Possible ways that vitamin D does its magic
Expect that within a few years we will know that the vitamin D magic is
One of these ways
Several of these ways
Some nnumber of these ways + ways not yet proposed
Personally, I am rooting for DNA repair
- because it sounds so good, not because any better case has been made. Henry Lahore March 2012
Vitamin D and cancer: a review of molecular mechanisms. (Jan 2012)
Biochem J. 2012 Jan 1;441(1):61-76.
Fleet JC, Desmet M, Johnson R, Li Y.
Purdue University Interdisciplinary Life Sciences Program, Purdue University, West Lafayette, IN 47907-2059, U.S.A.
The population-based association between low vitamin D status and increased cancer risk can be inconsistent, but it is now generally accepted. These relationships link low serum 25OHD (25-hydroxyvitamin D) levels to cancer, whereas cell-based studies show that the metabolite 1,25(OH)2D (1,25-dihydroxyvitamin D) is a biologically active metabolite that works through vitamin D receptor to regulate gene transcription.
In the present review we discuss the literature relevant to the molecular events that may account for the beneficial impact of vitamin D on cancer prevention or treatment.
These data show that although
vitamin D-induced growth arrest and
apoptosis of tumour cells or their non-neoplastic progenitors are plausible mechanisms, other *chemoprotective mechanisms are also worthy of consideration.
These alternative mechanisms include
enhancing DNA repair,
antioxidant protection and
immunomodulation.
In addition, other cell targets, such as the
stromal cells,
endothelial cells and
cells of the immune system,
may be regulated by 1,25(OH)2D and contribute to vitamin D-mediated cancer prevention.
PMID: 22168439
Cellular and molecular effects of vitamin D on carcinogenesis (Nov 2011)
Archives of Biochemistry and Biophysics, doi:10.1016/j.abb.2011.10.019
JoEllen Welsh Corresponding Author Contact Information, E-mail The Corresponding Author
Cancer Research Center, University at Albany, Rensselaer, NY 12144, USA
Received 21 September 2011; Available online 9 November 2011
Epidemiologic data suggest that the incidence and severity of many types of cancer inversely correlates with indices of vitamin D status. The vitamin D receptor (VDR) is highly expressed in epithelial cells at risk for carcinogenesis including those resident in skin, breast, prostate and colon, providing a direct molecular link by which vitamin D status impacts on carcinogenesis. Consistent with this concept, activation of VDR by its ligand 1,25-dihydroxyvitamin D (1,25D) triggers comprehensive genomic changes in epithelial cells that contribute to maintenance of the differentiated phenotype, resistance to cellular stresses and protection of the genome. Many epithelial cells also express the vitamin D metabolizing enzyme CYP27B1 which enables autocrine generation of 1,25D from the circulating vitamin D metabolite 25-hydroxyvitamin D (25D), critically linking overall vitamin D status with cellular anti-tumor actions. Furthermore, pre-clinical studies in animal models has demonstrated that dietary supplementation with vitamin D or chronic treatment with VDR agonists decreases tumor development in skin, colon, prostate and breast. Conversely, deletion of the VDR gene in mice alters the balance between proliferation and apoptosis, increases oxidative DNA damage, and enhances susceptibility to carcinogenesis in these tissues.
Because VDR expression is retained in many human tumors, vitamin D status may be an important modulator of cancer progression in persons living with cancer. Collectively, these observations have reinforced the need to further define the molecular actions of the VDR and the human requirement for vitamin D in relation to cancer development and progression.
Does vitamin D protect against DNA damage? (Feb 2012)
Mutat Res. 2012 Feb 23.
Nair-Shalliker V, Armstrong BK, Fenech M.
Cancer Epidemiology Research Unit, Cancer Council New South Wales.
Vitamin D is a secosteroid best known for its role in maintaining bone and muscle health. Adequate levels of vitamin D may also be beneficial in maintaining DNA integrity. This role of vitamin D can be divided into a primary function that prevents damage from DNA and a secondary function that regulates the growth rate of cells.
The potential for vitamin D to reduce oxidative damage to DNA in a human has been suggested by clinical trial where vitamin D supplementation reduced 8-hydroxy-2'-deoxyguanosine, a marker of oxidative damage, in colorectal epithelial crypt cells.
Studies in animal models and in different cell types have also shown marked reduction in oxidative stress damage and chromosomal aberrations, prevention of telomere shortening and inhibition of telomerase activity following treatment with vitamin D.
The secondary function of Vitamin D in preventing DNA damage includes regulation of the poly-ADP-ribose polymerase activity in the DNA damage response pathway involved in the detection of DNA lesions.
It is also able to regulate the cell cycle to prevent the propagation of damaged DNA, and to regulate apoptosis to promote cell death. Vitamin D may contribute to prevention of human colorectal cancer, though there is little evidence to suggest that prevention of DNA damage mediates this effect, if real. Very limited human data mean that the intake of vitamin D required to minimise DNA damage remains uncertain.
Copyright © 2012. Published by Elsevier B.V.
PMID: 22366026
See also VitaminDWiki
Common Vitamin D gene variants and resulting diseases – Jan 2013
VitaminDWiki Blog post: How vitamin D deals with Cancer Feb 2012
Mechanisms of the Anti-Cancer and Anti-Inflammatory - 2011.PDF which has the following
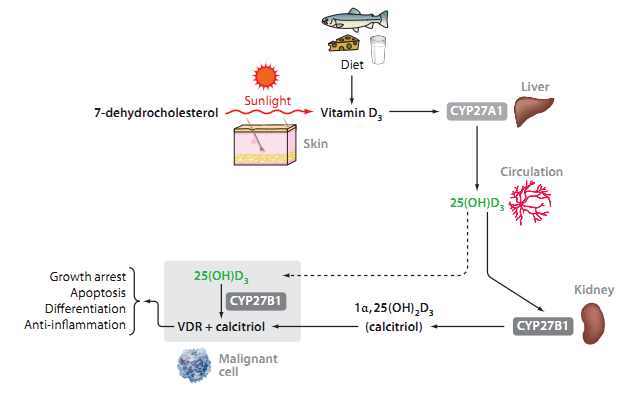

Vitamin D for prevention and treatment of Cancer - technical July 2010 file
Cancers and Vitamin D Council and Dr. Grant
Video on how Vitamin D reduces Cancer – Feb 2011 Dr. Garland
Search several other websites on vitamin D topics - such as Cancer
Vitamin D and Cancer Treatment and Prevention – presentations May 2011 which has the following


See also Web
GrassRoots Health Many papers and videos on Cancer and Vitamin D - especially Breast Cancer
Vitamin D and DNA repair Jan 2012 Vitamin D Councill -you must be a subscriber
