Fractures reduced 30 percent by Omega-3 (Omega-3 activates vitamin D)
Plasma phospholipid fatty acids and fish-oil consumption in relation to osteoporotic fracture risk in older adults: the Age, Gene/Environment Susceptibility Study
Am J Clin Nutr May 2015 vol. 101 no. 5 947-955
Tamara B Harris, Xiaoling Song, Ilse Reinders, Thomas F Lang, Melissa E Garcia, Kristin Siggeirsdottir, Sigurdur Sigurdsson, Vilmundur Gudnason, Gudny Eiriksdottir, Gunnar Sigurdsson, Laufey Steingrimsdottir, Thor Aspelund, Ingeborg A Brouwer, and Rachel A Murphy rachel.murphy@nih.gov
From the Laboratory of Epidemiology, and Population Sciences, National Institute on Aging, Bethesda, MD (TBH, IR, MEG, and RAM); the Biomarker Laboratory, Fred Hutchinson Cancer Research Center, Seattle, WA (XS); the Department of Health Sciences and the EMGO+ Institute for Health and Care Research, VU University, Amsterdam, The Netherlands (IR and IAB); the Department of Radiology and Biomedical Imaging, University of California, San Francisco, CA (TFL); the Icelandic Heart Association, Kopavogur, Iceland (KS, SS, VG, GE, GS, and TA); and the University of Iceland, Reykjavik, Iceland (VG, GS, and LS).
Supported by The Office of Dietary Supplements, NIH contract N01-AG012100, the NIA Intramural Research Program, Hjartavernd (the Icelandic Heart Association), the Althingi (the Icelandic Parliament), and a Banting Postdoctoral Fellowship (to RAM).
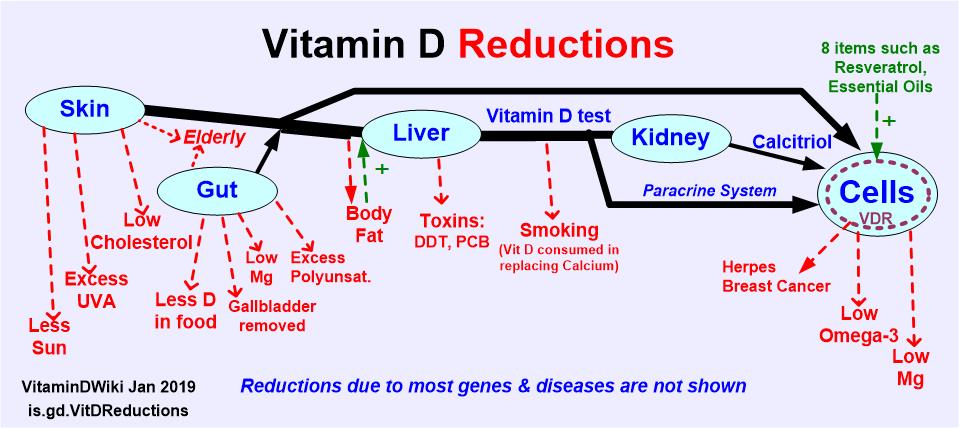 Notice Omega-3 and paracrine - click on chart for details
Notice Omega-3 and paracrine - click on chart for details
Background: Polyunsaturated fatty acids (PUFAs) may play a role in fracture, but studies have been largely confined to estimates of dietary intake.
Objective: We aimed to examine associations between fatty acids measured in late life and fish-oil consumption in early life, midlife, and late life with osteoporotic fracture risk.
Design: Osteoporotic fractures were determined from medical records over 5–9 y of follow-up in men and women aged 66–96 y. Data were analyzed from 1438 participants including 898 participants who were randomly selected from the Age, Gene/Environment Susceptibility Study, which is an observational study, and 540 participants with incident fracture. Plasma phospholipid fatty acids were assessed by using gas chromatography. Fish-oil consumption was assessed by using validated questionnaires as never (referent), less than daily, or daily. HRs and 95% CIs adjusted for age, education, height, weight, diabetes, physical activity, and medications were estimated by using Cox regression.
Results: In men, the highest tertile of PUFAs, n–3 (ω-3), and eicosapentaenoic acid were associated with decreased fracture risk [HRs (95% CIs): 0.60 (95% CI: 0.41, 0.89), 0.66 (0.45, 0.95), and 0.59 (0.41, 0.86), respectively]. In women, PUFAs tended to be inversely associated with fracture risk (P-trend = 0.06), but tertiles 2 and 3 were not independently associated with risk. Tertile 2 of n–6 and arachidonic acid was associated with fracture risk in women [HRs (95% CIs): 1.43 (1.10, 1.85) and 1.42 (1.09, 1.85), respectively].
Daily fish-oil consumption in late life was associated with lower fracture risk in men (HR: 0.64; 95% CI: 0.45, 0.91).
Daily fish-oil consumption in midlife was associated with lower fracture risk in women (HR: 0.75; 95% CI: 0.58, 0.98).
Conclusions: Greater PUFA concentrations may be associated with lower osteoporotic fracture risk in older adults, particularly in men. Critical time periods for n–3 fatty acid consumption may differ by sex.
Publisher wants $25 to access all of their content for 7 days
