Hay Fever treated by Vitamin D (50,000 IU weekly) – RCT
Therapeutic effect of vitamin D supplementation on allergic rhinitis.
Eur Arch Otorhinolaryngol. 2019 Jul 22. doi: 10.1007/s00405-019-05546-x.
Bakhshaee M1, Sharifian M1, Esmatinia F1, Rasoulian B2, Mohebbi M3.
 * Best supplements for hay fever (Quercetin, which activates the Vitamin D receptor) - June 2019
* Overview Allergies
* Allergic rhinitis in children reduced somewhat during pollen season by just 1,000 IU of vitamin D – RCT Jan 2018
* All items in Breathing and vitamin D ** items *
* Hay fever (Allergic Rhinitis) and Vitamin D - many studies
* One pill every two weeks gives you all the vitamin D most adults need
* Sub section of that page has a summary of weekly 50K Vitamin D, which includes the study on this page
* Best supplements for hay fever (Quercetin, which activates the Vitamin D receptor) - June 2019
* Overview Allergies
* Allergic rhinitis in children reduced somewhat during pollen season by just 1,000 IU of vitamin D – RCT Jan 2018
* All items in Breathing and vitamin D ** items *
* Hay fever (Allergic Rhinitis) and Vitamin D - many studies
* One pill every two weeks gives you all the vitamin D most adults need
* Sub section of that page has a summary of weekly 50K Vitamin D, which includes the study on this page
📄 Download the PDF from Sci-Hub via VitaminDWiki
Grassroots Health chart of the data__
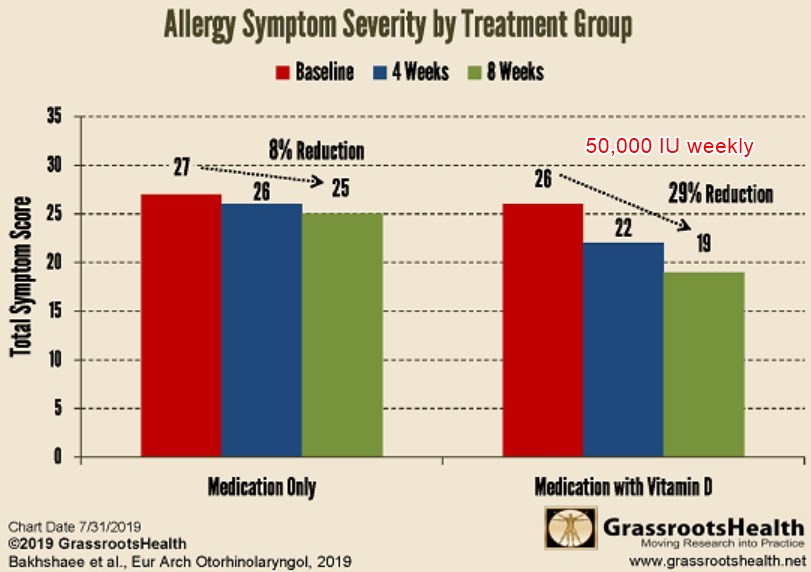
PURPOSE:
In this study, we aimed to determine whether short-term (2 months) vitamin D supplementation could improve the allergic symptoms in AR patients.
METHODS:
A randomized double-blind placebo-controlled clinical trial was performed on allergic rhinitis patients with vitamin D deficiency from Nov. 2017-2018. 80 cases with allergic rhinitis and vitamin D deficiency were divided into two groups and vitamin D plus routine antihistamine medication (cetirizine) was prescribed for the study group, whereas the control group received cetirizine plus placebo. The clinical symptoms questionnaire was completed at baseline and after 4 and 8 weeks of treatment initiation. Vitamin D levels were re-measured at the end of the 8-week treatment course.
RESULTS:
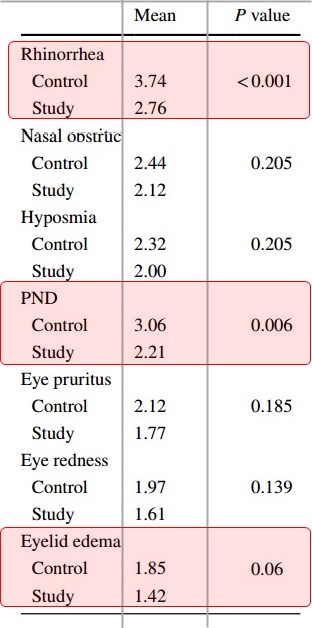
In total, 80 patients with allergic rhinitis and vitamin D deficiency were enrolled. Among them, 35 cases and 33 controls visited the clinic after 8 weeks; the mean age in the aforementioned groups was 29.68 years and 29.13 years demonstrating no meaningful difference (P > 0.05). At study initiation, the mean vitamin D level was 14 ng/ml and 14.67 ng/ml in the study and control groups, respectively, indicating no significant difference (P = 0.189). The mean serum vitamin D level at 8 weeks of treatment in the study group (24.08 ng/ml) indicated a statistically meaningful difference with the mean vitamin D level at baseline (P < 0.001). Comparison of the mean scores of symptoms severity showed no significant difference between the two groups at study initiation and 4 weeks later (P = 0.073), whereas a significant difference was obtained between baseline and 8 weeks of treatment initiation (P = 0.007).
CONCLUSION:
Based on the findings of the present study, it can be concluded that vitamin D supplementation along with antihistamines can result in relative symptoms improvement in AR patients with vitamin D deficiency.
