Breastfed Infants in Iowa got very little vitamin D, especially if winter or dark skin
Pediatrics 2006;118;603 DOI: 10.1542/peds.2006-0108
Ekhard E. Ziegler, Mda ekhard-ziegler@ uiowa.edu, Bruce W. Hollis, PhDb, Steven E. Nelson, BAa,Janice M.Jeter, RNa
aDepartment of Pediatrics, University of Iowa, Iowa City, Iowa; bDepartments of Pediatrics, Biochemistry, and Molecular Biology, Medical University of South Carolina, Charleston, South Carolina
^ See also VitaminDWiki
Overview Pregnancy and vitamin D
Items in both categories Infant-Child andSkikn-Dark are listed here:
{category}
Child bone conference: many vitamin D and ricket abstracts – June 2013
400 IU vitamin D was insufficient for 6 percent born of Vitamin D-Deficient Mothers – June 2013
Most European infants get vitamin D supplements, vs only 1 in 50 in US – June 2013
Breastfed infants: 90 percent had less than 20 ng of vitamin D, formula-fed: 15 percent – May 2013
Group is giving only 200 IU of Vitamin D to 70 million women and children to prevent Rickets
Black infants had far lower vitamin D levels which did not vary with season – Jan 2013
Third study found that Infants needed 1600 IU of vitamin D – JAMA RCT May 2013
Breastfed without vitamin D supplements – a problem for NZ infants Jan 2013
Only about 10 percent of breastfed infants get even the minimum recommended vitamin D – April 2010
most of the text, a few of the charts follow
. PDF with all of the text and charts is attached at the bottom of this page ^
OBJECTIVE. The purpose of this work was to assess the vitamin D status of breastfed infants living in Iowa (latitude: 41°N).
METHODS. Blood samples and dietary records from 84 breastfed infants participating in another study were used for a survey of vitamin D status at 280 days of age. The vitamin D status of those (35 infants) who did not receive preformed vitamin D at 280 days of age (unsupplemented infants) was assessed longitudinally between 112 days and 15 months of age. Plasma 25-hydroxyvitamin D and, in most cases, parathyroid hormone and alkaline phosphatase were determined.
RESULTS.At 280 days of age, 10% of breastfed infants were vitamin D deficient (25-hydroxyvitamin D <11 ng/mL). Deficiency was significantly more prevalent among dark-skinned infants and during winter and occurred exclusively in unsupplemented infants. During winter, 78% of unsupplemented infants were vitamin D deficient. During summer, only 1 infant who had dark skin pigmentation was vitamin D deficient. Longitudinal assessment of unsupplemented infants similarly showed that the majority of breastfed infants were vitamin D deficient during winter. Severe deficiency (25-hydroxyvitamin D <5 ng/mL) was common and was accompanied by elevation of parathyroid hormone and alkaline phosphatase. The prevalence of vitamin D deficiency decreased with age but was still 12% at 15 months of age if no preformed vitamin D was received.
CONCLUSIONS. Vitamin D deficiency, including severe deficiency, was common among breastfed infants in Iowa who did not receive preformed vitamin D. Deficiency occurred mostly during winter but was not completely absent during summer. It affected infants with light as well as dark skin pigmentation. Consumption of preformed vitamin D from vitamin supplements or formula is effective in preventing vitamin D deficiency. Vitamin D supplementation should be provided to all breastfed infants.
INFANTS ARE CAPABLE of producing all of the vitamin D they need in their skin during casual exposure to sunlight, provided the sunlight is of sufficient intensity. At northern latitudes, the power of sunlight is attenuated, especially during winter, so that little or no vitamin D is formed in the skin.1 Heavy skin pigmentation reduces the amount of vitamin D formed in the skin, which is why infants with dark skin pigmentation tend to be in less satisfactory vitamin D status than infants with light skin pigmentation2 and why they are at increased risk of vitamin D deficiency rickets.3-5 Infants living at northern latitudes depend on ingestion of preformed vitamin D for the maintenance of vitamin D sufficiency during winter and possibly year round in the case of infants with darkly pigmented skin. The amount of preformed vitamin D required by infants in the absence of endogenous synthesis is not exactly known but is thought to be between 100 and 200 international units (IU) per day . A daily intake of 400 IU of vitamin D is believed to prevent rickets reliably and is considered free of adverse effects.6 The Institute of Medicine considers 200 IU per day to be an adequate intake for infants.7
The breastfed infant receives preformed vitamin D in breast milk, the vitamin D content of which is lower in winter than in summer8,9 and is lower in black women than in women with light skin pigmentation.2 During winter in northern locations, the vitamin D content of breast milk is typically —10 to 30 IU/L and, thus, would seem insufficient to meet the infant's vitamin D needs. That breastfed infants are at risk of vitamin D deficiency has long been appreciated.6 Vitamin D supplementation of breastfed infants has been and continues to be recommended by the American Academy of Pediatrics.6,10-13 The recommended daily dose has long been 400 IU per day but was recently lowered to 200 IU per day.12 Vitamin D supplementation is recommended for all breastfed infants who receive <200 IU (<500 mL of formula) in addition to breastfeeding. Despite these recommendations, many health care providers do not prescribe vitamin supplements14-17 for breastfed infants.
In the course of a study concerning iron nutrition in breastfed infants, we became aware that few infants living in and around Iowa City were receiving supplemental vitamin D. The latitude of the area (—41°N) is such that vitamin D formation during the winter months should be low even with direct exposure to sunlight. We also knew that formula supplementation, although common, was often started late in the first year of life or not provided at all. We, thus, hypothesized that breastfed infants in the community were at risk of vitamin D deficiency, in particular during the winter months. Meanwhile, reports of vitamin D deficiency16 and outright rickets among breastfed infants kept appearing.3-5 We, therefore, undertook to assess the vitamin D status of breastfed infants participating in the study. Plasma that was left after completion of laboratory determinations for the iron study was used for determination of 25-hydroxyvitamin D (25-OHD) concentration and, if plasma volume permitted, of parathyroid hormone (PTH) concentration and alkaline phosphatase (AP) activity. We now report that vitamin D deficiency does indeed occur among breastfed infants, especially during winter months.
METHODS
Study Design
The parent study was a prospective, randomized trial of breastfed infants who were enrolled at 28 days of age and followed until 24 months of age. The study was composed of a control group with no intervention and 2 intervention groups who received different forms of iron supplementation (medicinal iron or iron-fortified cereal) between 112 and 280 days of age. At enrollment, infants were exclusively breast fed. They could receive supplemental formula beginning at 112 days of age, and there were some restrictions with regard to the types of complementary foods that they could receive after 112 days of age. There were no restrictions regarding the use of vitamin supplements. Infants visited the study center every 28 days during the first year of life and every 3 months during the second year of life and had blood drawn by heel stick at predetermined ages.
Assessment of vitamin D status was undertaken while the parent study was still in progress and 87 infants had reached at least 280 days of age. Vitamin D status could be assessed in 84 of these infants, who were born between October 2001 and March 2002. By parental report, 49 of these infants received some preformed vitamin D, either from formula (any amount of formula;N = 45), from vitamin supplements (N = 3), or both (N = 1;"supplemented" infants). The remaining 35 infants did not receive preformed vitamin D ("unsupplemented" infants) by parental report. Comparison of supplemented and unsupplemented infants at age 280 days constituted the first part of the present study. The second part was a longitudinal assessment of all 35 of the infants that were unsupplemented before and at 280 days of age (but in many cases not at subsequent ages). Longitudinal assessment was performed with plasma, where available, obtained at 112, 168, 224, 280, and 364 days and 15 months of age. In both parts of the study, determination of plasma 25-OHD concentration was given priority, with determinations of PTH and AP performed if sufficient plasma was available. Because of the retrospective nature of the study, physical or radiologic examination for signs of rickets could not be performed.
Subjects and Feedings
Subjects were term infants of either gender with birth weight >2500 g who were considered normal by their physicians and the investigators. They were recruited by visits to local maternity units, advertisements, and word of mouth. Family characteristics were not recorded. Iowa City is a relatively affluent community with a high education level. Many families of study infants were affiliated with the University of Iowa.
Seven of the 84 infants belonged to racial groups other than white (3 Asian, 3 black, and 1 Pacific Islander) and had noticeably more darkly pigmented skin than the white infants. Four of the 7 infants with dark skin did not receive preformed vitamin D at any time. Of the 35 infants in the longitudinal sample, 4 had dark skin pigmentation.
In the longitudinal sample, of 30 infants who were available at 12 months of age, 11 were still being breast fed without formula or vitamin supplementation, whereas the remaining infants received cow milk or formula alone or in combination with breastfeeding. At 15 months of age, 6 of 23 available infants were breast fed without supplemental milk or formula. Formulas and milk sold in the area provided >400 IU of vitamin D per liter.
The study protocol of the parent study and of the assessment of vitamin D status were reviewed and approved by the institutional review board, and parents provided written consent.
Procedures
Parents completed an infant diet questionnaire at each of the monthly study visits. This recorded the amount and type, if any, of formula, milk, and other foods, as well as nutritional supplements consumed by the infant. Information about the mother's diet and her use of supplements was not obtained. At the visits at 28, 112, 168, 224, and 280 days of age and at all of the visits thereafter, samples of capillary blood were obtained by heel stick using a disposable spring-loaded device (Tenderfoot, International Technidyne Corporation, Edison, NJ). Approximately 1 mL of blood was collected, and 0.5 mL was placed into heparin-treated tubes and 0.5 mL into ethylenediaminetetraacetic acid (EDTA)-treated tubes. The blood was centrifuged immediately and plasma separated from cells. Concentration of 25-OHD in either EDTA or heparin plasma (50 juL) was determined by radioimmunoassay.18 The assay had an intra-assay coefficient of variation of 6% and interassay coefficient of variation of 15%. AP was determined in heparin plasma (25 juL) by a colorimetric method using p-nitrophenol as described by Moss and Henderson19 using a commercially available kit (Procedure No. 104, Sigma Diagnostics, St Louis, MO). Intact PTH was determined in EDTA plasma (200 juL) by an immunoradiometric assay (Nichols Institute Diagnostics, San Clemens, CA).
Data Analysis
Vitamin D deficiency was defined as 25-OHD plasma concentration <11 ng/mL (27.5 nmol/L).7,8,20-22 Although higher cutoffs for 25-OHD have been proposed, especially for adult subjects, in the pediatric literature, 11 ng/mL has been used most widely, and that cutoff has therefore been retained. To define a more severe degree of vitamin D deficiency, a cutoff of 5 ng/mL was used. Elevated PTH was defined as concentration >28.1 pg/ mL, which is the 95th percentile for infants in the present study with 25-OHD concentration >11 ng/mL. Although solar winter comprises the period from November to February, for the purpose of this study, winter was defined as the period November through April and summer as May through October.
In the cross-sectional assessment, comparisons of subgroups (eg, summer versus winter) were made using the Wilcoxon rank sum test, but the test was applied only when there were >4 values in each cell. Relationships with other variables were explored using linear regression analysis and Spearman rank correlation. In the longitudinal assessment, the effect of season was assessed for each age group by Wilcoxon rank sum test, and the prevalence of vitamin D deficiency was assessed by continuity-adjusted x2 tests and by Fisher's exact test. The Kruskal-Wallis test was used to compare data across 25-OHD categories (Table 3).
RESULTS
Cross-Sectional Assessment at 280 Days of Age
Eight infants (10%) were vitamin D deficient with plasma 25-OHD concentrations <11 ng/mL (Table 1). Two of these infants (1 dark skinned) had 25-OHD concentrations <5 ng/mL. Dark-skinned infants had significantly lower plasma 25-OHD concentrations than light-skinned infants and were significantly more likely to be vitamin D deficient (43% vs 6%). In unsupplemented infants, plasma 25-OHD levels were significantly lower, and vitamin D deficiency was more prevalent (23% vs 0%) than in those who received preformed vitamin D. There was a marked seasonal effect on 25-OHD levels, with more infants being vitamin D deficient during winter (37%) than during summer (2%). The seasonal effect was particularly pronounced among unsupplemented infants, 78% of whom were vitamin D deficient during winter compared with only 4% during summer (P = .001). No supplemented infants were vitamin D deficient.
Also shown in Table 1 are data for AP and PTH. Although there was the occasional elevated AP value, there were no significant differences in AP activity between vitamin D-deficient and -sufficient subjects. AP activity and 25-OHD levels were not significantly correlated ( P = .29). PTH concentrations, on the other hand, were significantly higher in vitamin D-deficient than in vitamin D-sufficient subjects, and the (inverse) correlation (r =-0.344;P = .067) with 25-OHD was of borderline significance. PTH levels were significantly higher in dark-skinned than light-skinned infants. PTH was highest during winter in subjects who did not receive preformed vitamin D.
TABLE 1 Vitamin D Status Indicators of 84 Breastfed Infants at 280 Days of Age (From Cross-Sectional Assessment)
Longitudinal Assessment
Data for the 35 unsupplemented infants are summarized in Table 2. At all of the ages, concentrations of 25-OHD were significantly lower during winter than during summer, and a greater proportion of infants were vitamin D deficient during winter than during summer. Nevertheless, vitamin D deficiency did occur during summer, and, although it occurred predominantly in dark-skinned infants, white infants were not spared. The prevalence of vitamin D deficiency decreased with age but was still found during winter at 15 months of age in 3 subjects who were all breast fed without milk or formula supplementation.
Data from 6 infants (all white) born in October (Fig 1) illustrate the seasonal changes in 25-OHD levels. During January and February (at 112 days of age), 5 infants were vitamin D deficient and remained so during March and April (at 168 days of age). 25-OHD levels rose beginning in May, no doubt as a result of increasing sunlight exposure of the infants and/or their mothers. During the ensuing fall and winter, all remained in adequate vitamin D status; all but 1 started to receive milk at —12 months of age.
Severe vitamin D deficiency (25-OHD <5 ng/mL) was observed in 22 infants (4 with dark skin) on 38 occasions (36 in winter and 2 in summer). As Table 3 shows, when severe deficiency was present, PTH and AP levels were significantly elevated. Mild deficiency (25-OHD 5-11 ng/mL), on the other hand, was not associated with elevated PTH or AP. Twelve subjects were severely deficient on 2 occasions. Their mean PTH and AP values were 24.8 ± 25.2 pg/mL and 234 ± 222 U/L, respectively. Thus, persistent severe deficiency was not associated with greater elevation of PTH and AP than severe deficiency of shorter duration. One additional subject, a dark-skinned infant belonging to a Muslim family, had severe deficiency on 5 occasions. On 1 of the occasions, AP was elevated (1251 U/L) but was back to normal 3 months later. Attempts to contact the family failed, because the family had in the interim left the country.
TABLE 2 Plasma 25-OHD Concentrations in 35 Unsupplemented Breastfed Infants at Various Ages (from Longitudinal Assessment)
TABLE 3 Vitamin D Status Indicators From Longitudinal Assessment, Grouped by 25-OHD Level
FIGURE 1 Plasma 25-OHD concentrations of all 6 of the unsupplemented infants born in October
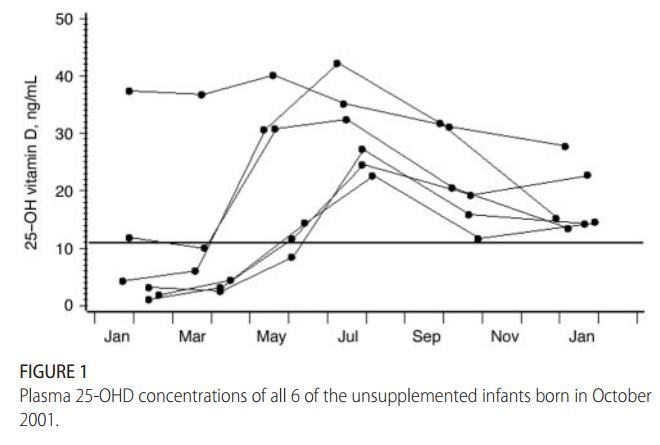
FIGURE 2 Relation between PTH and 25-OHD concentrations.
All of the available values are shown. Horizontal line indicates the 95th percentile of PTH in vitamin D-sufficient infants.
The relationship between 25-OHD and PTH is further illustrated in Fig 2, which is based on all of the available data. It is evident that elevated PTH levels (>28.1 pg/ mL) were seen mostly when 25-OHD levels were <5ng/mL. The 4 elevated PTH levels observed in the presence of higher 25-OHD levels belonged to 3 infants who had earlier had 25-OHD levels <5 ng/mL on 1 or 2 occasions. By linear regression analysis, the (inverse) relationship between 25-OHD and PTH was statistically significant (r =— 0.244;P = .013). The inverse relation between 25-OHD and AP was not statistically significant by Pearson coefficient (r =—0.113;P = .167) but was significant by Spearman rank coefficient (r =— 0.193;P = .013).
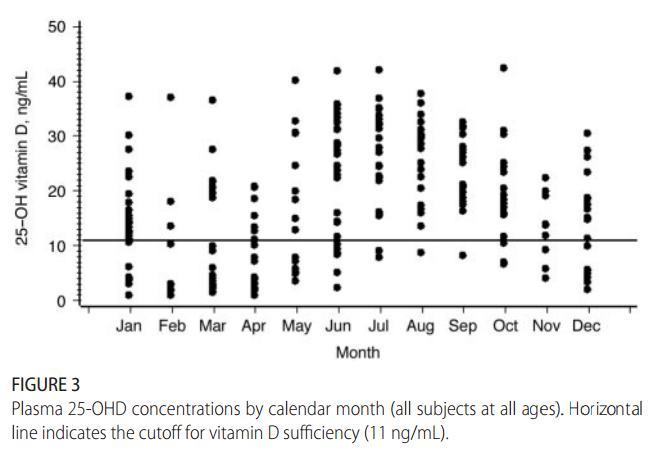
Fig 3 presents a summary of all 25-OHD data by time of year.
The strong seasonal influence on 25-OHD concentrations is evident, but even during early summer there were many values in the deficient range.
By late summer (August to October) only a handful of infants ( N = 5), 3 of whom were white, remained mildly vitamin D deficient.
DISCUSSION
It was to be expected to find some vitamin D deficiency among breastfed infants, but what was surprising was the extent and the severity of the deficiency that was encountered. It was particularly surprising to find vita min D deficiency among white infants and not only among black infants. Deficiency was present during winter in the great majority of infants who did not receive preformed vitamin D, whereas during summer it was found only occasionally. As expected, vitamin D deficiency was not found among infants who received preformed vitamin D.
FIGURE 3
Vitamin D deficiency was often severe (defined as plasma 25-OHD levels <5 ng/mL) but, although it typically persisted for several months, was in most cases self-limited. Severe vitamin D deficiency was accompanied by elevation of PTH. Increased secretion of PTH is induced by persistent hypocalcemia because of vitamin D deficiency.23 It is often associated with parathyroid hyperplasia, which explains why elevated PTH levels may persist for some time after normalization of vitamin D status, as was observed in the present study. The significance of elevated PTH levels is that they document long-lasting vitamin D deficiency. Elevation of AP suggested the presence of mild rickets. However, the presence of rickets could not be verified, because the retrospective nature of the study precluded the performance of physical and/or radiologic examinations.
Some additional limitations of the study must be noted. PTH and AP could not be determined in all instances. We could, therefore, have missed some elevated PTH and AP values. How representative the study population was of the general population is difficult to determine. Participation in the parent study was restricted to infants whose mothers planned to breastfeed for >6 months. Participation placed certain demands on the parents (monthly visits) and imposed some dietary restrictions (although none pertaining to vitamin supplements). The study population was probably representative of infants in the community who are breastfed for >6 months. Infants who are breastfed for 6 months probably come from families that are more educated or more affluent than the general population. We have no reason to suspect that participation would have interfered with the use of vitamin supplements. Thus, the low rate of supplement use is probably representative of use in the community at the time of the study.
Of the 38 infants who did not receive supplemental formula at 280 days of age, only 3 (8%) received vitamin supplements by parental report (1 additional infant received vitamin supplements but also received formula). Two additional study infants had persistently high plasma 25-OHD levels suggesting that they may have been receiving vitamin supplements despite parental reports to the contrary (plasma 25-OHD levels of 1 of these infants are shown in Fig 1). If we include these 2 infants, the proportion of infants receiving vitamin supplements was still only 13%. Vitamin supplements were started before 112 days of age in 3 infants and between 112 and 224 days of age in 3. Reluctance of health care providers to prescribe vitamin D supplements for breastfed infants has been documented for several locations.14-17 The predominant reason is the belief that vitamin D is not needed by breastfed infants, perhaps based on misperceptions regarding the effectiveness of sunlight exposure at northern latitudes during winter. Sunlight exposure is not likely to produce vitamin D during winter at northern latitudes. Furthermore, exposure of infants to sunlight faces practical difficulties in the cold climes prevailing in the northern United Sates during winter. The current recommendation by the American Academy of Pediatrics states that vitamin D supplements are needed "until the daily consumption of vitamin D-fortified formula or milk is 500 mL."13
The breastfed infant is at risk of vitamin D deficiency, because the same factors that limit endogenous synthesis of vitamin D in the infant simultaneously limit cutaneous synthesis in the mother and, thus, cause the vitamin D content of breast milk to be low. Antirachitic activity of breast milk (determined with use of bioassays) was reported to be 4-22 IU/L,24 whereas values obtained with specific chemical methods have generally been somewhat higher. Breast milk contains the parent vitamins (D2 and D3) and their 25-hydroxylation products (25-OHD2 and 25-OHD3) as well as all other metabolites
that are present in plasma.25,26 Most of the antirachitic activity of breast milk resides in 25-OHD.2,9,25,26 In Finland, the vitamin D content of breast milk, determined by chemical methods, averaged 14 IU/L in February and 124 IU/L in September.9 Thus, during winter, when the infant depends on an exogenous supply of vitamin D, breast milk does not provide the necessary amount of vitamin D. Vitamin D supplementation of the mother can increase the vitamin D content of breast milk but only to a modest degree. In the study by Ala-Houhala et al,9 maternal supplementation with 1000 IU per day in February increased vitamin D content of breast milk from 14 to 33 IU/L and in September from 89 to 124 IU/L. Intake of 2000 IU per day had a similarly modest effect.
Marked seasonal variation of vitamin D status has been observed in breastfed infants at locations with a latitude similar (41°N) to or more northern than Iowa City.8,16,20,21,27-30 Why unsupplemented breastfed infants in Madison, WI,28 had higher mean 25-OHD levels (20.2 + 9.3) than infants in Cincinnati, OH, where 4 of 7 infants at 26 weeks of age had 25-OHD levels <11 ng/mL,20 or infants in Iowa City (present study), remains unknown.
In the present study, infants with dark skin pigmentation were in worse vitamin D status than infants with light skin pigmentation, similar to what Specker et al2 reported. Although the mechanism is mainly decreased production of vitamin D in the infant's pigmented skin, lower vitamin D content of breast milk of black women is well documented2 and was probably also playing a role.
That breast milk cannot be relied on to provide the amounts of vitamin D needed to prevent rickets was at one time well appreciated.6 Supplementation with cod liver oil or other suitable sources of vitamin D was recommended and was widely practiced. When the feeding of formulas, which in the United States have long been fortified with vitamin D, replaced breastfeeding, vitamin D supplements were no longer needed. With the return to breastfeeding beginning in the early 1970s, vitamin D supplementation was not resumed for reasons that are unknown. Beginning in the 1980s, reports began to appear of vitamin D deficiency rickets in breastfed infants. The great majority of cases have involved infants and toddlers with dark skin pigmentation and/or those who consumed strict vegetarian diets (3-5,14,31-40). However, 1 report from Vancouver, British Columbia, Canada, included several subjects with light skin pigmentation who developed rickets.37
Although prevention of rickets is the primary reason why vitamin D supplements should be provided to breastfed infants, it is not the only reason.22 Vitamin D receptors are present in many organs, and vitamin D exerts antiproliferative effects,41 which may explain why it protects against colorectal cancer.42 Also, vitamin D supplementation during infancy may protect against type I diabetes mellitus43-46 and has been shown to lead to higher bone mineral mass in prepubertal girls.47
CONCLUSIONS
We report that vitamin D deficiency is common among normal breastfed infants living in Iowa and is more widespread and more severe than reported previously for the United States. Vitamin D deficiency occurs mainly, but not exclusively, during winter, and occurs in light-skinned infants as well as in dark-skinned infants. Breastfed infants who receive supplemental formula or cow milk or receive vitamin supplements are protected from vitamin D deficiency. Our findings reemphasize the need for all breastfed infants living in temperate climates to receive vitamin D supplements, at least during winter.
