Rational approach to COVID-19: 50k-100k of Vitamin D weekly
Vitamin D supplementation as a rational pharmacological approach in the COVID-19 pandemic
Am J Physiol Lung Cell Mol Physiol 319: L941-L948, 2020.
First published September 30,2020; doi:10.1152/ajplung.00186.2020.
Le6n Ferder,1 Virna Margarita Martin Gim nez,2 Felipe Inserra,1 Carlos Tajer,3 Laura Antonietti,3 4 Javier Mariani,3 and ©Walter Manucha56
1Maimonides University, Buenos Aires, Argentina; 2Institute of Research in Chemical Sciences, School of Chemical and Technological Sciences, Cuyo Catholic University, San Juan, Argentina; Department of Cardiology, Hospital El Cruce Nestor C. Kirchner, Buenos Aires, Argentina; 4Arturo Jauretche National University, Buenos Aires, Argentina; 5Pathology Department, Pharmacology Area, Medical Sciences College, National University of Cuyo, Mendoza, Argentina; and National Scientific and Technical Research Council, Institute of Medical and Experimental Biology of Cuyo (IMBECU, CONICET), Mendoza, Argentina

📄 Download the PDF from VitaminDWiki
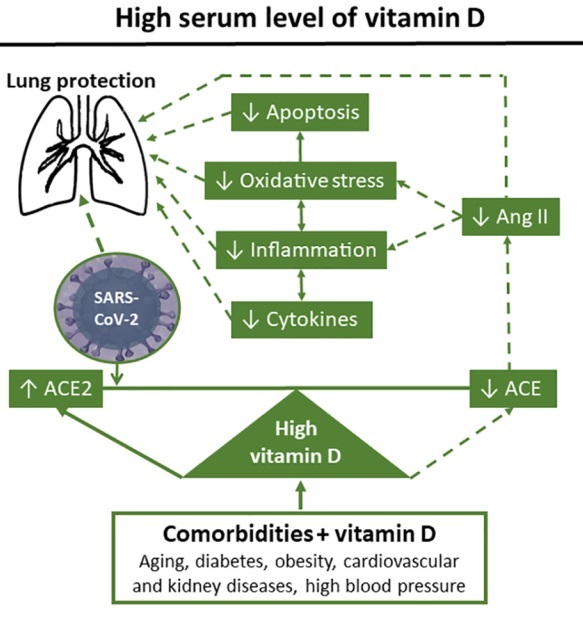
Solid lines = stimulation/induction, dashed lines = inhibition/blocking
The COVID-19 pandemic has reached most of the countries worldwide causing death, which often results from an inflammatory storm associated with severe acute respiratory syndrome (SARS). This has prompted researchers to seek specific novel and definitive treatments urgently. In this context, it is interesting to evaluate the preventive and therapeutic effects of existing pharmacological agents that could be useful. In this regard, vitamin D supplementation, particularly in individuals likely to be deficient, may be a promising option. Vitamin D is a hormone that modulates many of the same inflammatory and oxidative signaling pathways triggered during COVID-19. For example, vitamin D suppresses the actions of the renin-angiotensin system, which has a determining role in the pathophysiology of the inflammatory response related to COVID-19. This paper analyzes the evidence that vitamin D supplementation might be a valuable preventive/therapeutic measure in groups at risk for or infected with COVID-19. It also discusses how clinical studies could be best designed to evaluate the possible advantages of vitamin D supplementation for the benefit of public health during the pandemic.
INTRODUCTION
At present, multiple therapeutic strategies are being frantically sought to address the COVID-19 crisis. Among the most prominent approaches are the development of vaccines, antiretroviral drugs, corticosteroids, and immunomodulatory drugs. Due to the urgency of the epidemic outbreak and the lack of sufficient experience with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), some empirical treatments for COVID-19 are also proposed on a rational basis. More specifically, randomized controlled trials (RCTs) are lacking that support the benefit of vitamin D supplementation in the population and/or patients exposed to SARS-CoV-2. However, an ever-growing number of findings are strengthening and validating such a claim.
The system that integrates vitamin D has an ancestral origin that involves it with a primordial defense system. Vitamin D receptors (VDRs) were present in very primitive organisms that lacked skin, bones, cardiovascular systems, kidneys, and even lungs (20), indicating that the purpose must have been other than that conventionally known for vitamin D. More recently, VDRs were described in the cytoplasm, nuclear membrane, and even organelles such as mitochondria (21, 58). The genomic and nongenomic effects of vitamin D are ultimately the result of hormone-receptor binding that, after translocating to the nucleus, modulates the expression of genes involved in phos- phocalcium metabolism (36, 45). At the same time, a considerable number of “nonclassical” vitamin D actions have been described, including the inhibition of cell proliferation, secretion of other hormones, suppression of T-cell proliferation, and modulation of cytokines (14). Thus, vitamin D and its metabolites have been shown to participate actively in the regulation of innate and adaptive immune responses. Consequently, its deficiency is associated with a series of infections as well as autoimmune and allergic conditions (67). These data reinforce the original notion that the VDR-metabolite system would fulfill a central role in cellular and tissue defense through immune mechanisms and/or regulation of inflammatory processes. Furthermore, vitamin D would regulate the expression of 0.5-5% of the total human genome, which amounts to 〜100-1,250 genes. Therefore, it is not surprising that vitamin D interacts with multiple genes commonly expressed in humans, such as those related to the renin-angiotensin-aldosterone system (RAAS), among others (28).
LINK BETWEEN VITAMIN D/RAAS AND COVID-19
Apart from the immune system, evolution enabled vitamin D to interact with other fundamental systems in the maintenance of cellular homeostasis, such as the RAAS. As described in Fig. 1 (20), vitamin D opposes or modulates RAAS signaling pathways. The RAAS regulates body hydroelectrolyte composition and hemodynamics. Of central interest for the present perspective, it also functions as a complex proinflammatory system (20). Consequently, most mammalian cells express both VDR and different RAAS receptors. Vitamin D, its metabolites, and receptors, on the one hand, and RAAS molecules and its receptors, on the other hand, are part of a delicate cellular/tissue defense system mediating pro- and anti-inflammatory processes.
Additionally, there are some close connections between COVID-19 and the RAAS, since serum angiotensin II (Ang II) levels in infected patients were significantly elevated and directly proportional to the viral load and lung damage observed (35). SARS-CoV-2 has been shown to bind to angiotensin-converting enzyme 2 (ACE2) receptors to invade human lung epithelial cells and initiate the infection. At the same time, ACE2 produces anti-inflammatory, antioxidant, antifibrotic, and antihyperplasia effects. This leads to the degradation of Ang II at the lung level through the ACE2/Ang (1-7)/Mas receptor signaling pathway, i.e., the counterregulatory RAAS axis with opposite actions to the classical RAAS axis (ACE/Ang II/AT1 receptor pathway). The increase in the degradation of Ang II prevents its toxic overaccumulation, which would cause the acute respiratory distress syndrome often present in COVID-19 (13, 18, 59, 69). Independently ofCOVID-19, the RAAS is also involved in the regulation of lung tissue proliferation, inflammation, and fibrosis in several pulmonary pathologies, such as acute lung injury, asthma, pulmonary arterial hypertension, chronic obstructive pulmonary disease, and idiopathic pulmonary fibrosis, among others (62).
Concerning vitamin D/RAAS interaction, the participation of the ACE2/Ang (1-7)/MasR signaling pathway has been recently demonstrated in hypertensive rats (17). In humans, vitamin D was found to act as a cofactor in the attenuation of incident atrial fibrillation by RAAS inhibition (68). Additionally, exacerbated RAAS activation at the hepatic level causes liver dysfunction and increases the risk of developing diabetes mellitus. In this regard, calcitriol was shown to modulate the altered upregula- tion of liver RAAS under conditions of insulin resistance in mice (33). Vitamin D is a potent suppressor of renin production (Fig. 1) (20). Thus, low plasma levels of vitamin D are associated with an increase in renin synthesis, which results in overactivation of RAAS and increased production of Ang II, and vice versa (34, 55). It has been demonstrated that vitamin D deficiency also results in overexpression of angiotensin-converting enzymes (ACE and ACE2) (73). Furthermore, in patients with hypovitaminosis D, the reestablishment of normal vitamin D levels causes a blockade of peripheral RAAS (9).
In vitamin D receptor-null mice, the development of induced acute lung injury was found to be more severe than in wild-type mice, together with increased levels of pulmonary Ang II and renin. Pretreatment of vitamin D receptor-null mice with losar- tan reduced the severity of pulmonary injury, indicating that vitamin D, via its receptors, attenuates acute lung injury by blocking RAAS (30). Additionally, Xu et al. (73) showed that calcitriol inhibits ACE and induces ACE2 expression in rat lung while reducing Ang II levels and inhibiting AT1R expression. The authors suggest that VDR activation may exert protective effects on LPS-induced lung injury by regulating the balance between RAAS members. Moreover, if vitamin D deficiency is chronic, the uncontrolled RAAS overactivation for extended periods may induce pulmonary fibrosis through the exacerbated and accelerated increase in extracellular matrix deposition in lung tissues (56).
Lung epithelial cells exhibit a high expression of the enzyme 1-a-hydroxylase, allowing for the local synthesis of 1,25-dihy- droxyvitamin D——the most active form of vitamin D——also called calcitriol. Calcitriol inhibits the production and secretion of many cytokines from bronchial smooth muscle cells, such as platelet-derived growth factor, RANTES (regulator in the activation of expressed and secreted normal T-cells), and matrix metalloproteinases, leading to reduced proliferation and inflammation in lung smooth muscle cells. Vitamin D stimulates the synthesis of interleukin 10 by CD4+, CD25+, Foxp3+, and T- regulatory cells. At the same time, it inhibits the activation of dendritic cells by downregulating the expression of CD80/86 and CD40. Furthermore, vitamin D stimulates the expression of cath- elicidin and many other anti-infective molecules (12, 15, 54).
Supplementation with 1,25-dihydroxyvitamin D suppresses the recruitment of eosinophils and lymphocytes into the airways, decreases IL-4 production of T-cells, and inhibits T-cell migration by attenuating the inflammatory response (66). It also works as an adjuvant for other therapies, such as immunotherapy against allergens (60). Simultaneous administration of vitamin D and dexamethasone in steroid-resistant asthmatic patients increased IL-10 synthesis to levels similar to those found in steroid-sensitive patients treated with dexamethasone alone (74).
In a rat model of asthma, vitamin D treatment significantly reduced serum IgE and eotaxin levels (65). Additionally, it decreased the infiltration of inflammatory cells in the airways, serum levels of IL-6, tumor necrosis factor-alpha (TNFa), and IL-1p, as well as the expression of the apoptotic protein associated with Bcl 2, caspase-3, TLR4, nuclear factor kappa B (NF- kB), and phosphorylated p65 NF-kB. As a result, vitamin D raised serum levels of IL-10, reducing the inflammatory and ap- optotic response in this rat model of asthma (77). Importantly, vitamin D suppressed the synthesis of 8-isoprostane (8-iso), IL- 6, and granulocyte-macrophage colony-stimulating factors in human bronchial epithelial cells exposed to contaminating particles. Vitamin D also increased the expression of genes of the glucose 6-phosphate dehydrogenase (G6PD) antioxidant pathway and the levels of oxidized glutathione. Therefore, vitamin D seems to protect the lungs and airways of asthma patients through its anti-inflammatory and antioxidant effects (46) (Fig. 2).
In the murine model of bleomycin-induced lung inflammation, calcitriol reduced early lung inflammation by attenuating immune cell infiltration, suppressing the secretion of inflammatory cytokines, blocking translocation of NF-kB p65, and inhibiting phosphorylation of lung p38 MAPK and protein kinase B (Akt). It also attenuated the expression of smooth muscle alpha-actin (a marker for epithelial-mesenchymal transition in the lungs, which promotes fibrosis) while decreasing the phosphorylation of intracellular effectors of the TGF-p superfamily proteins (Smad) and the upregulation of transforming growth factor-beta 1 (TGF-p1) (63). In addition, calcitriol caused a 40% reduction in the recruitment of neutrophils to the lungs in an animal model of acute lung injury. The anti-inflammatory effect of vitamin D may be mediated by the inhibition of IL-8 secretion at the lung level (61).
Administration of vitamin D to neonatal rats exhibiting hyperoxia-induced lung injury (as a model of bronchopulmonary dysplasia) attenuated lung injury through various protective actions, such as preserving the integrity of lung structure, decreasing inflammation by negatively regulating TLR4 activation, and reducing extracellular matrix deposition and the inhibition of lung cell apoptosis (75). Vitamin D was also shown to have immunomodulatory and anti-inflammatory effects in the treatment of cystic fibrosis of the airways, as it reduces the expression of CD279 (PD-1) in CD4+ and CD8+ T-cells. Furthermore, vitamin D decreases the frequency of CD8+ T- cells and invariant mucosa-associated T-cells that coexpress activation markers for CD38 and D antigen in human leukocytes. Therefore, vitamin D treatment would prevent the progression of lung damage associated with cystic fibrosis of the airways (49) (Fig. 2).
VITAMIN D LUNG PROTECTION: A RATIONAL APPROACH TO COVID-19
Oxidative stress caused by tobacco smoke is known to worsen the progression of chronic obstructive pulmonary disease (COPD). In this sense, vitamin D has also been proposed as a natural anti-inflammatory and antioxidant capable of improving the prognosis of this pulmonary pathology in smokers (6).
Patients with COPD were shown to have lower plasma vitamin D levels than healthy patients, suggesting a possible correlation between weak antioxidant defense and the development of this lung disease (1). In this respect, a few years ago, our group raised the discussion about a worldwide pandemic of vitamin D deficiency as a possible explanation for the high cellular inflammatory activity induced by the RAAS (20). The original discussion involved a significant number of pathologies, mainly cardiovascular, although all of them with a similar inflammatory basis. Currently, with the main focus on acute lung inflammation caused by COVID-19, the Irish Longitudinal Study on Aging (TILDA 2020) reinforces the idea that adequate vitamin D supplementation, especially in older people, may be beneficial for the vulnerable population during the COVID-19 outbreak (31).
In summary, the anti-inflammatory, antioxidant, and antiviral properties of vitamin D, in addition to its ability to modulate the RAAS, make it an attractive strategy for preventing COVID-19 and its associated organic damage (5) (Fig. 2).
PROMISING RESULTS ACCORDING TO VITAMIN D LEVELS AND SUPPLEMENTATION
An increasing number of papers, including systematic reviews and meta-analyses, confirm the link between a higher incidence of severe COVID-19, including death, and low serum levels of vitamin D. Remarkably, serum vitamin D concentration was inversely associated with the risk and severity of acute respiratory tract infection (47). A fundamental analysis of the link between vitamin D deficiency and its treatment, associated with the incidence of COVID-19, was performed by Meltzer and colleagues (40) using data from the electronic health record at the University of Chicago Medicine. The main result of this analysis is the comparison of patients with a low measured basal level of vitamin D and no supplementation treatment versus patients with a low basal level of vitamin D but supplemented with this vitamin. The nonsupplemented group showed a significantly higher number of positive tests for COVID-19. Among the treated patients, the vitamin D protective effect against the SAR-CoV-2 virus infection was significant only in the group with basal vitamin D deficiency (40).
Additionally, there is robust information showing that as vitamin D levels increase, the number and severity of respiratory infections decrease (70, 76). Several studies that evaluated the role of vitamin D in respiratory viral infections, using different methodologies and dosages and comparing vitamin D supplementation versus placebo, have mostly found a positive effect for vitamin D (4, 26). Although the mechanisms are not fully understood, the combined improvements in the immunomodulatory and anti-inflammatory response, together with the proven germicidal effects of vitamin D, take part in its protective effects. This background provides the medical community with enough support to investigate whether vitamin D effects are also beneficial in the context of COVID-19.
Different strategies are available to increase vitamin D levels: food fortification programs, increasing sun exposure by stimulating outdoor activities, and vitamin D supplementation, among others. Both vitamin D food fortification and sun exposure are useful to improve low serum levels of vitamin D. It is evident that this strategy enhances human defense against viral and bacterial infections. Vitamin D food fortification represents both a feasible and a recommended measure, whose implementation as a health policy was suggested in a recent review, taking as a guide the program used in Finland. The related legislation, however, must be generated by each of the interested countries (48). Both historical and recent evidence on the mechanisms of sun- dependent vitamin D production and its protective effects were reviewed by Wacker and Holick (71). It is worth noting that the cutaneous production of vitamin D depends on many variables. The lower rates of skin vitamin D production occur among individuals with darker skin or reduced sun exposure, subjects living in higher latitudes in winter, nursing home residents, or elderly people. Accordingly, COVID-19 is more prevalent among African Americans, individuals living in northern cities in late winter, and older individuals, all of whom have an increased risk of vitamin D deficiency (39). As shown in a recent systematic review and meta-analysis (42), vitamin D supplementation is superior to sunbathing at elevating vitamin D serum levels. However, increasing sun exposure or improving the general health condition of the population at high risk of vitamin D deficiency described earlier is not easy to achieve. This explains the key role of vitamin D supplementation. Notwithstanding this, a balanced and healthy diet that includes foods with high vitamin D content and an exercise routine, preferably outdoors, aimed at reducing or at least maintaining body weight and improving aerobic capacity are essential preventive strategies to enhance the defenses against SARS-CoV-2 (41).
Recently, Grant and colleagues (24) suggested that vitamin D supplementation could reduce the risk of influenza and COVID-19 infections. This conclusion is in line with the existence of abundant data in support of the protective action of vitamin D in multiple inflammatory and oxidative pulmonary diseases, such as those caused by SARS-CoV-2. Grant et al. showed that the degree of protection against influenza and COVID-19 increases as vitamin D levels increase. However, the results have not allowed establishing an adequate cutoff point level yet. Nonetheless, an observational study reported that 38 ng vitamin D/mL is an appropriate serum value to decrease the risk of acute viral respiratory infections (53). Additionally, some authors suggest maintaining a serum vitamin D level of at least 30 ng/mL or even within a range of between 40 and 60 ng/mL to reduce infectious processes. Thus, it has been reported that postsurgical hospital infections are three times higher when vitamin D values are lower than 30 ng/mL (51) and that these types of infections were reduced by 33% for every 10 ng/mL of increase in serum vitamin D (32) levels.
Following medical evidence, frequent clinical behavior suggests that in the face of severe vitamin D deficiency, a two-stage therapeutic scheme should be established. The first stage consists of a high loading dose followed by a lower maintenance dose. In this regard, the use of the so-called “loading dose” of vitamin D has been reported to achieve a target plasma level of 30 ng/mL vitamin D by using different dosage regimens (daily, weekly, biweekly, and monthly). Remarkably, in patients with elevated inflammatory markers——such as obese subjects——the necessary supplementation should be two- to threefold higher than that established for the general population. In the case of overweight patients, such supplementation should be at least 1.5 times higher than the general population (19).
Even though knowledge about the role of vitamin D is still scarce, pooled data support its role as an adjuvant strategy aimed at providing rapid and effective protection against the risk of infection by SARS-CoV-2. In this scenario, different approaches have been tried, such as daily vitamin D doses for a short time or the use of an initial loading dose followed by high vitamin D doses for a short time. In each case, and in times of a pandemic, this allows achieving plasma concentrations within appropriate ranges of 30-50 ng/mL or higher. More specifically, strategies such as that suggested by Grant et al. (23) propose a dose of 10,000 IU/day for a month to quickly reach the goal of 40-60 ng vitamin D/mL, followed by 5,000 IU/day for a few more weeks.
The proposed level of high vitamin D doses is striking, neglecting its possible toxic effects; however, in this respect, some studies show that a dose of 10,000 IU/day for 4-6 mo has no adverse effects. Amir et al. (2) verified no toxic effects in Canadian women with breast cancer and bone metastases. Similarly, the research team led by Dr. Holickone of the most prominent groups in vitamin D studies——supplemented cancer patients with high doses of vitamin D, finding no toxicity; on the contrary, it improved the intestinal microbiota of treated patients (11). The same group worked with 10,000 IU/day for 6 mo without causing hypercalcemia and achieving vitamin D levels of the order of 78.6±13 ng/mL (57). Another study treated psychiatric patients with doses of 5,000 or 50,000 IU/ day for 16 mo without adverse effects. The only caveat was that if a patient also received calcium supplementation, the dose should not be high to minimize the risk of hypercalcemia (38). The bet was higher in other studies with proposals for an initial dose of 100,000 IU to achieve serum concentrations above 20 ng/mL, an initial dose of 300,000 IU for levels above 30 ng/mL, and even an initial dose of 500,000 IU for healthy adults (16, 29). In another clinical trial, a monthly dose of 100,000 IU increased neither the incidence rate of kidney stone events nor the incidence rate of hypercalcemia (37).
Current information is controversial regarding what should be the supplemental dose of vitamin D to be administered to patients. Age, diet, weight, sun exposure, and concomitant diseases may have clinical relevance because they may change the requirements and production capacity. Consider the dose of vitamin D needed to attain its bone action; the maximum dose suggested for this purpose is 4,000 IU daily .
Nevertheless, the optimal serum level needed to protect our body against infections remains unclear. In this sense, serum levels of 50-60 ng vitamin D/mL seem to be adequate. With 11,000 IU vitamin D/ day, it takes about 4 wk to achieve the above serum levels, and with 4,000 IU vitamin D/day, it takes over 12 wk.
[Comment by VitaminDWiki Those are average responses - need larger daily doses for 97% of people]
The proposed higher dose is not associated with an increased risk of toxicity. In a recently published consensus, it was suggested that doses ranging from 4,000 IU (for bone action) to 10,000 IU (for noncalcemic effects) are safe and effective to achieve the advantageous effects of vitamin D (22, 23, 27). However, additional studies are required to confirm what is the best protection threshold against COVID-19 or to treat recently infected patients (10).
Based on scarce information comparing a high single dose versus daily doses of vitamin D, some authors have expressed concern about data that show better results with daily doses of vitamin D. However, it is interesting to note that the end point evaluated in this randomized study was not infectious diseases (3). Additionally, in a recent publication of a randomized trial, 120 children with a confirmed diagnosis of sepsis were assigned to receive either a single dose of 150,000 IU of vitamin D3 or a placebo. Cardiovascular sequential organ failure assessment (SOFA) score and the percentage of children with septic shock were lower in the vitamin D group (72).
Finally, latest reports have proposed that vitamin D supplementation could improve the clinical course of patients infected with SARS-CoV-2 (8, 43). The same recommendation was reinforced by Grant and colleagues (24), who suggested that vitamin D supplementation could reduce the risk of COVID-19.
CONCLUSIONS AND PROSPECTS
To sum up, and in the face of this devastating epidemic for which we still lack effective treatments, the present perspective proposes to explore the potentially protective effect of high doses of vitamin D to increase blood and tissue levels rapidly. This approach intends to counteract RAAS overload, thus improving the course of COVID-19 and its respiratory complications, even protecting other organs. The purpose is to open the discussion and create an appropriate debate on the prospect of prescribing vitamin D to the general population—particularly the most vulnerable—as well as achieving a serum and tissue vitamin D level to counteract the imbalance of the RAAS and manifest its anti-inflammatory effects.
We believe that this strategy applied at the population level could provide an additional tool for the defense against the SARS-CoV-2 virus without adverse effects, as demonstrated in the review of more than 76,000 patients included in controlled trials with vitamin D supplementation.
A possible dose to obtain rapid increases in plasma vitamin D levels could range between 5,000 IU and/or 10,000 IU daily or 50,000 IU to 100,000 IU weekly (7). Given the tentativeness of the proposed dose, the use of lower doses could be considered in children or young adults with low exposure risk to the virus. In this regard, our working group is advancing in the development of controlled protocols with different populations of people at risk or already infected, evaluating physiological parameters and clinical events. Even though the said intervention does not intend to eliminate the virus, its potential is promising to hinder viral entry and/or improve patient evolution. That is, vitamin D intake could improve the health of the patients so that they can be in a better shape to face COVID-19 and boost their defenses against this infection or even against other equivalent diseases. Furthermore, it should be borne in mind that quarantine, as a protection strategy for the population against infection, complicates the defense mechanisms due to a significant decline in serum vitamin D levels by reduced sun exposure.
As previously described, we consider that the present recommendation finds support in multiple reports. Accordingly, Grant and colleagues (25) recently proposed to raise serum vitamin D concentrations through supplementation, claiming that this strategy could reduce the incidence, severity, and risk of death from influenza, pneumonia, and the current COVID-19 epidemic. Additionally, Panarese and Shahini (44) proposed the prophylactic use of usual vitamin D doses to mitigate the aggressive progression of the disease in Europe. In turn, Rhodes and collaborators (52) have proposed vitamin D supplementation, at least for people in the northern hemisphere who are at higher risk of severe illness and death. The same is recommended by the United Kingdom Association of Dietitians (64).
Finally, 10 RCTs around the world (50), including one by our group (No. NCT04411446), are currently investigating whether supplementation with vitamin D could be an effective strategy against viral complications. Such trials aim to validate this hypothesis for the benefit of public health, particularly in the context of the COVID-19 crisis.
REFERENCES
Al-Azzawi MA, Ghoneim AH, Elmadbouh I. Evaluation of vitamin D, vitamin D binding protein gene polymorphism with oxidant - antioxidant profiles in chronic obstructive pulmonary disease. J Med Biochem 36: 331340,2017. doi:10.1515/jomb-2017-0012.
Amir E, Simmons CE, Freedman OC, Dranitsaris G, Cole DE, Vieth R, Ooi WS, Clemons M. A phase 2 trial exploring the effects of high-dose (10,000 IU/day) vitamin D(3) in breast cancer patients with bone metasta- ses. Cancer 116: 284-291,2010. doi:10.1002/cncr.24749.
Apaydin M, Can AG, Kizilgul M, Beysel S, Kan S, Caliskan M, Demirci T, Ozcelik O, Ozbek M, Cakal E. The effects of single high-dose or daily low-dosage oral colecalciferol treatment on vitamin D levels and muscle strength in postmenopausal women. BMC Endocr Disord 18: 48, 2018. doi:10.1186/s12902-018-0277-8.
Arihiro S, Nakashima A, Matsuoka M, Suto S, Uchiyama K, Kato T, Mitobe J, Komoike N, Itagaki M, Miyakawa Y, Koido S, Hokari A,
Saruta M, Tajiri H, Matsuura T, Urashima M. Randomized trial of vitamin D supplementation to prevent seasonal influenza and upper respiratory infection in patients with inflammatory bowel disease. Inflamm Bowel Dis 25: 1088-1095,2019. doi:10.1093/ibd/izy346.
Aygun H. Vitamin D can prevent COVID-19 infection-induced multiple organ damage. Naunyn Schmiedebergs Arch Pharmacol 393: 1157-1160, 2020. doi:10.1007/s00210-020-01911-4.
Biswas S, Hwang JW, Kirkham PA, Rahman I. Pharmacological and dietary antioxidant therapies for chronic obstructive pulmonary disease. Curr MedChem 20: 1496-1530,2013.doi:10.2174/0929867311320120004.
Bolland MJ, Grey A, Gamble GD, Reid IR. The effect of vitamin D supplementation on skeletal, vascular, or cancer outcomes: a trial sequential meta-analysis. Lancet Diabetes Endocrinol 2: 307-320, 2014. doi:10.1016/ S2213-8587(13)70212-2.
Carpagnano GE, Di Lecce V, Quaranta VN, Zito A, Buonamico E, Capozza E, Palumbo A, Di Gioia G, Valerio VN, Resta O. Vitamin D deficiency as a predictor of poor prognosis in patients with acute respiratory failure due to COVID-19. JEndocrinol Invest In press. doi:10.1007/s40618- 020-01370-x.
Carrara D, Bruno RM, Bacca A, Taddei S, Duranti E, Ghiadoni L, Bernini G. Cholecalciferol treatment downregulates renin-angiotensin system and improves endothelial function in essential hypertensive patients with hypovitaminosis D. J Hypertens 34: 2199-2205, 2016. doi:10.1097/ HJH.0000000000001072.
- Chakhtoura M, Napoli N, El Hajj Fuleihan G. Commentary: myths and facts on vitamin D amidst the COVID-19 pandemic. Metabolism 109: 154276,2020. doi:10.1016/j.metabol.2020.154276.
Charoenngam N, Shirvani A, Kalajian TA, Song A, Holick MF. The effect of various doses of oral vitamin D3 supplementation on gut microbiota in healthy adults: a randomized, double-blinded, dose-response study. AnticancerRes 40: 551-556,2020. doi:10.21873/anticanres.13984.
Chen WW, Cai XX, Tian WM, Shang YX. Expression ofRANTES in the lung tissue of asthmatic rats, and the intervention effect of vitamin D on RANTES expression. Zhongguo Dang Dai Er Ke Za Zhi 14: 863-868, 2012.
Cheng H, Wang Y, Wang GQ. Organ-protective effect of angiotensin-converting enzyme 2 and its effect on the prognosis of COVID-19. J Med Virol 92: 726-730,2020. doi:10.1002/jmv.25785.
Christakos S, Raval-Pandya M, Wernyj RP, Yang W. Genomic mechanisms involved in the pleiotropic actions of 1,25-dihydroxyvitamin D3. BiochemJ 316: 361-371,1996. doi:10.1042/bj3160361.
Chung C, Silwal P, Kim I, Modlin RL, Jo EK. Vitamin D-cathelicidin axis: at the crossroads between protective immunity and pathological inflammation during infection. Immune Netw 20: e12, 2020. doi:10.4110/ in.2020.20.e12.
Cipriani C, Romagnoli E, Scillitani A, Chiodini I, Clerico R, Carnevale V, Mascia ML, Battista C, Viti R, Pileri M, Eller-Vainicher C, Minisola S. Effect of a single oral dose of 600,000 IU of cholecalciferol on serum cal- ciotropic hormones in young subjects with vitamin D deficiency: a prospective intervention study. J Clin Endocrinol Metab 95: 4771-4777, 2010. doi:10.1210/jc.2010-0502.
Cui C, Xu P, Li G, Qiao Y, Han W, Geng C, Liao D, Yang M, Chen D, Jiang P. Vitamin D receptor activation regulates microglia polarization and oxidative stress in spontaneously hypertensive rats and angiotensin II- exposed microglial cells: role of renin-angiotensin system. Redox Biol 26: 101295, 2019. doi:10.1016/j.redox.2019.101295.
Danser AHJ, Epstein M, Batlle D. Renin-angiotensin system blockers and the COVID-19 pandemic: at present there is no evidence to abandon renin-angiotensin system blockers. Hypertension 75: 1382-1385, 2020. doi:10.1161/HYPERTENS IONAHA. 120.15082.
Ekwaru JP, Zwicker JD, Holick MF, Giovannucci E, Veugelers PJ. The importance of body weight for the dose response relationship of oral vitamin D supplementation and serum 25-hydroxyvitamin D in healthy volunteers. PLoS One 9: e111265, 2014. doi:10.1371/journal.pone.0111265.
Ferder M, Inserra F, Manucha W, Ferder L. The world pandemic of vitamin D deficiency could possibly be explained by cellular inflammatory response activity induced by the renin-angiotensin system. Am J Physiol CellPhysiol 304: C1027-C1039, 2013. doi:10.1152/ajpcell.00403.2011.
Garcia IM, Altamirano L, Mazzei L, FornesM, MolinaMN, FerderL, Manucha W. Role of mitochondria in paricalcitol-mediated cytoprotection during obstructive nephropathy. Am J Physiol Renal Physiol 302: F1595- F1605, 2012. doi:10.1152/ajprenal.00617.2011.
Giustina A, Adler RA, Binkley N, Bollerslev J, Bouillon R, Dawson- Hughes B, Ebeling PR, Feldman D, Formenti AM, Lazaretti-Castro M, Marcocci C, Rizzoli R, Sempos CT, Bilezikian JP. Consensus statement from 2nd International Conference on Controversies in Vitamin D. Rev Endocr MetabDisord 21: 89-116, 2020. doi:10.1007/s11154-019-09532-w.
Grant WB, Baggerly CA, Lahore H. Reply: “Vitamin D supplementation in influenza and COVID-19 infections. Comment on: Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths Nutrients 2020, 12(4), 988”. Nutrients 12: 1620, 2020. doi:10.3390/nu12061620.
Grant WB, Lahore H, McDonnell SL, Baggerly CA, French CB, Aliano JL, Bhattoa HP. Evidence that vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths. Nutrients 12: E988, 2020. doi:10.3390/nu12040988.
Grant WB, Lahore H, McDonnell SL, Baggerly CA, French CB, Aliano JL, Bhattoa HP. Vitamin D supplementation could prevent and treat influenza, coronavirus, and pneumonia infections (preprint). Preprints 2020030235: 2020. doi:10.20944/preprints202003.0235.v1.
Gruber-Bzura BM. Vitamin D and influenza—Prevention or therapy? Int J MolSci 19: 2419, 2018. doi:10.3390/ijms19082419.
Heaney RP, Davies KM, Chen TC, Holick MF, Barger-Lux MJ. Human serum 25-hydroxycholecalciferol response to extended oral dosing with cholecalciferol. Am J Clin Nutr 77: 204-210, 2003. doi:10.1093/ajcn/ 77.1.204.
Hossein-nezhad A, Spira A, Holick MF. Influence of vitamin D status and vitamin D3 supplementation on genome wide expression of white blood cells: a randomized double-blind clinical trial. PLoS One 8: e58725, 2013. doi:10.1371/journal.pone.0058725.
Kearns MD, Alvarez JA, Tangpricha V. Large, single-dose, oral vitamin D supplementation in adult populations: a systematic review. Endocr Pract 20: 341-351, 2014. doi:10.4158/EP13265.RA.
Kong J, Zhu X, Shi Y, Liu T, Chen Y, Bhan I, Zhao Q, Thadhani R, Li YC. VDR attenuates acute lung injury by blocking Ang-2-Tie-2 pathway and renin-angiotensin system. Mol Endocrinol 27: 2116-2125, 2013. doi:10.1210/me.2013-1146.
Laird E, Kenny RA. Vitamin D Deficiency in Ireland - Implications for COVID-19. Results from the Irish Longitudinal Study on Ageing. Dublin: The Irish Longitudinal Study on Ageing (TILDA), 2020, doi:10.38018/ TildaRe.2020-05.
Laviano E, Sanchez Rubio M, Gonzaiez-Nicoliis MT, Palacian MP, Lopez J, Gilaberte Y, Calmarza P, Rezusta A, Serrablo A. Association between preoperative levels of 25-hydroxyvitamin D and hospital-acquired infections after hepatobiliary surgery: a prospective study in a third-level hospital. PLoS One 15: e0230336,2020. doi:10.1371/journal.pone.0230336.
Leung PS. The modulatory action of vitamin D on the renin-angiotensin system and the determination of hepatic insulin resistance. Molecules 24: 2479, 2019. doi:10.3390/molecules24132479.
Li YC, Qiao G, Uskokovic M, Xiang W, Zheng W, Kong J. Vitamin D: a negative endocrine regulator of the renin-angiotensin system and blood pressure. J Steroid Biochem Mol Biol 89-90: 387-392, 2004. doi:10.1016/j. jsbmb.2004.03.004.
Liu Y, Yang Y, Zhang C, Huang F, Wang F, Yuan J, Wang Z, Li J, Li J, Feng C, Zhang Z, Wang L, Peng L, Chen L, Qin Y, Zhao D, Tan S, Yin L, Xu J, Zhou C, Jiang C, Liu L. Clinical and biochemical indexes from 2019-nCoV infected patients linked to viral loads and lung injury. Sci ChinaLife Sci 63: 36374,2020. doi:10.1007/s11427-020-1643-8.
Macoova L, Bicoikova M, Hampl R. Impaired vitamin D sensitivity. Physiol Res 67, Suppl 3: S391-S400,2018. doi:10.33549/physiolres.934006.
Malihi Z, Lawes CmM, Wu Z, Huang Y, Waayer D, Toop L, Khaw KT, Camargo CAJr, Scragg R. Monthly high-dose vitamin D supplementation does not increase kidney stone risk or serum calcium: results from a randomized controlled trial. Am J Clin Nutr 109: 1578-1587, 2019. doi:10.1093/ajcn/nqy378.
McCullough PJ, Lehrer DS, Amend J. Daily oral dosing of vitamin D3 using 5000 TO 50,000 international units a day in long-term hospitalized patients: insights from a seven year experience. J Steroid Biochem Mol Biol 189: 228-239,2019. doi:10.1016/j.jsbmb.2018.12.010.
Meftahi GH, Jangravi Z, Sahraei H, Bahari Z. The possible pathophysiology mechanism of cytokine storm in elderly adults with COVID-19 infection: the contribution of “inflame-aging”. Inflamm Res 69: 825-839, 2020. doi:10.1007/s00011-020-01372-8.
Meltzer DO, Best TJ, Zhang H, Vokes T, Arora V, Solway J. Association of vitamin D deficiency and treatment with COVID-19 incidence (preprint). medRxiv 2020: 05.08.20095893, 2020. doi:10.1101/ 2020.05.08.20095893.
Mohamed AA, Alawna M. Role of increasing the aerobic capacity on improving the function of immune and respiratory systems in patients with coronavirus (COVID-19): a review. Diabetes Metab Syndr 14: 489^96, 2020. doi:10.1016/j.dsx.2020.04.038.
Moradi S, Shahdadian F, Mohammadi H, Rouhani MH. A comparison of the effect of supplementation and sunlight exposure on serum vitamin D and parathyroid hormone: a systematic review and meta-analysis. Crit Rev FoodSciNutr 60: 1881-1889, 2020. doi:10.1080/10408398.2019.1611538.
Panagiotou G, Tee SA, Ihsan Y, Athar W, Marchitelli G, Kelly D, Boot CS, Stock N, Macfarlane J, Martineau AR, Burns G, Quinton R. Low serum 25-hydroxyvitamin D (25[OH]D) levels in patients hospitalized with COVID-19 are associated with greater disease severity. Clin Endocrinol (Oxf) 93: 508-511, 2020. doi:10.1111/cen.14276.
Panarese A, Shahini E. Letter: Covid-19, and vitamin D. Aliment Pharmacol Ther 51: 993-995,2020. doi:10.1111/apt.15752.
Perret C, Colnot S, Romagnolo B, Thomasset M. Control of nuclear transcription of vitamin D-dependent genes by vitamin D. Curr Opin Nephrol Hypertens 6:31 320,1997. doi:10.1097/00041552-199707000-00003.
Pfeffer PE, Lu H, Mann EH, Chen YH, Ho TR, Cousins DJ, Corrigan C, Kelly FJ, Mudway IS, Hawrylowicz CM. Effects of vitamin D on inflammatory and oxidative stress responses of human bronchial epithelial cells exposed to particulate matter. PLoS One 13: e0200040, 2018. doi:10.1371/journal.pone.0200040.
Pham H, Rahman A, Majidi A, Waterhouse M, Neale RE. Acute respiratory tract infection and 25-hydroxyvitamin D concentration: a systematic review and meta-analysis. Int J Environ Res Public Health 16: 3020, 2019. doi:10.3390/ijerph16173020.
Pilz S, Marz W, Cashman KD, Kiely ME, Whiting SJ, Holick MF, et al. Rationale and plan for vitamin D food fortification: a review and guidance paper. Front Endocrinol (Lausanne) 9: 373, 2018. doi:10.3389/ fendo.2018.00373.
Pincikova T, Paquin-Proulx D, Sandberg JK, Flodstrom-Tullberg M, Hjelte L. Vitamin D treatment modulates immune activation in cystic fibrosis. ClinExplmmunol 189: 359-371,2017. doi:10.1111/cei.12984.
Quesada-Gomez JM, Entrenas-Castillo M, Bouillon R. Vitamin D receptor stimulation to reduce acute respiratory distress syndrome (ARDS) in patients with coronavirus SARS-CoV-2 infections. J Steroid Biochem Mol Biol 202: 105719, 2020. doi:10.1016/j.jsbmb.2020.105719.
Quraishi SA, Bittner EA, Blum L, Hutter MM, Camargo CA Jr. Association between preoperative 25-hydroxyvitamin D level and hospital- acquired infections following Roux-en-Y gastric bypass surgery. JAMA Surg 149: 112-118,2014. doi:10.1001/jamasurg.2013.3176.
Rhodes JM, Subramanian S, Laird E, Kenny RA. Editorial: low population mortality from COVID-19 in countries south of latitude 35 degrees North supports vitamin D as a factor determining severity. Aliment PharmacolTher 51: 143 1437, 2020. doi:10.1111/apt.15777.
Sabetta JR, DePetrillo P, Cipriani RJ, Smardin J, Burns LA, Landry ML. Serum 25-hydroxyvitamin d and the incidence of acute viral respiratory tract infections in healthy adults. PLoS One 5: e11088, 2010. doi:10.1371/journal.pone.0011088.
Sandhu MS, Casale TB. The role of vitamin D in asthma. Ann Allergy Asthmalmmunol 105: 191-199, 2010. doi:10.1016/j.anai.2010.01.013.
Santoro D, Caccamo D, Lucisano S, Buemi M, Sebekova K, Teta D, De Nicola L. Interplay of vitamin D, erythropoiesis, and the renin-angiotensin system. BioMedResInt 2015: 145828, 2015. doi:10.1155/2015/145828.
Shi Y, Liu T, Yao L, Xing Y, Zhao X, Fu J, Xue X. Chronic vitamin D deficiency induces lung fibrosis through activation of the renin-angiotensin system. SciRep 7: 3312, 2017. doi:10.1038/s41598-017-03474-6.
Shirvani A, Kalajian TA, Song A, Holick MF. Disassociation of vitamin D’s calcemic activity and non-calcemic genomic activity and individual responsiveness: a randomized controlled double-blind clinical trial. Sci Rep 9: 17685,2019. doi:10.1038/s41598-019-53864-1.
Silvagno F, De Vivo E, Attanasio A, Gallo V, Mazzucco G, Pescarmona G. Mitochondrial localization of vitamin D receptor in human platelets and differentiated megakaryocytes. PLoS One 5: e8670, 2010. doi:10.1371/ journal.pone.0008670.
Sun ML, Yang JM, Sun YP, Su GH. Inhibitors of RAS might be a good choice for the therapy of COVID-19 pneumonia. Zhonghua Jie He He Hu Xi Za Zhi 43: E014,2020. doi:10.3760/cma.j.issn.1001-0939.2020.0014.
Taher YA, van Esch BCAM, Hofman GA, Henricks PAJ, van Oosterhout AJM. 1a,25-dihydroxyvitamin D3 potentiates the beneficial effects of allergen immunotherapy in a mouse model of allergic asthma: role for IL-10 and TGF-beta. J Immunol 180: 5211-5221, 2008. doi:10.4049/jimmunol.180.8.5211.
Takano Y, Mitsuhashi H, Ueno K. 1a,25-Dihydroxyvitamin D3 inhibits neutrophil recruitment in hamster model of acute lung injury. Steroids 76: 1305-1309,2011. doi:10.1016/j.steroids.2011.06.009.
Tan WSD, Liao W, Zhou S, Mei D, Wong WF. Targeting the renin-angiotensin system as novel therapeutic strategy for pulmonary diseases. Curr Opin Pharmacol 40: 9-17,2018. doi:10.1016/j.coph.2017.12.002.
Tan ZX, Chen YH, Xu S, Qin HY, Zhang C, Zhao H, Xu DX. Calcitriol inhibits bleomycin-induced early pulmonary inflammatory response and epithelial-mesenchymal transition in mice. Toxicol Lett 240: 161-171, 2016. doi:10.1016/j.toxlet.2015.10.022.
The Association of UK Dietitians. COVID-19, Coronavirus - Advice for General Public (Online). https://www.bda.uk.com/resource/covid-19-corona- virus-advice-for-the-general-public.html [March 16, 2020].
Tian WM, Yang YG, Shang YX, Cai XX, Chen WW, Zhang H. Role of 1,25-dihydroxyvitamin D3 in the treatment of asthma. Eur Rev Med PharmacolSci 18: 1762-1769,2014.
Topilski I, Flaishon L, Naveh Y, Harmelin A, Levo Y, Shachar I. The anti-inflammatory effects of 1,25-dihydroxyvitamin D3 on Th2 cells in vivo are due in part to the control of integrin-mediated T lymphocyte homing. EurJ Immunol 34: 1068-1076,2004. doi:10.1002/eji.200324532.
Trochoutsou AI, Kloukina V, Samitas K, Xanthou G. Vitamin-D in the immune system: genomic and non-genomic actions. Mini Rev Med Chem 15: 953-963,2015. doi:10.2174/1389557515666150519110830.
Turin A, Bax JJ, Doukas D, Joyce C, Lopez JJ, Mathew V, Pontone G, Shah F, Singh S, Wilber DJ, Rabbat MG. Interactions among vitamin D, atrial fibrillation, and the renin-angiotensin-aldosterone system. Am J Cardiol 122: 780-784, 2018. doi:10.1016/j.amjcard.2018.05.013.
Vaduganathan M, Vardeny O, Michel T, McMurray JJV, Pfeffer MA, Solomon SD. Renin-angiotensin-aldosterone system inhibitors in patients with Covid-19. N Engl J Med 382: 1653-1659, 2020. doi:10.1056/ NEJMsr2005760.
Vuichard Gysin D, Dao D, Gysin CM, Lytvyn L, Loeb M. Effect of vitamin D3 supplementation on respiratory tract infections in healthy individuals: a systematic review and meta-analysis of randomized controlled trials. PLoS One 11: e0162996, 2016. doi:10.1371/journal.pone.0162996.
Wacker M, Holick MF. Sunlight and vitamin D: a global perspective for health. Dermatoendocrinol 5: 51-108, 2013. doi:10.4161/derm.24494.
Wang Y, Yang Z, Gao L, Cao Z, Wang Q. Effects of a single dose of vitamin D in septic children: a randomized, double-blinded, controlled trial. J IntMedRes 48: 300060520926890, 2020. doi:10.1177/0300060520926890.
Xu J, Yang J, Chen J, Luo Q, Zhang Q, Zhang H. Vitamin D alleviates li- popolysaccharide-induced acute lung injury via regulation of the renin-angiotensin system. Mol Med Rep 16: 7432-7438, 2017. doi:10.3892/ mmr.2017.7546.
Xystrakis E, Kusumakar S, Boswell S, Peek E, Urry Z, Richards DF, Adikibi T, Pridgeon C, Dallman M, Loke TK, Robinson DS, Barrat FJ, O’Garra A, Lavender P, Lee TH, Corrigan C, Hawrylowicz CM.
Reversing the defective induction of IL-10-secreting regulatory T cells in glucocorticoid-resistant asthma patients. J Clin Invest 116: 146-155, 2006. doi:10.1172/JCI21759.
Yao L, Shi Y, Zhao X, Hou A, Xing Y, Fu J, Xue X. Vitamin D attenuates hyperoxia-induced lung injury through downregulation of Toll-like receptor 4. IntJMolMed 39: 1403-1408, 2017. doi:10.3892/ijmm.2017.2961.
Zemb P, Bergman P, Camargo CA Jr, Cavalier E, Cormier C, Courbebaisse M, Hollis B, Joulia F, Minisola S, Pilz S, Pludowski P, Schmitt F, Zdrenghea M, Souberbielle JC. Vitamin D deficiency and the COVID-19 pandemic. J Glob Antimicrob Resist 22: 133-134, 2020. doi:10.1016/j.jgar.2020.05.006.
Zhang H, Yang N, Wang T, Dai B, Shang Y. Vitamin D reduces inflammatory response in asthmatic mice through HMGB1/TLR4/NF-kB signaling pathway. Mol Med Rep 17: 2915-2920, 2018. doi:10.3892/ mmr.2017.8216.
