yet the age-standardised mortality rate for coronary heart disease in males aged 0-64 years was less than half that of the UK in 1990 (3, 92). Post communism Albania is in transition and perhaps shedding some of its paradox. However since 1990 infant mortality in Albania has decreased and life expectancy increased (93, 94) while cardiovascular risk factors appear to remain less common than in many other European countries (95). Mortality in Albania is lowest in the south west where most of the olive oil, fruits and vegetables are grown. Thus the Albanian paradox is very similar to the French paradox and again latitude stands out as a major variable. Grimes et al. have proposed that the Albanian paradox can be accounted for by the major protective effect that sunlight has in preventing heart disease (6, 96).
The Swiss paradox has been stated as follows. "Consumption of milk and milk products in Switzerland is very high, but premature cardiovascular mortality of Swiss men and women was and is the lowest in Europe" (5). Ginter et al. point out that cardiovascular mortality is generally lower in those European countries with highest cheese consumption. Switzerland, the Netherlands, Italy, France and Greece. They theorize that milk products from cows that graze at higher alpine localities contain higher levels of n-3 polyunsaturated fatty acids which prevent development of the metabolic syndrome, although it is not clear how this explains the relatively low mortality in the Netherlands where some cows may actually graze below sea level.
Switzerland (latitude 46° to 48° north) has the lowest mortality in Europe. The health of the Swiss is almost certainly linked, in part, to social factors associated with wealth. However the Swiss population also lives at a higher altitude than any other nation in Europe. Most Swiss live above 400 m altitude where they get some 5% more UVB than people living at the same latitude at sea level and, probably more important, a longer summer season when UVB remains available. Furthermore, all the cheese eaten in Switzerland provides the Swiss with a relatively high calcium diet, so sparing vitamin D for other functions (1923). The net effect of a 1000 m increase in altitude of residence has been found to be a 33% decrease in cardiovascular mortality and a 12% decrease in stroke (97). The hypothesis that lower cancer rates observed at high altitudes arise from enhanced sunlight-induced vitamin D production levels has advanced (98).
Finally the Greek (or Italian) Paradox has been expressed as follows. "Why is it that the people of Greece who enjoy one of the lowest mortality rates from coronary heart disease and one of the highest life expectancies in Europe smoke the most cigarettes per head of the population?" (4) Grimes, who named the Greek paradox, suggests that the southern location of Greece (latitude 35° to 41° north) with its sunshine protects Greek smokers against heart disease and lung cancer, whereas Scotland's murky weather appears to put smokers at greater risk. A study of Scottish smokers in Renfrew and Paisley found that there are more deaths from lung cancer per cigarette smoked in Scotland than in England or the United States (99). Explanation of lung cancer incidence in Greece and Scotland in terms of the UVB-vitamin D hypothesis is encouraged by a study of lung cancer and UVB irradiance in 111 countries (100) which shows that lower levels of UVB are associated with a higher incidence of lung cancer.
Testing by the Bradford Hill Criteria
Explaining national differences in incidence of disease and mortality is a major project involving many variables, as illustrated here by the example of Scotland. Elsewhere, 17 different hypotheses have been considered as explanations of the Scots' paradox and the Bradford Hill criteria have been used to assess the validity of each hypothesis (9, 101). The UVB-vitamin D hypothesis is tested below against the criteria of Bradford Hill as a valid explanation of the Scots' paradox (criteria in bold). Examples suggest that these criteria may be satisfied and so the Scots' paradox may in large part be explained by the UVB-vitamin D hypothesis.
Strength of association . A meta-analysis of clinical trials of vitamin D has established a significant association between supplementation with vitamin D and reduction in mortality (37, 38). Low serum levels of vitamin D have also been associated with reduced mortality in adults in the US (35) and in the Tromso study (34).
Consistency . Many observations have shown consistent associations between low levels of vitamin D and health outcomes. Indeed the Bradford Hill criteria have been used to assess the UVB-vitamin D-cancer hypothesis suggesting that insufficient vitamin D or UVB is the cause of some 14 types of cancer (102).
Specificity . Diseases which have a higher incidence or prevalence in Scotland than in England include those for which insufficient vitamin D is an established risk factor. Examples are bowel cancer, MS, diabetes, arthritis, and dental decay (10). This suggests that the UVB-vitamin D hypothesis has specificity.
Temporality. The time course of changes in lifestyle and environmental factors influencing UVB can explain how mortality in Scotland fell behind other countries after 1950 as discussed above.
Biological gradient. A biological gradient of vitamin D serum levels measured in 45 year olds has been demonstrated between Scotland and England consistent with the gradient of mortality between the two countries (16). A latitude gradient for MS has been shown within Scotland (58).
Plausibility . Vitamin D is known to activate more than a thousand genes and to play an important role in cell differentiation and apoptosis. At least five other metabolic systems are modulated by vitamin D, so accounting for its influence on so many different diseases (103, 104).
Coherence . The vitamin D hypothesis is entirely consistent with modern knowledge of epidemiology and disease processes, with no need to invoke any additional mechanisms to explain awkward facts.
Experiment. The vitamin D hypothesis is supported by some clinical trials (37, 69, 104) and many others are in progress. Many steps in the disease pathway have been tested by detailed experimentation, for example, the link between MS and insufficient vitamin D is now known to be mediated by vitamin D-responsive genes (105).
Analogy. The understanding we are now developing of epidemic disease caused by insufficient sunshine and insufficient vitamin D can be compared with the development of understanding of the importance of clean water for prevention of epidemics in the 19th century and clean air in the 20th Century. Changes in living patterns and housing brought about by industrialisation led to diseases caused by dirty air, indoor work and polluted air. We are now beginning to understand the full consequences of dirty air and indoor work and indoor living which block out sunlight, our natural source of vitamin D.
Summary
Scotland's northern location and climate provide little sunshine and so Scots have low vitamin D levels compared with England. Since 1950 a number of factors have emerged which increased the likelihood that sun exposure of Scots was reduced below threshold levels for good health. These factors include. mistaken advice and publicity campaigns from government and Cancer Research UK, changes in clothing fashions, greater time spent indoors watching TV or computer screens, and increased air pollution from car exhausts which prevents normal UVB radiation reaching ground level. In addition consumption of oily fish has almost certainly decreased. These factors are shown as a pathway which provides a substantial explanation of the Scots' paradox. Latitude and differences in sun exposure may explain other paradoxes noted by epidemiologists. Low vitamin D levels may easily be corrected if the political will can be found.
Acknowledgements
This article owes much to David Grimes, who first named the Scots and Greek paradoxes, and to William Grant, whose pioneering ecological studies of sunlight, vitamin D and disease have done much to explain differences in the health of nations. I also wish to thank George Ebers and many others who have helped me.
References
1 Richard JL. Coronary risk factors. The French paradox. Arch Mal Coeur Vaiss 80. 17-21, 1987 (in French).
2 de Lorgeril M, Salen P, Paillard F, Laporte F, Boucher F and de Leiris J. Mediterranean diet and the French paradox. two distinct biogeographic concepts for one consolidated scientific theory on the role of nutrition in coronary heart disease. Cardiovasc Res 54(3). 503-515, 2002.
3 Gjonca A and Bobak M. Albanian paradox, another interesting example of protective effect of Mediterranean lifestyle? Lancet 350(9094). 1815-1817, 1997.
4 Grimes D. Vitamin D and cholesterol. York, UK. Tennison Publishing, 2009.
5 Ginter E, Simko V and Dolinska S. Paradoxes in medicine. an access to new knowledge? Bratisl Lek Listy 110(2): 112-115, 2009.
6 Grimes DS, Hindle E and Dyer T. Albanian paradox, another example of protective effect of Mediterranean lifestyle? Lancet 351(9105). 835-836, 1998.
7 Grimes DS, Hindle E and Dyer T. Respiratory infection and coronary heart disease. progression of a paradigm. Quart J Med 93(6). 375-383, 2000.
8 Hanlon P, Lawder R, Buchanan D, Redpath A, Walsh D, Wood R, Bain M, Brewster DH and Chalmers J. Why is mortality higher in Scotland than in England and Wales? Decreasing influence of socioeconomic deprivation between 1981 and 2001 supports the existence of the 'Scottish Effect'. J Public Health (Oxf) 27(2).199-204, 2005.
9 McCartney G, Collins C, Walsh D and Batty D. Accounting for Scotland's excess mortality. towards a synthesis. Glasgow. Glasgow Centre for Population Health, pp. 1-87, 2011.
10 Gillie O. Scotland's health deficit. an explanation and a plan. London. Health Research Forum, 2008
11 Holick MF and Chen TC. Vitamin D deficiency. a worldwide problem with health consequences. Am J Clin Nutr 87(4). 1080S-1086S, 2008.
12 Macdonald HM, Mavroeidi A, Reid DM and Fraser WD. Sunlight or diet. What is the answer for providing sufficient vitamin D in the U.K.? Br J Dermatol 163(2). 434-435, author reply 435-6, 2010.
13 Gies P, Roy C, Javorniczky J, Henderson S, Lemus-Deschamps L and Driscoll C. Global solar UV index. Australian measurements, forecasts and comparison with the UK. Photochem Photobiol 79(1). 32-39, 2004.
14 Macdonald HM, Mavroeidi A, Barr RJ, Black AJ, Fraser WD and Reid DM. Vitamin D status in postmenopausal women living at higher latitudes in the UK in relation to bone health, overweight, sunlight exposure and dietary vitamin D. Bone 42(5). 996-1003, 2008.
15 Zgaga L, Theodoratou E, Farrington SM, Agakov F, Tenesa A, Walker M, Knox S, Wallace AM, Cetnarskyj R, McNeill G, Kyle J, Porteous ME, Dunlop MG and Campbell H. Diet, environmental factors, and lifestyle underlie the high prevalence of vitamin d deficiency in healthy adults in Scotland, and supplementation reduces the proportion that are severely deficient. J Nutr 141(8). 1535-1542, 2011.
16 Hypponen E and Power C. Hypovitaminosis D in British adults at age 45 y. nationwide cohort study of dietary and lifestyle predictors. Am J Clin Nutr 85(3). 860-868, 2007.
17 Ahmed SF, Franey C, McDevitt H, Somerville L, Butler S, Galloway P, Reynolds L, Shaikh MG and Wallace AM. Recent trends and clinical features of childhood vitamin D deficiency presenting to a children's hospital in Glasgow. Arch Dis Child 96(7). 694-696, 2011.
18 Shaper AG, Packham RF and Pocock SJ. The British Regional Heart Study. cardiovascular mortality and water quality. J Environ Pathol Toxicol 4(2-3). 89-111, 1980.
19 Mason RS, Sequeira VB and Gordon-Thomson C. Vitamin D. the light side of sunshine. Eur J Clin Nutr 65(9). 1485-1494, 2011.
20 Berlin T and Bjorkhem I. Effect of calcium intake on serum levels of 25-hydroxyvitamin D 3. Eur J Clin Invest 18(1). 5255, 1988.
21 Brock K, Cant R, Clemson L, Mason RS and Fraser DR. Effects of diet and exercise on plasma vitamin D (25(OH)D) levels in Vietnamese immigrant elderly in Sydney, Australia. J
Steroid Biochem Mol Biol 103(3-5). 786-792, 2007.
22 Clements MR, Johnson L and Fraser DR. A new mechanism for induced vitamin D deficiency in calcium deprivation. Nature 325(6099). 62-65, 1987.
23 Pfeiffer M, Begerow B, Minne H, Nachtigal D and Hansen C. Effects of a short-term vitamin D3 and calcium supplementation on blood pressure and parathyroid hormone levels in elderly women. J Clin Endocrinol Metab 86. 1633-1667, 2001.
24 IARC. Vitamin D and Cancer. Lyon. IARC, 2008.
25 Giovannucci E. Vitamin D and cancer incidence in the Harvard cohorts. Ann Epidemiol 19(2). 84-88, 2009.
26 Garland CF, Gorham ED, Mohr SB and Garland FC. Vitamin D for cancer prevention. global perspective. Ann Epidemiol 19(7). 468-483, 2009 .
27 Parker J, Hashmi O, Dutton D, Mavrodaris A, Stranges S, Kandala NB, Clarke A and Franco OH. Levels of vitamin D and cardiometabolic disorders. systematic review and meta-analysis. Maturitas 65(3). 225-236, 2010.
28 Zittermann A and Gummert JF. Sun, vitamin D, and cardiovascular disease. J Photochem Photobiol B 101(2). 124129, 2010.
29 Zitterman A and Gummert J. Nonclassical Vitamin D Actions. Nutrients 2. 408-425, 2010.
30 Anderson JL, May HT, Horne BD, Bair TL, Hall NL, Carlquist JF, Lappe DL and Muhlestein JB. Relation of vitamin D deficiency to cardiovascular risk factors, disease status, and incident events in a general healthcare population. Am J Cardiol 106(7). 963-968, 2010.
31 Pilz S, Tomaschitz A, Drechsler C, Zittermann A, Dekker JM and Marz W. Vitamin D supplementation. a promising approach for the prevention and treatment of strokes. Curr Drug Targets 12(1). 88-96, 2010.
32 Pilz S, Tomaschitz A and Marz W. Vitamin D deficiency and stroke. time to act! Am J Cardiol 106(11). 1674, 2010.
33 Boucher BJ. Vitamin D insufficiency and diabetes risks. Curr Drug Targets 12(1). 61-87, 2011.
34 Hutchinson MS, Grimnes G, Joakimsen RM, Figenschau Y and Jorde R. Low serum 25-hydroxyvitamin D levels are associated with increased all-cause mortality risk in a general population. the Tromso study. Eur J Endocrinol 162(5). 935942, 2011.
35 Ginde AA, Scragg R, Schwartz RS and Camargo CA Jr.. Prospective study of serum 25-hydroxyvitamin D level, cardiovascular disease mortality, and all-cause mortality in older U.S. adults. J Am Geriatr Soc 57(9). 1595-1603, 2009.
36 Grant W. An estimate of the global reduction in mortality rates through doubling vitamin D levels. Eur J Clin Nutr 65. 10161026, 2011.
37 Autier P and Gandini S. Vitamin D supplementation and total mortality. a meta-analysis of randomized controlled trials. Arch Intern Med 167(16). 1730-1737, 2007. 246 Gillie. Major Paradoxes in Epidemiology (Review)
38 Bjelakovic G, Gluud LL, Nikolova D, Whitfield K, Wetterslev J, Simonetti RG, Bjelakovic M and Gluud C. Vitamin D supplementation for prevention of mortality in adults. Cochrane Database Syst Rev Jul 6;(7). CD007470, 2011.
39 Kinney DK, Teixeira P, Hsu D, Napoleon SC, Crowley DJ, Miller A, Hyman W and Huang E. Relation of schizophrenia prevalence to latitude, climate, fish consumption, infant mortality, and skin color. A role for prenatal vitamin D deficiency and infections? Schizophr Bull 35(3). 582-595, 2009.
40 Cannell J. On the aetiology of autism. Acta Paediatrica 99. 1128-1130, 2010.
41 Jorde R, Sneve M, Figenschau Y, Svartberg J and Waterloo K. Effects of vitamin D supplementation on symptoms of depression in overweight and obese subjects. randomized
double blind trial. J Intern Med 264(6). 599-609, 2008.
42 Lee DM, Tajar A, O'Neill TW, O'Connor DB, Bartfai G, Boonen S, Bouillon R, Casanueva FF, Finn JD, Forti G, Giwercman A, Han TS, Huhtaniemi IT, Kula K, Lean ME, Punab M, Silman AJ, Vanderschueren D, Wu FC and Pendleton N. Lower vitamin D levels are associated with depression among community-dwelling European men. J Psychopharmacol Sep 7 [Epub ahead of print] 2010.
43 Lee DM, Tajar A, Ulubaev A, Pendleton N, O'Neill TW, O'Connor DB, Bartfai G, Boonen S, Bouillon R, Casanueva FF, Finn JD, Forti G, Giwercman A, Han TS, Huhtaniemi IT, Kula K, Lean ME, Punab M, Silman AJ, Vanderschueren D and Wu FC; EMAS study group. Association between 25-hydroxyvitamin D levels and cognitive performance in middle-aged and older European men. J Neurol Neurosurg Psychiatry
80(7). 722-729, 2009.
44 Evatt ML, Delong MR, Kumari M, Auinger P, McDermott MP and Tangpricha V. High Prevalence of Hypovitaminosis D Status in Patients With Early Parkinson Disease. Arch Neurol 68(3). 314-319, 2011.
45 Grant WB. Does vitamin D reduce the risk of dementia? J Alzheimers Dis 17(1). 151-159, 2009.
46 Fernandes de Abreu D, Eyles D and Feron F. Vitamin D, a neuro-immunomodulator. Implications for neurodegenerative and autoimmune diseases. Psychoneuroendocrinology 34(supp 1). S265-S277, 2009.
47 Eyles D, Brown J, MacKay-Sim A, McGrath J and Feron F. Vitamin D 3 and brain development. Neuroscience 118. 641653, 2003.
48 Lucas RM, Ponsonby AL, Dear K, Valery PC, Pender MP, Taylor BV, Kilpatrick TJ, Dwyer T, Coulthard A, Chapman C, van der Mei I, Williams D and McMichael AJ. Sun exposure and vitamin D are independent risk factors for CNS demyelination. Neurology 76(6). 540-548, 2011.
49 Willer CJ, Dyment DA, Sadovnick AD, Rothwell PM, Murray TJ and Ebers GC, Canadian Collaborative Study Group. Timing of birth and risk of multiple sclerosis. population based study.
BMJ 330(7483). 120, 2005.
50 Campbell M. Death rates from diseases of the heart. BMJ ii. 528-535, 1963.
51 Florey CdV, Melia R and Darby S. Changing mortality from ischaemic heart disease in Great Britain 1968-76. BMJ 1. 63537, 1978.
52 Appleby J. Does poor health justify NHS reform. BMJ 342. 310, 2011.
53 Bischoff-Ferrari H. How to select the doses of vitamin D in the management of osteoporosis. Osteoporosis Int 18. 401-407, 2007.
54 Staples J, Ponsonby A-L and Lim L. Low maternal exposure to ultraviolet radiation in pregnancy, month of birth, and risk of multiple sclerosis in offspring. longitudinal analysis. BMJ 340. c1640, 2010.
55 Handel AE, Handunnetthi L, Giovannoni G, Ebers GC and Ramagopalan SV. Genetic and environmental factors and the distribution of multiple sclerosis in Europe. Eur J Neurol 17(9).
1210-4, 2010.
56 Mirzaei F, Michels KB, Munger K, O'Reilly E, Chitnis T, Forman MR, Giuovannucci E, Rosner B and Ascherio A. Gestational vitamin D and the risk of multiple sclerosis in offspring. Ann Neurol 70(1). 30-40, 2011.
57 Ascherio A, Munger KL and Simon KC. Vitamin D and multiple sclerosis. Lancet Neurol 9(6). 599-612, 2010.
58 Handel AE, Jarvis L, McLaughlin R, Fries A, Ebers GC and Ramagopalan SV. The epidemiology of multiple sclerosis in Scotland. inferences from hospital admissions. PLoS One 6(1). e14606,2011.
59 West RR and Lowe CR. Mortality from ischaemic heart disease. Inter-town variation and its association with climate in England and Wales. Int J Epidemiol 5(2). 195-201, 1976.
60 Crombie IK, Kenicer MB, Smith WC and Tunstall-Pedoe HD. Unemployment, socio-environmental factors, and coronary heart disease in Scotland. Br Heart J 61(2). 172-177, 1989.
61 Buka I, Koranteng S and Osornio-Vargas AR. The effects of air pollution on the health of children. Paediatr Child Health 11(8). 513-516, 2006.
62 Lee D, Ferguson C and Mitchell R. Air pollution and health in Scotland. a multicity study. Biostatistics 10(3). 409-23, 2009.
63 Grant WB and Garland CF. Air pollution and breast cancer. Epidemiology 16(3). 421, 2005.
64 Gorham ED, Garland CF and Garland FC. Acid haze air pollution and breast and colon cancer mortality in 20 Canadian cities. Can J Public Health 80(2). 96-100, 1989.
65 Bertone-Johnson ER. Vitamin D and breast cancer. Ann Epidemiol 19(7). 462-467, 2009.
66 Jenab M, Bueno-de-Mesquita HB, Ferrari P, van Duijnhoven FJ, Norat T, Pischon T, Jansen EH, Slimani N, Byrnes G, Rinaldi S, Tj0nneland A, Olsen A, Overvad K, Boutron-Ruault MC, Clavel-Chapelon F, Morois S, Kaaks R, Linseisen J, Boeing H, Bergmann MM, Trichopoulou A, Misirli G, Trichopoulos D, Berrino F, Vineis P, Panico S, Palli D, Tumino R, Ros MM, van Gils CH, Peeters PH, Brustad M, Lund E, Tormo MJ, Ardanaz E, Rodriguez L, Sanchez MJ, Dorronsoro M, Gonzalez CA, Hallmans G, Palmqvist R, Roddam A, Key TJ, Khaw KT, Autier P, Hainaut P and Riboli E. Association between pre-diagnostic circulating vitamin D concentration and risk of colorectal cancer in European populations.a nested case-control study. BMJ 340. b5500, 2010.
67 Yin L, Grandi N, Raum E, Haug U, Arndt V and Brenner H. Meta-analysis. longitudinal studies of serum vitamin D and colorectal cancer risk. Aliment Pharmacol Ther 30(2). 113-125, 2009.
68 Rejnmark L, Tietze A, Vestergaard P, Buhl L, Lehbrink M, Heickendorff L and Mosekilde L. Reduced prediagnostic 25-hydroxyvitamin D levels in women with breast cancer. a nested case-control study. Cancer Epidemiol Biomarkers Prev 18(10). 2655-2660, 2009. 247 Anticancer Research 32. 237-248 (2012)
69 Bolland MJ, Grey A, Gamble GD and Reid IR. Calcium and vitamin D supplements and health outcomes. a reanalysis of the Women's Health Initiative (WHI) limited-access data set. Am J Clin Nutr 94. 1144-1149, 2011.
70 Lee D. A comparison of conditional autoregressive models used in Bayesian disease mapping. Spatio-tempor Epidemiol 2(2). 79-89, 2011.
71 Cathcart E, Murray A and Beveridge J. An inquiry into the Diet of Families in the Highlands and Islands of Scotland. Studies in Nutrition. London. Medical Research Council, HMSO, 1940.
72 King J. Dental disease in the island of Lewis. London. Medical Research Council, 1940.
73 Report of Committee on Scottish Health Services. Edinburgh. Department of Health for Scotland, 1936.
74 Roberts C. The Unnatural History of the Sea. The Past and Future of Humanity and Fishing. London. Gaia Thinking, 2007.
75 Smylie M. Herring. a History of the Silver Darlings. Stroud, UK. Tempus, 2004.
76 Cluness A. The Shetland Isles. London. Hale 1951.
77 Gillie O. Epidemics in the North Atlantic Islands. Chapter 6. In. Scotland's Health Deficit. an explanation and a plan. Health Research Forum Occasional Reports 3. 42-49, 2008.
78 Wagner CL, Taylor SN and Hollis BW. Does vitamin D make the world go 'round'? Breastfeed Med 3(4). 239-250, 2008.
79 Hypponen E and Boucher B. Avoidance of vitamin D deficiency in pregnancy in the United Kingdom; the case for a unified approach in national policy. Brit J Nutr 104. 309-314, 2010.
80 Gillie O. Sunlight robbery. A critique of public health policy on vitamin D in the UK. Mol. Nutr. Food Res. 54. 1-16, 2010.
81 Hope J. Mad dogs and Englishmen were right! We SHOULD go out in the midday sun say experts. Daily Mail, London, 16 Dec 2010.
82 Consensus Vitamin D Position Statement. Cancer Research UK and others, London, 2010.
83 Moan J, Lagunova Z, Cicarma E, Aksnes L, Dahlback A, Grant WB and Porojnicu AC. Sunbeds as vitamin D sources. Photochem Photobiol 85(6). 1474-1479, 2009.
84 Moan J, Porojnicu A, Dahlback A and Setlow R. Addressing the health benefits and risks, involving vitamin D or skin cancer, of increased sun exposure. PNAS 105. 668-673, 2008.
85 Moan J, Baturaite Z, Juzeniene A and Porojnicu A. Vitamin D, sun, sunbeds and health. Publ. online. DOI.10.1017/ S1368980011002801 Public Health Nutrition 2011
86 Sayre RM and Dowdy JC. Darkness at noon. sunscreens and vitamin D3. Photochem Photobiol 83(2). 459-463, 2007.
87 Garland CF and Garland FC. Do sunlight and vitamin D reduce the likelihood of colon cancer? Int J Epidemiol 9(3). 227-231, 1980.
88 Garland CF, Garland FC, Gorham ED, Lipkin M, Newmark H, Mohr SB and Holick MF. The role of vitamin D in cancer prevention. Am J Public Health 96(2). 252-261, 2006.
89 Garland CF and Garland FC. Commentary. progress of a paradigm. Int J Epidemiol 35(2). 220-222, 2006.
90 Grant WB and Boucher BJ. Current impediments to acceptance of the ultraviolet-B-vitamin D-cancer hypothesis. Anticancer Res 29(9). 3597-3604, 2009. 248
91 Grimes DS. Mediterranean diet revisited. Quart J Med 94(3). 173-174, 2001.
92 Grimes DS. Vitamin D and the social aspects of disease. Quart J Med Aug 3. Epub ahead of print. 2011.
93 European Mortality Database. Copenhagen. WHO Regional Office for Europe, 2007.
94 European Health for All Database. Copenhagen. WHO Regional Office for Europe, 2007.
95 Shapo L, Pomerleau J and McKee M. Epidemiology of hypertension and associated cardiovascular risk factors in a country in transition. a population based survey in Tirana City, Albania. J Epidemiol Community Health 57(9). 734-739, 2003.
96 Grimes D, Hindle E and Dyer T. Sunlight, cholesterol and coronary heart disease. Quart J Med 89. 579-589, 1996.
97 Faeh D, Gutzwiller F and Bopp M. Lower mortality from coronary heart disease and stroke at higher altitudes in Switzerland. Circulation 120(6). 495-501, 2009.
98 Hayes D. Cancer protection related to solar ultraviolet, altitude and vitamin D. Medical Hypotheses 75(4). 378-382, 2010.
99 Gillis CR, Hole DJ and Hawthorne V. Cigarette smoking and male lung cancer in an area of very high incidence - II. Report of a general population cohort study in the West of Scotland. J Epidemiol Comm Health 42. 44-48, 1988.
100 Mohr SB, Garland CF, Gorham ED, Grant WB and Garland FC. Could ultraviolet B irradiance and vitamin D be associated with lower incidence rates of lung cancer? J Epidemiol Community Health 62(1). 69-74, 2008.
101 Hill A. The Environment and Disease. Association or Causation. Proc Royal Soc Med 58. 295-300, 1965.
102 Grant WB and Boucher BJ. Current impediments to acceptance of the ultraviolet B-vitamin D-cancer hypothesis. Anticancer Res 29(9). 3597-3604, 2009.
103 Norman AW and Bouillon R. Vitamin D nutritional policy needs a vision for the future. Exp Biol Med (Maywood) 235(9). 1034-1045, 2010.
104 Lappe JM, Travers-Gustafson D, Davies KM, Recker RR and Heaney RP. Vitamin D and calcium supplementation reduces cancer risk. results of a randomized trial. Am J Clin Nutr 85(6). 1586-1591, 2007.
105 Ramagopalan SV, Heger A, Berlanga AJ, Maugeri NJ, Lincoln MR, Burrell A, Handunnetthi L, Handel AE, Disanto G, Orton SM, Watson CT, Morahan JM, Giovannoni G, Ponting CP, Ebers GC and Knight JC. A ChlP-seq defined genome-wide map of vitamin D receptor binding. Associations with disease and evolution. Genome Res 20. 1352-1360, 2010.
Short URL = http://is.gd/Paradox
