Kidney Inflammation: both prevented and reduced by Vitamin D – review
Vitamin D and the Immune System from the Nephrologist's Viewpoint
ISRN Endocrinology; Volume 2014 (2014), Article ID 105456, 11 pages, http://dx.doi.org/10.1155/2014/105456
Cheng-Lin Lang,1 Min-Hui Wang,2 Chih-Kang Chiang,3 and Kuo-Cheng Lu2
1 Department of Internal Medicine, Cardinal Tien Hospital, Yonghe Branch, New Taipei 23445, Taiwan
2 Division of Nephrology, Department of Internal Medicine, Cardinal Tien Hospital, School of Medicine, Fu-Jen Catholic University, 362 Chung-Cheng Road, Hsin-Tien District, New Taipei 23148, Taiwan
3 Division of Nephrology, Department of Internal Medicine, National Taiwan University Hospital, College of Medicine, National Taiwan University, Taipei 10002, Taiwan
Received 25 October 2013; Accepted 4 December 2013; Published 22 January 2014
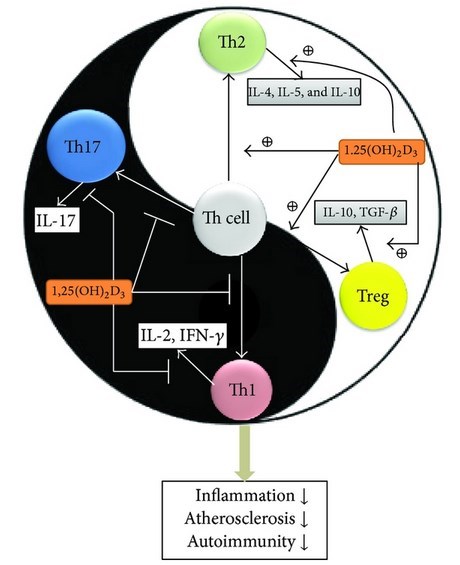
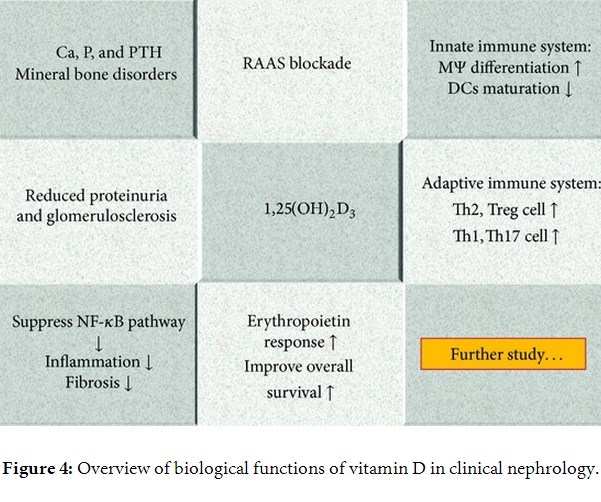
Vitamin D and its analogues are widely used as treatments by clinical nephrologists, especially when treating chronic kidney disease (CKD) patients with secondary hyperparathyroidism. As CKD progresses, the ability to compensate for elevations in parathyroid hormone (PTH) and fibroblast growth factor-23 and for decreases in 1,25(OH)2D3 becomes inadequate, which results in hyperphosphatemia, abnormal bone disorders, and extra-skeletal calcification. In addition to its calciotropic effect on the regulation of calcium, phosphate, and parathyroid hormone, vitamin D has many other noncalciotropic effects, including controlling cell differentiation/proliferation and having immunomodulatory effects. There are several immune dysregulations that can be noted when renal function declines. Physicians need to know well both the classical and nonclassical functions of vitamin D. This review is an analysis from the nephrologist's viewpoint and focuses on the relationship between the vitamin D and the immune system, together with vitamin's clinical use to treat kidney diseases.
Images from PDF
PDF is attached at the bottom of this page
See also VitaminDWiki
Kidney Inflammation not reduced by 30 ng Vitamin D (many health problems need 50 ng) – Nov 2022
Overview Kidney and vitamin D contains
{include}
