Less cognitive decline in women consuming more Magnesium (and vitamins)
Relations of magnesium intake to cognitive impairment and dementia among participants in the Women’s Health Initiative Memory Study: a prospective cohort study
BMJ Open http://dx.doi.org/10.1136/bmjopen-2019-030052
Kenneth Lo1,2, Qing Liu2, Tracy Madsen2,3, Steve Rapp4, Jiu-Chiuan Chen5, Marian Neuhouser6, Aladdin Shadyab7, Lubna Pal8, Xiaochen Lin2, Sally Shumaker4, JoAnn Manson9, Ying-Qing Feng1, Simin Liu2,10
📄 Download the PDF from VitaminDWiki
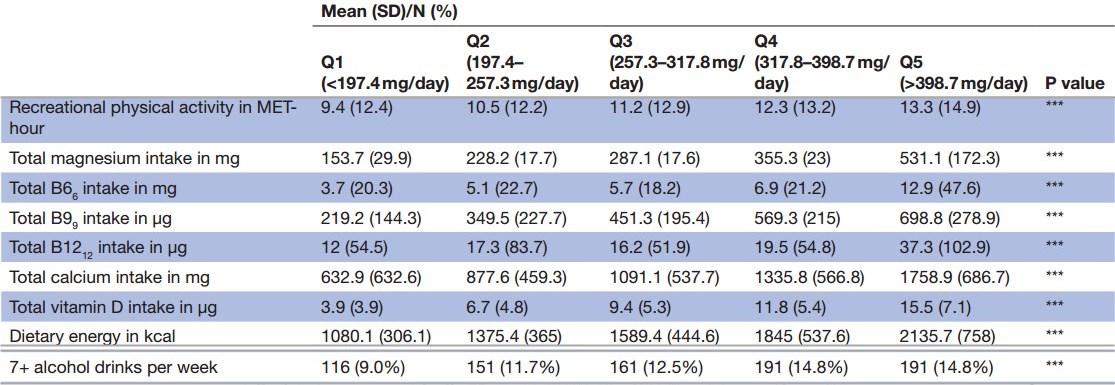
Many vitamins increase with increase in Magnesium
Objective To examine the associations of dietary and supplemental magnesium (Mg) as assessed by a semi-quantitative food frequency questionnaire with cognitive outcomes among ageing women.
Design This work conducts a prospective cohort study of participants enrolled in the Women’s Health Initiative Memory Study (WHIMS), which was subsequently extended and named WHIMS-Epidemiology of Cognitive Health.
Setting Forty clinical centres in the USA.
Participants Postmenopausal women aged 65–79 years without dementia on enrollment.
Main outcome measures Physician-adjudicated mild cognitive impairment (MCI) and/or probable dementia (PD).
Results Participants were excluded (n=1006) if they had extreme values of dietary energy intake, had missing or extreme body mass index values, with prevalent MCI/PD at baseline, received only one cognitive assessment or had been followed up for <1 year. During >20 years of follow-up, 765 (11.8%) out of 6473 participants developed MCI/PD. For MCI/PD and MCI, the risks tended to be lower among participants in quintiles Q2–Q5 of Mg consumption compared with those in the lowest quintile. Participants in Q3 had a significantly lower risk of MCI/PD (HR 0.69, 95% CI 0.53 to 0.91) and MCI (HR 0.63, 95% CI 0.45 to 0.87) after multivariate adjustments. No significant association was observed between total Mg intake and PD. The association between total Mg intake, MCI/PD and MCI was non-linear as suggested by the likelihood test.
Conclusions Total Mg intake between the estimated average requirement and the recommended dietary allowances may associate with a lower risk of MCI/PD and MCI.
Trial registration number NCT00685009.
Strengths and limitations of this study
A large prospective cohort with long follow-up and careful adjudication of mild cognitive impairment/probable dementia events to ensure a high quality of outcome assessment.
Lacking information on serum magnesium levels in the studied population.
The cohort included only postmenopausal women, and the findings may not be generalisable to elderly men.
