Less labor pain if higher level of vitamin D
Effect of intrapartum vitamin D levels on labor pain
J Obstet Gynaecol Res. 2021 Aug 9. doi: 10.1111/jog.14960 Publisher will rent the PDF for $14
Refika G Koyucu 1, Tuğba Özcan 2
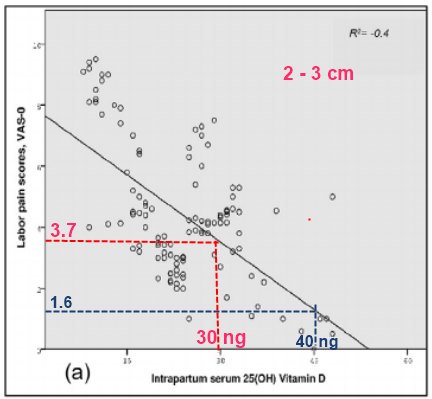
Zero pain at 2-3 cm with 50 ng?
 1. See also web
* Could Vitamin D Make Childbirth Less Painful? webmd Oct 2014
* [Reviesw of this study by GrassrootsHealth](https://www.grassrootshealth.net/blog/higher-vitamin-d-levels-associated-lower-labor-pain-scores/?utm_source=newsletter-main&utm;_medium=email&utm;_campaign=Newsletters)
1. See also web
* Could Vitamin D Make Childbirth Less Painful? webmd Oct 2014
* [Reviesw of this study by GrassrootsHealth](https://www.grassrootshealth.net/blog/higher-vitamin-d-levels-associated-lower-labor-pain-scores/?utm_source=newsletter-main&utm;_medium=email&utm;_campaign=Newsletters)

Aim: Vitamin D has widespread receptor distribution in the body, and therefore it has vital roles in numerous pathophysiological conditions. It also affects pain manifestation through its functions at various stages of the pain pathways. This study aimed to investigate the effects of intrapartum vitamin D levels on pain experienced by women during the first stage of labor.
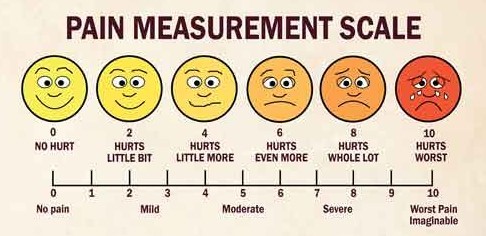
Methods: A total of 127 term-nulliparous women at the early stage of labor were included in the study. Serum 25 (OH) vitamin D levels were measured at the beginning of labor to determine intrapartum vitamin D levels. Labor pain was assessed using the Visual Analog Scale at different stages of cervical dilation (VAS0 , VAS1 , VAS2 ). Postpartum pain (VASpp ) and women's birth satisfaction score (BSS) were also evaluated during the early postpartum period.
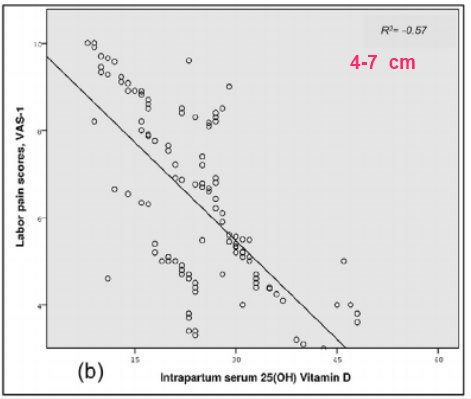
Results: There was a moderate negative correlation between vitamin D and VAS0 and VAS1 (r2 = 0.4, p = 0.000; r2 = -0.570, p = 0.000, respectively), and a weak negative correlation between vitamin D and VAS2 (r2 = -0.373, p = 0.000). No significant correlation was found between vitamin D and BSS and length of labor (p = 0.127, p = 0.126, respectively).
Conclusion: In nulliparous women with low vitamin D levels, the first stage of labor and the early postpartum period may be more painful. To facilitate management of labor pain, during the antenatal period vitamin D levels should be monitored, and in cases where the levels are deficient, vitamin D supplementation should be started.
References
Deuster E, Jeschke U, Ye Y, Mahner S, Czogalla B. Vitamin D and VDR in gynecological cancers-a systematic review. Int J Mol Sci. 2017;18:2328.
Bikle DD. Vitamin D metabolism, mechanism of action, and clinical applications. Chem Biol. 2014;21:319-29. https://doi.org/10.1016/j.chembiol.2013.12.016
Shipton EA, Shipton EE. Vitamin D and pain: vitamin D and its role in the aetiology and maintenance of chronic pain states and associated comorbidities. Pain Res Treat. 2015;2015:904967.
Aziato L, Acheampong AK, Umoar KL. Labour pain experiences and perceptions: a qualitative study among post-partum women in Ghana. BMC Pregnancy Childbirth. 2017;17:1-9.
Jones L, Othman M, Dowswell T, Alfirevic Z, Gates S, Newburn M, et al. Pain management for women in labour: an overview of systematic reviews. Cochrane Database Syst Rev. 2012;2012:CD009234.
Mårtensson L, Wallin G. Sterile water injections as treatment for low-back pain during labour: a review. Aust N Z J Obstet Gynaecol. 2008;48:369-74.
Melzack R, Schaffelberg D. Low-back pain during labor. Am J Obstet Gynecol. 1987;156:901-5.
Lowe NK. The pain and discomfort of labor and birth. J Obstet Gynecol Neonatal Nurs. 1996;25:82-92. https://doi.org/10.1111/j.1552-6909.1996.tb02517.x
Imai K. Elevated maternal serum C-reactive protein levels and neonatal infection in term pregnancy. Clin Obstet Gynecol Reprod Med. 2020;6:1-5.
De Meeus JB, Pourrat O, Gombert J, Magnin G. C-reactive protein levels at the onset of labour and at day 3 post-partum in normal pregnancy. Clin Exp Obstet Gynecol. 1998;25:9-11.
Hirshberg JS, Tuuli MG, Stout MJ, Conner SN, Lopez JD, Macones GA, et al. 465: what is the threshold of maternal leukocytosis in labor associated with maternal or neonatal morbidity? Am J Obstet Gynecol. 2017;216:S274. https://doi.org/10.1016/j.ajog.2016.11.723
Tita ATN, Andrews WW. Diagnosis and management of clinical chorioamnionitis. Clin Perinatol. 2010 Jun;37:339-54.
Delgado DA, Lambert BS, Boutris N, McCulloch PC, Robbins AB, Moreno MR, et al. Validation of digital visual analog scale pain scoring with a traditional paper-based visual analog scale in adults. J Am Acad Orthop Surg Glob Res Rev. 2018;2:e088-8.
Martin CH, Fleming V. The birth satisfaction scale. Int J Health Care Qual Assur. 2011;24:124-35.
Cetin FC, Sezer A, Merih YD. The birth satisfaction scale: Turkish adaptation, validation and reliability study. North Clin Istanb. 2015;2:142-50.
National Institutes of Health. Vitamin D [Internet]. 2021. Available from: https://ods.od.nih.gov/factsheets/Vitamind-HealthProfessional/
Atherton K, Berry DJ, Parsons T, Macfarlane GJ, Power C, Hyppönen E. Vitamin D and chronic widespread pain in a white middle-aged British population: evidence from a cross-sectional population survey. Ann Rheum Dis. 2009;68:817-22.
Lotfi A, Abdel-Nasser AM, Hamdy A, Omran AA, El-Rehany MA. Hypovitaminosis D in female patients with chronic low back pain. Clin Rheumatol. 2007;26:1895-901.
Lowe NK. The nature of labor pain. Am J Obstet Gynecol. 2002;186:S16-24. Available from:. https://www.sciencedirect.com/science/article/pii/S0002937802701798
Ropers S, Tran Q, Geller AW, Lamb A, Hobel C, Zakowski MI. Effect of vitamin D levels on intrapartum epidural consumption [internet]. Am Soc Anesthesiologists. 2014; Available from: http://www.asaabstracts.com/strands/asaabstracts/abstract.htm?year=2014&...
Helde-Frankling M, Björkhem-Bergman L. Vitamin D in pain management. Int J Mol Sci. 2017;18:2170.
Olson DM, Ammann C. Role of the prostaglandins in labour and prostaglandin receptor inhibitors in the prevention of preterm labour. Front Biosci. 2007;12:1329-43.
Boulvain M, Kelly A, Irion O. Intracervical prostaglandins for induction of labour. Cochrane Database Syst Rev. 2008;1:CD006971.
Li QB, Chang L, Ye F, Luo QH, Tao YX, Shu HH. Role of spinal cyclooxygenase-2 and prostaglandin E2 in fentanyl-induced hyperalgesia in rats. Br J Anaesth. 2018;120:827-35. https://doi.org/10.1016/j.bja.2017.11.103
Liu W, Zhang L, Xu H-J, Li Y, Hu C-M, Yang J-Y, et al. The anti-inflammatory effects of vitamin D in tumorigenesis. Int J Mol Sci. 2018;19:2736.
Barcikowska Z, Rajkowska-Labon E, Grzybowska ME, Hansdorfer-Korzon R, Zorena K. Inflammatory markers in dysmenorrhea and therapeutic options. Int J Environ Res Public Health. 2020;17:1191.
Zeynali M, Haghighian HK. Is there a relationship between serum vitamin D with dysmenorrhea pain in young women? J Gynecol Obstet Hum Reprod. 2019;48:711-4.
Bahrami A, Avan A, Sadeghnia HR, Esmaeili H, Tayefi M, Ghasemi F, et al. High dose vitamin D supplementation can improve menstrual problems, dysmenorrhea, and premenstrual syndrome in adolescents. Gynecol Endocrinol. 2018 Aug;34:659-63.
Tournaire M, Theau-Yonneau A. Complementary and alternative approaches to pain relief during labor. Evid Based Complement Alternat Med. 2007;4:409-17.
Ross A, Manson J, Abrams S, Aloia J, Brannon P, Clinton S, et al. The 2011 report on dietary reference intakes for calcium and vitamin D from the Institute of Medicine: what clinicians need to know. J Clin Endocrinol Metab. 2011;96:53-8.
Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2011;96:1911-30.
Hollis BW, Wagner CL. Vitamin D and pregnancy: skeletal effects, nonskeletal effects, and birth outcomes. Calcif Tissue Int. 2013;92:128-39.
Amrein K, Scherkl M, Hoffmann M, Neuwersch-Sommeregger S, Köstenberger M, Tmava Berisha A, et al. Vitamin D deficiency 2.0: an update on the current status worldwide. Eur J Clin Nutr. 2020;74:1498-513. https://doi.org/10.1038/s41430-020-0558-y
American College of Obstetricians and Gynecologists. ACOG Committee opinion no. 742: postpartum pain management. Obstet Gynecol. 2018;132:e35-43.
Deussen AR, Ashwood P, Martis R, Stewart F, Grzeskowiak LE. Relief of pain due to uterine cramping/involution after birth. Cochrane Database Syst Rev. 2020;10(10):CD004908. https://doi.org/10.1002/14651858.CD004908.pub3
Direkvand-Moghadam A, Delpisheh A, Rezaeian M, Khosravi A. Factors affecting the labor: a review article. Biomed Pharmacol J. 2013;6:161-7.
Gernand A, Klebanoff M, Simhan D, Bodnar L. Maternal vitamin D status, prolonged labor, and cesarean and instrumental delivery in an era with a low cesarean rate. J Perinatol. 2015;35:23-8.
Jafari E, Mohebbi P, Mazloomzadeh S. Factors related to Women's childbirth satisfaction in physiologic and routine childbirth groups. Iran J Nurs Midwifery Res. 2017;22:219-24.
