Pain reduced when enough vitamin D was given – review
Vitamin D Supplementation for Pain
US Pharm. 2015;40(3):43-46.
Christan M. Thomas, PharmD, Assistant Clinical Professor, St. John’s University, College of Pharmacy, Jamaica, New York
Clinical Pharmacist, Lymphoma/Multiple Myeloma, New York-Presbyterian/Weill Cornell Medical Center. New York, New York
Peter Campbell, PharmD, PGY-2 Resident, Hematology/Oncology, New York-Presbyterian Hospital. New York, New York
Vitamin D, a fat-soluble vitamin found in few natural food sources, is synthesized in human skin after sun exposure. Up to 80% of patients in U.S. healthcare facilities are deficient in vitamin D, which is thought to contribute to a wide range of health issues. Vitamin D has long been utilized in combination with calcium to improve bone health and reduce the risk of fractures. Vitamin D supplementation has been linked to the prevention of high blood pressure, cancer, and other diseases. Recent research also points to a possible association between vitamin D deficiency and chronic pain.
Vitamin D is a fat-soluble vitamin. In humans, two forms are used—ergocalciferol (vitamin D2) and cholecalciferol vitamin (D3). While D2 is primarily synthesized by plants, sunlight can promote synthesis of D3 in human skin. Since few foods naturally contain vitamin D, dermal synthesis is typically the main source of vitamin D. Natural food sources include egg yolks and fish. Certain varieties of cereal, milk, and orange juice are fortified with vitamin D by the manufacturer.1,2
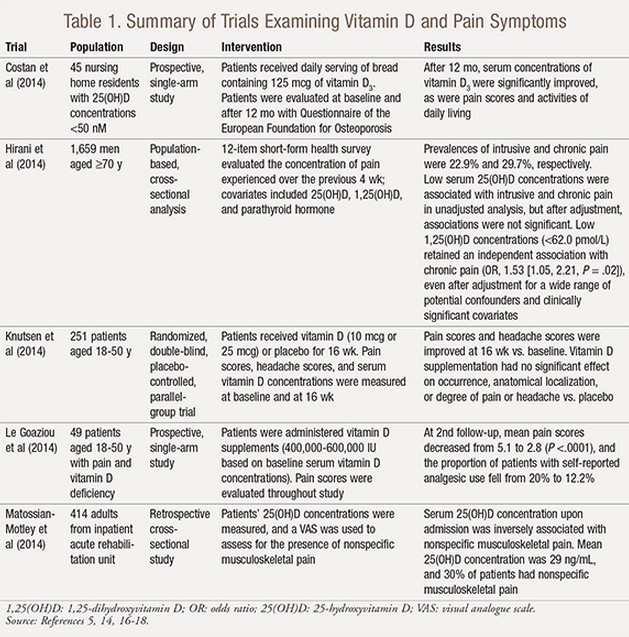
Table 1
Background
In humans, vitamin D helps maintain normal concentrations of serum calcium and phosphorus by regulating absorption and excretion. Thus, vitamin D is a key player in bone homeostasis and formation. Vitamin D has long been given alone or in combination with calcium to improve bone health and reduce the risk of fractures. Some sources suggest that vitamin D supplementation may prevent high blood pressure, cancer, and other diseases.3,4
It is estimated that 50% to 80% of patients in U.S. healthcare facilities are deficient in vitamin D.5 Recent research also points to a possible association between low vitamin D concentrations and chronic pain. This pain may or may not respond to traditional therapies. In these patients, vitamin D supplementation may help control the pain.
Mechanism and Pharmacokinetics
Vitamin D is a hormone precursor that controls calcium absorption in the small intestine. In humans, vitamin D obtained from sun exposure, food, and supplements is biologically inert. To become active, vitamin D must undergo two separate hydroxylations in the body.6
In the liver, the first hydroxylation converts vitamin D to 25-hydroxyvitamin D (25(OH)D). This form, also known as calcidiol, has a half-life of approximately 3 weeks. The second hydroxylation takes place primarily in the kidney. After this step, the physiologically active 1,25-dihydroxyvitamin D (1,25(OH)2D) is formed. This type of vitamin D, also known as calcitriol, has a much shorter half-life of 4 to 6 hours.6,7
Once activated, vitamin D is responsible for the regulation of calcium and phosphate homeostasis.6,7 Vitamin D maintains normal serum concentrations of these minerals by enhancing the absorption efficiency of the small intestine.8 When dietary calcium intake is insufficient, the body signals monocytic stem cells in the bone marrow to become mature osteoclasts. In turn, these osteoclasts mobilize calcium from the bones in order to maintain calcium concentrations in the blood.9
Dietary vitamin D is well absorbed from the small intestine, primarily in the duodenum and jejunum.8 It is mainly excreted in bile, but a small amount is reabsorbed in the small intestine.8
Vitamin D and Health
According to the National Institutes of Health’s Office of Dietary Supplements, the serum concentration of 25(OH)D is the best indicator of vitamin D status.9,10 This measurement incorporates both the vitamin D produced through sun exposure and that obtained from food and supplements. However, the NIH notes that although the 25(OH)D concentration functions as a biomarker of exposure to vitamin D, it is unclear how it relates to overall health status or outcomes. Additionally, the serum 25(OH)D concentration does not reflect the vitamin D that may be stored in body tissues. 9,10 Circulating 1,25(OH)2D is not considered a good indicator of vitamin D. The 1,25(OH)2D concentration typically does not decrease until vitamin D deficiency is severe. 9,10
Although there is some debate about what constitutes vitamin D deficiency, the Institute of Medicine (IOM) suggests that serum 25(OH)D concentrations <30 nmol/L (<12 ng/mL) indicate a risk of deficiency. Concentrations of 30 to 50 nmol/L (12-20 ng/mL) indicate a potential risk of inadequate vitamin D. For most people, concentrations 50 nmol/L (20 ng/mL) constitute sufficient vitamin D. In contrast, concentrations >125 nmol/L (>50 ng/mL) may be associated with adverse effects, primarily hypercalcemia.9,10
Most people are able to obtain at least some vitamin D from daily sunlight exposure. The amount of vitamin D produced in the skin, however, may be affected by climate and other environmental factors. In addition, skin exposure must be balanced with prevention of sunburns and skin cancer.9-12
The recommended daily allowance of vitamin D varies by age. The IOM recommends a daily dietary allowance of 600 IU/day for most adults. Adults >70 years should consume 800 IU/day.9,10
Vitamin D concentrations may drop when normal intake is lowered, sunlight exposure decreases, or disruptions in activation or metabolism occur.9,10 In children, vitamin D deficiency may lead to rickets, which causes soft bones and skeletal deformities. In adults, vitamin D deficiency can result in decreased bone density.9,10 Research suggests that sufficient vitamin D concentrations may contribute to the prevention and treatment of disorders such as cancer, hypertension, glucose intolerance, and multiple sclerosis.7,11,12
Vitamin D Deficiency and Pain
Currently, there is controversy over the role vitamin D deficiency plays in pain occurrence. While some studies have demonstrated no correlation between pain concentrations and vitamin D, others have found an increased incidence of chronic pain with serum vitamin D concentrations <20 ng/mL.5 Along with an increased frequency of chronic and nonspecific musculoskeletal pain, these patients often report a poorer quality of life.13 The type of pain associated with vitamin D deficiency varies, but it generally presents as chronic musculoskeletal or generalized bone pain.14
The correlation between serum vitamin D concentrations and pain has been studied in various types of pain, including chronic pain, musculoskeletal pain, rheumatoid arthritis, obesity-associated back pain, and headaches.5,13,15,16 The mechanism of vitamin D in pain symptoms depends greatly upon the type of pain involved. While it is thought that vitamin D may contribute to the release of inflammatory cytokines in rheumatoid arthritis, in musculoskeletal pain it is believed that vitamin D may decrease the sensitivity of nerve fibers in the muscles.15,17 Observational and placebo-controlled studies and meta-analyses have been conducted to investigate the correlation between vitamin D concentrations and pain symptoms.
See TABLE 1 for a summary of trials.
In an epidemiologic study conducted by Hirani and colleagues, vitamin D concentrations and pain symptoms were investigated in 1,659 men aged >70 years.14 A 12-item short-form health survey evaluated the concentration of pain experienced over the previous 4 weeks, and the Physical Activity Scale for the Elderly was used to assess each patient’s level of physical activity. Patients with low vitamin D concentrations had a higher incidence of both intrusive and chronic pain, but statistical significance was lost after adjustment for covariates. Chronic pain incidence retained significance in patients in the lowest quartile of vitamin D concentrations compared with incidence in those in the highest quartile, even after adjustment for covariates.14
A retrospective observational study by Matossian-Motley and colleagues reviewed the records of 414 adults admitted to a rehabilitation facility over a 1-year period.5 Patients’ serum vitamin D concentrations were recorded, along with visual analogue scale (VAS) pain-intensity scores upon admission. Patients with vitamin D concentrations <20 ng/mL had higher odds of nonspecific musculoskeletal pain (adjusted odds ratio [OR], 2.33; 95% CI, 1.23-4.17) compared with those with serum vitamin D concentrations >20 ng/mL. Similarly, patients with serum vitamin D concentrations <30 ng/mL had higher odds of nonspecific musculoskeletal pain (adjusted OR, 2.04; 95% CI, 1.15-3.57) compared with patients with serum vitamin D concentrations >30 ng/mL. Adjustment for the use of supplemental vitamin D and environmental season at time of admission did not significantly change the results.5
In a prospective, randomized, double-blind, placebo-controlled study by Knutsen and colleagues, the change in pain from baseline with administration of vitamin D was examined.16 Patients received vitamin D 10 mcg, vitamin D 25 mcg, or placebo for 16 weeks. At baseline and again at 16 weeks, patients were assessed using a VAS for pain intensity and a blank body mannequin for pain location, and serum nonfasting vitamin D concentrations were measured. Compared with baseline, there was no significant difference in VAS pain severity, pain location, or use of painkillers between the vitamin D and placebo groups at 16 weeks. Although not statistically significant, there was an improvement in VAS pain severity in all groups.16
Another prospective study, conducted by Le Goaziou and colleagues, examined the effect of vitamin D supplementation on pain in 49 patients who presented to their physician with complaints of diffuse musculoskeletal pain and were determined to have low serum vitamin D concentrations.17 Patients were administered high doses of vitamin D (400,000-600,000 IU) based on the severity of the vitamin D deficit. Pain was assessed (according to location, duration, intensity, and analgesic use) at baseline and after intervention. At second follow-up, patients’ mean pain scores dropped from 5.1 to 2.8 (P <.0001), and the proportion of patients self-reporting analgesic use declined from 20% to 12.2% (P = .03).17
The use of fortified foods has also been investigated as a means of vitamin D supplementation. Costan and colleagues administered a daily serving of bread containing 125 mcg of vitamin D3 to 45 nursing home residents.18 After 12 months, serum vitamin D3 concentrations were significantly improved, as were pain scores and activities of daily living.18
While most studies have examined the association between vitamin D concentrations and pain, some studies have also investigated vitamin D concentrations and surrogate markers for inflammation and pain.15 In a retrospective analysis by Hong and colleagues, the correlation between vitamin D concentrations and inflammatory cytokines and disease status was evaluated in patients with rheumatoid arthritis.15 Patients with lower concentrations of vitamin D had significantly higher instances of disease symptoms such as swollen joints, joint stiffness, and joint pain. Also, vitamin D concentrations were negatively associated with the presence of inflammatory cytokines, in particular interleukin-17 and interleukin-23.15
Conclusion
Between 50% and 80% of patients in U.S. healthcare facilities are deficient in vitamin D. Although many foods and drinks are fortified with supplementary vitamin D, the amounts are often insufficient for normal serum concentrations. Although research has demonstrated mixed results regarding pain incidence and serum vitamin D concentrations, observational and prospective studies suggest that correction of vitamin D concentrations may decrease pain of multiple origins. Vitamin D supplementation in patients with low serum concentrations may be an easy and safe way to decrease pain occurrences.
REFERENCES
1. Holick MF. Vitamin D: photobiology, metabolism, mechanism of action, and clinical applications. In: Favus MJ, ed. Primer on the Metabolic Bone Diseases and Disorders of Mineral Metabolism. 3rd ed. Philadelphia, PA: Lippincott-Raven; 1996:92-98.
2. Holick MF. Vitamin D: a millenium perspective. J Cell Biochem. 2003;88:296-307.
3. Holick MF. Sunlight and vitamin D for bone health and prevention of autoimmune diseases, cancers, and cardiovascular disease. Am J Clin Nutr. 2004;80(suppl 6):1678S-1688S.
4. Christakos S, Dhawan P, Benn B, et al. Vitamin D: molecular mechanism of action. Ann N Y Acad Sci. 2007;1116:340-348.
5. Matossian-Motley DL, Drake DA, Samimi JS, et al. Association between serum 25(OH)D level and nonspecific musculoskeletal pain in acute rehabilitation unit patients. JPEN J Parenter Enteral Nutr. October 14, 2014 [Epub ahead of print].
6. Brannon PM, Yetley EA, Bailey RL, Picciano MF. Overview of the conference “Vitamin D and Health in the 21st Century: an Update.” Am J Clin Nutr. 2008;88(suppl):483S-490S.
7. Kulie T, Groff A, Redmer J, et al. Vitamin D: an evidence-based review. J Am Board Fam Med. 2009;22:698-706.
8. Rodríguez-Martínez MA, García-Cohen EC. Role of Ca(2+) and vitamin D in the prevention and treatment of osteoporosis. Pharmacol Ther. 2002;93:37-49.
9. Institute of Medicine. Dietary Reference Intakes for Calcium and Vitamin D. Washington, DC: National Academies Press; 2011.
10. National Institutes of Health. Vitamin D fact sheet for professionals. http://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional. Accessed November 12, 2014.
11. Forrest KY, Stuhldreher WL. Prevalence and correlates of vitamin D deficiency in US adults. Nutr Res. 2011;31:48-54.
12. Yetley EA. Assessing the vitamin D status of the US population. Am J Clin Nutr. 2008;88:558S-564S.
13. Powanda MC. Is there a role for vitamin D in the treatment of chronic pain? Inflammopharmacology. 2014;22:327-332.
14. Hirani V, Blyth FM, Naganathan V. Active vitamin D (1,25 dihydroxyvitamin D) is associated with chronic pain in older Australian men: The Concord Health and Ageing in Men Project. J Gerontol A Biol Sci Med Sci. August 7, 2014 [Epub ahead of print].
15. Hong Q, Xu J, Xu S, et al. Associations between serum 25-hydroxyvitamin D and disease activity, inflammatory cytokines and bone loss in patients with rheumatoid arthritis. Rheumatology (Oxford). 2014;53:1994-2001.
16. Knutsen KV, Madar AA, Brekke M, et al. Effect of vitamin D on musculoskeletal pain and headache: a randomized, double-blind, placebo-controlled trial among adult ethnic minorities in Norway. Pain. 2014;155:2591-2598.
17. Le Goaziou MF, Kellou N, Flori M, et al. Vitamin D supplementation for diffuse musculoskeletal pain: results of a before-and-after study. Eur J Gen Pract. 2014;20:3-9.
18. Costan AR, Vulpoi C, Mocanu V, et al. Vitamin D fortified bread improves pain and physical function domains of quality of life in nursing home residents. J Med Food. 2014;17:625-631.
