Dry eyes associated with low vitamin D
200,000 IU Vitamin D injection reduced most measures of dry eye - Sept 2016
Vitamin D Supplementation for Patients with Dry Eye Syndrome Refractory to Conventional Treatment.
Sci Rep. 2016 Oct 4;6:33083. doi: 10.1038/srep33083.
Bae SH1, Shin YJ1, Kim HK1, Hyon JY2,3, Wee WR3, Park SG4.
1Department of Ophthalmology, Hallym University College of Medicine, Seoul, Republic of Korea.
2Department of Ophthalmology, Seoul National University Bundang Hospital, Seongnam, Gyeonggi, Korea.
3Department of Ophthalmology, Seoul National University College of Medicine, Seoul, Republic of Korea.
4Department of Occupational and Environmental Medicine, Inha University School of Medicine, Incheon, Republic of Korea.
This study investigated the effect of vitamin D supplementation in patients with dry eye syndrome (DES) refractory to conventional treatment with vitamin D deficiency. A total of 105 patients with DES refractory to conventional treatment and vitamin D deficiency that was treated with an intramuscular injection of cholecalciferol (200,000 IU). Serum 25-hydroxyvitamin D (25(OH)D) levels were measured. Eye discomfort was assessed using ocular surface disease index (OSDI) and visual analogue pain score (VAS). Tear break-up time (TBUT), fluorescein staining score (FSS), eyelid margin hyperemia, and tear secretion test were measured before treatment, and 2, 6, and 10 weeks after vitamin D supplementation. Mean serum 25(OH)D level was 10.52 ± 4.61 ng/mL. TBUT, and tear secretion test showed an improvement at 2 and 6 weeks after vitamin D supplementation compared to pretreatment values (p < 0.05 for all, paired t-test). Eyelid margin hyperemia and the severity of symptoms showed improvement at 2, 6, and 10 weeks after vitamin D supplementation (p < 0.05 for all). Compared to pre-treatment values, FSS, OSDI and VAS were decreased at 2 weeks (p < 0.05 for all). In conclusion, vitamin D supplementation is effective and useful in the treatment of patients with DES refractory to conventional treatment and with vitamin D deficiency.
PMID: 27698364 DOI: 10.1038/srep33083
Many great charts in the PDF
📄 Download the PDF from VitaminDWiki
Note: Refractory to Conventional Treatment = Dry Eyes not respond by Conventional Teatment?
Dry Eye Assessment in Patients With Vitamin D Deficiency. - Sept 2016
Eye Contact Lens. 2016 Sep 22. [Epub ahead of print]
Demirci G1, Karaman Erdur S, Ozsutcu M, Eliacik M, Olmuscelik O, Aydin R, Kocabora MS.
1Departments of Ophthalmology (G.D., S.K.E., M.O., M.E., R.A., M.S.K.), and Internal Medicine (O.O.), Istanbul Medipol University, Istanbul, Turkey.
OBJECTIVES: The aim of this study was to evaluate tear film function in patients with vitamin D deficiency.
METHODS: In a single center, 60 eyes of 30 patients with vitamin D deficiency (group 1), and 60 eyes of 30 healthy individuals (group 2) were evaluated using the Ocular Surface Disease Index (OSDI) questionnaire, Schirmer I test, tear break-up time (TBUT), scoring of ocular surface fluorescein staining using a modified Oxford scale, and tear osmolarity.
RESULTS: Tear osmolarity values, OSDI, and Oxford scale scores were significantly higher in group 1 (309±9 mOsm/L, 35.78±21.44 and 1.3±0.9, respectively) compared with group 2 (295±10 mOsm/L, 18.69±17.21 and 0.4±0.8, respectively) (P<0.001 for all). Schirmer I test and TBUT results in group 1 (8.5±3.7 mm and 8.7±0.6 sec, respectively) were significantly lower compared with group 2 (16.6±2.4 and 18.1±0.5, respectively) (P<0.001 for all).
CONCLUSIONS: This study demonstrates that vitamin D deficiency is associated with tear hyperosmolarity and tear film dysfunction. Patients with vitamin D deficiency may be prone to dry eye.
PMID: 27660921 DOI: 10.1097/ICL.0000000000000325 (behind paywall)
Serum 25-Hydroxyvitamin D Levels and Dry Eye Syndrome: Differential Effects of Vitamin D on Ocular Diseases. - Feb 2016
PLoS One. 2016 Feb 19;11(2):e0149294. doi: 10.1371/journal.pone.0149294. eCollection 2016.
Jee D1,2, Kang S3, Yuan C4, Cho E5,6, Arroyo JG7; Epidemiologic Survey Committee of the Korean Ophthalmologic Society.
Collaborators (14)
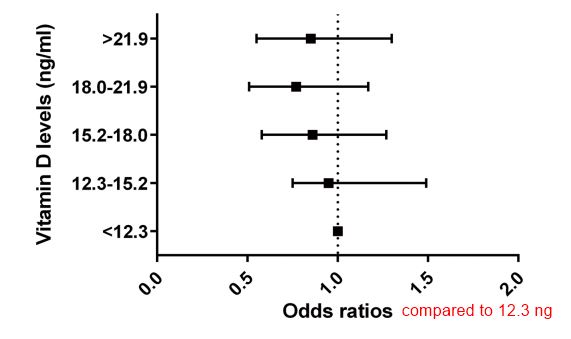
PURPOSE:
To investigate associations between serum 25-hydroxyvitamin D levels and dry eye syndrome (DES), and to evaluate the differential effect of vitamin D on ocular diseases including age-related macular disease (AMD), diabetic retinopathy (DR), cataract, and DES.
METHODS:
A total of 16,396 participants aged >19 years were randomly selected from the Korean National Health and Nutrition Examination Survey. All participants participated in standardized interviews, blood 25-hydroxyvitamin D level evaluations, and comprehensive ophthalmic examinations. DES was defined by a history of clinical diagnosis of dry eyes by a physician. The association between vitamin D and DES was compared to the associations between vitamin D and AMD, DR, cataract, and DES from our previous studies.
RESULTS:
The odds of DES non-significantly decreased as the quintiles of serum 25-hydroxyvitamin D levels increased (quintile 5 versus 1, OR = 0.85, 95%CI: 0.55-1.30, P for trend = 0.076) after adjusting for potential confounders including age, sex, hypertension, diabetes, smoking status, and sunlight exposure times. The relative odds of DES (OR = 0.70, 95% CI: 0.30-1.64) and cataract (OR = 0.76, 95% CI: 0.59-0.99) were relatively high, while those of DR (OR = 0.37, 95% CI: 0.18-0.76) and late AMD (OR = 0.32, 95% CI: 0.12-0.81) were lower in men.
CONCLUSIONS:
The present study does not support an association between serum 25-hydroxyvitamin D levels and DES. The preventive effect of serum 25-hydroxyvitamin D may be more effective for DR and late AMD than it is for cataract and DES.
📄 Download the PDF from VitaminDWiki
The association of vitamin D deficiency with tear break-up time and Schirmer testing in non-Sjögren dry eye - June 2015
Eye , (12 June 2015) | doi:10.1038/eye.2015.96
B E Kurtul, P A Özer and M S Aydinli
(TBUT) | 5 sec | 7 sec | | Schirmer scores | 12 mm | 19 mm | | Dry eye symptoms | 100% | 15% |
Purpose: To investigate the effect of vitamin D deficiency on tear break-up time (TBUT) and Schirmer test scores and to assess their relationship in non-Sjögren dry-eye patients.
Methods: Thirty-four patients with serum vitamin D deficiency and 21 control subjects with normal vitamin D levels were included in this study. The TBUT and Schirmer-1 test without topical anesthesia were performed to all patients.
Results: The mean TBUT were 5.18±2.15 and 7.36±3.10 s and Schirmer scores were 12.18±6.44 and 18.57±8.99 mm in the study and control groups, respectively. TBUT scores and Schirmer-1 results of the study group were significantly lower than the control group (P=0.01 and 0.007, respectively). The mean vitamin D levels were 11.50±1.8 ng/ml in the study group and 32.8±8.72 ng/ml in control group (P=0.001). Dry-eye symptoms were detected in all patients in the study group and 15% of the patients in the control group.
Conclusions: We demonstrated that vitamin D deficiency decreases the TBUT and Schirmer test values and may be associated with dry-eye symptoms in non-Sjögren syndrome.
Publisher rents the PDF for $5
Unsure if Dry Eye causes low Omega-3 or the other way around - May 2018
Clinical trials with multiple endpoints can establish a correlation, but not (yet) causality, between dietary supplementation with omega-3 fatty acids and keratoconjunctivitis sicca
Journal of Medical Economics https://doi.org/10.1080/13696998.2018.1478838
Roger Lee Mendoza
Aim: We review clinical evidence of therapeutic efficacy and effectiveness of omega-3 fatty acids (omega-3s) in keratoconjunctivitis sicca, colloquially known as dry eye disease. In doing so, we identify relevant literature to address the following questions: 1) What definitive guidance can clinical evidence offer eye physicians and their patients? 2) What aspects of omega-3 supplementation lack definitive evidence, and how might economic assessments help?
Methods: A targeted and systematic search strategy based on PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) was designed in this study for refereed clinical trials of omega-3s in dry eye treatment. Four key databases were accessed. Records were filtered through a three-step process using predetermined inclusion criteria. Data was extracted for experimental design, sample population characteristics, content of test and control groups, symptoms and associated conditions, diagnostic measures, patient health outcomes, adverse events, and model time horizon.
Results: A total of 219 records were initially identified, of which 21 prospective clinical trials, with a total of 2,973 participants, were admitted for review. Clinical evidence indicates that daily supplementation with omega-3s statistically correlates with dry eye treatment in the general symptomatic population as well as induced sub-populations. Reported adverse events are minimal. These trials nonetheless exhibit considerable heterogeneity in clinical endpoints, particularly as a result of continuous advances in scientific knowledge and technology. Their findings and recommendations appear to be of limited external validity. And causal inferences are needed, but difficult to establish. These have encouraged and sustained variations in medical practice and normative decision-making.
Conclusions: Comparability of omega-3 therapeutic efficacy and effectiveness remains a major challenge in dry eye disease management. Notwithstanding its multi-factorial character, addressing prevailing methodological and empirical issues in clinical trials will help reduce knowledge gaps and normative choices among physicians and patients alike. In this regard, pharmacoeconomics offers a useful and robust toolset through which analysis of cost-minimization, cost-effectiveness, and cost-utility as well as meta-analysis can be comparatively pursued.
--
See also VitaminDWiki
Dry eyes associated with low Vitamin D – meta-analysis May 2020
Dry eye decreased with weekly 50,000 IU vitamin D injection for 8 weeks – Sept 2017
Omega-3 reduced dry eye (computer related) by 3X - RCT June 2015
Dry Eyes treated by Omega-3 and Vitamin D – many studies
Personal Note: Admin of VitaminDWiki used to have dry eyes
Since I starting taking of Omega-3 and Vitamin D I no longer have dry eyes
Sjögren’s syndrome (2nd most common rheumatic disease) and vitamin D - many studies - SS is also a source of dry eyes
Vision category listing has items along with related searches
See also web
- The time required for dry spots to appear on the corneal surface after blinking
- >10 seconds is thought to be normal,
- 5 to 10 seconds, marginal
- <5 seconds low (with high likelihood of dry eye symptoms)
- New study suggests vitamin D deficiency is related to dry eye Vitamin D Council
- reporting on: Yildirim P., et al. Dry eye in vitamin D deficiency: more than an incidental association. International Journal of Rheumatic Diseases, 2015.
- Vitamin D levels: Associated with dry eyes? Vitamin D Council
- Reporting on: Galor A et al. Effect of a Mediterranean Dietary Pattern and Vitamin D Levels on Dry Eye Syndrome. Cornea, 2014.
