Shingles and vitamin D
Summary: Vitamin D and Magnesium both treat shingles
Shingles worse with low vitamin D, low UV, high latitude, and winter
Treating shingles with Vitamin D or UV lowers the pain
Treating shingles with Vitamin D almost eliminates the risk of recurrence
Vitamin D has even been patented to help with shingles
- A patent is always a good sign that it probably works
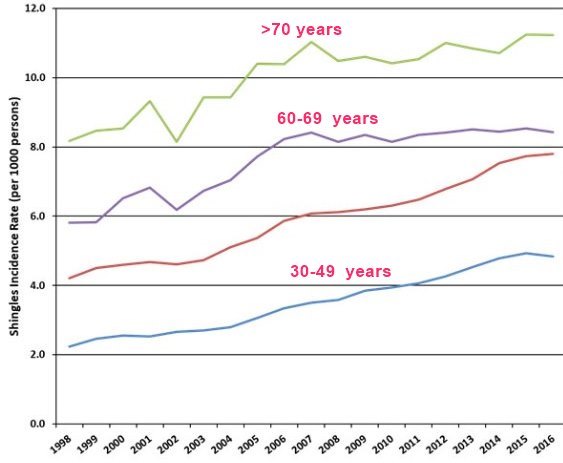
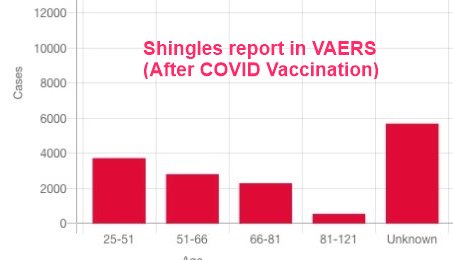
2X increase in younger age-groups
see also: Incidence of 22 health problems related to vitamin D have doubled in a decade
all are associated with low Vitamin D
See also VitaminDWiki
The role of solar ultraviolet irradiation in zoster file, not a webpage
See on the web
Use Google to search for (zoster OR shingles) magnesium 7,180,000 as of Feb 2023
Prevent Herpes Outbreaks With Vitamin D HerpesBulletin 2012
Bill Sardi April 2014
50,000 IU of vitamin D, and shingles pain subsides in an hour or two- VitaminDWiki suggests sublingual pill, spray, powder -Bio-Tech or topical for fast action
- Person applied Vitamin D directly on Shingles and also took 15,000 IU internally daily in May 2016
- Shingles disappeared in 3 days, and pain in 5 days
- Shingles Vaccine Dangers Exposed In FDA Letter to Merck GreenMed Info May 2017
- "Despite the fact that the CDC claims that the shingles vaccine carries no real risks, the FDA wrote to Merck in February 2016 telling them to add, ‘Eye Disorders: necrotizing retinitis (patients on immunosuppressive therapy)’ to their product information.' "
- "With the meningitis vaccine, is it worth killing three children and making 1000 more seriously ill to prevent one case of the disease?"
- "Additionally, most people think that most vaccines control the spread of disease, but they don't. Many control how sick anyone gets should they come down with the disease, but the vaccine does not control the spread of that disease."
- vaccination for COVID and shingles should be separated by at least 14 days. ConsumerLab April 2021
Hypothesis- Shingles associated with low vitamin D – Oct 2015
Vitamin D is closely linked to the clinical courses of herpes zoster: From pathogenesis to complications
Medical Hypothesis, Volume 85, Issue 4, Pages 452–457, October 2015
Chia-Ter Chao, Chih-Kang Chiang, Jenq-Wen Huangcorrespondenceemail, Kuan-Yu Hung
Table of contents

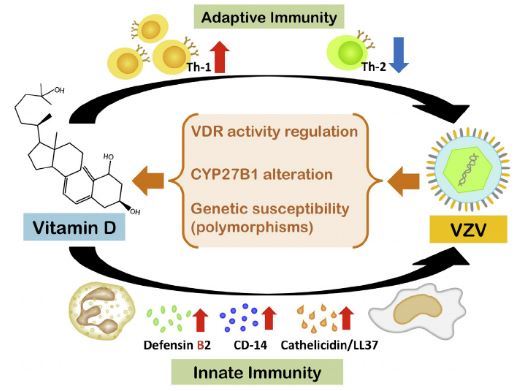
Vitamin D is renowned for its pleiotropic effects, including but not limited to bone integrity, and it has assumed an important role in the current research era. As vitamin D receptors are present in a variety of human tissues, particularly immune cells, the immunomodulatory potential of vitamin D cannot be overemphasized. Herpes zoster, which presents as grouped cutaneous vesicles over dermatomes or visceral/central nervous system infection in its severe form, has a higher incidence in immune-suppressed patients.
Considering the importance of vitamin D in host immunity, we hypothesize that vitamin D acts as an effect-modifier for the entire herpes zoster spectrum with regard to
disease susceptibility,
manifestation,
efficacy of pharmacologic management, and
emergent complications during treatment.
Moreover, the possibility exists that vitamin D might affect the course of postherpetic neuralgia. In line with this theory, we comprehensively searched the existing herpes zoster literature and provided important insight into the relationship between the disease courses of herpes zoster and vitamin D.
📄 Download the PDF from sci-hub via VitaminDWiki
The Varicella-Zoster Virus and Multiple Sclerosis
Journal of Clinical Epidemiology Volume 51, Issue 7, Pages 533-535 (July 1998)
R.T. Rossa
This article reviews the evidence suggesting a unique relationship between the varicella-zoster virus (as a possible antigen or antigen mimic) and multiple sclerosis (MS). Both MS and varicella have increased prevalences in temperate zones, and both are rare in countries closer to the equator . Migration studies suggest an infectious agent acquired prior to age 14 plays a role in the risk of subsequent MS. Hutterites, who educate their children at home, have less varicella, MS, and herpes zoster than their neighbors and have the appropriate reduced varicella-zoster seropositivity matching these clinical observations. Paradoxically, patients with MS report more herpes zoster at an earlier age and more often than a group of non-MS patients.
Zoster patients: With UV 58% pain-free, without UV 38% pain-free - 2006
Broad-band ultraviolet B phototherapy in zoster patients may reduce the incidence and severity of postherpetic neuralgia.
Photodermatol Photoimmunol Photomed. 2006 Oct;22(5):232-7.
Jalali MH, Ansarin H, Soltani-Arabshahi R.
Department of Dermatology, Hazrat-e Rasool University Hospital, Iran University of Medical Sciences, Tehran, Iran.
BACKGROUND: Postherpetic neuralgia (PHN) is one of the common complications of herpes zoster infection, particularly in the elderly. Current therapeutic measures are only partially effective in the affected patients. As inflammatory mediators released by different cells play an important role in the pathogenesis of this neuropathic pain and regarding the immunomodulatory effects of the ultraviolet B (UVB) spectrum, we presumed that UVB phototherapy might be effective in preventing PHN.
METHOD: This study was performed in two phases. Phase I was a prospective open controlled trial. Twenty-five patients with severe pain in the first 7 days of zoster rash were divided into two groups: the prevention group (n=12) received oral acyclovir (800 mg five times a day for 10 days) plus broad-band UVB to the affected dermatomes, starting with 20 mJ/cm(2) and gradually increasing the dose by 10 mJ/cm(2) each session to a maximum dose of 100 mJ/cm(2). Treatment sessions were repeated thrice a week until pain relief or to a maximum of 15 sessions. The control group (n=13), with disease characteristics similar to the prevention group, received only oral acyclovir with the same dose. All patients reported their severity of pain on a verbal rating scale (VRS, score 0-4) before treatment and at 1 and 3 months follow-up. In phase II of the study, five patients with established PHN (more than 3 months after rash onset) received UVB with the above-mentioned protocol.
RESULTS: A total of 17 patients older than 40 (10 females, seven males; mean age, 65.5 years; range: 47-82 years) who had intractable pain due to zoster infection received UVB in two phases of the study. In patients who received phototherapy in the first 7 days of rash, 58.33% and 83.33% were completely pain-free at 1-and 3-month follow-up. The corresponding figure in the control group was significantly lower (38.46% at 1 month and 53.85% at 3 months). The severity of pain was also lower in the phototherapy group than in the control group (mean VRS 2.50 vs. 3.28 at 3 months). None of the patients who were treated more than 3 months after rash onset (established PHN) experienced significant (more than 50%) pain relief.
CONCLUSION: UVB phototherapy in the acute stage of zoster rash might reduce the incidence and severity of PHN.
Treatment after 3 months does not seem to have a significant beneficial effect.
16X less likely to get Zoster during hemodialysis if added vitamin D drug - 2012
Risk factors for herpes zoster reactivation in maintenance hemodialysis patients
Eur J Intern Med. 2012 Sep 5.doi: 10.1016/j.ejim.2012.08.005
Chao CT, Lai CF, Huang JW.
OBJECTIVE:
Herpes zoster (HZ) reactivation is common in immunocompromised patients. Advanced renal failure is also reportedly associated with impairment of cellular immunity. No study has yet assessed the risk factors of HZ reactivation in hemodialysis patients.
METHODS:
All patients undergoing maintenance hemodialysis for over 3 months and who developed HZ between 2000/01/01 and 2009/12/31 in a tertiary referral medical center were identified and matched 1:1 to hemodialysis patients without HZ by age and gender.
A multivariate-adjusted conditional logistic regression model was constructed to determine possible risk factors.
RESULTS:
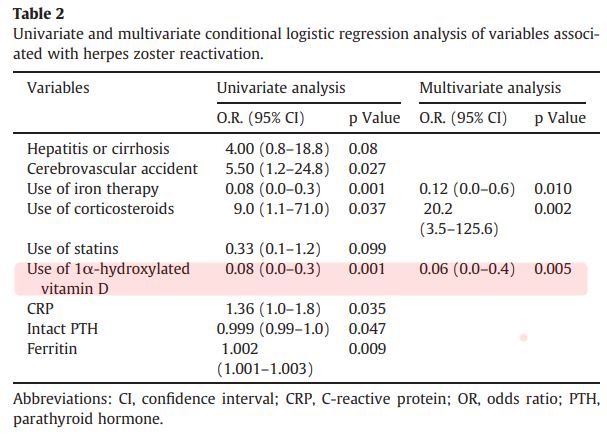
Out of a total of 126 maintenance hemodialysis patients (65.3% female), 63 belonged to the HZ reactivation group and 63 to the age/sex-matched control patients. Conditional logistic regression model linked corticosteroid use with heightened risk (odds ratio [OR] 20.2, 95% confidence interval [CI] 3.5-125.6; p=0.002),
While iron therapy and 1-apha-hydroxylated vitamin D were associated with a significantly lower likelihood of developing HZ (OR 0.12, 95%CI 0.0-0.6; p=0.01, and OR 0.06 , 95% CI 0.0-0.4; p=0.005 respectively).
CONCLUSIONS: Iron preparations and 1?-hydroxylated vitamin D are potentially associated with less risk of developing HZ reactivation in maintenance hemodialysis patients.
📄 Download the PDF from VitaminDWiki
Herpes Zoster Is Associated with Prior Statin Use: A Population-Based Case-Control Study
Published: October 24, 2014DOI: 10.1371/journal.pone.0111268 PLOS ONE
Shiu-Dong Chung is an equal contributor, Ming-Chieh Tsai is an equal contributor,
Shih-Ping Liu, Herng-Ching Lin, Jiunn-Horng Kang mail
Background: This study investigated the association between statin use and herpes zoster (HZ) occurrence in a population-based case-control study.
Methods
Study subjects were retrieved from the Taiwan Longitudinal Health Insurance Database 2000. This study included 47,359 cases with HZ and 142,077 controls. We performed conditional logistic regression analyses to calculate the odds ratio (OR) to present the association between HZ and having previously been prescribed statin.
Results
We found that 13.0% of the sampled subjects had used statins, at 15.5% and 12.1% for cases and controls, respectively (p<0.001).
Conditional logistic regression analysis suggested that the adjusted OR of being a statin user before the case index date was 1.28 (95% confidence interval (CI): 1.24~1.32) compared to controls.
Subjects aged 18~44 years had the highest adjusted OR for prior statin use among cases compared to controls (OR: 1.69; 95% CI: 1.45~1.92).
Furthermore, we found that the ORs of being a regular and irregular statin user before the index date for cases were 1.32 (95% CI: 1.27~1.38) and 1.23 (95% CI: 1.181.29), respectively, compared to controls.
Conclusions
We concluded that prior statin use was associated with HZ occurrence.
📄 Download the PDF from VitaminDWiki.
See also VitaminDWiki
Pain following shingles 3X more likely if less than 30 ng of Vitamin D – Nov 2019
Hypovitaminosis Din Postherpetic Neuralgia-High Prevalence and Inverse Association with Pain: A Retrospective Study
Nutrients. 2019 Nov 15;11(11). pii: E2787. doi: 10.3390/nu11112787.
Chen JY1,2, Lin YT1, Wang LK1, Hung KC1, Lan KM1, Ho CH3, Chang CY4,5.
Hypovitaminosis D (25-hydroxyvitamin D (25(OH)D) <75 nmol/L) is associated with neuropathic pain and varicella-zoster virus (VZV) immunity. A two-part retrospective hospital-based study was conducted. Part I (a case-control study): To investigate the prevalence and risk of hypovitaminosis D in postherpetic neuralgia (PHN) patients compared to those in gender/index-month/age-auto-matched controls who underwent health examinations. Patients aged ≥50 years were automatically selected by ICD-9 codes for shingle/PHN. Charts were reviewed. Part II (a cross-sectional study): To determine associations between 25(OH)D, VZV IgG/M, pain, and items in the DN4 questionnaire at patients' first pain clinic visit. Independent predictors of PHN were presented as adjusted odds ratios(AOR) and 95% confidence intervals (CI). The prevalence (73.9%) of hypovitaminosis D in 88 patients was high. In conditional logistic regressions, independent predictors for PHN were hypovitaminosis D (AOR3.12, 95% CI1.73-5.61), malignancy (AOR3.21, 95% CI 1.38-7.48), and Helicobacter pylori-related peptic ulcer disease (AOR3.47, 95% CI 1.71-7.03). 25(OH)D was inversely correlated to spontaneous/brush-evoked pain. Spontaneous pain was positively correlated to VZV IgM. Based on the receiver operator characteristic curve, 25(OH)D cutoffs to predict spontaneous and brush-evoked pain were 67.0 and 169.0 nmol/L, respectively. A prospective, longitudinal study is needed to elucidate the findings.
📄 Download the PDF from VitaminDWiki
Shingles Vaccine Shingrix approved in US - Fall 2017
No Excuses, People: Get the New Shingles Vaccine New York Times
Perhaps 90% effective for elderly
Costs over $150, Medicare will cover Shingrix under Part D
two Vaccinations needed
Remains effective ~5 years
About half of those over age 70 reported more systemic side effects like fatigue, fever, or aching joints, lasting one to two days
$9,520 of Shringrix to vaccinate 34 people to prevent one case of Shingles - April 2018
Dr. Brownstein: New Shingrix Vaccine for Shingles Fails 97% of Time April 9, 2018
"Six people out of 7,344 who received the two doses of Shingrix developed shingles—that is 0.08%. 210 out of 7,415 people who received the placebo became ill with shingles—that is 3%. How do they get 98% efficacy out of these numbers? Again, I have written about how the Big Pharma Cartel manipulates statistics to make a poorly performing drug or therapy look better than it actually is by using relative risk (RR).
"The ARR for this study can be calculated here: 3%-0.08%=2.9%. Therefore, a more appropriate determination of the effectiveness of Shingrix is that it is 2.9% effective at preventing shingles for a median of 3.1 years (the length of the study). And a true statement about Shingrix is that it takes 34 people to be vaccinated with Shingrix (1/2.9%) to prevent one case of shingles .
Note: PDR listing shows Shringrix is far less efficient for those over age 80
Dr. Greger likes the Shingles vaccine - 5 minute video April 2024
Adult vaccination can be thought of as a cornerstone of successful aging, but a major issue hampering the uptake of shingles vaccination is the lack of awareness of the disease. Shingles is caused by a reactivation of the chicken pox virus later in life. After your body beats back chicken pox, the virus hides in waiting in your spinal cord, waiting for an opportunity to strike back. When it does, the virus can surge forth, traveling along the path of a nerve branching off the spinal cord, wrapping around one side of the body to the front, producing skin blisters along the way in a characteristic belt-like pattern that does not cross the midline in front. (Both shingles and the name of the virus, zoster, are from the Latin and Greek, respectively, for “belt”).
The blistering rash can be intensely painful and leave scarring or discoloration behind but usually disappears in a few weeks on its own. However, approximately 30 to 50 percent of people suffer “postherpetic neuralgia,” persistent pain that can last for a year or more, that sometimes can be debilitating. Usually, it affects nerves around your trunk, but in 10 to 25 percent of cases, it can erupt across your face, which can lead to permanent facial muscle weakness, hearing loss, or blindness. As if that’s all not bad enough, having shingles as much as quintuples your odds of having a stroke over the subsequent few weeks, a risk that gradually declines over the following six to twelve months.
It’s surprising more people don’t know about it, since the lifetime risk of shingles is 30 percent ––meaning nearly one in three will get it sometime in their lives. Young adults only have about a one in 1,000 chance of getting it every year, whereas in older adults that climbs to closer to one in 100 each year . That comes out to a million cases of shingles every year in the United States. Thankfully, there is a shingles vaccine.
The first became available in 2006, using a live weakened strain of the virus. The efficacy was only about 50 percent, and couldn’t be used in immunocompromised individuals, such as those with HIV or on immunosuppressive drugs, such as many on chemotherapy. Thankfully, in 2017, a recombinant shingles vaccine was approved, with a 90 to 97 percent efficacy for preventing an outbreak. It requires two separate injections 2 to 6 months apart and is expensive ($280) , but covered by Medicare and most private insurance plans. It also can cause transient systemic symptoms, such as muscle aches, fatigue, headaches, or fever and chills serious enough to interfere with everyday activities about 10 percent of the time. But the new vaccine is considered so much more effective that it’s recommended for everyone starting at age 50, even if you were previously immunized with the old one. Given that the new vaccine is only about five years old, longer-term safety and efficacy data are still coming in, but, so far so good. As soon as I turned 50, I lined up for mine.
Founder of VitaminDWiki (age 75) got shingles on his left neck and shoulder in April 2021
My physician's assistant prescribed Valacyclovir 3 times per day orally, + triamcinolone Acetonide topical ointment on the rash.
Also took Topical vitamin D, Magnesium and treated with Low-Level Laser Therapy.
The slight pain was gone in 1 week, and the rash was gone in 2 weeks.
Shingles risk increases 15% with COVID, and if COVID vaccine is in those under age 50 – Jan 2023
Shingles Activation Associated With COVID Jab Mercola Jan 2023
- "Another study details the cases of six patients with autoimmune inflammatory rheumatic diseases who developed shingles shortly after their Pfizer jabs. None of the healthy controls developed shingles post-jab."
Persistent varicella-zoster virus infection following mRNA COVID-19 vaccination was associated with the presence of encoded spike protein in the lesion- Aug 2022 https://doi.org/10.1002/cia2.12278 FREE PDF
Assessment of Herpes Zoster Risk Among Recipients of COVID-19 Vaccine Nov 2022 doi:10.1001/jamanetworkopen.2022.42240 FREE PDF
- did NOT find an increased risk of Herpes Zoster
Real-world evidence from over one million COVID-19 vaccinations is consistent with reactivation of the varicella-zoster virus - April 2022 https://doi.org/10.1111/jdv.18184 FREE PDF.
"The researchers found that 0.2% and 0.11% of vaccinated and unvaccinated individuals developed shingles in the 60 days after their clinic visits."
1.8X increased risk - did not appear to mention age
